Achilles Tendinopathy - Biomechanical Properties
Original Editors - Jacob Wong as part of The University of Waterloo Biomechanics Project
Top Contributors - Jacob Wong, Cindy John-Chu, Natasha Ivanochko, Ashmita Patrao, Simisola Ajeyalemi and Kim Jackson
Introduction[edit | edit source]
Achilles Tendinopathy is a degenerative, non-inflammatory condition affecting the Achilles tendon[1]. It is one of the common sports-related injuries of the lower extremity with an annual incidence rate of 7-9% in elite runners[2]. Tendinopathy is a term that describes clinical conditions of tendons that arise from overuse[1]. It can be further classified as tendinosis or tendinitis after a histopathological examination describing the pathology of the condition[1]. Tendinosis describes intratendinous degeneration characterized by collagen fiber disorientation and thinning, with no inflammation. While tendinitis describes tendon inflammation[1]. This article is aimed to establish biomechanical factors relating to running and walking gait that contribute to the development of Achilles Tendinopathy through the analysis of EMG, kinetic, and kinematic factors. Analysis of biomechanical factors may provide insight on how to treat specific Achilles Tendinopathy cases.
Achilles Tendon[edit | edit source]
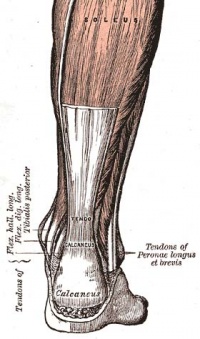
Tendons enable joint motion and stabilization through force transmission of tensile loads produced by muscles onto bones[3]. The Achilles tendon forms through the merger of the gastrocnemius and soleus through two types of junctions[1]. The more common junction is when the aponeuroses of the gastrocnemius and soleus join 12cm proximal to the calcaneal insertion[1]. While the less common junction has the gastrocnemius aponeurosis inserting directly into the soleus aponeurosis[1]. Anatomically, the Achilles tendon has an upper portion that is round with a flat distal insertion[1]. The collagen fibers spiral at 90 degrees and help release energy stored during locomotion[1]. The Achilles tendon crosses the ankle joint and inserts on the calcaneus, so it is important to be familiar with the structure and function of the foot and ankle.
Etiology[edit | edit source]
The etiology of the condition remains somewhat unclear[1]. However, various theories link factors relating to overuse stresses, impaired vascularity, inflexibility, and many others to the development of Achilles Tendinopathy[1]. The main mechanism that is thought to contribute to the development of Achilles Tendinopathy is excessive loading during vigorous activities, such as running, without enough rest[1]. Without enough time to repair, this can lead to cumulative microtrauma[1]. Microtrauma is the result of non-uniform stress in the tendon caused by different force contributions from gastrocnemius and soleus creating frictional forces and localized collagen fiber damage[1]. These concepts will be further discussed in the Biomechanical Analysis section.
Gait Characteristics[edit | edit source]
To analyze gait deviations, it is important to understand what is considered a ‘normal’ gait pattern. The gait cycle is defined as two consecutive foot contacts of the same limb[4]. The major difference in running biomechanics is the single support phase occurring rather than the double support phase in walking gait[4]. Deviations in running biomechanics lead to the adaptations of different common running styles that can alter performance.
Biomechanical Analysis[edit | edit source]
EMG[edit | edit source]
Those with Achilles Tendinopathy exhibit reduced and delayed muscular activity compared to unaffected individuals[5]. Before heel-strike, there is a reduction of tibialis anterior activity with a calculated effect size of -1.00[6]. After heel-strike, during weight acceptance, there was reduced activation of rectus femoris, gluteus medius, peroneus longus, and medial gastrocnemius by a calculated effect size of -1.40, -1.05, -0.54, -0.63, respectfully[6][7]. Lastly, there was reduced activation of the gluteus maximus during the midstance phase, resulting in lower hip extensor moments[8]. These reductions in muscle activity may impact the biomechanical factors in the gait such as uneven ground reaction force, alterations in joint positions, and temporospatial parameters[5]. Lower hip extensor moments may result in increases in joint moments and compensations down the kinetic chain affecting the forces placed on the Achilles tendon[5].
Kinetic[edit | edit source]
McCrory and colleagues found that those with Achilles Tendinopathy display delay in reaching peak forces for the first vertical peak and increases in braking force and average propulsive force[9]. These alterations may serve as a protective mechanism to reduce pain[5].
Kinematic[edit | edit source]
Clement and colleagues introduced the idea of functional overpronation producing a whipping action contributing to the development of Achilles Tendinopathy[10]. During heel-strike, individuals are in a pronated position with a flexed knee, imparting internal rotation moments on the tibia[10]. Normally, during the transition to midstance, the knee goes into extension while the foot transitions to a supinated position creating external rotation moments[10]. However, in functional overpronation, the foot remains in a pronated position creating opposing external and internal rotation moments[10]. In turn, this produces a whipping effect drawing the Achilles tendon medially and resulting in microtears[10]. This is backed by McCrory et al. as they found increased time to maximum pronation[9]. Further supporting evidence by Donoghue and colleagues, showed that there was greater ankle eversion in those with Achilles Tendinopathy[11]. In addition, Clement found that those with poor flexibility of the triceps surae may use foot pronation as compensation to gain range of motion during dorsiflexion[10].
Foot posture, concerning arch height, was found to redirect plantar pressure[12]. Those with a low longitudinal arch displayed decreased peak pressures under the lateral forefoot foot[12]. This is a result of increased contact area and maximum pressures on the medial midfoot[12]. In contrast, those with a high longitudinal arch had increased peak pressure under the lateral forefoot due to the reduced contact area of the medial midfoot[12]. As a result of the difference in plantar pressures, those with low arches display more injuries occurring on the medially, while those with high arches display more injuries laterally[12].
Conclusion[edit | edit source]
Deviations in the gait cycle can contribute to microtears through repetitive loading of uneven stress on the Achilles Tendon. Reduction in muscle activations, force production, and kinematic compensations such as functional overpronation may be factors in the development and persistence of associated symptoms in Achilles Tendinopathy. Exercise programs that work on optimal biomechanics of the lower limb may help mitigate Achilles Tendinopathy symptoms. Resources such as algorithms and toolkits may help practitioners develop a treatment plan for their clients with Achilles Tendinopathy.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Kader C, Saxena A, Movin T, Maffulli N. Achilles tendinopathy: some aspects of basic science and clinical management. (Review). British Journal of Sports Medicine. 2002;36:239+.
- ↑ Johannsen FE, Gam AN. [Achillodynia is not just a sports injury]. Ugeskrift for laeger. 2010;172:3325-9.
- ↑ Wang JHC, Guo Q, Li B. Tendon Biomechanics and Mechanobiology – A Minireview of Basic Concepts and Recent Advancements. Journal of Hand Therapy. 2012;25:133-141.
- ↑ 4.0 4.1 Cappellini G, Ivanenko YP, Poppele RE, Lacquaniti F. Motor Patterns in Human Walking and Running. Journal of Neurophysiology. 2006;95:3426-3437.
- ↑ 5.0 5.1 5.2 5.3 Ogbonmwan I, Kumar BD, Paton B. New Lower-limb gait biomechanical characteristics in individuals with Achilles tendinopathy: A systematic review update. Gait & Posture. 2018;62:146-156.
- ↑ 6.0 6.1 Azevedo LB, Lambert MI, Vaughan CL, O’Connor CM, Schwellnus MP. Biomechanical variables associated with Achilles tendinopathy in runners. British Journal of Sports Medicine. 2009;43:288-92.
- ↑ Baur H. Müller S, Hirschmüller A, Cassel M, Weber J, Mayer F. Comparison in lower leg neuromuscular activity between runners with unilateral mid-portion Achilles tendinopathy and healthy individuals. Journal of electromyography and kinesiology. 2011;21:499-505.
- ↑ Franettovich MM, Honeywill C, Wyndow N, Crossley KM, Creaby MW. Neuromotor control of gluteal muscles in runners with achilles tendinopathy. Medicine and science in sports and exercise. 2014;46:594-9.
- ↑ 9.0 9.1 McCrory JL, Martin DF, Lowery RB, Cannon DW, Curl WW, Read Jr HM et al. Etiologic factors associated with Achilles tendinitis in runners. Medicine and science in sports and exercise. 1999;31:1274-81.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 Clement DB, Taunton JE, Smart GW. Achilles tendinitis and peritendinitis: Etiology and treatment. The American Journal of Sports Medicine. 1984;12:179-184.
- ↑ Donoghue OA, Harrison AJ, Laxton P, Jones RK. Lower limb kinematics of students with chronic achilles tendon injury during running. Research in Sports Medicine. 2008;16:23-38.
- ↑ 12.0 12.1 12.2 12.3 12.4 Hollander K, Zech A, Rahlf AL, Orendurff MS, Stebbins J, Heidt C. The relationship between static and dynamic foot posture and running biomechanics: A systematic review and meta-analysis. Gait & Posture. 2019;72:209-122.