Parasympathetic System
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
The parasympathetic nervous system (PNS) is one of the two functionally distinct and continuously active divisions of the autonomic nervous system (ANS). It is in opposition to the other, the sympathetic nervous system (SNS). The parasympathetic nervous system predominates in quiet “rest and digest” conditions while the sympathetic nervous system drives the “fight or flight” response in stressful situations. The main purpose of the PNS is to conserve energy to be used later and to regulate bodily functions like digestion and urination[1].
Structure[edit | edit source]
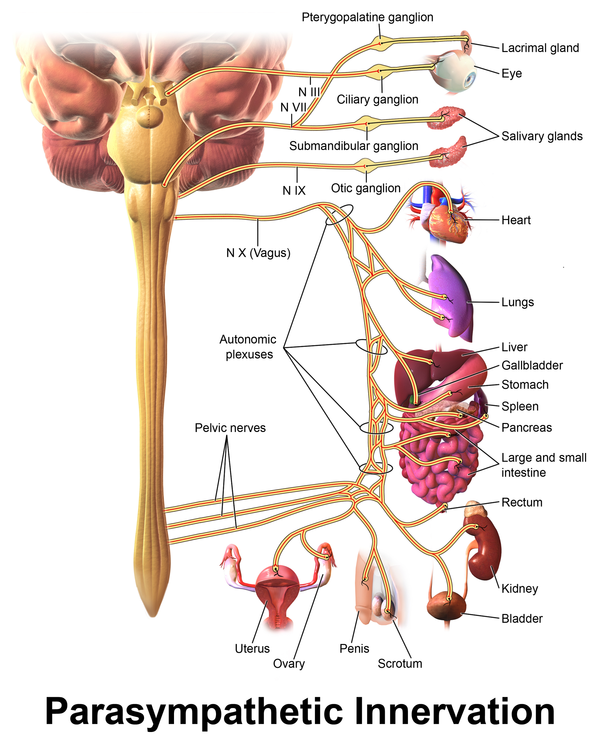
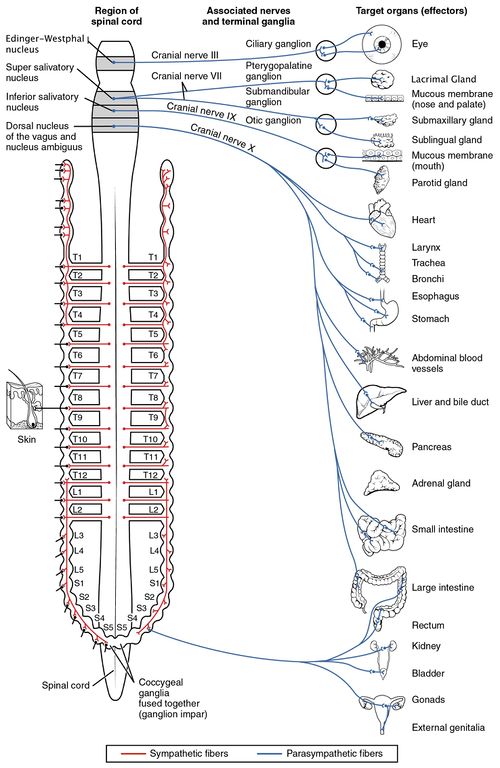
Both divisions of the ANS are comprised of a complex network of pathways responsible for maintaining the physiologic integrity of organs, tissues, and cells. They are composed of pre- and postganglionic neurons that act on effector organs. The parasympathetic nervous system originates from medial medullary sites (nucleus ambiguous, nucleus tractus solitarius, and dorsal motor nucleus) and is modulated by the hypothalamus.[2]
- The preganglionic neurons of the PNS come from brainstem nuclei and the sacral spinal cord (specifically S2-S4).
- The axons of preganglionic PNS neurons are much longer than those of the SNS and synapse with the postganglionic neurons in ganglia at or near the effector organs.
- The very short postganglionic axons then relay signals to the cells of the effector organs.
- Those preganglionic parasympathetic neurons that begin in the brainstem leave the central nervous system (CNS) through cranial nerves, including the oculomotor nerve (III) acting on the eyes, the facial nerve (VII) working on the lacrimal gland, the salivary glands, and the mucous membranes within the nasal cavity, the glossopharyngeal nerve (IX) acting on the parotid gland, and the vagus nerve (X) acting on the viscera of the abdomen and thorax. Amazing fact: The vagus nerve is particularly influential within the PNS as it carries 75% of all parasympathetic fibers.
- The preganglionic fibers coming from the sacral cord join to form pelvic splanchnic nerves, which act on the pelvic cavity viscera[1]
Functions[edit | edit source]
An easy acronym to remember how and where the PSNS works is SLUDD. This stands for:
- Salivation: As part of its rest-and-digest function, the PSNS stimulates production of saliva, which contains enzymes to help your food digest.
- Lacrimation: ie making tears. Tears keep your eyes lubricated, preserving their delicate tissues.
- Urination: The PSNS contracts the bladder, which squeezes it so urine can come out.
- Digestion: The PSNS stimulates the release of saliva to promote digestion. It also enacts peristalsis, or the movement of the stomach and intestines, to digest food as well as release bile for the body to digest fats.
- Defecation: The PSNS constricts the sphincters in the intestine and moves digested food material down the digestive tract so a person can have a bowel movement.
Also the PNS supplied the nerves and blood vessels responsible for the male erection[3]
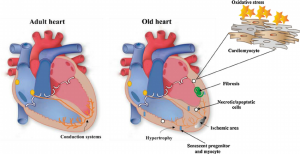
PSNS and the Heart[edit | edit source]
There are a number of special receptors for the PSNS in your heart called muscarinic receptors (M2 receptors). Parasympathetic stimulation of M2 receptors causes decreased heart rate and velocity of conduction through the AV node, inhibiting sympathetic nervous system action. This means they’re responsible for helping to maintain resting heart rate. For most people, the resting heart rate is between 60 and 100 beats per minute (on the other hand, the sympathetic nervous system increases heart rate).
According to an article in the Circulation (AHA)[2] a person’s resting heart rate can be one indicator of how well a person’s PSNS, specifically the vagus nerve, is working. This is usually only the case when a person doesn’t take medications that affect heart rate, like beta-blockers, or have medical conditions affecting the heart. Eg heart failure reduces the response of the parasympathetic nervous system. The results can be an increased heart rate, which is the body’s way of trying to improve the amount of blood it pumps through the body[3].
PSNS and the Lungs[edit | edit source]
In the lungs, parasympathetic stimulation of M3 receptors leads to bronchoconstriction. It also increases bronchial secretions.
- Parasympathetic nerves play an important role in modulating smooth muscle tone and mucus secretion in the airways (through a variety of afferent inputs, from the central nervous system, at parasympathetic ganglia, and on post-ganglionic efferent fibres).
- Abnormalities at any of these sites could, and in some patients probably do, contribute to the abnormalities in smooth muscle contraction and mucus secretion that characterize a number of airway diseases, including asthma. [4]
Parasympathetic/Sympathetic Interactions[edit | edit source]
The sympathetic and parasympathetic nervous systems are not “opposites”; rather, the interactions are complex. A dynamic interaction occurs between them; these interactions are modulated partially by secondary messengers (cAMP and cGMP). The parasympathetic nervous system can inhibit sympathetic nerve traffic presynaptically. Likewise, sympathetic activation can inhibit parasympathetic activation presynaptically.
Vagal “tone” (tonic parasympathetic activation) predominates over sympathetic tone at rest.[2]
- Some of us have stronger vagus activity, which means our bodies can relax faster after a stress. The stronger your vagus response or vagal tone is the stronger your body is at regulating blood glucose levels, reducing the likelihood of diabetes, stroke and cardiovascular disease.
- Low vagal tone, however, has been associated with chronic inflammation and if low vagal tone persists, regulation of inflammation can become less effective.
- Vagal tone can be determined by using an electrocardiogram to measure heart rate[5]
Dysfunction[edit | edit source]
- There are many ways that parasympathetic dysfunction can manifest, given the scope of organs on which it acts.
- Some examples of clinically significant conditions involving the PNS include: sexual dysfunction; priapism; gastrointestinal issues; Horner syndrome; urinary retention; cholinergic toxicity.[1]
- Many people have an underactive parasympathetic nervous system and an overactive sympathetic nervous system[6]. Techniques to stimulate the parasympathetic nervous system include: Yoga[7]; Massage[6]: Tai Chi[8]; Relaxation Breathing[9].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Tindle J, Tadi P. Neuroanatomy, Parasympathetic Nervous System. StatPearls [Internet]. 2020 Jan 11Available from:.https://www.statpearls.com/articlelibrary/viewarticle/26653/ (accessed 30.1.2021)
- ↑ 2.0 2.1 2.2 Olshansky B, Sabbah HN, Hauptman PJ, Colucci WS. Parasympathetic nervous system and heart failure: pathophysiology and potential implications for therapy. Circulation. 2008 Aug 19;118(8):863-71.Available from: https://www.ahajournals.org/doi/full/10.1161/circulationaha.107.760405(accessed 30.1.2021)
- ↑ 3.0 3.1 Healthline PNS Available from: https://www.healthline.com/health/parasympathetic-nervous-system#in-the-heart (accessed 31.1.2021)
- ↑ Sheppard D. Physiology of the parasympathetic nervous system of the lung. Postgraduate medical journal. 1987 Jan 1;63:21-7.Available from: https://pubmed.ncbi.nlm.nih.gov/3321011/(accessed 30.1.2021)
- ↑ Melt Vagus Nerve Available from https://www.meltmethod.com/blog/vagus-nerve/ (accessed 30.1.2021)
- ↑ 6.0 6.1 Review of Pertinent Anatomy and Physiology Sandy Fritz MS, NCTMB, ... Glenn M. Hymel EdD, LMT, in Clinical Massage in the Healthcare Setting, 2008Available from: https://www.sciencedirect.com/topics/neuroscience/parasympathetic-nervous-system(accessed 30.1.2021)
- ↑ Streeter CC, Gerbarg PL, Saper RB, Ciraulo DA, Brown RP. Effects of yoga on the autonomic nervous system, gamma-aminobutyric-acid, and allostasis in epilepsy, depression, and post-traumatic stress disorder. Medical hypotheses. 2012 May 1;78(5):571-9.Available from: https://pubmed.ncbi.nlm.nih.gov/22365651/(accessed 31.1.2021)
- ↑ Lu WA, Kuo CD. The effect of Tai Chi Chuan on the autonomic nervous modulation in older persons. Medicine and science in sports and exercise. 2003 Dec 1;35(12):1972-6.Available from: https://pubmed.ncbi.nlm.nih.gov/14652490/(accessed 31.1.2021)
- ↑ Stromberg SE, Russell ME, Carlson CR. Diaphragmatic breathing and its effectiveness for the management of motion sickness. Aerospace medicine and human performance. 2015 May 1;86(5):452-7.Available from: https://pubmed.ncbi.nlm.nih.gov/25945662/(accessed 31.1.2021)