Plantar Fibromatosis
Original Editor - Anja Vanroelen
Top Contributors - Anja Vanroelen, Laura Ritchie, Kirenga Bamurange Liliane, Kim Jackson, Lucinda hampton, Admin, WikiSysop, 127.0.0.1 and Evan Thomas
Introduction[edit | edit source]
Plantar fibromatosis is a benign fibroblastic, connective tissue proliferative disorder of the superficial plantar aponeurosis of the foot, more specifically on the medial plantar side of the foot arch and on the forefoot region. It belongs to a family of similar diseases ie Peyronie (penile fibromatosis) and Dupuytren.[1]
- Presentation is slow, and patients usually only present when the disease becomes locally aggressive, causing pain and swelling in the medial non-weight bearing plantar surface of the feet.[1]
- Phases: Proliferative phase: Nodular fibroblastic proliferation; Active phase: Collagen synthesis and deposition; Mature phase: Reduced fibroblastic activity and collagen maturation.[2]
Etiology[edit | edit source]
The exact etiology leading to plantar fibromatosis is unknown. It seems to have a multifactorial etiology, including congenital and traumatic causes as well as prolonged immobilization followed by trauma.[1][3][4] Patients with the Dupuytren's contractures, diabetes mellitus, epilepsy, alcoholics with liver disease, stressfull work and keloids, stressfull work have a higher risk to develop the disease of Ledderhose and/or a Peyronie's disease.[3][5]
Epidemiology[edit | edit source]
Plantar fibromatosis is rare, affecting less than 200,000 people in the United States. It typically presents in middle-aged patients, most commonly in the 4th and 5th decades of life. [1] It can be seen in both children and adults, although there is a recognized male predilection (M: F of 2:1), with an increased incidence with advancing age.[6][7]
Characteristics/Clinical presentation [edit | edit source]
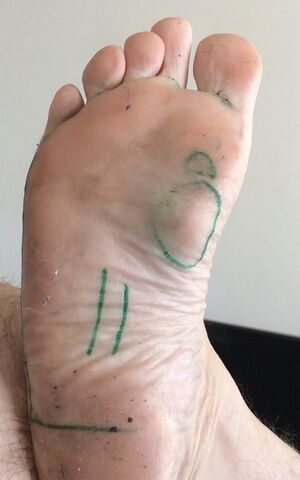
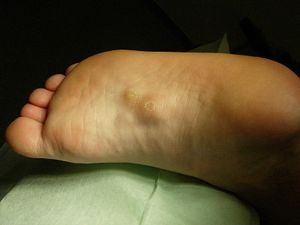
Nodules or masses of plantar fibromatosis are usually located in the middle to the medial aspect of the plantar arch, possibly extending to involve the skin or deep structures of the foot. Lesions may be symptomatic because of a mass effect or invasion of adjacent muscles or neurovascular structures. In contrast to Dupuytren disease, flexion deformities usually do not occur and patients frequently have normal radiographs. [3][6]
Patients commonly present symptoms after experiencing increased pain in the plantar surface of the foot after long walks. Specific activities, eg long walks, standing for long periods, specific shoe wear, and walking barefoot, can exacerbate the symptoms. The diagnosis is made clinically by evaluating the plantar surface of the foot for fibromas.
The foot should be examined for tenderness over bony prominences and tendon insertions. Hindfoot alignment, as well as the presence of an Achilles or gastrocnemius contracture, should be evaluated as these can contribute to symptoms.[1]
Differential Diagnosis[edit | edit source]
Plantar Fibromatosis is sometimes associated with other diseases such as:
• Peyronie's disease
• Knuckle pads [8]
Some others main differential diagnoses include: [9]
• Chronic rupture of the plantar fascia
Diagnostic procedures[edit | edit source]
Lesions, extension, characteristics, structures involved and local recurrence can be identified on the following scans:[3][2]
- Ultrasound
- MRI: Well-defined nodule tcontinuous with the plantar fascia; Low signal intensity on T1-weighted sequences; Low to intermediate signal intensity on T2-weighted sequences.
- CT scan: Used for tissue comparison; identify tissue mass (non-specific) in characteristic area; attenuation equal or higher than in skeletal muscles.
Physiotherapy management[edit | edit source]
Conservative measures are initiated first which include physiotherapy. In patients presenting with no or mild pain can be managed very well conservatively in the form of padded shoes with soft insole or tailored insoles which will redistribute the weight from the prominent nodules.
The treatment of a mild case of Ledderhose disease consists of:[7][10]
- Massage using cortisone cream
- Gentle passive stretching of the retracted structures
- Isometric exercises of the toe extensors
- Symptom relief in the form of padded shoes with soft insole or tailored insoles which will redistribute the weight from the prominent nodules.
- Extra Corporeal Shock Wave Therapy (ESWT). Originally stems from its effective use as a treatment in Peyronie. The original protocol for shock wave therapy was described using 2000 pulses at a frequency of 3 Hz at 7-day intervals for 2 weeks. This study found a softening of nodes in the patients who chose to undergo this treatment option.
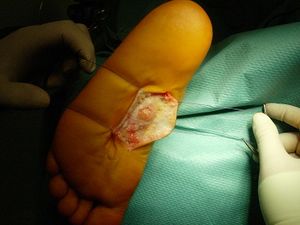
Post Surgical Intervention: After surgical intervention: non-weight bearing for 3 weeks until the incision heals. After healing has occurred, full weight-bearing is allowed. Rehabilitate foot as assessment dictates.
The wound healing phase (8-15th day) will consist of: mobilization of the free articulations, circulatory and scar tissue massage (although there is only weak evidence for massage in scar management), lymphatic drainage, pneumatic/air pressure therapy, recovery of the joint capsulas, cartilage and muscles of the toes (slow and painless passive mobilization, active mobilization, work on the posture extension), ionization, lasers, ultrasound if there is a bad wound healing.
Calf muscle and/or plantar fascia-specific stretching can be applied to provide short-term (2-4 months) pain relief and improvement in calf muscle flexibility. The dosage for this stretching can be either 3 times a day or 2 times a day utilizing either a sustained (3 minutes) or intermittent (20 seconds) stretching time, as neither dosage produced a better effect.[11][12]
The phase after the wound healing will consist of: circulation and scar massage, bath of hot water or paraffin with active movements, total recovery of the articular amplitudes (by using analytic and global active-passive exercises and postural extension if needed with a dynamic brace), recovery of the muscle force (manually and later on with growing mechano-therapy appliances).
There is minimal evidence to support the use of manual therapy to provide short-term (1 to 3 months) pain relief and improved function. Suggested manual therapy procedures include anterior and posterior glides of tarsometatarsal, metatarsalphalangeal and interphalangeal joints. [11]
This video explains the different causes of Plantar fibromatosis such as injury, trauma and other unsure causes. It also explains that PF is usually diagnosed by examination and by taking an MRI. The different treatment used are cortisone injections, use of orthotics, Physiotherapy Management and Surgery as last option although it has a high risk of recurrence.<be>
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Meyers AL, Marquart MJ. Plantar fibromatosis. InStatPearls [Internet] 2020 Jun 30. StatPearls Publishing.
- ↑ 2.0 2.1 Griffith JF, Wong TY, Wong SM, Wong MW, Metreweli C. Sonography of plantar fibromatosis. American Journal of Roentgenology 2002;179(5):1167-72.
- ↑ 3.0 3.1 3.2 3.3 Murphey MD, Ruble CM, Tyszko SM, Zbojniewicz AM, Potter BK, Miettinen M. Musculoskeletal fibromatoses: radiologic-pathologic correlation. Radiographics 2009;29(7):2143-83.
- ↑ Hoeber PB. Tumors of the soft somatic tissues and bone. In: Pack GT, Ariel IM. Treatment of cancer and allied diseases. Volume VIII, 1964. p. 8-14.
- ↑ Knobloch K, Vogt PM. High-energy focussed extracorporeal shockwave therapy reduces pain in plantar fibromatosis (Ledderhose’s disease). BMC research notes 2012;5(1):542.
- ↑ 6.0 6.1 Radiopedia Plantar fibromatosis Available:https://radiopaedia.org/articles/plantar-fibromatosis (accessed 16.5.2022)
- ↑ 7.0 7.1 Walker EA, Petscavage JM, Brian PL, Logie CI, Montini KM, Murphey MD. Imaging features of superficial and deep fibromatoses in the adult population. Sarcoma 2012.
- ↑ Fausto de Souza, D. et al. (2010). Ledderhose Disease: An Unusual Presentation. The journal of Clinical and Aesthetic Dermatology, 3. Level of evidence: 3B
- ↑ Young JR, Sternbach S, Willinger M, Hutchinson ID, Rosenbaum AJ. The etiology, evaluation, and management of plantar fibromatosis. Orthopedic Research and Reviews. 2019;11:1.
- ↑ Xhardez Y. Vade-mecum de kinésithérapie et de rééducation fonctionnelle (5e édition). Prodim: Paris, 2002.
- ↑ 11.0 11.1 Eugene G. McNally, Shilpa Shetty. (2010). Plantar Fascia: Imaging Diagnosis and Guided Treatment. Department of Radiology, Nuffield Orthopaedic Centre, Oxford, Oxfordshire, United Kingdom. Level of evidence 1B
- ↑ Haedicke, G.J., Sturim, H.S. (1989). Plantar fibromatosis: an isolated disease. Plast Reconstr Surg.
- ↑ Donald Pelto. Plantar Fibroma . Available from: http://www.youtube.com/watch?v=pjoLXaeD4E0 [last accessed 11/01/17]