Falls and Traumatic Brain Injury
Original Editor - Anna Ziemer
Top Contributors - Naomi O'Reilly, Kim Jackson, Tarina van der Stockt, Lucinda hampton, Rachael Lowe, Lauren Lopez, Admin and Simisola Ajeyalemi
Introduction[edit | edit source]
We are witnessing the populations across the world ageing dynamically. The Great Britain older people population is increasing (according to ONS in 2018 one in 5 was 65 or over when by 2050 one in four people will be 65 or over). Due to the advances in emergency medicine, intensive care and neuro-rehabilitation we are also witnessing the increase in the population of people leaving with acquired brain injury.
A Fall is as an event which results in a person coming to rest inadvertently on the ground or floor or other lower level. Fall-related injuries are mostly non-fatal but can also be fatal.[1] Falls tie age with traumatic brain injury in a two-way relationship:
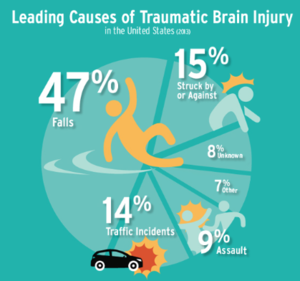
- Falls are the leading cause of the traumatic brain injury in children and older adults, with the greatest incidence in 83-90 years old. Falls are also the second leading cause of death related to accidental or unintentional injury worldwide. One out of five falls causes a serious injury such as broken bones or a head injury, where approximately three quarters require hospital admission. The cost of falls for the British National Health Service is approximately £4.6 million a day! Mortality in older adults following traumatic brain injury is significantly increased. Older adults represent approximately 10% of all the population of patients with traumatic brain injury, however, they represent 50% of traumatic brain injury-related deaths (Eapen at al 2018).
- Traumatic brain injury causes complex and often multi-system impairment and requires multifaceted therapeutic intervention. Moreover, the rehabilitation itself exposes traumatic brain injury survivors to greater risk of falls. Therefore, the risk and occurrence of falls in this population and settings is much greater and the majority of individuals with traumatic brain injury will be at increased risk of falls.
Risks of Falls and Contributing Factors[edit | edit source]
- Age: The most susceptible groups for falls are people 65 years and older with the highest risk of serious head injury, in children under 15 when combined with insufficient supervision from an adult. Older adults who hit their head due to fall are more likely to have brain injury due to age related changes in brain structure and circulation as well as medication taken like blood thinners. The below video gives some statistics and overview of kids and TBI.
- History of Fall: Half of people who fall will fall again in the next 12 months.
- Fear of Falling: May relate to being cognitively preoccupied (anxious and impacting attention) and use of cognitive reserve, which would mimic dual tasking conditions. Fear of falling causes reducing activity level.
- Muscle Changes: decreased strength; altered tone and flexibility;
- Altered Balance: Impaired balance results in gradual withdrawal behaviour from more complex activities like community mobility or playing sports, and adjustment of execution of some tasks eg using trolleys to carry a drink.
- Polypharmacy: 4 or more prescribed medications significantly increases the risk of falls
- Visual Deficits or Visuo-Spatial Disturbances
- Vestibular Disorder e.g. BBPV, Labyrinthine Concussion (Sensorineural hearing loss with or without vestibular symptoms occurring after head trauma [2])
- Cognitive Deficits: Can manifest as slow processing; impaired executive functions; attention deficits; inability to dual task/multitask. 2 out of 3 individuals with dementia or cognitive impairment are statistically likely to fall each year.
- Low Mood and Related Medication
- Incontinence
- Chronic Condition e.g Traumatic Brain Injury, Stroke, Multiple Sclerosis (MS), Dementia
- Short Term Factors e.g medication side effects, alcohol intake
- Activity Related e.g walking, stairs climbing,
- Environmental Factors e.g light poor lighting, bad kitchen organisation, carpets and rugs, clothing and footwear
This means that physical and cognitive falls risk factors overlap strongly with traumatic brain injury sequels often resulting in survivors of traumatic brain injury being at greater risk of falling than the general population. The risk is not clearly age related and people with traumatic brain injury are at risk of falls at any age. Approximately 30-65% of survivors of traumatic brain injury report disequilibrium or dizziness in sitting or standing, which affect activities of daily living and mobility. The severity of the problems depends on the severity of the traumatic brain injury, the location of the injury, other injuries or comorbidities and medication related to the traumatic brain injury.
It needs to be noted that Rehabilitation itself imposed increased falls risks and there is a trend of falls in neurorehabilitation settings during active times. [3] Physiotherapists should regularly reassess the risk of falls in patients with traumatic brain injury as the change in them is not linear with the recovery time either general outcomes.
Prevention and Treatment[edit | edit source]
The preventative activities should be multifactorial. They should aim to reduce number of falls or severity of falls related injuries if they occur. According to the World Health Organisation, [1] the elements to include in programmes preventing falls are:
- Motor-cognitive falls interventions for people with falls risks, fear of falling or history of falls
- Education strategies rising awareness about falls risk and prevention
- Creating safer environments
- Training health care professionals about falls risk, burden and prevention.
Multifactorial interventions with emphasis on behavioural change impacting the lifestyle choices and addressing environmental factors are deemed to have the highest effectiveness. [4][5] There is a strong belief these interventions should be long term and contain at least 50 hours of exercises over a 6 month period. Where balance and mobility outcome measures like the Berg Balance Scale or Timed Up and Go highlight balance and mobility impairments for people with traumatic brain injury, they should continue working on prevention of falls and have access to professional advice and interventions upon discharge from Neurorehabilitation Services.[6]
Multiple and complex traumatic brain injury sequel are often overlapping with impairment contributing to falls risk
- Weakness
- Reduced joints mobility
- Slow processing speed
- Inability to complete complex tasks
- Cognitive impairment
The multifactorial preventative and reactive approaches should:
- Encourage patients to share information about their falls with General Practitioners or Physiotherapist. Professionals to obtain and store the data to establish patients at risk
- Contain education about fear of falling impact on daily activity level and participation as well as developing coping strategies like building confidence through practice of on / off the floor transfers, rolling and crawling on the floor, exposing to near falls with developing the sensory memory about initial stages of falls and learning how to react to avoid fall
- Build progressive, optimally challenging exercise-based programmes addressing strength, flexibility, agility and balance systems training
- Contain vestibular, visual, proprioceptive demand during exercise training using scanning, head movements, eyes closed/open, even/uneven base of support, etc.
- Include dual tasking demands using additional motor or/and cognitive tasks, increasing complexity and speed of practice
- Including cognitive-motor tasks enhancing thinking related to mobility and balance using tools like dance mat, “Clock Yourself App”
- Contain medication review every 12 months against accumulative side effects and further need of use of particular medication
- Include regular vision assessment and promotion of habits like cleaning glasses daily
- Contain vestibular assessment and treatment when required
- Include psychological and emotional wellbeing review and treatment based not only on pharmacological agents
- Include regular continence review when required
- Include environment and personal choices review and advice about lighting, kitchen or bathroom organisation, decluttering, marking stairs, avoiding carpets or rugs, choosing stable supportive footwear, comfortable but neat clothing of right length, animal keeping, etc.
Various balance components should be integrated into balance retraining exercise programmes:
- Postural alignment, body mechanics, and static postural control including midline orientation (steady stance)
- Dynamic postural control, including musculoskeletal responses necessary for control of movement and posture including strength, flexibility and ability to make effective anticipatory postural adjustment prior to voluntary movements (pro-active and reactive balance components to address various tasks’ attributes requiring stability, mobility or skills)
- Balance skills and balance reactions repertoire for various task and environmental conditions like ankle, hip, stepping strategies
- Mobility training
- Use of sensory monitoring for postural control (visual, vestibular, proprioceptive)
- Cognitive skills training with evidence emerging that cognitive-motor tasks combined have the greatest effectiveness [7]
The training to be efficient needs to meet individual person’s needs and be designed at optimal level of challenge balance components without compromising safety. Working in a comfort zone, i.e.: using a chair-based exercises programme only is not going to address balance either reduce the falls risk. Equally, working only on one balance components, i.e.: strength is not going to address the complexity of balance.
Use of various postural sets and techniques like rhythmic stabilisation or stabilising reversal, even versus uneven base of support like balance pads, reduced base of support like feet together, tandem standing/walking, 1 legged standing, use of head and upper limbs movements, complexity of tasks like dual tasking with cognitive or additional physical element can be used to tailor the programme to individual’s goal.
Falls Programmes[edit | edit source]
There are well research programmes for falls prevention and mobility and balance retraining, which were designed for other patients population like stroke survivors or elderly, however their principles and routine can be applied successfully in falls prevention after TBI:
Otago Exercise Programme is an evidenced-based, "home-based, individually tailored strength and balance retraining programme” which is carried out by physiotherapists and/or trained providers such as community nurses. It is designed to be carried out over 12 months (or more recently, six months). You can access the OTAGO Manual here or there is now an Otago APP available on Google Apps.
Fitness And Mobility Exercise Program (FAME) developed at the University of British Columbia by Professor Janice Eng’s Team with easy accessible resources, which can be used on electronic devices or printed. While the purpose of the FAME Program is to optimise the physical ability of people living with a stroke and to minimise the risk of secondary complications such as falls, fractures and heart disease, much of the programme can be implemented by those with traumatic brain injury. The FAME Program was developed to address multiple domains, including balance, muscle strength, bone health, mobility, cardiovascular fitness and depression.
Falls Management Exercise (FaME) is an exercise programme that has been shown to improve strength, stability and confidence in balance developed by Later Life Training and Professor Dawn Skelton in UK. This toolkit, for the Falls Management Exercise (FaME) programme, has been developed from falls programmes that were effective and had high programme fidelity when commissioned routinely by public sector services. You can download the Implementation Kit here.
References[edit | edit source]
- ↑ 1.0 1.1 WHO. Falls Factsheet Available from: https://www.who.int/en/news-room/fact-sheets/detail/falls (last accessed 03/09/2019)
- ↑ Villarreal IM, Méndez D, Silva JM, Álamo P. Contralateral cochlear labyrinthine concussion without temporal bone fracture: unusual posttraumatic consequence. Case reports in otolaryngology. 2016;2016. Available from: https://www.hindawi.com/journals/criot/2016/2123182/ (last accessed 20.10.2019)
- ↑ McKechnie D, Pryor J, Fisher MJ. Falls and fallers in traumatic brain injury (TBI) rehabilitation settings: an integrative review. Disability and Rehabilitation. 2015;37:24: 2291-2299, DOI:10.3109/09638288.2014.1002578
- ↑ Sherrington C, Michaleff ZA, Fairhall N, et al. Exercise to prevent falls in older adults: an updated meta-analysis and best practice recommendations. NSW Public Health Bulletin. 2011 22(4) 78-83.
- ↑ A, Gruber W, Baldwin M, Liao S. The effect of multidimensional exercises on balance, mobility, and fall risk in community-dwelling older adults. Phys Ther. 1997 Jan;77(1):46-57.
- ↑ Klima D, Morgan L, Baylor M, Reilly C, Gladmon D, Davey A. Physical Performance and Fall Risk in Persons With Traumatic Brain Injury. Perceptual and Motor Skills. 2019;126(1):50-69. doi: 10.1177/0031512518809203. Epub 2018 Nov 20.
- ↑ Sturnieks DL, Menant J, Valenzuela M, et al Effect of cognitive-only and cognitive-motor training on preventing falls in community-dwelling older people: protocol for the smart±step randomised controlled trial. BMJ Open 2019;9:e029409. doi: 10.1136/bmjopen-2019-029409