Hydrocephalus
Introduction[edit | edit source]
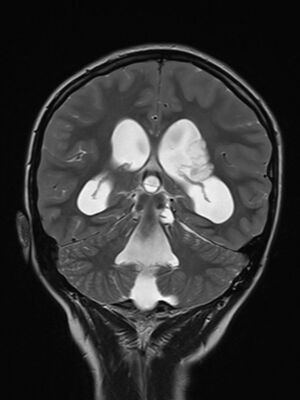
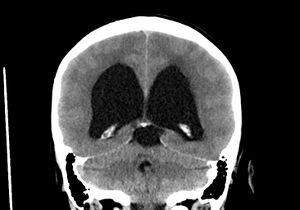
Hydrocephalus is an abnormal build-up of cerebrospinal fluid(CSF) within and around the brain, which can be due to excess fluid production, obstruction to its flow, and inadequate absorption[1] If left untreated, the excess fluid can cause an increase in the pressure put on the skull and brain, which can be damaging[2].
Causes[edit | edit source]
The CSF is the clear, and colourless fluid that cushions and protects the spinal cord and brain. The CSF circulates through the ventricles and bathes the brain and spinal cord after which it is reabsorbed into the bloodstream.[3] The production of CSF is performed by the ependymal cells in the choroid plexus of the lateral ventricles of the brain.[4] Under physiologic conditions, the same amount of CSF is produced and absorbed daily. Yet, when there is a disruption in the normal flow or absorption of CSF, a buildup of CSF can result. This can impair the functioning of the brain due to elevated pressure from the CSF buildup and can result in brain damage, and in severe conditions, death.[3]
The etiology of hydrocephalus can be congenital or acquired. Hydrocephalus due to any obvious external cause is termed as congenital hydrocephalus whereas hydrocephalus secondary to any condition such as hemorrhage, is known as acquired hydrocephalus. The most common cause of acquired hydrocephalus in infants is hemorrhage due to prematurity. In addition to this, the other causes include neoplasm, an infection most often bacterial meningitis, intrauterine infections with enterovirus, lymphocytic choriomeningitis, toxoplasmosis, and cytomegalovirus(CMV). Infantile hydrocephalus is associated with certain medications taken during pregnancy such as anti-depressants, misoprostol, and metronidazole. Hydrocephalus which is not caused by any of the above-mentioned extrinsic causes is regarded as congenital hydrocephalus with some underlying genetic pathology. X-linked hydrocephalus is associated with aqueductal stenosis, which forms one of the most common hereditary forms of hydrocephalus affecting 10% of males with isolated idiopathic hydrocephalus. In addition to these causes, neural tube defects also cause hydrocephalus[5].
Classification[edit | edit source]
Classification of hydrocephalus has always been controversial, the first attempt at the classification of hydrocephalus was made by Walter Dandy in 1913. The current classification with relation to the latest evidence, hydrocephalus can be classified as communicating hydrocephalus and non communicating hydrocephalus.
Communicating hydrocephalus is further divided into obstructive and non-obstructive types.
Communicating hydrocephalus results when there is impedance of cerebrospinal fluid after it exits the ventricles. Communicating hydrocephalus can be obstructive in nature where there is obstruction at some point between basal cisternae and arachnoid granulations. This obstruction can be due to conditions like subarachnoid haemorrhage, meningitis, and congenital or acquired pathologies[6][7][8].
Location of the obstruction and corresponding causes of obstruction[9]
| Location | Cause |
|---|---|
| Lateral, 3rd and
4th ventricles |
Intraventricular haemorrhage |
| 3rd ventricle at foramen
of Monro |
Colloid cyst |
| 3rd ventricle | Tumours |
| Cerebral aqueduct | Aqueduct stenosis
Tumours |
| 4th ventricle | Dandy Walker malformation
Tumours |
| Impaired absorption at the
arachnoid granulations |
Subarachnoid haemorrhage
Trauma Meningitis |
Non-obstructive communicating hydrocephalus includes normal pressure hydrocephalus which can be idiopathic or secondary following trauma[10].
Non communicating hydrocephalus occurs when there is intra-ventricular obstruction of CSF flow, therefore non-communicating hydrocephalus is always of obstructive type. This obstruction in the CSF flow can be due to conditions such as TORCH infections (Toxoplasmosis, Other (syphilis, varicella-zoster, parvovirus B19), Rubella, Cytomegalovirus (CMV), and Herpes) which are the most common forms of infections that are associated with congenital abnormalities.[1] The sites of obstruction includes Foramen of Munro and cerebral aqueduct[11].
Pathophysiology - Change in CSF dynamics[edit | edit source]
With the development of hydrocephalus, there is an alteration in CSF dynamics. The CSF exchange between the lateral ventricles and the third ventricles is compromised. With the development of hydrocephalus, the Foramen of Munro undergoes dilation. Both the lateral ventricle and the third ventricle become monoventricle, however, the cerebral aqueduct retains its function. Also, there is exaggerated motion of CSF through the cerebral aqueduct. In addition to this CSF pulsatility (i.e with every heartbeat, the arterial blood volume increases briefly and venous blood and CSF are pushed out of the cranium which leads to the pulsatile flow of CSF)is also disturbed. These changes lead to compromise in the unidirectional flow of CSF from the site of production to the site of absorption[12].
Clinical features[edit | edit source]
Neurological consequences, postnatally, include developmental delay, failure to thrive, apnea, and bradycardias. Patients with aqueductal stenosis (AS), regardless of the type of postnatal treatment or intervention, showed a high incidence of epilepsy, developmental delay, cerebral palsy, and attention deficit hyperactivity disorders[13].
Clinical features of hydrocephalus widely vary according to the age of the patient and the rate of progression[9].
- Clinical features of hydrocephalus before the closure of the cranial sutures (<2 years of age ) include macrocephaly, increasing head circumference of the head, sunsetting sign, distended scalp veins, developmental delay, poor feeding and regression.
- After the closure of cranial sutures, the acute presentation includes, headache, vomiting, drowsiness, papilledema, and coma in extreme cases.
- Chronic presentation and clinical features of normal pressure hydrocephalus include Urinary Incontinence cognitive impairments and gait disturbances.
Neuropsychological deficits[edit | edit source]
The major neuropsychological deficits include deficits in visuoperceptual and visuomotor functions. This deficit depends on the severity and etiology of hydrocephalus. Corpus callosum abnormalities resulting from the stretching of colossal fibers and other white cortical tracts contribute to these deficits. Children with hydrocephalus present with a higher verbal IQ( intelligence quotient ) than performance IQ.[14]
Management[edit | edit source]
Non - Surgical Management[edit | edit source]
Non-surgical management is a symptomatic treatment for hydrocephalus. Medications such as Acetazolamide or Isosorbide are used temporarily to reduce CSF production, and also increase CSF absorption by producing hyperosmotic diuresis.[15]
In premature infants, hydrocephalus develops due to intraventricular hemorrhage , which causes obstruction in the arachnoid granulations by the products which are broken down due to hemorrhage. In such cases, lumbar puncture is one form of non-surgical in premature infants with periventricular dilation following periventricular hemorrhage. Removal of CSF with blood and protein approximately 10-15 ml/kg normal resorption of CSF to prevent the development of hydrocephalus after periventricular hemorrhage.
Despite few studies supporting this method, other studies revealed that repeated lumbar puncture did not reduce the need for shunting of cerebrospinal fluid and also this method did not decrease the likelihood of death or disability in these patients.
Surgical management[edit | edit source]
Babies born or children who have developed hydrocephalus usually require swift treatment to reduce the pressure on their brains. If the condition is not treated, the increase in pressure will damage the brain. Both congenital and acquired hydrocephalus can be treated with shunt surgery or neuroendoscopy[16].
Shunt Surgery[edit | edit source]
Shunt surgery consists of inserting a thin tube (a shunt) in the brain, which is used to remove excess fluid from the brain. There are two major types of shunt surgeries namely ventriculoatrial shunt, ventriculoperitoneal shunt and lumboperitoneal shunt.
Ventriculo Atrial shunt.
This shunt drains the CSF from the cerebral ventricle to the right atrium of the heart. After placing the ventricular side of the catheter by a neurosurgeon, following the neck is dissected with a parallel longitudinal incision to the sternocleidomastoid muscle and the branch of the internal jugular vein which is compatible with the diameter of the shunt is selected and the distal end is placed which drains the fluid into the right atrium.[17]
Ventriculoperitoneal shunt
With the proximal catheter being inserted into the cerebral ventricle, the distal catheter is placed into the peritoneal cavity.[18]
Lumboperitoneal shunt
One end of the catheter is inserted into the lumbar theca either percutaneously or through an open operation and the other end of the catheter is inserted into the peritoneal cavity.[18]
Shunt complications[edit | edit source]
Even though shunting is one of the most common surgical approaches for management, however, it presents with the following complications:[18]
- Thoracic occlusion
- Ventricular occlusion
- Shunt separation
- Kinked Tubing
- CSF fistula
- Migrating catheter, distal as well as ventricular
- Subdural Hematoma
- Ventricular Hemorrhage
- Surfacing shunt
- Infections such as meningitis, peritonitis extending along the channel
- Following a shunt surgery, some patients may experience headaches and vomiting in standing and sitting positions this is known as low pressure state which can be gradually resolved by increased fluid intake and gradual mobilisation.
Endoscopic third ventriculostomy (ETV)
ETV is a surgical method that is somewhat helpful in avoiding certain shunt-related complications such as shunt obstruction, infection, and over drainage. This is the treatment of choice in obstructive hydrocephalus where a burr hole is created at the base of the third ventricle using a flexible or rigid endoscope for the fluid to drain in the basal cisternae[18].
Physiotherapy Management[edit | edit source]
Regardless of the different surgical management, children with hydrocephalus still have some disabilities. Therefore, early involvement with physiotherapists via different methods of rehabilitation is essential, whether surgical or non-surgical management is required. Additionally, successful shunting is usually related to more obvious and rapid improvements in rehabilitation efforts[19]. Specific treatment procedures are numerous, functional training for activities of daily living; therapeutic exercise; manual techniques such as mobilization and stretching; and therapeutic modalities[20].
Physiotherapy goals are aimed at:
- Improving functional skills and reducing secondary impairment, such as obesity, contractures, and fractures, which could delay developmental skills. Furthermore, physiotherapists can work with children in their homes and in the hospital or clinic, depending on their medical conditions and age[21].
- Motor control (co-ordination of muscles and limbs), learning theories, and development are factors that contribute to the occurrence of motor behaviour (how the muscles and limbs react to movement, control, development, and learning). These factors include not only the central nervous system (brain and spinal cord) as the driving force, but also biomechanical (human movement principles), psychological, social, and environmental components[20].
- Teaching and practising skills under these theories is task-oriented (specific to everyday movements e.g. sitting to standing), which should be intermittent and repetitive. A high level of learning occurs via a child’s problem-solving instead of by the therapist's hands-on facilitation. It is also important that emphasis is placed on family-centered care and treatment in natural environments.
- The mutual goal is usually to increase functional activity, which in turn, decreases disability[20].
These goals should be achieved by[22]:
- Promoting physical milestones of achievement such as sitting, crawling, standing
- Optimizing mobility independence
- Improving balance and coordination via exercise
- Stretching tight muscles via exercise
- Strengthening weak muscles via exercise
- Increasing quality of life and confidence
- Improving endurance and exercise tolerance
References[edit | edit source]
- ↑ Shepherd RB. Physiotherapy in paediatrics. Heinemann Medical Books; 1980.
- ↑ Socci DJ, Bjugstad KB, Jones HC, Pattisapu JV, Arendash GW. Evidence that oxidative stress is associated with the pathophysiology of inherited hydrocephalus in the H-Tx rat model. Experimental neurology. 1999 Jan 1;155(1):109-17.
- ↑ 3.0 3.1 Hydrocephalus Fact Sheet. National Institute of Neurological Disorders and Stroke. Available from: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Hydrocephalus-Fact-Sheet Accessed on: 30 January 2022
- ↑ Sakka L, Coll G, Chazal J. Anatomy and physiology of cerebrospinal fluid. European Annals of Otorhinolaryngology, Head and Neck Diseases. 2011 Dec 1;128(6):359-66.
- ↑ Tully HM, Dobyns WB. Infantile hydrocephalus: a review of epidemiology, classification and causes. European journal of medical genetics. 2014 Aug 1;57(8):359-68.
- ↑ Rekate HL. A consensus on the classification of hydrocephalus: its utility in the assessment of abnormalities of cerebrospinal fluid dynamics. Child's nervous system. 2011 Oct;27(10):1535-41.
- ↑ Rekate HL. A contemporary definition and classification of hydrocephalus. InSeminars in pediatric neurology 2009 Mar 1 (Vol. 16, No. 1, pp. 9-15). WB Saunders.
- ↑ Mori K, Shimada J, Kurisaka M, Sato K, Watanabe K. Classification of hydrocephalus and outcome of treatment. Brain and Development. 1995 Sep 1;17(5):338-48.
- ↑ 9.0 9.1 Corns R, Martin A. Hydrocephalus. Surgery (Oxford). 2012 Mar 1;30(3):142-8.
- ↑ Kiefer M, Unterberg A. The differential diagnosis and treatment of normal-pressure hydrocephalus. Deutsches Ärzteblatt International. 2012 Jan;109(1-2):15.
- ↑ Maller VV, Gray RI. Noncommunicating hydrocephalus. InSeminars in Ultrasound, CT and MRI 2016 Apr 1 (Vol. 37, No. 2, pp. 109-119). WB Saunders.
- ↑ Yamada S, Kelly E. Cerebrospinal fluid dynamics and the pathophysiology of hydrocephalus: new concepts. InSeminars in Ultrasound, CT and MRI 2016 Apr 1 (Vol. 37, No. 2, pp. 84-91). WB Saunders.
- ↑ Peiro JL, Fabbro MD. Fetal therapy for congenital hydrocephalus—where we came from and where we are going. Child's Nervous System. 2020 Aug;36(8):1697-712.
- ↑ Erickson K, Baron IS, Fantie BD. Neuropsychological functioning in early hydrocephalus: Review from a developmental perspective. Child Neuropsychology. 2001 Dec 1;7(4):199-229.
- ↑ Karimzadeh P. Management of hydrocephalus. InHydrocephalus 2012 Feb 24. IntechOpen.
- ↑ NHS CHOICES., 2014. [viewed 15 October 2014] Available from: http://www.nhs.uk/Conditions/Hydrocephalus/Pages/Treatment.aspx
- ↑ Yavuz C, Demırtas S, Calıskan A, Kamasak K, Karahan O, Guclu O, Yazıcı S, Mavıtas B. Reasons, procedures, and outcomes in ventriculoatrial shunts: A single-center experience. Surgical neurology international. 2013;4.
- ↑ 18.0 18.1 18.2 18.3 Lindsay KW, Bone I, Fuller G. Neurology and neurosurgery illustrated e-book. Elsevier Health Sciences; 2010 Sep 9.
- ↑ Bontke CF, Zasler ND, Boake C. Rehabilitation of the head-injured patient. Neurotrauma. New York, NY: McGraw-Hill. 1996:841-58.
- ↑ 20.0 20.1 20.2 Instep Physical Therapy., 2014. [viewed 15 October 2014] Available from: http://www.instepphysio.ca/Neurorehabilitation/Neurorehabilitation/a~3553--c~343920/article.html
- ↑ Karimzadeh, P. 2012. Management of hydrocephalus. Hydrocephalus [online]. Available from: http://www.intechopen.com/books/hydrocephalus/management-of-hydrocephalus-
- ↑ Manchester Physio., 2014 [viewed 15 October 2014] Available from: http://www.manchesterphysio.co.uk/what-we-treat/paediatric-physiotherapy/hydrocephalus.html