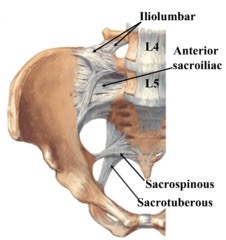
Iliolumbar ligament
Original Editor - Andeela Hafeez
Top Contributors - Andeela Hafeez, Kim Jackson, Esraa Mohamed Abdullzaher, WikiSysop, Wanda van Niekerk, Rishika Babburu, 127.0.0.1, Evan Thomas, Naomi O'Reilly and Lucinda hampton
Description[edit | edit source]
The iliolumbar ligament is a strong band of connective tissue[1] and one of the three vertebropelvic ligaments. The others being the sacrotuberous and the sacrospinous ligaments. They help stabilise the lumbosacral spine on the pelvis.[2]
The iliolumbar ligaments are crucial in supporting the lower lumbar spine; they join the 4th and 5th lumbar vertebrae (L4 and L5) to the iliac bone crest at the back of the pelvis. Injury to this area, fairly common among certain athletes due to the amount of frantic spinal motion involved in many sports, can develop into sacroiliac joint pain and associated problems. The sacroiliac joint is located in the pelvis and helps to keep the spine stable.[3]
Anatomy[edit | edit source]
The portion of the iliolumbar ligament originating from the L-5 transverse process is made up of two bands (anterior and posterior). The anterior band is broad and flat and has two different anatomic varieties. Type 1 originates from the anterior aspect of the inferolateral portion of the L-5 transverse process and fans out widely before inserting on the anterior portion of the iliac tuberosity. Type 2 originates anteriorly, laterally, and posteriorly from inferolateral aspect of the L-5 transverse process and fans out before inserting on the anterior portion of the iliac tuberosity. The posterior band of the iliolumbar ligament originates from the apex of the L-5 transverse process and is fusiform. Just before inserting on the anterior margin and apex of the iliac crest it widens, assuming the aspect of a small cone. This posterior band is thinner than the anterior band, with a smaller insertional base on the iliac crest, which explains its lesser resistance to torsional overloading and also explains the frequency of this painful syndrome. It is probable that the spatial disposition of the iliolumbar ligament influences its anti-torsional role. [4]A study was conducted in routine autopsy, to determine possible racial differences in the structure and attachments of the iliolumbar ligament.The ligament in black people was found to be made up of long single band and in white people two short bands.[5]
Attachments[edit | edit source]
Origin: transverse process of L5[6]
Insertion: deep into ventral margin of iliac crest 6-7cm from midline[6]
The main part of ILL originates from L5 transverse processes.[7] insertion is shielded by the crest dorsally, making it inaccessible to palpation.[6]
Function[edit | edit source]
It plays an important role in restraining movement in the lumbosacral and sacroiliac joints.[8] The iliolumbar ligament strengthens the lumbosacral joint assisted by the lateral lumbosacral ligament, and, like all other vertebral joints, by the posterior and anterior longitudinal ligaments, the ligamentum flava, and the interspinous and supraspinous ligaments.[9]
Pathology/Injury[edit | edit source]
Iliolumbar ligament syndrome, also known as iliac crest pain syndrome, involves inflammation or tearing of the iliolumbar ligament [10]. Soft tissue injury to the iliac insertion of the ligament can be from direct trauma, a fall in which the ligament is pulled at that iliac crest insertion site, or a lifting injury. Pain can be exacerbated by physical activity involving the spine, e.g. twisting or bending, and long periods of sitting can also cause pain[11]. This pain is usually chronic or recurring, unilateral low back pain with a tender point at the posterior iliac crest. The patient points to the most painful spot, which is lateral to the more midline facets and pain is exacerbated with prolonged sitting or standing.[12]
If the initial iliolumbar ligament injury is aggravated, this is generally due to instability in the affected lumbar vertebrae that causes the 4th vertebra to slip and the 5th to move. This can lead to disc herniation. [11]
Technique[edit | edit source]
Palpation[edit | edit source]
The patient is placed in prone lying with the hip joint in slight extension. Pressure is then applied over the ligament as it extends from the transverse process of the fifth lumbar vertebrae to the iliac crest.[13]
Examination[edit | edit source]
- Frequently painful with the FABER's/Patrick test[14]
- Tender point(s) along the posterior iliac crest — must cause concordant low back pain when pressed, otherwise it is just soft tissue pain from overzealous pressure by the examiner.
- NOT painful with facet loading (as facetogenic pain would be)
Treatment[edit | edit source]
- Acute cases may resolve with relative rest, ice, and analgesics.[14]
- Friction massage along the ligament may also be tried
- Chronic cases frequently need injections of local anaesthetic (and sometimes steroid) along the posterior iliac crest.
- When you are pain free, consult your doctor or a physical therapist about an appropriate program of stretching and strengthening exercises for the buttocks and hips. This is crucial in building up strength and support for the lumbar spine in order to prevent similar future injuries, and for maintaining smooth movement in the injured areas. The doctor might also prescribe a course of medication for this purpose.[15]
See also[edit | edit source]
Reference[edit | edit source]
- ↑ 1. Carrino JA, Campbell PD, Lin DC et-al. Effect of Spinal Segment Variants on Numbering Vertebral Levels at Lumbar MR Imaging. Radiology. 2011;259 (1): 196-202. doi:10.1148/radiol.11081511 - Pubmed citation
- ↑ A STUDY OF ITS ANATOMY. DEVELOPMENT AND CLINICAL SIGNIFICANCE. D. K. LUK, H. C. HO. J. C. Y. Franz the Utzit’ersiti’ of Hong Kong, Queen Mart’ Hospital, Hong
- ↑ http://www.medic8.com/healthguide/sports-medicine/iliolumbar-ligament-injury.html
- ↑ Am J Phys Med Rehabil. 1996 Nov-Dec;75(6):451-5.fckLRAnatomy of the iliolumbar ligament: a review of its anatomy and a magnetic resonance study.fckLRRucco V1, Basadonna PT, Gasparini D.
- ↑ Hanson P, Magnusson SP, Sorensen H, Simonsen EB. Differences in the iliolumbar ligament and the transverse process of the L5 vertebra in young white and black people. Acta Anat (Basel). 1998;163(4):218-23. doi: 10.1159/000046501. PMID: 10072570.
- ↑ 6.0 6.1 6.2 http://www.sofmmoo.org/iliac_crest_point_or_ill.htm
- ↑ [CT axial imaging of the iliolumbar ligament and its significance on locating lumbosacral vertebral segments].fckLR[Article in Chinese]fckLRLiu KC1, Xiang GZ, Chen GH, Zhou Y, Cao XQ, Xia JD, Li K.
- ↑ The sacroiliac part of the iliolumbar ligament. L. POOL-GOUDZWAARD, G. J. KLEINRENSINK, C. J. SNIJDERS, C. ENTIUS, R. STOECKART. Departments of " Anatomy and #
- ↑ Palastanga, Nigel; Field, Derek; Soames, Roger (2006). Anatomy and Human Movement: Structure and Function. Elsevier Health Sciences. pp. 332–333. ISBN 0-7506-8814-9.
- ↑ http://www.caringmedical.com/treatment/iliolumbar-syndrome/
- ↑ 11.0 11.1 http://www.medic8.com/healthguide/sports-medicine/iliolumbar-ligament-injury.html
- ↑ frequently painful with the FABERs/Patrick test, though I have not seen this.fckLRTender point(s) along the posterior iliac crest — must cause concordant low back pain when pressed, otherwise it is just soft tissue pain from overzealous pressure by the examiner
- ↑ Palpation of the iliolumbar ligament. Ewan Kennedy, Brendan Cullen, Haxby Abbott, Stephanie Woodley
- ↑ 14.0 14.1 CONDITIONS - MAIN MENU, ILIOLUMBAR SYNDROME / BY CHRISTOPHER FAUBEL, M.D. / ON DECEMBER 12, 2011 AT 8:37 PM / Download article as PDF By Chris Faubel, M.D.
- ↑ http://www.medic8.com/healthguide/sports-medicine/iliolumbar-ligament-injury.html
- ↑ https://www.youtube.com/watch?v=MdnoFW80HNA
- ↑ https://www.youtube.com/watch?v=NaX_kvZEUzs