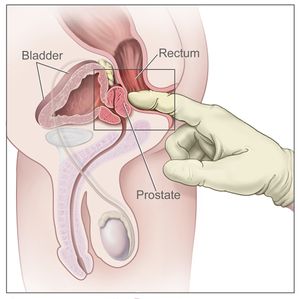
Physiotherapy Assessment After Prostate Cancer
Introduction[edit | edit source]
Physiotherapists are not commonly known for their role in Prostate Cancer (PCa) and the rehabilitation after PCa treatment. The various treatment options for managing PCa all come with disabling side effects and Physiotherapy intervention can be beneficial for men in managing these side effects. It is generally known that physiotherapists can help with pelvic floor muscle problems. Still, there is also a role for physiotherapy in the management of urinary incontinence (UI) and sexual dysfunction.
Adequate post-graduate training in the pelvic floor as well as cancer treatments are essential to manage these men appropriately, and incorrect management can be more damaging than no management at all.
The Therapeutic Relationship[edit | edit source]
Issues around UI and sexual dysfunction can be uncomfortable to talk about, particularly in men. Men may be embarrassed about their sexual dysfunction, and it has been shown that only a fifth of men will discuss issues of sexual dysfunction with their health care practitioner (HCP) after cancer.[1] The development of a strong therapeutic relationship is beneficial in making sure your patient feels comfortable and at ease. Confidentiality and privacy are important for pelvic health patients. A private treatment room, preferably soundproof, will allow the patient to disclose sensitive information. It is also advisable to ask whether the patient would like their partner to come into the room with them and if they do request it, make sure there is enough comfortable seating for everyone.
Education[edit | edit source]
Issues around the pelvic floor, incontinence and sexual dysfunction can be very overwhelming, and education around the condition is very helpful. When sharing information, it is important to remember not to use complex medical jargon, to only give the information the patient would like to know, to use visual aids and pictures to help with the explanations and to give resources to take with them. Certain patients arrive with a referral letter and are very informed about their current situation, and some patients are self-referred. Establishing their base knowledge is a helpful way to make sure you can correct any misinformation and fill in any blanks they may have.
Questionnaires [edit | edit source]
Since only a fifth of men will openly discuss their issues around sexual dysfunction with their HCP[1], the use of questionnaires may provide a non-threatening strategy for a patient to voice any presenting symptoms. Questionnaires may be sent to patients before, or they may complete them in the room with you. The Expanded Prostate Cancer Index Composite (EPIC) and International Index of Erectile Function (IIEF) are both validated instruments that assess general sexual dysfunction, and they were recommended at the Fourth International Consultation for Sexual Medicine in 2015 [2][3]
Subjective Examination/ The Interview[edit | edit source]
Every good assessment starts with a well-structured subjective assessment, and every interview should start with a well-phrased open-ended question such as ”What can I help you with/What has brought you in to see me today”. Make sure not to interrupt your patient as to get the full extent of their situation, and listen carefully to their ideas, concerns and expectations. After carefully listening to their story, the therapist can then start asking more specific questions to gain more insight into their condition.
Current History[edit | edit source]
It is important to gather information about the specific interventions they have had, and all the details of each procedure. Make sure to ask the specifics such as the dosage of radiotherapy that was given, or whether the nerves were spared during a radical prostatectomy. What are the time frames between their diagnosis and their intervention for PCa?
Past History[edit | edit source]
Did they have any pain, erectile dysfunction or incontinence before they were diagnosed with PCa, and if so, how was it managed? (Remember symptoms of erectile dysfunction or problems with urination are often how PCa is picked up). Is there a history of spinal pain, hip pain or pelvic pain? Any Psychiatric conditions, or other medical conditions for which they are being treated?
Medication[edit | edit source]
Ask about all the medication they are taking. Make sure to ask about specific medicines for erectile dysfunction as well as any “herbal” products they may be taking. While the prescription of medication is not within a physiotherapists scope of practice, it is important to know what the patient is taking to be aware of any interaction or side effects.
Bladder[edit | edit source]
Issues with incontinence, urgency, frequency or any other bladder problems frequently occur after prostate cancer treatment.[4]
Generally speaking, post-surgical patients will present with stress incontinence, whereas radiotherapy patients are more likely to present with urge incontinence,[5] frequency, and urgency. There can, however, be some overlap[5] - some patients may present with both stress and urge incontinence, especially if they have had multiple treatment approaches.[4]
Once the type of incontinence after prostate cancer treatment is recognised, the cause of the incontinence must be identified. Stress incontinence is due to a problem with urethral closure, but what is the reason for the problem? Is it because the pelvic floor muscles are too weak and cannot provide the quick contraction needed for the extra closure pressure or is it in spasm and does not have the range of movement required to close the urethra quickly. Urinary frequency means they are going to urinate much more often than normal. Are they experiencing frequency because their bladder capacity has decreased due to decreased compliance of the detrusor muscle and bladder wall after radiation? Or do they have frequency as a learned behaviour because they are afraid of leaking because their urethral closure pressure is poor and they and they are nervous that a fuller bladder will result in leaking (stress incontinence)? It is important to get the full picture as the type of incontinence is just a symptom, and to adequately treat it, the root cause needs to be uncovered.
Some helpful questions.
- Do they leak with activity eg coughing, sneezing, running, jumping or simply just sitting to standing? (stress incontinence)
- When the leak is it a lot or a small dribble?
- How frequently do they urinate? (frequency, urgency)
- Do they get a sudden urge and are unable to delay? (frequency, urgency)
- How much is leaking, how many pads a day are they using?
- Do they use pads just in case? (behavioural)
Objective testing of incontinence may involve continence pad weighing accompanied by strict fluid intake and output measurements over a specific time frame. Weighing of pads is helpful to determine the amount of leakage that is occurring.
Bladder Diary[edit | edit source]
A bladder diary is a helpful tool to identify the patient’s pattern or urination as well as leakage. This very useful assessment tool identifies all the food and fluids a patient may take in, and the consequence thereof. It also helps to keep track of the number of incontinence pads used every day.
Sexual Dysfunction. [edit | edit source]
Sexual dysfunction after Prostate Cancer Treatment is very common, and men can be uncomfortable talking about their specific issues.[1] The use of the EPIC and IIEF is particularly helpful to open up the dialogue about what type of dysfunction they are experiencing.[6] These questionnaires do not address every aspect of male sexual function, and there is a collection of sexual dysfunctions known as the neglected side-effects that should also be screened for.[7] Again similar to incontinence, the full clinical picture is needed because there are a host of causes that can result in the various dysfunctions, and they are the key to being able to rehabilitate these men.
Sexual dysfunction symptoms to screen for
- Erectile dysfunction (ED)
- Sexual interest dysfunctions
- Sexual arousal dysfunctions
- Premature/rapid/early or delayed ejaculation
- Anejaculation
- Orgasmic dysfunction
- Sexual aversion disorder
- Priapism (prolonged erection of the penis)
- Peyronie’s disease (a painful curvature of the penis)
- Orgasm-associated incontinence
- Urinary incontinence in relation to sexual stimulation
- Altered perception of orgasm,
- Orgasm associated pain
- Penile shortening
- Penile deformity
Dietary Habits[edit | edit source]
Dietary habits play a role in both bladder and bowel health. The volume of fluid intake affects bladder health. Men may restrict fluids to try and prevent leaking, but this can result in more concentrated urine that can irritate the bladder and subsequently cause frequency, urgency or urge incontinence. Certain fluids can also irritate the bladder lining such as caffeine, citric juices and alcohol.
A bladder diary may be handy in this instance to monitor volumes as well as types of fluid intake.
Pelvic Floor Pain[edit | edit source]
Pain can occur after treatment for PCa. Post-operative pain after a radical prostatectomy typically resolves, however, pain can become persistent for a few reasons. Continued spasm in the pelvic floor muscles can result in persistent nociceptive pain. Or injury to the surrounding nerves can result in neuropathic pain. Focused questioning around the type of pain, area of pain, aggravating and easing factors as well as a 24-hour pattern can help to determine the source of the painful symptoms.[3]
Objective Assessment or Physical Examination[edit | edit source]
The physiotherapy physical examination is important to assess the pelvic floor function. As a physiotherapist, you want to determine if the pelvic floor has adequate muscle strength, length and endurance to function optimally. As mentioned above, it is imperative to determine the root cause of the symptoms. Your objective examination should be based on your findings from the interview and used to determine the origins of the symptoms.
There are a few ways to assess the male pelvic floor objectively.
External Observation[edit | edit source]
External observation of the scrotum, testicles and penis during a pelvic floor muscle (PFM) contraction can be observed. This allows the Physiotherapist to visualise if there is any bearing down during contraction (incorrect technique) or whether there is a lifting action during contraction (correct technique). In men, a correct pelvic floor contraction will result in a lifting action of the penis.[3]
Digital Rectal Examination[edit | edit source]
A per rectal assessment/digital rectal examination (DRE) can be performed to evaluate the effectiveness of pelvic floor muscle contraction as well as whether there are any tight or painful structures. This is a relatively invasive option and can be quite painful, especially in patients post radical prostatectomy.[8] For urinary incontinence assessment, a DRE may also not be reliable in assessing the muscles that are primarily responsible for urethral closure pressure so may not be as helpful for urinary incontinence.[9]
An alternative to DRE is real-time ultrasound, and this can be used as an alternative method when DRE is contraindicated.[10] For patients after radiation that are experiencing tightness and spasm of the pelvic floor, a DRE can be helpful to feel the soft tissue and muscles. Men are often reluctant to have a DRE which can be associated with a sense of shame [8]
Real-Time Ultrasound Testing (RTUS)[edit | edit source]
Transabdominal RTUS is a valid and reliable method objective method of measuring the male pelvic floor functioning.[11] An ultrasound (US) probe is placed on the lower abdomen supra-pubically in a mid-sagittal location. A clear transverse image of the bladder is seen if the bladder has enough urine in it, and a bladder base (floor) lift, in a cephalad direction, is seen as a correct action for the PFM[10]. Specific components of PFM cannot be identified with this method. A limitation of RTUS is that the patient requires the bladder to be relatively full of urine to be able to assess the movement thereof, which can be a problem for men with more severe continence problems [12]
Transperineal RTUS is another method used that is slightly more complicated. The US probe is placed on the perineum, mid-sagittal between the anus and the penis. Sagittal images of the bladder are obtained. It is possible with this method to assess and focus on anterior structures when it comes to teaching correct PFM contractions.[11]
Another limitation of real-time ultrasound of the pelvic floor is that the absence of movement on ultrasound may be from a lack of mobility eg tightness or spasm of the pelvic floor muscles rather than just weakness or absence of contraction.[13] This is another example in pelvic health physiotherapy where it is so important to put the full clinical picture of the patient together and not only look at isolated findings.
Putting It All Together[edit | edit source]
Assessing a man for dysfunction in the pelvic region is complex. Putting together all the symptoms and findings into a comprehensive clinical picture is challenging and can take a fair amount of skill and practice. The baseline knowledge of pathology, physiology and anatomy around the pelvic floor, bladder and bowel is essential to understand the clinical picture and formulate a comprehensive management plan.
Additional Resources[edit | edit source]
WCPT 2017 Focused Symposium on Men's Health Physiotherapy
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Charif AB, Bouhnik AD, Courbiere B, Rey D, Préau M, Bendiane MK, Peretti-Watel P, Mancini J. Patient discussion about sexual health with health care providers after cancer—A national survey. The journal of sexual medicine. 2016 Nov 1;13(11):1686-94.
- ↑ Salonia A, Adaikan G, Buvat J, Carrier S, El-Meliegy A, Hatzimouratidis K, McCullough A, Morgentaler A, Torres LO, Khera M. Sexual rehabilitation after treatment for prostate cancer—part 1: recommendations from the Fourth International Consultation for Sexual Medicine (ICSM 2015). The journal of sexual medicine. 2017 Mar 1;14(3):285-96.
- ↑ 3.0 3.1 3.2 Jane O’Brien Franczak Pelvic Physical Therapy Distance Journal Club . Available at: https://pelvicptblog.files.wordpress.com/2020/03/bft-pop-journal-club-outline-final.pdf
- ↑ 4.0 4.1 Hodges PW, Stafford RE, Hall L, Neumann P, Morrison S, Frawley H, Doorbar-Baptist S, Nahon I, Crow J, Thompson J, Cameron AP. Reconsideration of pelvic floor muscle training to prevent and treat incontinence after radical prostatectomy. InUrologic Oncology: Seminars and Original Investigations 2019 Dec 25. Elsevier.
- ↑ 5.0 5.1 Shabataev V, Saadat SH, Elterman DS. Management of erectile dysfunction and LUTS/incontinence: the two most common, long-term side effects of prostate cancer treatment. Can J Urol. 2020;27(27 Suppl 1):17-24.
- ↑ Heidenreich A, Bellmunt J, Bolla M, Joniau S, Mason M, Matveev V, Mottet N, Schmid HP, van der Kwast T, Wiegel T, Zattoni F. EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and treatment of clinically localised disease. European urology. 2011 Jan 1;59(1):61-71.
- ↑ Frey AU, Sønksen J, Fode M. Neglected side effects after radical prostatectomy: a systematic review. The journal of sexual medicine. 2014 Feb 1;11(2):374-85.
- ↑ 8.0 8.1 Romero FR, Romero KR, Brenny Filho T, Pilati R, Kulysz D, de Oliveira Júnior FC. Reasons why patients reject digital rectal examination when screening for prostate cancer. Archivos espanoles de urologia. 2008;61(6):759-65.
- ↑ Frawley HC, Galea MP, Phillips BA, Sherburn M, Bø K. Reliability of pelvic floor muscle strength assessment using different test positions and tools. Neurourology and Urodynamics: Official Journal of the International Continence Society. 2006;25(3):236-42.
- ↑ 10.0 10.1 Nahon I, Waddington G, Adams R, Dorey G. Assessing muscle function of the male pelvic floor using real time ultrasound. Neurourology and urodynamics. 2011 Sep;30(7):1329-32.
- ↑ 11.0 11.1 Stafford RE, Ashton-Miller JA, Constantinou CE, Hodges PW. Novel insight into the dynamics of male pelvic floor contractions through transperineal ultrasound imaging. The Journal of urology. 2012 Oct;188(4):1224-30.
- ↑ Milios JE. Therapeutic interventions for patients with prostate cancer undergoing radical prostatectomy: A focus on urinary incontinence, erectile dysfunction and Peyronie’s disease. Thesis Document University of Western Australia. 2019
- ↑ Stafford RE, Coughlin G, Lutton NJ, Hodges PW. Validity of estimation of pelvic floor muscle activity from transperineal ultrasound imaging in men. PLoS One. 2015;10(12).