Femoroacetabular Impingement
Original Editor - Douglas Wix
Top Contributors - Laura Ritchie, Ewa Jaraczewska, Admin, Kim Jackson, Margaret Chislett, Lucinda hampton, Rachael Lowe, Douglas Wix, Johnathan Fahrner, Jess Bell, Anas Mohamed, Stacy Schiurring, Rishika Babburu, Kai A. Sigel, WikiSysop and Wanda van Niekerk
Introduction[edit | edit source]
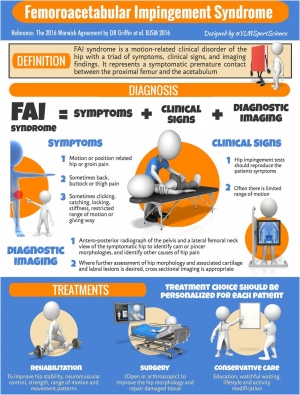
Femoroacetabular impingement (FAI) syndrome is a motion-related clinical disorder of the hip involving premature contact between the acetabulum and the proximal femur, which results in particular symptoms, clinical signs and imaging findings.[1][2] Degenerative changes and osteoarthritis may develop in the long-term as a result of this abnormal contact.[3]
Clinically Relevant Anatomy[edit | edit source]
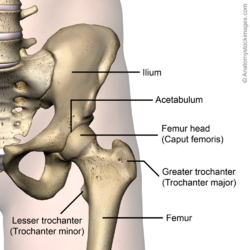
The hip (acetabulofemoral joint) is a synovial joint formed between the femur and acetabulum of the pelvis. The head of the femur is covered by Type II collagen (hyaline cartilage) and proteoglycan. The acetabulum is the concave portion of the ball and socket joint. The acetabulum has a ring of fibrocartilage called the labrum that deepens the acetabulum and improves the stability of the hip joint. A detailed review of the anatomy of the hip is available here.
Mechanism of Injury / Pathological Process[edit | edit source]
FAI syndrome is associated with three variations in the morphology of the hip joint: cam, pincer and the combination of cam and pincer.[4][5] These morphologies are thought to be fairly common (around 30% of the general population),[6] including in people without hip symptoms. Raveendran et al.[7] found that 25% of men and 10% of women had evidence of cam morphology in at least one hip while 6-7% of men and 10% of women demonstrated pincer morphology. Thus, the isolated presence of either cam or pincer morphology is insufficient for a diagnosis of FAI syndrome.[2]
- Cam morphology describes a flattening or convexity of the femoral head-neck junction.[2] This morphology is more common in young, athletic men.[3][7]
- Pincer morphology describes "overcoverage" of the femoral head by the acetabulum in which the acetabular rim is extended beyond the typical amount, either in one focal area or more generally across the acetabular rim.[2] This morphology is more common in women.[3][7]
- The population with a combination of cam and pincer often suffer from a slipped capital femoral epiphysis called the S C F E. They show varying degrees of hip impingement. An estimated 85% of patients with FAI have this type of mixed morphology, [3]although Raveendran et al.[7] found only 2% of subjects in their prospective longitudinal cohort study had mixed morphology (albeit in a primarily middle-aged population).[7]
Cam and pincer morphology can lead to damage of the articular cartilage and the labrum due to impingement between the acetabular rim and the femoral head during movement, which causes the symptoms of FAI syndrome.[10] Metabolic analysis of tissue samples by Chinzei et al.[10] suggested that articular cartilage may be the main site of inflammation and degeneration in hips with FAI and that if OA progresses, metabolic activity spreads to the labrum and synovium and labrum.
Given that both types of morphologies can be present in asymptomatic individuals, Casartelli et al.[11] propose that other factors out with the bony structures may be involved with FAI syndrome including:
- Weakness of the deep hip muscles which compromises hip stability and leads to an overload of secondary movers of the hip. The femoral head glides anteriorly into the acetabulum and increases joint loading.[11]
- Repeated loading of the labrum leads to upregulation of nociceptive receptors in that structure through the production of neurotransmitters such as substance P.[11]
Etiology[edit | edit source]
Based on a systematic review performed by Chaudhry and Ayeni,[3] the aetiology of FAI syndrome is likely multifactorial. Further research is required to better understand the development of the FAI-associated morphologies, but the following factors may be associated with its development:[3]
- Intrinsic factors supported by:
- Radiological findings of FAI-associated morphologies among subjects with affected siblings
- Higher instances of cam morphology in men and pincer morphology in women
- Exposure to repetitive and often supraphysiologic hip rotation and hip flexion during development in childhood and adolescence (e.g. hockey, basketball or football). The repeated stress of this type may trigger adaptive remodelling and eventually the development of FAI-associated morphologies and symptoms
- History of childhood hip disease (e.g. slipped capital femoral epiphysis (SCFE) or Legge-Calve-Perthes disease) which may have altered the shape of the femoral head
- Malunion following femoral neck fractures which may have altered the contour of the femoral head/neck
- Surgical over-correction of conditions such as hip dysplasia may lead to the pincer morphology
Clinical Presentation[edit | edit source]
Heterogeneity of diagnostic criteria in past research has meant that it has been difficult to ascertain the full scope of physical impairments stemming from FAI.[12] However, pain from FAI is commonly held to be aggravated with acceleration sports as well as squatting, climbing stairs and prolonged sitting.[13] With FAI that may have advanced to hip osteoarthritis, signs and symptoms more typical of this condition may be identified.
In the Warwick Agreement on FAI syndrome published in 2016, the authors noted that a particular triad of symptoms, clinical findings and imaging findings are required for a diagnosis of FAI.[2]
Symptoms[edit | edit source]
The primary symptoms reported with this condition are:
- Moderate to marked hip or groin pain related to certain movements or positions[2]
- Pain reported in the thigh, back or buttock[2][14]
- Stiffness
- Restricted hip range of motion
- Clicking and/or catching
- Locking or giving way [2][14]
- Decreased ability to perform activities of daily living and sports.[15]
Clinical Findings[edit | edit source]
As per the Warwick Agreement from 2016, there is no single clinical sign that will indicate a diagnosis of FAI.[2] Issues with low specificity of tests such as the impingement test (FADIR) limit their accuracy and usage as stand-alone tests.[16] [17] As a consequence, false positives, inaccurate diagnosis of FAI syndrome and incorrect treatment may occur.[16] Smithson[16] suggests that a cluster of tests could be studied to develop a clinical prediction rule to achieve both high specificity and sensitivity and thus a more accurate diagnosis in a clinical setting.
- Various pain-provocation hip impingement tests are used clinically. The most commonly used test is flexion adduction internal rotation (FADIR), but it is not specific.[2][18] The FADIR position of provocation is associated with impingement at the anterior rim of the acetabulum.[14] Pain associated with the posterior rim can be provoked by passively bringing the hip from flexion to extension while maintaining a position of hip abduction and external rotation with the leg hanging off the examination table.[14]
- Hip range of motion is often restricted, most commonly internal rotation with the hip flexed.[2] However, Diamond et al.[12] noted that in some studies, controls were not imaged for asymptomatic FAI. Thus, caution is needed with generalising these results and further research will help clarify the impact of FAI on hip range of motion.[12]
- The single limb squat can help to identify hip abductor weakness.[14]
- Reproduction of pain with hip flexion could indicate FAI or other intra-articular pathology.[14]
- Assessing stair ascending and descending as this requires greater hip flexion than walking on a flat surface.[14]
- Findings of strength deficits associated with FAI have been reported in the literature (particularly hip flexion and adduction) but as with studies investigating range of motion and FAI, some controls were not imaged for asymptomatic FAI, so caution is needed with generalising these results.[12] Further research will help clarify the impact of FAI on strength, particularly at functional as opposed to maximal levels of muscle contraction.[12]
You can find an overview of the clinical evaluation of the Femoroacetabular Impingement here.
Imaging Findings[edit | edit source]
- AP x-rays of the pelvis and lateral x-rays of the femoral neck are recommended initially for suspected FAI syndrome. These views can provide general information relating to the hips, as well as specific information related to cam or pincer morphologies or other potential sources of the patient's pain.[2]
- Dunn lateral view shows the deformity present on the anterolateral side
- Frog-leg position shows the deformity present on the anterior side.[20]
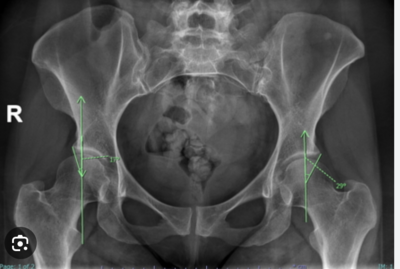
Alpha angle is a radiological measurement for the evaluation of cam morphology. This angle's horizontal line is drawn from the centre of the head of the femur towards the base of the neck of the femur and the vertical line is drawn along the edge of the socket, matching the centre of the femur.[20] Most recently a value of ≥60° has been proposed as a definition of cam morphology.[21]
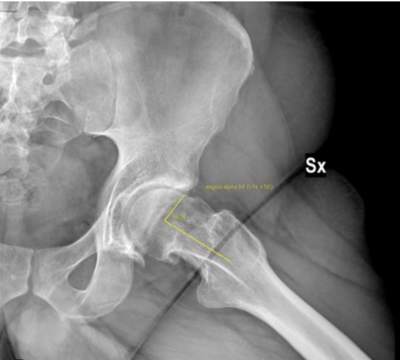
; rID:68548 ]
The lateral centre-edge angle (LCEA) measures femoral head bony coverage by the acetabulum. First the best fit circle for the inferior and medial margins of femoral head is drawn. Next, the angle between two lines drawn from the centre of the circle is measured: one line runs vertically along the longitudinal axis of the pelvis and the other line runs to the lateral acetabular rim.[20] LCEA greater than 39 degrees defines pincer type impingement vs. LCEA less than 20 degrees indicate acetabular dysplasia.[22]
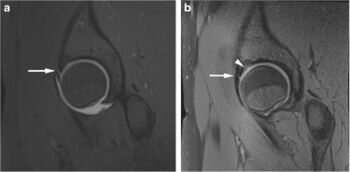
- If further assessment is required (e.g. for better appreciation of 3D morphology of the hip or for associated cartilage and labral lesions), cross-sectional imaging (CT or MR arthrogram) is recommended.[2]
- MR arthrogram has typically been preferred over MRI because it has shown greater accuracy in identifying defects in the labrum and cartilage.[23] However, more recent research suggests that 3T MRI is at least equivalent to 1.5T MRA for detecting these types of defects.[23]
The role of advanced imaging for the diagnosis of FAI syndrome is somewhat controversial:
- Reiman et al.[24] report that in the studies included in their systematic review, patients had such high pre-test probabilities of FAI that advanced imaging would do little to improve on the probability of that diagnosis.
- Cunningham et al.[25] found that advanced imaging (MRA or MRI) was never a cost-effective adjunct to a thorough history and physical examination for diagnosing FAI.
- Supplementing history and physical examination with diagnostic injection may be of value for general practitioners, but is of equivocal benefit for specialists with a higher prevalence of FAI in their patient populations and with more sensitive physical examination skills.[24]
- Kaya[26] proposed and tested a method of assessing contact pressure within the hip during flexion for cam morphologies. Because this measurement is done using a fibre-optic transducer during arthroscopic surgery, the diagnosis of FAI will already be made before this point. It is suggested, however, that this intra-articular measurement will be helpful for:[26]
- Providing a more detailed assessment of cam morphologies and associated pathophysiology
- Establishing an intraoperative index for the proper area and depth of corrective trimming of bone.
A video of this arthroscopic procedure can be viewed near the end of Kaya's[26] open access article here.
Differential Diagnosis[edit | edit source]
Acute hip pain red flag conditions include:
- Tumour
- Infection
- Septic arthritis
- Osteomyelitis
- Fracture
- Avascular necrosis[27]
In athletes, other causes of hip pain include inguinal pathology, adductor pathology and athletic pubalgia.[14]
Outcome Measures[edit | edit source]
- International Hip Outcome Tool (iHOT)
- Hip and Groin Outcome Score (HAGOS)
- Hip Outcome Score (HOS)
- Harris Hip Score (HHS)[28]
- Non-arthritic Hip Score[28]
Management / Interventions[edit | edit source]
"There is currently no high-level evidence to support the choice of a definitive treatment for FAI syndrome."[2]
Researchers are still trying to ascertain the best approach to managing this condition:
- Hip arthroscopy has been a common procedure, but has showed only short-term benefits.[7][18][29][30]
- Peters et al.[31] found heterogeneity in the surgical criteria reported in the literature questioning whether the same condition was in fact being treated in all studies. Only 56% of the reviewed studies included at least one surgical criterion from each of the three categories recommended in the Warwick Agreement.[31]
- The vast majority of the studies (92%) in this scoping review included diagnostic imaging as a criterion, yet there is currently no consensus on specific imaging modalities or cut-off values to determine when surgery is indicated.[31]
- Failed conservative treatment was found to be an infrequent surgical criterion in this review.[31]
- The issue of heterogeneity of diagnostic and surgical criteria in the research has been raised by multiple authors.[12][18][24]
- Reiman and Thorburg[18] likened the rapid increase in surgical correction for FAI to the rise in shoulder arthroscopies between 2000 and 2010 which was not based on quality evidence.
Surgical Management[edit | edit source]
Arthroscopy is the most common surgical procedure for FAI discussed in the literature and typically involves:
- Acetabuloplasty (trimming and reshaping the acetabular rim)
- Labral repair/debridement
- And/or femoroplasty (reshaping the femoral head-neck junction).[30]
- A systematic review by Diamond et al.[12] found that hip arthroscopy for FAI appears to improve range of motion in the sagittal plane, but not the frontal plane during gait. In addition, limitations in hip range of motion during stair climbing did not improve following surgical correction of morphological findings, leading the authors to suggest that hip function in the sagittal and transverse planes may not resolve spontaneously following surgery and that patients may require post-operative training in order to regain normal functional range of motion.[12]
- In a systematic review published in 2017, a complication rate of 3.3% was calculated from hip arthroscopies reported in English literature.[33] Potential complications from surgical management include the following:
- Neuropraxia[33]
- Chrondral injury[33]
- Labral injury[33]
- Heterotopic ossification[33]
- Compression injuries e.g. pudendal nerve, scrotum, labia major[33]
- Injury to the femoral head[33]
- Adhesion[18][33]
- Infection[33]
- DVT[18][33]
- CRPS[18][33]
- Perineal skin damage[33]
- Vascular injury (haematoma)[33]
- Muscle pain[33]
- Incomplete reshaping[33]
- Femoral neck fracture[33]
- Hip instability[33]
- Iliopsoas tendinitis[33]
- Avascular necrosis of femoral head[33]
- Ankle pain[33]
- Bursitis[33]
Surgical complications are a recommended area of future research to help inform the clinical decision-making process.[18]
Surgery with a Post-Operative Physiotherapy Programme[edit | edit source]
A physiotherapist-prescribed rehabilitation programme following arthroscopy was found to improve primary outcomes (International Hip Outcome Tool and sport subscale of the Hip Outcome Scale) to a clinically-relevant degree at 14 weeks post-surgery compared to a control group who followed a self-management programme with general guidance from their surgeon.[29] In the same study, the results at 24 weeks were inconclusive due to the small sample size.[29] Physical outcomes were not evaluated in this study.
- Subjects in the physiotherapy treatment group attended one pre-operative and six post-operative 30-minute sessions with a physiotherapist.[29]
- The post-operative visits were two weeks apart on average, ending at 12 weeks.
- Treatment during these sessions consisted of education, manual therapy (mandatory release of key trigger points, optional lumbar mobilisation) and, starting at 6-8 weeks post-surgery, functional and sport-specific drills.[29]
- Training within the patient's normal sport environment started at 10-12 weeks post-surgery.[29]
- In addition, these patients performed a daily home exercise programme (see exercise sheet below) and an unsupervised gym and aquatic programme (pool walking, stationary bike, cross-trainer and eventually swimming and lower body resistance) at least twice per week.[29]
The full treatment protocol can be viewed here. The home exercise sheets provided to patients in the physiotherapy group can be viewed here in PDF format. The return to sport guidelines provided to the treating physiotherapists can be viewed here in PDF format.
Conservative Management[edit | edit source]
- Casartelli et al.[11] suggest that improving the neuromuscular function of the hip should be a goal of conservative protocols for FAI syndrome due to weakness of deep hip musculature and an expected subsequent reduction in dynamic stability of the hip joint.[11] The authors recommend:[11]
- A randomised controlled trial by Mansell et al.[35] compared patient outcomes for surgical intervention versus physiotherapy. There was no statistically significant difference in outcomes found between the surgical and non-surgical groups and on average subjects in both groups reported no improvement in their condition at the two-year follow-up. Outcomes were the Hip Outcome Score (including daily activity and sports subscales), International Hip Outcome Tool, Global Rating of Change and return to work. The surgical procedure included a possible combination of labral repair or debridement, trimming of the acetabular rim and/or femoroplasty, as determined by the surgeon. The physiotherapy protocol was tailored to each subject based on a standardised assessment conducted by a physiotherapist. The programme could consist of manual therapy, motor control exercises and mobility/stretching exercises as follows:[30]
| Manual Therapy | Motor Control Exercises | Mobility Exercises |
|---|---|---|
| Hip Extension in Standing Mobilisation with Movement (MWM) | Reverse Lunge with Front Ball Tap | Kneeling Internal Rotation Self-Mobilisation with Lateral Distraction |
| Hip Distraction during Internal Rotation MWM | Isolateral Romanian Deadlift with Dowel | Half-Kneel FABER Self-Mobilisation |
| Loaded Lateral Hip Distraction MWM | Lateral Step-Down with Heel Hover | Quadruped Rock Self-Mobilisation with Lateral Distraction |
| Loaded Internal Rotation | Side Plank | Prone Figure-4 Self-Mobilisation |
| Lateral Glide in External Rotation | Seated Isometric Hip Flexion | ITB Soft Tissue Self-Mobilisation on Foam Roll |
| Long Axis Hip Distraction | Supine Hip Flexion with Theraband | Quadriceps Soft Tissue Self-Mobilisation on Foam Roll |
| x | x | Piriformis/Glut Min Self Myofascial Release on Ball |
| x | x | Standing Figure-4 Stretch |
| x | x | Kneeling Tri-Planar Mobilisations |
The above programme has been described in detail in the authors' supplemental files which can be viewed here.
Personalised Hip Therapy - The UK FASHIoN Trial[edit | edit source]
Wall et al.[6] developed a conservative care protocol based on a systematic review of the literature and a Delphi study group. The Personalised Hip Therapy Protocol was designed to last for 12 weeks with a minimum of three face-to-face and three phone/email contacts with the treating physiotherapist. A maximum of 10 contacts with the physiotherapist were permitted for the purposes of the FASHIoN trial. The comparison study between hip arthroscopy and the Personalised Hip Therapy Protocol demonstrated the following:
- Hip arthroscopy and personalised hip therapy both the improved hip-related quality of life for patients with femoroacetabular impingement syndrome.
- Hip arthroscopy led to a greater improvement than personalised hip therapy, and this difference was clinically significant.
- Further follow-up will reveal whether the clinical benefits of hip arthroscopy are maintained and whether it is cost-effective in the long term.
The full Personalised Hip Therapy protocol is as follows:[6]
| Core Component | Description |
|---|---|
| 1 Patient Education and Advice | Relative rest and lifestyle/ADL/sport modifications to try to avoid FAI e.g. avoidance of deep hip flexion, adduction and internal rotation |
| 2 Patient Assessment | Thorough patient history, pain-free PROM of the hip, hip impingement testing and strength of hip flexion, extension, abduction, adduction, internal rotation and external rotation |
| 3 Help with Pain Relief | Anti-inflammatories for 2-4 weeks or simple analgesics if anti-inflammatories don't help, adherence to a personalised exercise programme |
| 4 Exercise-Based Hip Programme | Start with muscle control work (pelvis, hip, glutes, abdominals), progressing to non-vigorous stretching (hip external rotation, hip abduction in flexion and extension) and strengthening (glut max, short external rotators, glut med, abdominals, lower limb in general) |
| Optional Components[6] | Description |
|---|---|
| Manual therapy | Hip joint mobilisations (e.g. distraction, AP glides) and trigger point work |
| Hip joint injection | For patients who do not improve with core treatment components above. For purposes of the FASHIoN trial, a maximum of one steroid injection could be included |
| Orthotics | Custom orthotics as an alternative to treatment of biomechanical abnormalities by a physiotherapist |
| Taping | To assist with postural modification e.g. tape thigh into external rotation and abduction |
| Group-based treatments | For the purposes of the FASHIoN trial, group treatments could be included but only in addition to the core components |
| Treatment of additional pathology/symptoms | Based on the findings of the treating physiotherapist, pathology/symptoms that were felt to be affecting the FAI could also be treated |
For the purposes of the FASHIoN trial, hydrotherapy, acupuncture, electrotherapy and forceful manual techniques were excluded from the protocol.[6]
Bracing[edit | edit source]
Newcomb et al.[13] investigated the immediate and longer-term effects of wearing a brace. The brace is a Don Joy S.E.R.F./Stability through External Rotation of the Femur model.[13] They found that:[13]
- The brace did modify the kinematics of patients with FAI by limiting movements that were associated with hip impingement (flexion, internal rotation and adduction of the hip) during common activities (squat, stair climbing and stair descending).
- The brace did not change the kinematics involved with the single-limb squat.
- The identified kinematic changes did not lead to decreased pain or improvement in patient-reported outcomes either immediately or after four weeks of daily brace use.
The authors' conclusion was that there may be a sub-group of patients with FAI syndrome that may benefit from bracing but based on their particular study, the use of bracing is not supported as a general conservative therapy for this condition.[13]
Prognosis[edit | edit source]
Patients treated for symptomatic FAI syndrome frequently report improvement in their symptoms and are able to return to their usual activities.[2] However, the long-term prognosis is not known, nor is it known if treatment of FAI syndrome prevents the development of hip OA.[2] According to the authors in the Warwick Agreement, symptoms of FAI syndrome will probably worsen if no treatment is provided.[2]
Resources[edit | edit source]
Presentations[edit | edit source]
 |
Femoral Acetabular Impingement by Adam Smithson, University of Nottingham
This presentation, created by Adam Smithson as part of the MSc programme at the University of Nottingham, discusses FAI and the accuracy of commonly-used impingements tests.[16] View the presentation |
References[edit | edit source]
- ↑ Murphy NJ, Eyles J, Bennell KL, Bohensky M, Burns A, Callaghan FM et al. Protocol for a multi-centre randomised controlled trial comparing arthroscopic hip surgery to physiotherapy-led care for femoroacetabular impingement (FAI): the Australian FASHIoN trial. BMC Musculoskelet Disord. 2017 Sep 26;18(1):406.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 Griffin DR, Dickenson EJ, O'Donnell J, Agricola R, Awan T, Beck M et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement. Br J Sports Med. 2016; 50(19):1169-76.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Chaudhry H, Ayeni OR. The aetiology of femoroacetabular impingement: what we know and what we don't. Sports Health. 2014 Mar;6(2):157-61.
- ↑ Trigg SD, Schroeder JD, Hulsopple C. Femoroacetabular impingement syndrome. Current Sports Medicine Reports. 2020 Sep 1;19(9):360-6.
- ↑ Maupin JJ, Steinmetz G, Thakral R. Management of femoroacetabular impingement syndrome: current insights. Orthop Res Rev. 2019 Aug 27;11:99-108.
- ↑ 6.0 6.1 6.2 6.3 6.4 Wall PD, Dickenson EJ, Robinson D, Hughes I, Realpe A, Hobson R, Griffin DR, Foster NE. Personalised Hip Therapy: development of a non-operative protocol to treat femoroacetabular impingement syndrome in the FASHIoN randomised controlled trial. Br J Sports Med. 2016;50(19):1217-23.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Raveendran R, Stiller JL, Alvarez C, Renner JB, Schwartz TA, Arden NK, Jordan JM, Nelson AE. Population-based prevalence of multiple radiographically-defined hip morphologies: the Johnston County Osteoarthritis Project. Osteoarthritis Cartilage. 2018 Jan;26(1):54-61.
- ↑ RegencyMarketing. Cam impingement. Available from: http://www.youtube.com/watch?v=1Q11jjHguPI[last accessed 12/02/18]
- ↑ RegencyMarketing. Pincer impingement. Available from: http://www.youtube.com/watch?v=ucLy6em3d_w[last accessed 12/02/18]
- ↑ 10.0 10.1 Chinzei N, Hashimoto S, Fujishiro T, Hayashi S, Kanzaki N, Uchida S, Kuroda R, Kurosaka M. Inflammation and Degeneration in Cartilage Samples from Patients with Femoroacetabular Impingement. J Bone Joint Surg Am. 2016 Jan 20;98(2):135-41.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 Casartelli NC, Maffiuletti NA, Bizzini M, Kelly BT, Naal FD, Leunig M. The management of symptomatic femoroacetabular impingement: what is the rationale for non-surgical treatment? Br J Sports Med. 2016 May;50(9):511-2.
- ↑ 12.0 12.1 12.2 12.3 12.4 12.5 12.6 12.7 Diamond LE, Dobson FL, Bennell KL, Wrigley TV, Hodges PW, Hinman RS. Physical impairments and activity limitations in people with femoroacetabular impingement: a systematic review. Br J Sports Med. 2015 Feb;49(4):230-42.
- ↑ 13.0 13.1 13.2 13.3 13.4 Newcomb NRA, Wrigley TV, Hinman RS, Kasza J, Spiers L, O'Donnell J, Bennell KL. Effects of a hip brace on biomechanics and pain in people with femoroacetabular impingement. J Sci Med Sport. 2018 Feb;21(2):111-116.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 14.7 Frangiamore S, Mannava S, Geeslin AG, Chahla J, Cinque ME, Philippon MJ. Comprehensive Clinical Evaluation of Femoroacetabular Impingement: Part 1, Physical Examination. Arthrosc Tech. 2017 Oct 30;6(5):e1993-e2001.
- ↑ Philippon MJ, Maxwell RB, Johnston TL, Schenker M, Briggs KK. Clinical presentation of femoroacetabular impingement. Knee Surg Sports Traumatol Arthr 2007; 15:1041–1047.
- ↑ 16.0 16.1 16.2 16.3 Adam Smithson. Femoral Acetabular Impingement by Adam Smithson, University of Nottingham. Available from: http://www.youtube.com/watch?v=uY9N8hmrr_g[last accessed 02/03/18]
- ↑ Caliesch R, Sattelmayer M, Reichenbach S, Zwahlen M, Hilfiker R. Diagnostic accuracy of clinical tests for cam or pincer morphology in individuals with suspected FAI syndrome: a systematic review. BMJ open sport & exercise medicine. 2020 Apr 1;6(1):e000772.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 18.7 Reiman MP, Thorborg K. Femoroacetabular impingement surgery: are we moving too fast and too far beyond the evidence? Br J Sports Med. 2015 Jun;49(12):782-4.
- ↑ The Physio Channel. How to do the FADIR hip impingement test.2018. Available from: https://www.youtube.com/watch?v=PqgPWRqmQ_A[last accessed 5/03/22]
- ↑ 20.0 20.1 20.2 Pandya R. Femoroacetabular Impingement Course. Plus. 2022.
- ↑ Dijkstra HP, Ardern CL, Serner A, Mosler AB, Weir A, Roberts NW, Mc Auliffe S, Oke JL, Khan KM, Clarke M, Glyn-Jones S. Primary cam morphology; bump, burden or bog-standard? A concept analysis. Br J Sports Med. 2021 Nov;55(21):1212-1221.
- ↑ Sheikh Z, Adams M. Lateral centre-edge angle. Reference article, Radiopaedia.org. (accessed on 07 Mar 2022) https://doi.org/10.53347/rID-62982
- ↑ 23.0 23.1 23.2 Chopra A, Grainger AJ, Dube B, Evans R, Hodgson R, Conroy J, Macdonald D, Robinson P. Comparative reliability and diagnostic performance of conventional 3T magnetic resonance imaging and 1.5T magnetic resonance arthrography for the evaluation of internal derangement of the hip. Eur Radiol. 2018 Mar;28(3):963-971.
- ↑ 24.0 24.1 24.2 Reiman MP, Thorborg K, Goode AP, Cook CE, Weir A, Hölmich P. Diagnostic Accuracy of Imaging Modalities and Injection Techniques for the Diagnosis of Femoroacetabular Impingement/Labral Tear: A Systematic Review With Meta-analysis. Am J Sports Med. 2017 Sep;45(11):2665-2677.
- ↑ Cunningham DJ, Paranjape CS, Harris JD, Nho SJ, Olson SA, Mather RC 3rd. Advanced Imaging Adds Little Value in the Diagnosis of Femoroacetabular Impingement Syndrome. J Bone Joint Surg Am. 2017 Dec 20;99(24):e133.
- ↑ 26.0 26.1 26.2 Kaya M. Measurement of Hip Contact Pressure During Arthroscopic Femoroacetabular Impingement Surgery. Arthrosc Tech. 2017 May 1;6(3):e525-e527.
- ↑ Martin RL, Enseki KR, Draovitch P, Trapuzzano T, Philippon MJ. Acetabular labral tears of the hip: Examination and diagnostic challenges. JOSPT. 2006;36(7):503-15.
- ↑ 28.0 28.1 Emara K, Samir W, Hausain Motasem EH, Abd El Ghafar K. Conservative treatment for mild femoroacetabular impingement. Journal of Orthopaedic Surgery. 2011;19(1):41-5.
- ↑ 29.0 29.1 29.2 29.3 29.4 29.5 29.6 Bennell KL, Spiers L, Takla A, O'Donnell J, Kasza J, Hunter DJ, Hinman RS. Efficacy of adding a physiotherapy rehabilitation programme to arthroscopic management of femoroacetabular impingement syndrome: a randomised controlled trial (FAIR). BMJ Open. 2017 Jun 23;7(6):e014658.
- ↑ 30.0 30.1 30.2 Mansell NS, Rhon DI, Marchant BG, Slevin JM, Meyer JL. Two-year outcomes after arthroscopic surgery compared to physical therapy for femoracetabular impingement: A protocol for a randomized clinical trial. BMC Musculoskelet Disord. 2016 Feb 4;17:60.
- ↑ 31.0 31.1 31.2 31.3 Peters S, Laing A, Emerson C, Mutchler K, Joyce T, Thorborg K, Hölmich P, Reiman M. Surgical criteria for femoroacetabular impingement syndrome: a scoping review. Br J Sports Med. 2017;51(22):1605-1610.
- ↑ RegencyMarketing. Soft Tissue Hip Surgery - part 1. 2010. https://www.youtube.com/watch?v=iE9cgvI7OKw [last accessed 6/03/22]
- ↑ 33.00 33.01 33.02 33.03 33.04 33.05 33.06 33.07 33.08 33.09 33.10 33.11 33.12 33.13 33.14 33.15 33.16 33.17 33.18 33.19 33.20 Nakano N, Lisenda L, Jones TL, Loveday DT, Khanduja V. Complications following arthroscopic surgery of the hip: a systematic review of 36 761 cases. Bone Joint J. 2017 Dec;99-B(12):1577-1583.
- ↑ Casartelli NC, Bizzini M, Maffiuletti NA, Sutter R, Pfirrmann CW, Leunig M, Naal FD. Exercise therapy for the management of femoroacetabular impingement syndrome: preliminary results of clinical responsiveness. Arthritis Care Research, 2019; 71(8):1074-1083.
- ↑ Mansell NS, Rhon DI, Meyer J, Slevin JM, Marchant BG. Arthroscopic Surgery or Physical Therapy for Patients With Femoroacetabular Impingement Syndrome: A Randomized Controlled Trial With 2-Year Follow-up. Am J Sports Med. 2018 Feb 1:363546517751912.