Plantar Plate Injuries
Top Contributors - Ewa Jaraczewska and Jess Bell
Introduction[edit | edit source]
The plantar plate complex is essential for foot mechanics.[1] It comprises the plantar aspect of the first metatarsophalangeal joint (MTPJ). It provides dynamic and static joint stability while protecting the joint's articular surfaces.[1] The lesser toe plantar plates also provide joint stability and articular surface protection. When discussing plantar plate pathologies, clinicians must recognise two categories of injuries: MTPJ (great toe) and second through fifth (lesser toe) injuries.[2]
Clinically Relevant Anatomy[edit | edit source]
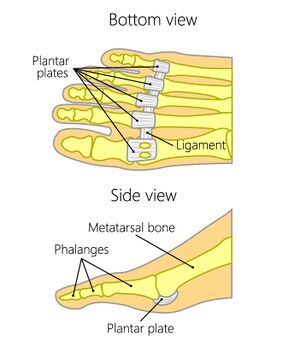
The plantar plate complex has a thick, distal attachment at the base of the proximal phalanges of the feet. The thin proximal attachment extends to the metatarsal head-neck junction or to the intersesamoid ligament. It is inseparable from the plantar capsule, ligaments, and musculotendinous structures. It provides a cushioning system for the metatarsal heads and prevents them from dropping.[3][1] The plantar plates of the lesser toes are a single dominant fibrocartilaginous capsular thickening and extend from the metatarsal head to the proximal phalanx base at each joint.
The plantar plate complex is a fibrocartilaginous pad that consists of three parts: bony, ligamentous, and musculotendinous.[2]
The bony part includes:
- Medial and lateral sesamoids
- The proximal phalanx
- The articular surfaces of the metatarsal head
The ligamentous part is comprised of:
- Sesamoid phalangeal ligaments (SPLs): these are the thickest ligaments of the first metatarsophalangeal joint (MTPJ). They prevent proximal sesamoid subluxation during hyperextension while walking or running.[1]
- Intersesamoid ligament (ISL): transverse bundles of collagen fibres connecting two sesamoids bones.[1]
- Paired metatarsosesamoid ligaments (MTSLs): are called suspensory ligaments. Their role is to assist with sesamoid stabilisation.[1]
The musculotendinous part consists of the following:
- Medial and lateral heads of the flexor hallucis brevis which have a proximal attachment to the proximal and plantar surfaces of the medial and lateral sesamoids.[1]
- Flexor hallucis longus which has an insertion at the base of the distal phalanx.[1]
- Adductor hallucis which has its the main insertion at the sesamoids.[1]
- Abductor hallucis which inserts at the sesamoids.[2]
Plantar plate complex supportive structures:
- Medial and lateral metatarsophalangeal ligaments (collateral ligaments):
- These are not part of the plantar plate complex.
- They act as static stabilisers when valgus or varus forces are applied.
- Extensor hallucis longus (EHL) and extensor hallucis brevis (EHB):
- These are dynamic stabilisers during plantar flexion.
- Plantar fascia
- The plantar plate is attached to the central component of plantar aponeurosis and may be considered a distal extension of the plantar fascia.[4]
The plantar plate receives its blood supply from the vascular network of the surrounding soft tissue; however, the mid portion of the plantar plate lacks sufficient vascularity.[5]
Mechanism of Injury / Pathological Process[edit | edit source]
The first MTPJ plantar plate complex can be injured after an acute trauma or a chronic, degenerative process can occur.
- Acute trauma
- Osteochondral injuries of the sesamoids:[1]
- Sesamoiditis: a painful, inflammatory condition in the acute phase, with sclerosis in the chronic phase
- Sesamoid fractures
- Osteonecrosis diastasis of a bipartite sesamoid
- Chondral injuries with loose osteochondral fragments
- Joint hyperextension causes injury to the sesamoid phalangeal ligaments[2]
- Turf toe is an injury of the first metatarsophalangeal (MTP) articulation. It occurs during hyperextension of the MTP joint, with fixed equinus at the ankle.[6] When unrecognised, it can become a debilitating condition with persistent pain, progressive deformity and joint degeneration.[6] You can read more about Turf toe here.
- Articular surface injuries of the proximal phalanx and metatarsal head
- Caused by increased load on the metatarsal heads in the extended position of the metatarsophalangeal joint[3]
- Jumping down from a height[3]
- Injuries in dancers or sprinters (i.e. athletes who do a lot of work on their forefoot)[3]
- Osteochondral injuries of the sesamoids:[1]
- Degenerative process
- Osteoarthritis
- Hallux valgus deformities: lateral deviation of the great toe.[2]
- Other foot pathologies which overload the MTPJ and cause plantar plate injuries include:
- Excessive pronation
- Short first metatarsal
- Long second metatarsal
The most common injuries of the plantar plates of the lesser toes include the second and third MTPJ plantar plates. The pathologies are:
- Degeneration (thickening of the plate)
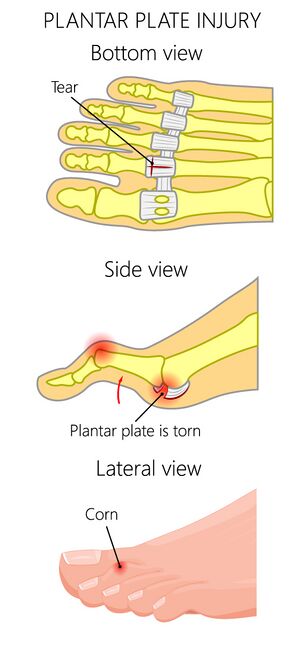
- Partial thickness tearing
- Complete tearing (defect at the plate insertion)
Clinical Presentation[edit | edit source]
The following signs and symptoms can indicate plantar plate injuries:
- The onset of persistent, constant, activity-related pain and tenderness over the metatarsal head (ball of the foot).[7][8][9][10]
- Swelling under the ball of the foot that extends towards the toes.[3]
- Symptoms similar to compression syndromes of the plantar digital nerves, as a result of micro trauma or a space occupying lesion. Symptoms include tenderness of the heel and medial plantar arch and numbness along the medial plantar foot.[11]
- Widening of the interdigital space: The toe gapping sign (Churchill sign) - i.e. there is a greater spread between the 2nd and 3rd toe.[12]
- Loss of ground touch: incapacity of the toes to touch the ground normally.[13]
- Presence of minor toe deformities: dorsal elevation, crossover toe, pronation or supination.[13]
Diagnostic Procedures[edit | edit source]
To confirm plantar plate injuries, the following diagnostic procedures are recommended:
- X-ray: completed in standing to visualise dropped metatarsals.
- Ultrasound: considered a first-line tool to quickly and accurately localise and characterise forefoot pathologies.[9] Using static and dynamic ultrasound techniques is common for assessing plantar plate pathology, with dynamic assessment offering greater sensitivity.[14] A partial- or full-thickness plantar plate defect is the most common presentation of a plantar plate tear that can be easily detected on ultrasound.[15]
- Computerised tomography (CT) can be used in challenging situations where surgery is required for plantar plate injury. This is a diagnostic procedure of choice when signs and symptoms of soft tissue injury are present.[3]
- Magnetic resonance imaging (MRI) has high accuracy in diagnosing plantar plate injuries. It is a preferred procedure to differentiate between plantar plate injury and Morton's neuroma.[3][2]
Assessment[edit | edit source]
Interview[edit | edit source]
Taking a patient's history is an excellent point of reference.[3] The patient should be asked about the following:
- Predisposing factors (e.g. wearing high heels)
- Activities and habits associated with the condition (sports-related trauma, professional dancers)
- History of wearing orthotics
Observation/Palpation[edit | edit source]
Observation should be completed with the patient in a standing position to determine the direction of weight shift, the presence of smaller toes abnormalities or deviations, or an increase in space between the toes.[3] Next, the clinician should observe while the patient performs a single-leg stance. In addition, the patient may report:[13]
- A history of acute pain in the MTPJs of the smaller toes
- Feeling of local oedema
Tests[edit | edit source]
- A positive anterior-posterior draw test (Modified Lachman Test). The clinician stabilises the patient's toe at the metatarsal and exerts a drawer test on the phalanges. A slight clunk can be heard as the joint subluxes in the plantar direction. It is considered the most reliable and accurate tool to classify and grade a plantar plate lesion. Thompson and Hamilton[16] proposed a classification system based on the level of subluxation of the proximal phalanx:[13]
- G0: stable joint. Pain is present, but no joint deformity.
- G1: mild instability (subluxation < 50%) characterised by widening the space between the toes and medial displacement. Joint pain and swelling.
- G2: moderate instability (subluxation > 50%) with medial, lateral, dorsal or dorsomedial deformity and toe hyperextension. Joint pain with little or no swelling.
- G3: severe instability (capacity for joint dislocation): dorsal or dorsomedial deformity with the second toe overlapping on hallux. A flexible toe clawing may be present. Joint and feet pain, little or no oedema.
- G4: dislocated joint: severe deformity and fixed toe clawing. Joint and feet pain, little or no oedema.
- The negative plantar grip test or "paper-pulling" test: this test is assessed using an 8cm x 1cm strip of paper placed under the 2nd toe of the standing patient. The patient is unable to ‘grip’ the paper.
- A positive Reverse Windlass Test: The patient is standing on the little box with the metatarsals supported at the edge of the box. No pathology: the windlass mechanism plantarflexes the proximal phalanx over the edge of the box. Pathology: lack of toes plantar flexion.
- Manual muscle strength test for the intrinsic muscles and flexor digitorum longus (toe plantar flexion).
Management / Interventions[edit | edit source]
The conservative management of a plantar plate injury should utilise a holistic approach, which addresses shoe wear, local foot support, local and global strength and mobility (foot and lower leg), and a posture assessment.
Shoe wear: no barefoot walking, no high heels, no flexible, minimalist type shoes, like open-toes or flip-flops. Instead, a stiff-soled shoe, a stiff boot or a rocker shoe with a soft insert is recommended.
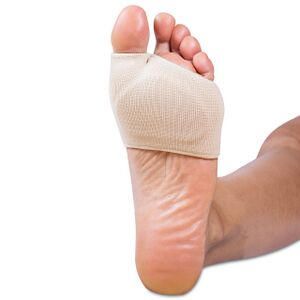
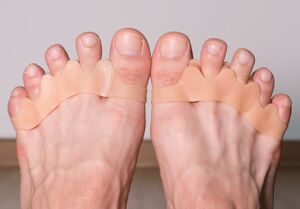
Local foot support: can include customised orthotics, taping, and toe spacers.
- Customised orthotics usually involve a metatarsal pad
- Toe spacers keep the toes apart
- Taping to offload metatarsal head
- Kinesiotaping method: little fork method
- Cloth adhesive tape: "AIDS" ribbon tape to limit the extension of the second MPTJ
- Local and global strength and mobility: midfoot mobilisation, strengthening of the intrinsics and toe plantar flexors, improving neuromuscular control of the pelvis and hip[18]
Other Interventions[edit | edit source]
- Shock wave therapy[19]
- Cortisone injections - caution: may weaken the plantar plate
- Surgery - however, surgery is complex, and recovery is slow
Resources[edit | edit source]
- Turf toe
- Yamada AF, Crema MD, Nery C, Baumfeld D, Mann TS, Skaf AY, Fernandes ADRC. Second and Third Metatarsophalangeal Plantar Plate Tears: Diagnostic Performance of Direct and Indirect MRI Features Using Surgical Findings as the Reference Standard. AJR Am J Roentgenol. 2017 Aug;209(2):W100-W108.
- Understanding The Biomechanics Of Plantar Plate Injuries
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Hallinan JTPD, Statum SM, Huang BK, Bezerra HG, Garcia DAL, Bydder GM, Chung CB. High-Resolution MRI of the First Metatarsophalangeal Joint: Gross Anatomy and Injury Characterization. Radiographics. 2020 Jul-Aug;40(4):1107-1124.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Gyftopoulos S, Woertler K. Ankle and foot. Musculoskeletal Diseases 2021-2024. 2021:107-20.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Simpson H. Plantar Plate Injuries Course. Plus 2022
- ↑ Chen DW, Li B, Aubeeluck A, Yang YF, Huang YG, Zhou JQ, Yu GR. Anatomy and biomechanical properties of the plantar aponeurosis: a cadaveric study. PLoS One. 2014 Jan 2;9(1):e84347.
- ↑ Finney FT, McPheters A, Singer NV, Scott JC, Jepsen KJ, Holmes JR, Talusan PG. Microvasculature of the Plantar Plate Using Nano–Computed Tomography. Foot & ankle international. 2019 Apr;40(4):457-64.
- ↑ 6.0 6.1 Najefi AA, Jeyaseelan L, Welck M. Turf toe: A clinical update. EFORT Open Rev. 2018 Sep 24;3(9):501-506. doi: 10.1302/2058-5241.3.180012.
- ↑ Pelly T, Holme T, Tahir MA, Kunasingam K. Forefoot pain. BMJ. 2020 Oct 9;371.
- ↑ Lai SH, Tang CQ, Thevendran G. Forefoot Injuries in Sports. Journal of Foot and Ankle Surgery (Asia Pacific). 2020 Jul;7(2):51.
- ↑ 9.0 9.1 Chen X, Zhou G, Xue H, Wang R, Bird S, Sun D, Cui L. High-Resolution Ultrasound of the Forefoot and Common Pathologies. Diagnostics (Basel). 2022 Jun 24;12(7):1541.
- ↑ Klein EE, Weil L Jr, Weil LS Sr, Coughlin MJ, Knight J. Clinical examination of plantar plate abnormality: a diagnostic perspective. Foot Ankle Int. 2013 Jun;34(6):800-4.
- ↑ Feger J. Medial plantar nerve entrapment. Reference article, Radiopaedia.org. (accessed on 19 Oct 2022)
- ↑ Nery C, Coughlin MJ, Baumfeld D, Raduan FC, Mann TS, Catena F. Classification of metatarsophalangeal joint plantar plate injuries: history and physical examination variables. Journal of Surgical Orthopaedic Advances. 2014 Jan 1;23(4):214-23.
- ↑ 13.0 13.1 13.2 13.3 Nery C, Coughlin M, Baumfeld D, Raduan F, Mann TS, Catena F. How to classify plantar plate injuries: parameters from history and physical examination. Rev Bras Ortop. 2015 Oct 26;50(6):720-8.
- ↑ Feuerstein CA, Weil L Jr, Weil LS Sr, Klein EE, Fleischer A, Argerakis NG. Static Versus Dynamic Musculoskeletal Ultrasound for Detection of Plantar Plate Pathology. Foot Ankle Spec. 2014 Aug 1;7(4):259-265.
- ↑ Albright RH, Brooks B, Chingre M, Klein EE, Weil Jr LS, Fleischer AE. Diagnostic accuracy of magnetic resonance imaging (MRI) versus dynamic ultrasound for plantar plate injuries: A systematic review and meta-analysis. European Journal of Radiology. 2022 Apr 30:110315.
- ↑ Thompson FM, Hamilton WG. Problems of the second metatarsophalangeal joint. Orthopaedics. 1987 Jan;10(1):83-9.
- ↑ Kevin Kirby. Plantarflexion Taping for Plantar Plate Tears. 2016. Available from: https://www.youtube.com/watch?v=meUFV2UQyf8 [last accessed 10/10/2022]
- ↑ Ojofeitimi S, Bronner S, Becica L. Conservative management of second metatarsophalangeal joint instability in a professional dancer: a case report. Journal of orthopaedic & sports physical therapy. 2016 Feb;46(2):114-23.
- ↑ Labbad ZG, Love E, Shah DN, Kihira Y, Greensberg V. Treatment of lesser metatarsophalangeal joint plantar plate tear via Extracorporeal Pulse Activation Technology (EPAT) with MRI Follow-up: A case report. The Foot and Ankle Online Journal 2020; 13(2): 5. Available from http://faoj.org/2020/07/31/treatment-of-lesser-metatarsophalangeal-joint-plantar-plate-tear-via-extracorporeal-pulse-activation-technology-epat-with-mri-follow-up-a-case-report/ [last access 10.10.2022]