Communication: The Most Potent Tool In The Box
Communication in Medicine[edit | edit source]
Communication is the central cornerstone on which successful medical management is built.[1] Without it, it will be exceedingly difficult or impossible to make diagnoses, devise treatment plans, advise and educate patients and optimally pursue the continuation of care[2]. Conversely, communication errors have been identified as a major factor in adverse events in healthcare,[3] leading to poor outcomes.[4] In fact, according to patients, excellent communication and interpersonal skills rank higher than medical competency in the make-up of a good doctor.[5] In nursing, it has been found that good communication is considered by patients to be “more significant than physical care".[6]
Advantages of Good Clinical Communication[edit | edit source]
Proper communication has shown to improve the quality and efficiency of medical care in various ways. Patient adherence is directly related to good communication: Good quality of transmission and retrieval of clinical and psychosocial information allow for the formation of a detailed patient profile; patients feel supported, involved and empowered to collaborate in decision-making, which per implication facilitates buy-in and compliance to treatment. An environment facilitating good communication creates a safe place for disclosure and discussion, and eventually builds a relationship of trust and respect between the patient and the clinician.[7]
Improved accuracy and effectivity in diagnosis, together with the reduction of costs in unnecessary tests and imaging can save a lot of time and money for both patient and health care provider. From a clinical business perspective, good communication leads to improved patient satisfaction and loyalty, better patient turnover and appointment compliance, word-of-mouth advertising and overall better practice success. There is also a significant correlation between good communication and lower incidences of medical malpractice claims.[8][9][10]
Communication ability is seen as a personality trait, but it is fortunately also a skill that can be learned and refined. Medical schools have placed an increasing amount of emphasis on the teaching of clinical communication in recent years and clinicians are encouraged to engage in post-graduate learning of communication[11]. In medicine, communication occurs between a number of role players and via different media. This includes the physician-patient relationship, communication among doctors in similar and different specialities, interdisciplinary communication, and correspondence between clinician and patient family, to mention a few. For the purpose of this article, the focus will be on physician-patient communication.
The Communication Process[edit | edit source]
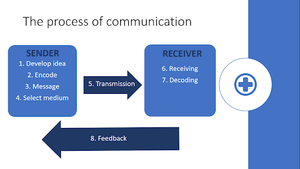
To communicate is to exchange information, according to the Oxford Advanced Learner’s Dictionary. Analysis of the communication process reveals eight steps that occur between a sender and receiver:[12]
SENDER:[edit | edit source]
1. Developing an idea, which will initiate communication
2. Encoding the message, by selecting words, gestures or symbols to convey it with
3. Message formulation, which is the product of encoding. The message can be either/a combination of verbal, non-verbal or written.
4. Selecting a medium through which to transmit the message, such as face-to-face confrontation, a telephone conversation or writing a letter.
5. Transmission of the message
RECEIVER[edit | edit source]
6. Receiving the message
7. Decoding the message into meaningful information
8. Feedback, which is some form of response to the sender; acknowledging receipt and understanding of the message.
Verbal and Non-verbal Communication[edit | edit source]
We distinguish between verbal and non-verbal communication. Verbal communication is performed by using words to create a meaningful message. Non-verbal communication includes aspects such as eye contact, posture, tone of voice, head nods, gestures, and postural position. Interestingly, in cases where verbal and non-verbal messages contradict each other, non-verbal communication tends to outweigh the verbal message. Empathy and emotion are communicated more distinctively via non-verbal communication than verbally, making good non-verbal communication an integral, often overlooked part of the medical interview. Empathy is expressed by acting warm, friendly and reassuring, and has been linked with better patient satisfaction and recovery rates, and subsequently better health outcomes.[10]
Potential Pitfalls in Communication[edit | edit source]
During any conversation, the role of sender and receiver is frequently switched as information is exchanged. Eventually, the aim of communication is to lead to a mutual understanding between the two parties. By being aware of and minimising potential barriers, the communication process and transfer of information can be optimised.
Factors that distort the clear transmission of the message are referred to as noise. Noise is classified according to four factors, namely process barriers, physical barriers, semantic barriers, and psychosocial barriers.[12]
Process barriers occur when any of the eight steps of the communication process becomes disrupted. Blocked steps become barriers in the process. These will now be discussed at the hand of examples:
Sender barrier: A patient fails to disclose critical information because he does not feel it is relevant to his condition and fears being inappropriate.
Encoding barrier: An English-speaking patient struggles to convey her message in French, her second language, to a French-speaking doctor.
Medium barrier: A referring colleague phones to provide a detailed handover of a patient that you will only see in a week’s time, instead of sending a referral letter with the patient.
Decoding barrier: An older doctor does not precisely understand what her millennial patient refers to when he says that he feels “spacey”.
Receiving barrier: During a patient interview, the physician remains preoccupied with a difficult case that he had attended to earlier in the day and is not concentrating on what his patient is saying.
Feedback barrier: Although the patient does not thoroughly grasp the doctor’s explanation, he is too shy to ask the doctor to explain again. Because the patient does not ask any questions, the doctor wrongfully interprets it that the patient fully understands.
Physical barriers are physical objects, people or occurrences that disturb the communication process. Examples can be a phone call or a knock on the door mid-interview.
Semantic barriers refer to the words we choose to use, with a possible difference in meanings or interpretations of words between different people and contexts. An example may be the use of the word “productive” referring to a cough – a patient might interpret it as an effective cough and not necessarily one in which sputum is produced. Using jargon instead of laymen terms is also a typical semantic barrier, and as discussed in the examples above, patients often do not have the confidence to ask for clarity when they do not understand.
Psychosocial barriers encompass three important concepts: Field of experience, filtering and psychosocial distance. Field of experience refers to individual backgrounds, contexts, perceptions, biases, needs and expectations. This can become a barrier when the sender and receiver have very different fields of experience. Filtering is the process by which we focus on and perceive things that we are emotionally centred upon, and is determined by each person’s needs and interests. Filtering becomes a barrier if important information is “filtered out” because of not being included in the receiver’s present viewpoint. Psychosocial distance occurs when the sender and receiver perceive each other on different social levels and act accordingly. A patient may feel that a doctor is talking down to her, for example.
The communication process is a dialogue and it is important for both sender and receiver to optimise all steps of communication. However, as clinicians, the onus rests upon us to take the lead in the facilitation of the medical interview and to guide our patients, in order to gain optimal medical detail and be able to provide them with sufficient feedback. Patient-centred care assists to guide us in this direction.
Patient-Centred Care[edit | edit source]
Patient-centred care embodies “a shift from a traditional, paternalistic, provider-driven and disease-focused approach towards one that fully integrates the patient’s perceptions, needs and experiences, into every phase of medical consultation, treatment and follow-up.”[13] The widely used model by Mead and Bower[14] outlines the five pillars of patient-centred care: Biopsychosocial perspective, patient-as-a-person, sharing power and responsibility, therapeutic alliance and doctor-as-a-person.[14] Patient-centred care can also be formulated as care OF the person (and the totality of his/her health), FOR the person (optimising function and life quality), BY the person (also seeing the clinician as a person who is ethical and competent) WITH the person (in collaboration with the patient).[15]
In physiotherapy, "communication that actively involves the patient is seen as the foundation of patient-centered treatment."[16] Physiotherapy-specific attributes of patient-centred care have been further refined into the following points:[15]
- Individualised treatment, including patient-tailored education, communication and treatment.
- Continuous high-quality communication, including both verbal and non-verbal
- Clearly understandable patient education and advice regarding diagnosis, treatment strategies and the course of treatment
- Patient-defined goal setting
- Patient support and empowerment, with the therapist seeing the patient as a holistic person
- Access to a clinician with good social skills, confidence and proper knowledge in the field, who are able to relate to the patient.
From the above, it is clear that patient-centred care goes hand in hand with proper medical communication, and that the two aspects are, in fact, interdependent for optimal outcomes.
The Aim of Medical Communication[edit | edit source]
The overall goal of medicine is to optimise patient health. The same goal applies to medical communication, and for this reason, it is important to always reflect whether the communication with your patient is continuously contributing toward this greater goal.
The aim of good medical communication is summarised in a 6-function model:[2]
- Fostering the relationship(s) between health care worker(s) and patient/patient family.
- Gathering information from the patient, with the goal of diagnosis and/or interpretation of symptoms.
- Providing information to the patient, with the goal of addressing uncertainties, educating the patient and assisting with the process of informed decision making.
- Decision making in terms of treatment, based on proper information from various sources, and considering patient preferences.
- Facilitate disease-/treatment-related behaviour to optimise health and recovery
- Dealing with emotions and being able to adequately support the patient, enhance the patient-practitioner relationship and knowing when to refer on if applicable.
Where to Start?[edit | edit source]
Visiting a medical professional is often stressful. Apart from the fact that patients may feel physically unwell because of their presenting symptoms, the fear of a potentially serious diagnosis can cause anxiety. Many patients are also worried that they may not communicate their symptoms appropriately or that the doctor will not take their complaints seriously.[17] Pre-consultation stress can be reduced by already providing information prior to the consultation to allow patients to prepare themselves and know what to expect. A website is an ideal way to make such information available, and it can also serve as a booking and direct communication platform.[18] Below are some pointers on what consumers appreciate on medical professional’s website:
- Information on your facility and practice philosophy.
- All services provided at the facility. Include anything that may set you apart or that may be high in demand in your area.
- Information on the practising clinician(s). Include the following:
- Qualifications,
- Specialisations/special interests
- Any extra achievements and credentials (for example presenting at conferences or involvement in research)
- Adding something personal (such as a hobby or family) makes the clinician more relatable and enforces the idea of doctor-as-a-person as outlined in patient-centred practice. Also, include a photograph of the clinician if possible.
- Provide some information on what the patient can expect from the first consultation and follow-up consultations. Include your appointment lengths (and remain within the time limits).
- A map and clear direction to your facility.
- Contact details and office hours.
- Consider providing patients with the option to fill out their patient information online to be more time-efficient on the day of consultation. Acknowledgement to office policies and informed consent can also be signed online.
- Payment options should be provided beforehand. Make sure to mention whether the practice claims directly from medical insurance.
- Basic health questionnaires or specific outcome measure tools can be made available for patient completion prior to the first consultation.
Conclusion[edit | edit source]
The importance of proper communication in the medical field cannot be overstated. Sound clinician-patient communication establishes a solid relationship and leads to better medical outcomes altogether. Communication is not merely talking and listening – it involves complicated processes from the formulation of an idea by the sender to the acknowledgement of the message by the receiver. By being aware of potential barriers in communication, we can try to steer clear of them, or recognise and fix them as we go along. Empathy and patient-centredness assists to truly understand what your patient is trying to communicate. Provision of basic information prior to the first consultation already assists in decreasing patient anxiety and initiating a clinician-patient relationship.
References[edit | edit source]
- ↑ Chang DS, Chen WL, Wang R. Impact of the bidirectional relationship between communication and cognitive efficacy on orthopedic patient adherence behavior. BMC Health Serv Res. 2022 Feb 14;22(1):199.
- ↑ 2.0 2.1 de Haes, H., Bensing, J., 2009. Endpoints in medical communication research, proposing a framework of functions and outcomes. Patient Educ. Couns., Theories in Health Communication Research 74, 287–294.
- ↑ Guttman OT, Lazzara EH, Keebler JR, Webster KLW, Gisick LM, Baker AL. Dissecting communication barriers in healthcare: a path to enhancing communication resiliency, reliability, and patient safety. J Patient Saf. 2021 Dec 1;17(8):e1465-e1471.
- ↑ Morrison AK, Gibson C, Higgins C, Gutzeit M. Health literacy-related safety events: a qualitative study of health literacy failures in patient safety events. Pediatr Qual Saf. 2021 Jun 23;6(4):e425.
- ↑ Steiner-Hofbauer, V., Schrank, B., Holzinger, A., 2018. What is a good doctor? Wien. Med. Wochenschr. 168, 398–405.
- ↑ Kwame A, Petrucka PM. A literature-based study of patient-centered care and communication in nurse-patient interactions: barriers, facilitators, and the way forward. BMC Nurs. 2021 Sep 3;20(1):158.
- ↑ Haskard Zolnierek, K.B., DiMatteo, M.R., 2009. Physician Communication and Patient Adherence to Treatment: A Meta-analysis. Med. Care 47, 826–834.
- ↑ Kee, J.W.Y., Khoo, H.S., Lim, I., Koh, M.Y.H., 2018. Communication Skills in Patient-Doctor Interactions: Learning from Patient Complaints. Health Prof. Educ. 4, 97–106.
- ↑ Kuehl, S.P., 2011. Communication Tools for the Modern Doctor Bag. Physician Patient Communication Part 1: Beginning of a medical interview. J. Community Hosp. Intern. Med. Perspect. 1, 8428.
- ↑ 10.0 10.1 Vogel, D., Meyer, M., Harendza, S., 2018. Verbal and non-verbal communication skills including empathy during history taking of undergraduate medical students. BMC Med. Educ. 18, 157.
- ↑ Kurtz, S., Silverman, J., Benson, J., Draper, J., 2003. Marrying Content and Process in Clinical Method Teaching: Enhancing the Calgary–Cambridge Guides. Acad. Med. 78, 802–809.
- ↑ 12.0 12.1 Lunenburg, F.C., 2010. Communication: The Process, Barriers, And Improving Effectiveness. Schooling 1(1) 1-11.
- ↑ Fix GM, VanDeusen Lukas C, Bolton RE, Hill JN, Mueller N, LaVela SL, Bokhour BG. Patient‐centred care is a way of doing things: How healthcare employees conceptualize patient‐centred care. Health Expectations. 2018 Feb;21(1):300-7.
- ↑ 14.0 14.1 Mead, N., Bower, P., 2000. Patient-centredness: a conceptual framework and review of the empirical literature. Soc. Sci. Med. 51, 1087–1110.
- ↑ 15.0 15.1 Wijma, A.J., Bletterman, A.N., Clark, J.R., Vervoort, S.C.J.M., Beetsma, A., Keizer, D., Nijs, J., Wilgen, C.P.V., 2017. Patient-centeredness in physiotherapy: What does it entail? A systematic review of qualitative studies. Physiother. Theory Pract. 33, 825–840.
- ↑ Ahlsen B, Nilsen AB. Getting in touch: Communication in physical therapy practice and the multiple functions of language. Front Rehabil Sci. 2022 Aug 4;3:882099.
- ↑ Bensing, J.M., Verheul, W., Dulmen, A.M. van, 2008. Patient anxiety in the medical encounter: A study of verbal and nonverbal communication in general practice [WWW Document].
- ↑ Sanchez, M.H., Sanchez, P.M., 2011. Evidence on the Content of Physician Websites (SSRN Scholarly Paper No. ID 1874220). Social Science Research Network, Rochester, NY.