How We Breathe
Introduction[edit | edit source]
Breathing is one of our most crucial functions and is central to health - it is the foundation of movement, health, and wellbeing.[1][2] Respiration refers to the movement of oxygen into the body and the removal of carbon dioxide. It is essential in the metabolisation of energy.[2]
Breathing affects the entire body. It has a significant role in ensuring that allostasis (achieving homeostasis) is maintained, as well as being involved in postural stability and mobility of the trunk and spine.[3] Van Dixhoorn summarises the key functions of breathing as follows:[1]
- Gas exchange and respiratory function, which includes smell and speech
- Musculoskeletal movement, which includes the movement of body fluids, organ function, mobility and trunk stability
- The connection of conscious awareness with the state of the body.[1]
An optional breath is usually defined as a three-dimensional abdominal breath that results in the expansion of the lower ribs.[3].
While essential for survival, this pattern can be disrupted by several factors, including interference from our:
- Thoughts,
- Feelings
- Past experience.[2]
This disruption results in dysfunctional breathing.
- Factors that may interrupt optimal breathing include biomechanics, biochemistry and psychophysiology.
- Moreover, breathing patterns can, in turn, influence these functions.[2]
History of Breathing Pattern Disorders[edit | edit source]
One of the earliest discussions of the symptoms that are now associated with breathing pattern disorders was a report by Dr Jacob M Da Costa in 1871. He noted that several American civil war soldiers complained of a specific set of symptoms that mimicked those of heart disease: fatigue on exertion, palpitations, sweating, chest pain and shortness of breath[1][4] Da Costa’s syndrome became known as Soldier’s Heart or Irritable Heart, although he noted that similar features often presented in private practice as well.[1][5]
The term “Hyperventilation” was coined by Kerr and colleagues in 1937 and has been in common use since.
- Essentially, hyperventilation refers to someone who breathes over his or her metabolic demands, which results in hypocapnia.[1]
- While it has had many different names, Hyperventilation Syndrome was initially used to describe a state of anxiety that existed alongside other cardiovascular and emotional symptoms; patients were seen as neurotic, and their condition was not considered seriously.[1]
However, research into this condition continued from these early reports and definitions.
- In the 1950s, Konstantin Pavlovich Buteyko developed the Buteyko method, which uses breathing exercises to treat symptoms associated with low carbon dioxide levels.[2]
- In the 1960s, Dianna Innocenti, Rosemary Cluff and Professor Claude Lum collaborated to develop a series of breathing exercises,[2] now known as the Papworth Method, which has been found to improve respiratory symptoms, dysfunctional breathing and mood.[6]
- Recently, research on breathing pattern disorders has explored a range of symptoms associated with the influence of psychology on breathing, including anticipation, the suppression of emotions, association and conditioned responses.[1]
- Research has also explored the impact that the musculoskeletal system has on breathing (as well as the impact of breathing on the musculoskeletal system).[1]
Definitions[edit | edit source]
There is no formal definition of dysfunctional breathing, but the term is used to refer to a group of irregular breathing patterns that result in chronic changes in breathing patterns.[7][2]
- The primary symptom of dysfunctional breathing is dyspnoea. Still, it is also associated with other non-respiratory symptoms, including dizziness and palpitations[8]
- These occur in the absence of, or in excess of, a related physiological condition (cardiac or respiratory)[2][7]
Hyperventilation is the most widely recognised form of dysfunctional breathing.[9]
- It refers to breathing that is disproportionate to bodily functions
- Overbreathing reduces the levels of carbon dioxide in the bloodstream, causing respiratory alkalosis[2]
Breathing disorders are defined as inappropriate breathing, which is persistent enough to cause symptoms with no clear organic cause[10] - although an organic disorder (asthma, COPD, diabetes, anaemia) may be present[2]
While work on classification is continuing, it is important to note that breathing dysfunction has many components. An accurate subjective assessment will enable physiotherapists to determine what is driving the dysfunctional breathing.[2]
- Is it due to a mechanical dysfunction such as tight accessory respiratory muscles?
- Is it driven by biochemical factors?
- Could it have been caused by a traumatic event or anxiety?
Epidemiology[edit | edit source]
Breathing pattern disorders remain poorly understood, so it is thought that this condition is likely underdiagnosed or misdiagnosed:[8]
- Hyperventilation Syndrome is thought to affect 6-10% of the general population - in an asthmatic population, these rates may be as high as 20% and 18% (chronic vs acute hyperventilation) [11]
- A recent study by Vidotto and colleagues reports that dysfunctional breathing is identified in all age ranges[8]
- In adults presenting in primary care settings in the United Kingdom, prevalence rates are around 9.5%:[8]
- There are higher rates in patients with asthma
- One-third of women with asthma and one-fifth of men have dysfunctional breathing patterns
- It is impossible to determine the exact prevalence of dysfunctional breathing as there is no gold standard diagnostic criteria[12]
- While diagnosis is made after other organic pathologies have been ruled out, the Nijmegen Questionnaire is usually used as a diagnostic tool. However, it may not be valid in certain circumstances[13]
Basics of Breathing[edit | edit source]
Internal and External Respiration[edit | edit source]
The lungs play an essential role in providing cells with oxygen via the blood and cardiovascular system, which enables cells to produce energy.[14]
- On inhalation, oxygen enters the lungs and diffuses into the blood. The heart receives this oxygenated blood and pumps it to the cells.[14]
- Carbon dioxide waste diffuses back into the blood at the cell level and is transported to the lungs, where it is expelled on exhalation.[14]
- The exchange of gases in the lungs is called external respiration, and the exchange of gases in the cells is referred to as internal respiration.[14]
Conduction and Respiratory Zones[edit | edit source]
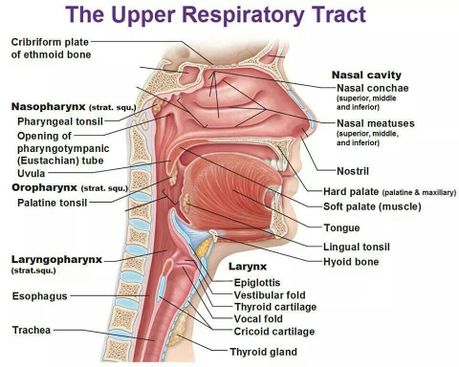
The conduction zone refers to the areas where the air is transported to the lungs from the external environment. These are the:[14]
- Nasal cavity
- Pharynx
- Larynx
- Trachea
- Bronchi and bronchioles
The nasal cavities and turbinates play an important physiological function as they humidify, moisten, warm and filter air.[2] The paranasal sinuses produce nitric oxide (NO), which diffuses to the lungs and bronchi, particularly during nasal breathing. NO has a vasodilatory and bronchodilatory effect.[16][17]. It plays a significant role in nasal patency, uptake of oxygen and the sterilisation of the lungs and airways.[2]
The upper portion of the pharynx is the nasopharynx, which plays an important role in pressure control.
The vocal cords are situated in the larynx.[18] Dysfunctions related to the vocal folds include vocal cord dysfunction, and Exercise-Induced Laryngeal Obstruction and should be considered when exploring breathing pattern disorders.[2]
After air travels to the bronchioles, it passes on to the alveoli where ventilation and perfusion take place (ie the respiratory zone).[2][14]
Respiratory Muscles[edit | edit source]
There are three groups of respiratory muscles:[19]
The diaphragm is the main musculoskeletal muscle involved in respiration. When the diaphragm contracts, the abdomen and lower part of the rib cage expand.[19]
The rib cage muscles, including the intercostals, the parasternal, the scalene and the neck muscles, are involved in inspiration and expiration. They mostly act on the upper part of the rib cage.[19]
The abdominal muscles are expiratory, and they act on the abdomen and the abdominal rib cage.[19]
Diaphragm[edit | edit source]
The diaphragm is a dome-shaped muscle that is primarily involved in respiration. The superior portion of the diaphragm originates at the xiphoid process anteriorly, the lower six costal cartilages of the thorax laterally and the first two lumbar vertebrae posteriorly. It converges into a central tendon which forms the dome’s crest.[20] The peripheral segment attaches to the chest wall and abdominal cavity.[20]
It is innervated by the right and left phrenic nerves (C3, 4, 5) and has three major openings - the aorta, vena cava and the oesophagus.[20][2]
The diaphragm and intercostal muscles are the only muscles that are active during quiet inspiration.[2]
The diaphragm contracts and pulls its central tendon down. This increases the negative pressure inside the thoracic cavity, which draws air in. At the same time, the external intercostal muscles raise the anterior chest wall - in a bucket handle action.[20] As the chest cavity becomes larger and wider, the air can enter from outside the body.[20]
During quiet exhalation, the rib cage and chest wall relax and return to their original position. Concurrently, the diaphragm relaxes and lifts. This movement expels the air from the lungs.[20] The diaphragm of individuals who have hyper-inflated chests (i.e. those with COPD or voluntary hyperinflation) will not be able to return to their natural resting position during exhalation.[2]
The diaphragm has many other roles aside from respiration. When it contracts, it works with the anterior abdominal wall muscles to increase intra-abdominal pressure - thus, it aids processes such as micturition (urination), defecation, and parturition (giving birth).[20] It is also integral to stability during locomotion.[2]
It also acts essentially as a pump.[2] On inhalation, its descent decreases intrathoracic pressure and improves intra-abdominal pressure. This compresses the inferior vena cava and helps push deoxygenated blood into the right atrium. It also compresses abdominal lymph vessels assisting lymph movement.[20] Similarly, cerebrospinal fluid is pumped into the brain and pumped back down on exhalation. Thus, the diaphragm plays a significant role in the movement, mobility and cleansing of the whole body.[2]
Accessory Respiratory Muscles[edit | edit source]
As breathing demands increase, humans require more air in larger volumes. Thus, we adopt an apical and a thoracic lateral breathing pattern, and our accessory respiratory muscles become involved. The primary accessory muscles are:[2]
- Scaleni
- Pectoralis major and minor
- Sternocleidomastoid
- Iliocostais
- Serratus anterior and posterior
- Latissimus dorsi
- Trapezius
- Transversus abdominus, multifidus and the pelvic floor muscles are also involved.
All muscles work together to ensure an efficient breathing pattern.[2]
- When patients present with neck or shoulder pain, or thoracic outlet problems (peripheral pins and needles etc.), it can be beneficial to consider their breathing patterns (i.e. breathing pattern, respiratory rate, location of breath).[2]
- Patients with neck pain present with several musculoskeletal deficits and respiratory dysfunction.[22] Their respiratory function may be affected due to strength deficits in their respiratory muscles.[23] If they have adopted a more apical breathing pattern, these respiratory muscles will be overworked, which results in increased muscular tension. This can significantly impact the neurovascular bundle, which travels under the clavicle, pectoralis minor and down the arm.[2]
- NB performing a neurodynamic tension test pre-and post-breathing retraining can highlight changes in tension caused by a reduction in accessory muscle work.
Pelvic Floor[edit | edit source]
The pelvic floor also plays an important role in breathing.
- It descends on inhalation and returns to its resting position on exhalation.[2]
- Contractions of the pelvic floor are combined with abdominal muscle activity - they work in conjunction with the anterolateral abdominal muscles and the diaphragm to control/react to changes in intra-abdominal pressure.
- All three muscle groups work together to protect organs against changes in pressure and contribute to the respiratory and postural function.[24][25]
Summary[edit | edit source]
Breathing is essential for survival and impacts many systems, including our biomechanics, biochemistry and psychophysiology.
- Breathing patterns can be disrupted by several factors
- A significant number of people are diagnosed with breathing pattern disorders, but due to a lack of understanding and gold standard diagnostic tool, prevalence rates may be higher than those recorded
- When assessing breathing pattern disorders, it is essential to understand the physiology and anatomy of respiration, but it is also important to look at biomechanics and the musculoskeletal system.
- It is impossible to breathe well unless this system is working effectively
- Consider the whole system, from the nose, vocal folds, diaphragm, pelvic floor and surrounding muscles[2]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Clifton‐Smith T, Rowley J. Breathing pattern disorders and physiotherapy: inspiration for our profession. Phys Ther Rev. 2011; 16: 75–86.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 Clifton-Smith T. How We Breathe Course. Plus. 2020.
- ↑ 3.0 3.1 Csepregi É, Gyurcsik Z, Veres-Balajti I, Nagy AC, Szekanecz Z, Szántó S. Effects of Classical Breathing Exercises on Posture, Spinal and Chest Mobility among Female University Students Compared to Currently Popular Training Programs. International Journal of Environmental Research and Public Health. 2022 Mar 21;19(6):3728
- ↑ Paul O. Da Costa's syndrome or neurocirculatory asthenia. Br Heart J. 1987 Oct;58(4):306-15.
- ↑ Borges GP, Tonon JH, Zunini PA, Martins da Silva AS, Garcia MD, de Azevedo-Marques Périco C, Lima DR, Torales J, Ventriglio A, Bhugra D, Castaldelli-Maia JM. Soldier’s heart: the forgotten circulatory neurasthenia–a systematic review. International Review of Psychiatry. 2020 Aug 17;32(5-6):510-9.
- ↑ Holloway EA, West RJ. Iintegrated breathing and relaxation training (the Papworth method) for adults with asthma in primary care: a randomised controlled trial. Thorax. 2007 Dec;62(12):1039-42.
- ↑ 7.0 7.1 Ionescu MF, Mani-Babu S, Degani-Costa LH, Johnson M, Paramasivan C, Sylvester K, Fuld J. Cardiopulmonary exercise testing in the assessment of dysfunctional breathing. Frontiers in Physiology. 2021 Jan 27;11:620955.
- ↑ 8.0 8.1 8.2 8.3 Vidotto LS, Carvalho CRF, Harvey A, Jones M. Dysfunctional breathing: what do we know?. J Bras Pneumol. 2019; 45(1): e20170347.
- ↑ Tavel ME. Hyperventilation syndrome: Why is it regularly overlooked?. The American Journal of Medicine. 2021 Jan 1;134(1):13-5.
- ↑ Bradley H, Esformes J. Breathing pattern disorders and functional movement. Int J Sports Phys Ther. 2014 Feb;9(1):28-39.
- ↑ Deenstra DD, van Helvoort HA, Djamin RS, van Zelst C, in’t Veen JC, Antons JC, Spruit MA, van’t Hul AJ. Prevalence of hyperventilation in patients with asthma. Journal of asthma. 2022 Aug 3;59(8):1560-7.
- ↑ Denton E, Bondarenko J, Hew M. Breathing pattern disorder. Complex Breathlessness (ERS Monograph). Sheffield, European Respiratory Society. 2022 Sep 1:109-22.
- ↑ Azizmohammad Looha M, Masaebi F, Abedi M, Mohseni N, Fakharian A. The Optimal Cut-off Score of the Nijmegen Questionnaire for Diagnosing Hyperventilation Syndrome Using a Bayesian Model in the Absence of a Gold Standard. Galen Med J. 2020 Jun 24;9:e1738.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 Cedar SH. Every breath you take: the process of breathing explained. Nursing Times [online]. 2018; 114(1): 47-50.
- ↑ Ted-ED. How do lungs work? - Emma Bryce. Available from https://www.youtube.com/watch?v=8NUxvJS-_0k [last accessed 5/8/2020]
- ↑ Martel J, Ko YF, Young JD, Ojcius DM. Could nasal nitric oxide help to mitigate the severity of COVID-19? Microbes Infect. 2020 May-Jun;22(4-5):168-171.
- ↑ Lundberg JO, Settergren G, Gelinder S, Lundberg JM, Alving K, Weitzberg E. Inhalation of nasally derived nitric oxide modulates pulmonary function in humans. Acta Physiol Scand. 1996 Dec;158(4):343-7.
- ↑ Suárez-Quintanilla J, Fernández Cabrera A, Sharma S. Anatomy, Head and Neck, Larynx. [Updated 2020 Sep 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538202/
- ↑ 19.0 19.1 19.2 19.3 Aliverti A. The respiratory muscles during exercise. Breathe (Sheff). 2016 Jun;12(2):165-8.
- ↑ 20.0 20.1 20.2 20.3 20.4 20.5 20.6 20.7 Bains KNS, Kashyap S, Lappin SL. Anatomy, Thorax, Diaphragm. [Updated 2020 Apr 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK519558/
- ↑ Kenhub - Learn Human Anatomy. Diaphragm - definition, function, muscles and anatomy. Available from https://www.youtube.com/watch?v=6IK-YHK1ToM [last accessed 5/8/2020]
- ↑ Wirth B, Amstalden M, Perk M, Boutellier U, Humphreys BK. Respiratory dysfunction in patients with chronic neck pain - influence of thoracic spine and chest mobility. Man Ther. 2014 Oct;19(5):440-4.
- ↑ Dimitriadis Z, Kapreli E, Strimpakos N, Oldham J. Respiratory weakness in patients with chronic neck pain. Manual therapy. 2012; 18(3): 248-53.
- ↑ Park H, Hwang B, Kim Y. The impact of the pelvic floor muscles on dynamic ventilation manoeuvres. J Phys Ther Sci. 2015 Oct;27(10):3155-7.
- ↑ Hodges PW, Sapsford R, Pengel LH. Postural and respiratory functions of the pelvic floor muscles. Neurourol Urodyn. 2007;26(3):362-71.