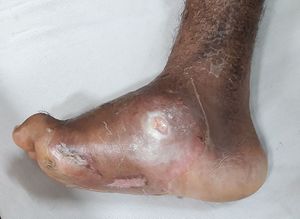
Charcot Foot
Original Editor - Chelsea McLene
Top Contributors - Chelsea Mclene, Kim Jackson and Nikhil Benhur Abburi
What is Charcot Foot?[edit | edit source]
Charcot foot is a serious complication which can affect persons with peripheral neuropathy, especially those with diabetes mellitus. This is a condition in which the nerves in the lower legs and feet have been damaged. The damage causes a loss of sensation in the feet. It affects the bones, joints, and soft tissues of the foot and ankle.[1] The bones become weak and can break. It has to be treated as early as possible or else the joints in the foot collapse and the foot eventually becomes deformed causing pressure sores to develop in the foot or ankle. An open wound with foot deformity can lead to an infection and even amputation.[2]
[For more information, click here to see the slide video]
Symptoms[edit | edit source]
- Swelling or redness of the foot or ankle.
- Skin feeling warmer at the point of injury.
- A deep aching feeling.
- Deformation of the foot.
Causes[edit | edit source]
- Alcohol or drug abuse.
- An infection.
- Spinal cord injury or disease.
- Parkinson's disease.
- HIV.
- Syphilis.
There’s no specific cause for Charcot foot. Some things can trigger it:
- A sprain or broken bone that doesn’t get treatment quickly
- A sore on your foot that doesn’t heal
- An infection
- Trauma
- Foot surgery that heals slowly[3]
Stages[edit | edit source]
Stage One: Fragmentation and destruction[edit | edit source]
- This is acute stage characterized by redness, swelling, warmth of foot and ankle.
- Internally, soft tissue swelling and small bone fractures are starting to occur. The result is destruction of the joints and surrounding bone. This causes the joints to lose stability, resulting in dislocation. The bones may even jellify, softening completely.
- Rocker bottom foot deformity
- Bony protrusions
- If not treated, this stage can last for up to one year.
Stage Two: Coalescence[edit | edit source]
The body attempts to heal the damage done during the first stage. Destruction of the joints and bones slows down, resulting in less swelling, redness, and warmth.
Stage Three: Reconstruction[edit | edit source]
- This is the final stage in which the joints and bones of the foot heal. Unfortunately, they do not go back to their original condition or shape on their own. While no further damage is being done to the foot, it is often left in a deformed, unstable condition.
- The foot may also be more prone to the formation of sores and ulcers, which might lead to further deformity or in some cases the need for amputation.[5]
Diagnosis[edit | edit source]
At early stages, it may be difficult to diagnose Charcot Foot since the X-ray and lab tests may be normal.
Later stages, X-rays produces images of structures inside the body, to examine the foot's bones and joints. An X-ray can reveal a bone fracture or joint dislocation related to Charcot foot, as well as any change in the shape, or alignment, of the foot.[5]
Other tests:
- Semmes-Weinstein 5.07/10 gram monofilament test analyzes sensitivity to pressure and touch in large nerve fibers
- Pinprick test assesses ability to feel pain
- Neurometer test identifies peripheral nerve dysfunction such as diabetic neuropathy
- Testing tendon reflexes and analyzing the muscle tone and strength in leg and foot.
Treatment[edit | edit source]
Medical Management[edit | edit source]
- Diabetic Wound Care Management.
- Antibiotic treatment is indicated in all infected wounds in combination with wound care, until the infection is cleared up.[7]
- Hospitilisation, immobilisation, and IV antibiotics are indicated for limb threatening or uncontrolled infections.[7]
- Urgent surgery is indicated if the infection is "accompanied by a deep abscess, extensive bone or joint involvement, crepitus, substantial necrosis or gangrene, or necrotising fasciitis."[7] Lepäntaloa et al. recommend that "surgical intervention for moderate or severe infections is likely to decrease the risk of major amputation."[7]
Conservative Management[edit | edit source]
It can take several months to treat Charcot foot.
A Charcot restraint orthotic walker (CROW)is used to stabilize the deformities of foot and ankle and minimize bone & joint destruction, it has a rocker bottom sole and total contact design immobilize the joints and allow the patients to ambulate
- Foot cast for 2-3months.
- Walking aids
- Braces
- Prevent new problems
- Wearing shoes that fit feet properly.[8]
- Life style modifications.
Surgical Management[edit | edit source]
It is done to stabilize any fractured bones or dislocated joints and allow them to heal. A surgeon may also realign or fuse the bones of the foot to better position them to bear weight.[9]
- Exostectomy
- Achilles Tendon Lengthening
- Fusion
Physical Therapy[edit | edit source]
- Physical Therapists are involved in both the prevention and management of diabetic foot complications. [10] This is done by gait, posture, and foot off-loading education and training.[10]
- Diabetes Medical and Physical Therapy Management
- Ankle and foot arthropathies Medical Management
- Physical Activity in Diabetes
- Diabetic foot Management
- Diabetic Neuropathy Management/Intervention
- The Physical Therapist is also involved in the rehabilitation process after an amputation.
Physical Therapy[edit | edit source]
- Physical Therapists are involved in both the prevention and management of diabetic foot complications. [11] This is done by gait, posture, and foot off-loading education and training.[11]
- Diabetes Medical and Physical Therapy Management
- Ankle and foot arthropathies Medical Management
- Physical Activity in Diabetes
- Diabetic foot Management
- Diabetic Neuropathy Management/Intervention
- The Physical Therapist is also involved in the rehabilitation process after an amputation.
Patient education[edit | edit source]
Diabetic Foot Care[edit | edit source]
- Inspect your feet daily. Check for cuts, blisters, redness, swelling or nail problems and inform doctor if you notice any changes.[12]
- Bathe feet in lukewarm water.
- Wash feet using a soft washcloth or sponge. Dry by blotting or patting and carefully dry between the toes.
- Moisturize your feet but not between toes as it can cause fungal infections.
- Cut nails carefully.[13]
- Never treat corns or calluses yourself.
- Wear clean, dry socks and change them daily.
- Wear socks to bed.
- Shake out your shoes and feel the inside before wearing to check for any foreign bodies.
- Keep your feet warm and dry. Consider using an antiperspirant on soles.
- Never walk barefoot.
- Keep blood sugar levels under control.
- Do not smoke.
- Get periodic foot exams.[14]
- Diabetes Complication and Amputation Prevention.
- Shoes and Orthotics for Diabetics
- In a 2009 evidence-based literature review, the authors found that TENS might be effective for pain treatment in diabetic neuropathy.[15]
- The authors of a 2008 control study of 30 neuropathic diabetic patients concluded that as part of the multidisciplinary approach physical therapy plays an important role in the treatment of diabetic neuropathic patients. [16]They used the following adjunct on the treatment group every day for twelve weeks:
- Low level laser irradiation for 10-15 minutes/session on the ulcer
- Laser biostimulation on the peroneal nerve trunk (at the fibula head) at 1000 Hz for 15 minutes
- Specific dorsiflexion and ankle ROM exercises
- Education on foot care and home exercises
Complications[edit | edit source]
- Weak bones
- Deformity: Rocker Bottom
- Toe curls
- Ankle may become twisted and unsteady.
- Bones may press against shoes.[1]
Prognosis[edit | edit source]
All persons with diabetes who have been treated for Charcot foot should have regular foot care with a foot and ankle specialist or a specialist in diabetic foot problems. Close watch should be done on new changes related to Charcot and other diabetic foot complications. Patients who have Charcot foot from other causes also should have regular follow up as recommended by the doctor.[2][6]
References[edit | edit source]
- ↑ 1.0 1.1 Rogers LC, Frykberg RG, Armstrong DG, Boulton AJ, Edmonds M, Van GH, Hartemann A, Game F, Jeffcoate W, Jirkovska A, Jude E. The Charcot foot in diabetes. Journal of the American Podiatric Medical Association. 2011 Sep;101(5):437-46.
- ↑ 2.0 2.1 Jeffcoate W, Lima J, Nobrega L. The charcot foot. Diabetic Medicine. 2000 Apr;17(4):253-8.
- ↑ Kaynak G, Birsel O, Fatih Güven M, Öğüt T. An overview of the Charcot foot pathophysiology. Diabetic foot & ankle. 2013 Jan 1;4(1):21117.
- ↑ FootScientific. What Causes Charcot Foot? Available from: https://www.youtube.com/watch?v=MWhzy9Us3R0 [last accessed 23/3/2021]
- ↑ 5.0 5.1 Sommer T, Lee TH. Charcot foot: the diagnostic dilemma. American Family Physician. 2001 Nov 1;64(9):1591.
- ↑ 6.0 6.1 TYLER FOOT CLINIC. Charcot Foot. Available from: https://www.youtube.com/watch?v=FcoykAh16jk [last accessed 23/3/2021]
- ↑ 7.0 7.1 7.2 7.3 Lepäntaloa M, Apelqvistc J, Setaccie C, Riccof JB, de Donatoe G, Beckerg F, Robert-Ebadig H, Caoh P, Ecksteini HH, De Rangok P, Diehml N. Chapter V: Diabetic Foot. European Journal of Vascular and Endovascular Surgery. 2011;42(S2):S60-74.
- ↑ Pinzur MS, Shields N, Trepman E, Dawson P, Evans A. Current practice patterns in the treatment of Charcot foot. Foot & ankle international. 2000 Nov;21(11):916-20.
- ↑ Pinzur M. Surgical versus accommodative treatment for Charcot arthropathy of the midfoot. Foot & ankle international. 2004 Aug;25(8):545-9.
- ↑ 10.0 10.1 Kalra S, Kalra B, Kumar N. Prevention and management of diabetes: the role of the physiotherapist. Diabetes Voice. 2007;52 (3)
- ↑ 11.0 11.1 Kalra S, Kalra B, Kumar N. Prevention and management of diabetes: the role of the physiotherapist. Diabetes Voice. 2007;52 (3)
- ↑ Reiber GE. Diabetic foot care. Financial implications and practice guidelines. Diabetes care. 1992 Mar 1;15:29-31.
- ↑ Bakker K, Apelqvist J, Schaper NC, International Working Group on the Diabetic Foot Editorial Board. Practical guidelines on the management and prevention of the diabetic foot 2011. Diabetes/metabolism research and reviews. 2012 Feb;28:225-31.
- ↑ Pinzur MS, Slovenkai MP, Trepman E, Shields NN. Guidelines for diabetic foot care: recommendations endorsed by the Diabetes Committee of the American Orthopaedic Foot and Ankle Society.
- ↑ Dubinsky RM, Miyasaki J. Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review) Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology. 2010 Jan 12;74(2):173-6.
- ↑ Zakaria HM, Adel SM, Tantawy SA. The Role of Physical Therapy Intervention in the Management of Diabetic Neuropathic Foot Ulcers. Bull. Fac. Ph. Th. Cairo Univ. 2008 Jul;13(2).