Double Crush Syndrome
Original Editor - Venus Pagare
Top Contributors - Venus Pagare, Lucinda hampton, Syeda Bushra Zehra Zaidi, Kim Jackson and Amanda Ager
Introduction[edit | edit source]
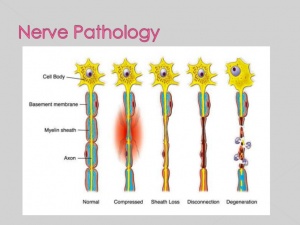
The double crush hypothesis was first formulated in 1973 and states that axons that have been compressed at one site become especially susceptible to damage at another site.[1]
This theory was originally described by Upton (1973) in a study of 115 patients. A comprehensive electromyographic study of 115 patients with carpal-tunnel syndromes or lesions of the ulnar nerve at the elbow was done. In 81 cases there was electrophysiological evidence, often supported by clinical symptoms, of associated neural lesions in the neck. This association was not thought to be fortuitous, but rather the result of serial constraints of axoplasmic flow in nerve fibres.[1]
The existence of double crush syndrome was further substantiated by Massey's (1981) study of nineteen cases of carpal tunnel syndrome co-existing with a cervical radiculopathy. [2]
Hypothesis[edit | edit source]
- It is suggested that compression of an axon at one location makes it more sensitive to effects of compression in another location,because of impaired axoplasmic flow.
- Hypothetically, two lesions with little or no independent clinical ramifications, when combined, lead to appearance or magnification of symptoms
- Two areas of compression affecting the same axons do not, alone, meet the criteria of the hypothesis.
- By definition, a first lesion must render axons more susceptible to effects of a second, leading to more than just the combined, independent effects of two lesions
- Upton and McComas used the double crush hypothesis to explain why patients with carpal tun-nel syndrome (CTS) sometimes feel pain in the forearm, elbow, upper arm, shoulder, chest, and upper back.
- They also used it to explain failed attempts at surgical repairs when neither surgery nor CTS diagnosis appeared faulty.
- They claimed that most patients with CTS not only have compressive lesions at the wrist, but also show evidence of damage to cervical nerve roots.
- Upton and McComas further suggested that a high proportion (75%) of patients with one peripheral nerve lesion did in fact have a second lesion elsewhere and they implied that both lesions were contributing to the symptoms.[3]
Physiotherapy treatment[edit | edit source]
Needs to be tailored to specific client and progressed as appropriate. Treatment may include all or some of the below.
- Education and rest from aggravating activities. The need to explain fully to the client why it is important to address: use of night splints if warranted; postural issues: cervical spine alignment; nerve and muscle lengths; muscle strength.
- Postural advice and training
- Cervical spine and carpal bone mobilisation
- Flossing of appropriate nerve(s)
- Stetching of involved upper limb muscles and soft tissue
- strengthening affected hand and upper limb muscles
- Fine and gross hand motor skills[4]
Additional Information[edit | edit source]
Evidence[edit | edit source]
- Experimental research by Nemoto et al., found evidence for double crush syndrome and concluded that two low grade compressions along a nerve are worse than either alone.
- In a study of 1,000 patients with carpal tunnel syndrome, Hurst et al., found a statistically significant incidence of bilateral carpal tunnel syndrome in patients with cervical spondylosis. They also found a relationship between diabetic neuropathy and this type of nerve entrapment phenomenon.
- In an EMG study, Raps found patients with cervical radiculopathy to be predisposed to a second lesion along the route of the same nerve, and suggested that double crush syndrome is a true entity.
- In a study by Osteman et al., it was concluded that double crush syndrome should be suspected in older age female patients who also have paresthesia, and grip strength weakness associated with distal prolonged sensory latencies on NCV studies.
- Thoracic outlet syndrome (TOS) is often seen and associated with double crush syndrome as well. In a paper by Naralcas, they found that the proximal neuropathy usually precedes the distal one. They found a high prevalence of TOS associated with carpal tunnel syndrome in 40 cases, TOS associated with ulnar neuropathy in 19 cases, and TOS associated with radial tunnel syndrome in 29 cases.
Other studies:
- 1000 hands in 888 patients – 11 felt to have double crush (1%) (Carroll 1982) [7]
- 100 clinically diagnosed CTS patients – 6% thought to have double crush (Kuntzer 1994) [8]
- Double crush in 0.7% of 12736 patients (Morgan 1998) [9]
- 40 of 271 patients with thoracic outlet syndrome felt to have CTS too (Narakas 1990) [10]
- 37 of 1183 patients with CTS found to have cervical radiculopathy (3.1%) (Wilbourn 1986) [11]
- 74 of 165 cases of thoracic outlet syndrome found to have a peripheral entrapment neuropathy (44%) (Wood 1990) [12]
- Evidence of double crush found in 74 limbs out of 758 in 681 patients with thoracic outlet syndrome (9.76%) (Abe 1999) [13]
- Of 525 patients with CTS 105 (20%) had other entrapments in the same limb (Yu 1979) [14]
References[edit | edit source]
- ↑ 1.0 1.1 Phan A, Shah S, Hammert W, Mesfin A. Double crush syndrome of the upper extremity. JBJS reviews. 2021 Dec 1;9(12):e21.
- ↑ Hurst LC, Weissberg D, Carroll RE. The relationship of the double crush to carpal tunnel syndrome (an analysis of 1,000 cases of carpal tunnel syndrome). The Journal of Hand Surgery: British & European Volume. 1985 Jun 1;10(2):202-4.
- ↑ Russell BS. Carpal tunnel syndrome and the. Chiropractic & osteopathy. 2008 Dec;16(1):1-9.
- ↑ PhysioWorks. Carpal Tunnel Syndrome. Available from: https://physioworks.com.au/injuries-conditions-1/carpal-tunnel-syndrome (last accessed 7.3.2019)
- ↑ Institute of sports and spines. Median nerve flossing. Available from: https://www.youtube.com/watch?v=wO07PxKLx8o (last accessed 7.3.2019)
- ↑ Physical therapy Video. Double Crush Carpal Tunnel Syndrome. Available from:https://www.youtube.com/watch?v=bysNNLEnNCU (last accessed 7.3.2019)
- ↑ Carroll RE, Hurst LC. The relationship of the thoracic outlet syndrome and carpal tunnel syndrome. Clin Orthop 1982;164:149-53.
- ↑ Kuntzer T. Carpal tunnel syndrome in 100 patients: sensitivity, specificity of multi-neurophysiological procedures and estimation of axonal loss of motor, sensory and sympathetic nerve fibres. J Neurol Sci 1994;127:221-29.
- ↑ Morgan G, Wilbourn AJ. Cervical radiculopathy and coexisting distal entrapment neuropathies: double-crush syndromes? Neurology 1998;50(1):78-83.
- ↑ Narakas AO. The role of thoracic outlet syndrome in the double crush syndrome. Ann Hand Surg 1990;9(5):331-40.
- ↑ Wilbourn AJ, Breuer AC. The double crush syndrome: a reappraisal (abstract). Neurology 1986;36(suppl 1):234-35.
- ↑ Wood VE, Bioni J. Double-crush nerve compression in thoracic-outlet syndrome. J Bone Joint Surg 1990;72A:85-88.
- ↑ Abe M, Ichinohe K, Nishida J. Diagnosis, treatment, and complications of thoracic outlet syndrome. J Orthop Sci 1999;4(1):66-69.
- ↑ Yu J, Bendler EM, Mentari A. Neurological disorders associated with carpal tunnel syndrome. Electromyogr Clin Neurophysiol 1979;19:27-32.