Chronic Obstructive Pulmonary Disease Rehabilitation Class
Original Editor - Sheena Lynch, Laura McCabe, Diane Smith, Mark Prior, James Lee, Laura McCabe as part of the Queen Margaret University's Current and Emerging Roles in Physiotherapy Practice Project
Top Contributors - Sheena Lynch, Laura McCabe, Mark Prior, Diane Smith, James Lee, Kim Jackson, Admin, 127.0.0.1, Rachael Lowe, Evan Thomas and Lucinda hamptonIntroduction[edit | edit source]
COPD is a chronic condition which can drastically alter a patient’s wellbeing and currently costs the NHS £1 billion annually. We believe that by implementing community based pulmonary rehabilitation programmes there will be increases in patients’ quality of life in addition to substantial long-term savings within the NHS. This is further detailed throughout the business case
Executive Summary [edit | edit source]
This business case plans to propose SecondWind, a pulmonary rehabilitation class for patients with Chronic Obstructive Pulmonary Disease (COPD). We are proposing that SecondWind runs twice weekly in a sports centre such as Edinburgh Leisure Meadowbank Complex. It will have a unique top-up component allowing participants to return if they feel as though they require further assistance in order to ensure adherence to exercise. This is essential in our programme as it is important for participants with COPD to add regular exercise into their lifestyle to maximise the benefits offered by pulmonary rehabilitation.
COPD is a long-term condition, which is becoming more prevalent in the UK. Currently, the NHS is spending £1 billion annually on COPD. The prevalence of COPD is largely influenced by age therefore, in conjunction with the current trend of an aging population it is probable to see a parallel rise in the cost of COPD to the NHS.
Due to the economic downturn and future spending freeze expected to occur in the NHS, there is a need for efficient utilisation of current resources. SecondWind will allow for the cost effective treatment of multiple participants in an accessible setting which is likely increase uptake and adherence of pulmonary rehabilitation. Along with the direct benefits participants will receive, there will be long-term savings within the NHS. This will occur due to decreased exacerbations, readmissions as well as reduced GP and practice nurse visits.
It is projected that starting up costs will be £2,127.61 with a yearly cost per participant of £449.86. To evaluate the effectiveness of the program, we propose to explore validated outcome measure to address patient improvements and health care utilisation costs.
Mission Statement:
Our mission is to provide a safe, cost effective and patient centered pulmonary rehabilitation programme in the community for individuals with COPD. SecondWind will provide an evidence base programme delivered by qualified and experienced cardiorespiratory staff. We plan on offering an exclusive top-up programme to help ensure adherence to long-term lifestyle changes. SecondWind will not only provide crucial benefits for participants but it will also decrease the financial demands of COPD on the already restricted NHS budget.
Background Information[edit | edit source]
Disease Process[edit | edit source]
Chronic obstructive pulmonary disease (COPD) describes a number of conditions including chronic bronchitis and emphysema, where people have difficulty breathing due to long-term damage to their lungs. Individuals with COPD will often have a mixture of both chronic bronchitis and emphysema. COPD leads to permanent damaged airways, which causes them to become narrower making it difficult for air to go into and out of lungs [1]. Chronic bronchitis is defined as inflammation of the bronchi, which increases muscus production in airways and, thus, causes obstruction. Emphysema involves the alveoli losing their elasticity and support which causes them to narrow and trap air in lungs during expiration. This also causes problems with oxygen delivery, which may result in increased work of breathing and shortness of breath. The pathophysiological changes that occur to the lungs depends on the nature of the patients disease [2].
Causes[edit | edit source]
The largest single cause of COPD is cigarette smoking [2]. The likelihood of developing COPD increases the more the patient smokes and the longer they have been smoking [1]. Smoking cessation will gradually reduce the patient's chances of getting COPD as it slows down the process. Other potential causes of COPD included:
- Exposure to air pollution
- Exposure to fumes or particles at work, for example, welding fumes or coal dust
- Alpha-1-antitrypsin deficiency, a genetic condition
Common symptoms of COPD are: cough, sputum production, shortness of breath, fatigue and decreased exercise tolerance [1].
Rational for Change[edit | edit source]
Pulmonary rehabilitation is an exercise programme combined with educational information. It can increase an individual’s exercise capacity, mobility and self-confidence leading to an increased quality of life [1]. Exercise has been shown to improve quality of life, control symptoms and decrease exacerbations and hospital re-admissions [3].
A top-up component has been included in the SecondWind programme, whereby participants can return to the class for a shortened period of time if they need further motivation or assistance. This has been included as a unique feature of our class to help improve uptake and adherence to exercise. Pulmonary rehabilitation based in a community sports facility may increase adherence, as it may be more accessible and individuals may feel less anxious about a class held in a community setting as opposed to a hospital.
The following is a further indepth look at the importance of pulmonary rehabiliation programmes in the community:
Impact on QoL[edit | edit source]
There is a large impact on quality of life for individuals living with COPD including, but not limited to;
- Decreased exercise tolerance
- Decreased ability to carry out activities of daily living (ADLs)
- May have a reduced income due to the patient’s inability to work (loss of productivity) [1].
Willgoss et al. [4] illustrated that many people living with COPD also suffer from
- Anxiety
- Feelings of isolation
- Decreased social participation
- Inability to carry out ADLs which all affect quality of life
Stahl et al. [5] determined that health related quality of life (HRQL) in COPD deteriorates in parallel with lung function impairment; HRQL decreases with increasing severity of the disease. They also found that HRQL deteriorates with increasing age.
Epidemiology Of COPD[edit | edit source]
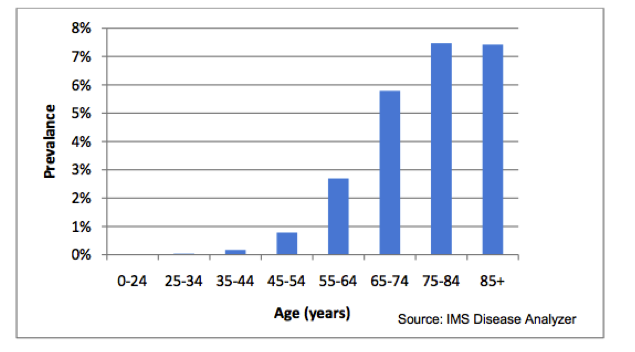
COPD is the 5th largest killer in the UK. It is the 2nd most common cause of emergency admission to hospital and it is the most costly inpatient condition treated by the NHS [1]. An estimated 3 million people have COPD in the UK although approximately 2 million of this estimation remain undiagnosed [6]. COPD affects more men than women, although rates of women with COPD are climbing [1]. The rate of COPD in the population is estimated at between 2% and 4% and the diagnosed prevelance of COPD in England alone is 1.6%. The prevalence of COPD is largely influenced by age. The diagnosed prevelance for individuals aged 45-54 is < 1% which increases to > 5% for individuals aged 65+ [6]. The mortality rate of COPD in the UK is estimated at 23,000 people per year.
Cost To NHS[edit | edit source]
In the UK the NHS is currently spends approximately £1 billion annually on COPD. It costs nearly 10 times more to treat severe COPD than the mild disease [7].
Current Service and Achievements[edit | edit source]
There are currently many guidelines and initiatives for COPD; NICE guidelines [8], British Thoracic Society guidelines [9], GOLD: global initiative for COPD [10], NHS improvement . All of these guidelines discuss the importance of smoking cessation and pulmonary rehabilitation. There is currently an NHS stop smoking service available in Lothian that offers one-to-one support. Hospital based pulmonary rehabilitation programmes are also available throughout the UK.
As of 2009, over 1,400 people have been referred to pulmonary rehabilitation in Lothian with a drop out rate of 25% [6]. There is clear evidence accoring to a Lothian pulmonary rehabilitation service audit [3] that the majority of patients who engaged in pulmonary rehabilitation show immediate benefits and sustained benefits of a year after the program. These benefits include:
- an increased exercise tolerance (improvements have shown to be sustrained at 1 year follow up)
- significant improvements to HRQL
- reduction in exacerbation
- reduction in number of admissions
The evidence therefore suggests there are numerous clinical benefits associated with pulmonary rehabilitation [3].
Evidence to Support Pulmonary Rehabilitation[edit | edit source]
“The opportunity for structured, on-going exercise with peer and professional support, in a suitable venue, is perceived as important to people with COPD in facilitating a physically active lifestyle following pulmonary rehabilitation” [11].
The National Institute for Clinical Excellence (NICE) 2010 guidelines for COPD management [8] states that there is evidence to show that pulmonary rehabilitation:
- Elicits meaningful improvements to health-related quality of life, functional and maximum exercise capacity in COPD patients
- Reduces dyspnoea
- Shows a trend towards decreased total hospitalisation days and total incidences of hospitalisation required for COPD patients in the years following a comprehensive pulmonary rehabilitation versus the year prior to rehabilitation
- Improves cost-effectiveness in terms of cost per quality of life-adjusted year (QALY) gained versus conventional treatment.
- Has a significantly greater effect on the above outcomes than bronchodilator drugs [8]
Ries et al. [12] reported that pulmonary rehabilitation brings about improvements in health-related quality of life and functional and maximal exercise capacity. In addition, they also report that it has a positive impact on dyspnoea, which, as previously mentioned, is a common problem for individuals with COPD [12]. British Thoracic Society Standards of Care Subcommittee on Pulmonary Rehabilitation [9] also support the finding that pulmonary rehabilitation reduces dyspnoea. Although there is mixed findings in regards to the effect of pulmonary rehabilitation, trends in study findings suggest that it reduces total hospitalisations [8] and significantly improved number of days in hospital [13]. It has also been shown that, when compared to traditional COPD treatment, pulmonary rehabilitation showed improved cost-effectiveness in terms of cost per quality of life-adjusted year (QALY) gained. This is an important measure in this population as quality of life has been shown to decrease with COPD [14]. In addition, NICE states that participation in pulmonary rehabilitation has a greater effect than use of bronchodilators in people with COPD [8].
Analysis of the Needs for COPD Exercise Rehabilitation Classes[edit | edit source]
NHS Budget Changes[edit | edit source]
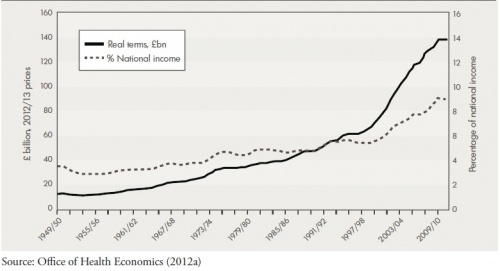
- According to Crawford & Emmerson [15], real public spending* on the NHS has increased faster than economy-wide inflation since the 1950s – from 3.5% of the national income in fiscal year 1949-1950 to 7.9% in fiscal year 2007-2008, prior to the financial crisis and subsequent recession.
- * Spending which has been adjusted for the effect of the general level of inflation in the economy.
- The fastest rate of average growth on record was 6.4% per annum between fiscal years 1996-1997 and 2009-2010. In the 2010 Spending Review, the UK government committed to protecting NHS funding for that year to ensure adequate healthcare delivery to UK citizens. However, a freeze for NHS spending has been planned for fiscal years 2011-2012 to 2014-2015. If implemented, it will be the tightest 4-year funding period on record for the past 50 years [15].
- For spending on public services to increase total public spending must increase proportionate to national income over the same period. As can be seen from the above, changes to NHS and other public service funding are highly dependent on the actual economic climate of a given period – if average growth dips below forecasts, the amount available for public spending will be even lower [15].
Scotland Budget[edit | edit source]
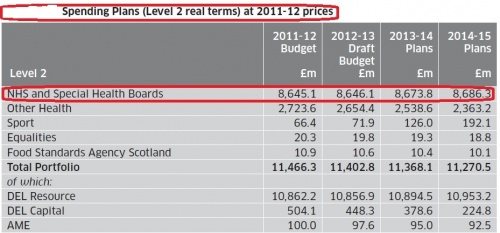
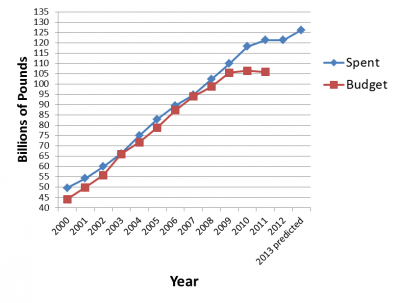
In Scotland, the current spending review and latest draft budget includes plans to freeze real NHS spending between fiscal years 2012 to 2015, as can be seen from Figure 3 [16].
- According to a report to the Holyrood health committee by Dr Andrew Walker of the University of Glasgow, NHS boards across Scotland have been directed to ensure 3% efficiency savings in fiscal year 2012-2013. Greater Glasgow and Clyde region leads the pack at a savings target of £58 million, with Lothian coming second at £27 million. Scottish Labour alleges that funding cuts have targeted mostly frontline staff, with more than 4500 NHS jobs cut since 2009, of which 2000 were nurses [17]
From the above, it may be seen that, across the UK, the NHS is experiencing a drastic shortage of resources with which to deliver healthcare. This shortage is being felt particularly in Scotland, where NHS boards nation-wide have been directed to make savings above the national average of 1.7% required to conform to spending plans. As a result, frontline care providers are being laid off, and it may be surmised that those who remain must take on even heavier workloads than before to compensate for the shortfall in personnel. As such, the NHS and its staff must make more efficient use of dwindling resources than ever before to ensure adequate healthcare delivery to those in need. By implementing our proposed community pulmonary rehabilitation class we can treat more paitents with less staff while contributing to long-term savings within the NHS due to reduced hospital readmissions
COPD Cost to NHS and Society[edit | edit source]
COPD in the United Kingdom[edit | edit source]
COPD is a major contributor to healthcare costs UK-wide. It has been estimated that the number of COPD sufferers in the UK ranges between 900,000 to 3 million [18].
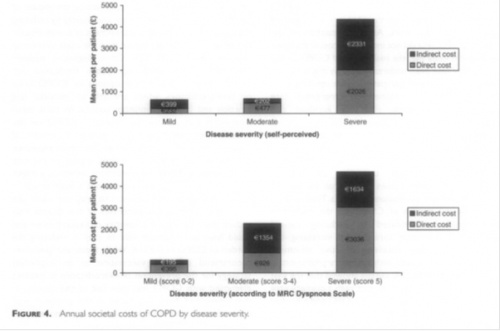
In 2003, the UK segment of the Confronting COPD survey estimated that the average annual direct costs per patient to the healthcare system came to £819.42, while average indirect costs to society such as paid sick leave, lost productivity and additional burden of care came to £819.66. UK-wide, 24 million lost working days, amounting to 9% of all certified sick leave, are attributable to COPD – nearly 20 times that of asthma.. 24% of all COPD patients were completely unable to work due to the disease, while 9% were limited in their ability to work and 5% had to miss work because of the disease. Furthermore More than 44% of COPD patients in the UK were found to be below retirement age. This figures illustrate the significant impact COPD has on the national economy [19].
As can be seen the later stages of COPD cause an across-the-board increase in direct and indirect costs, the former being attributable mostly to hospitalisation.
There has been a increase in prevalence in COPD of 25% in males and 69% in females from 1990 to 1997 [19], if this trend continues in the future or prevalence remains the same with an increasing population, the burden of COPD on the healthcare system will only increase, particularly as the population ages, allowing COPD to progress to its later and more care-intensive stages which has a greater cost to the NHS.
COPD in Scotland[edit | edit source]
According to Audit Scotland’s 2007 report [20], there are roughly 100,000 known cases of COPD in Scotland as of 2005, with a 33% increase in prevalence predicted for the next 20 years. COPD is the 3rd most common reason for hospital admission in Scotland, with 19% of patients readmitted more than once and 16% at least twice more, observed from 2003-2004 [20].
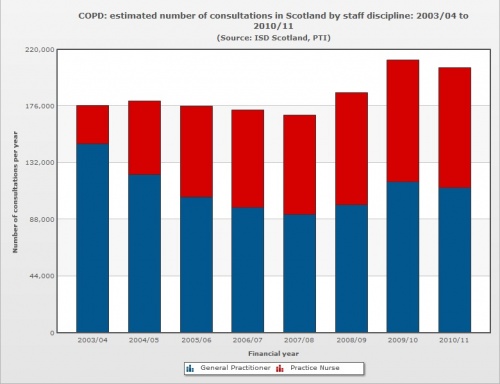
As of the end of 2010, the number of known cases in Scotland appears to have held remained relatively stable, ending the year at 89,170 documented cases [21]. COPD-related healthcare utilisation showed a definite rise from 2007 2010 as illustrated by figure 5 [21]
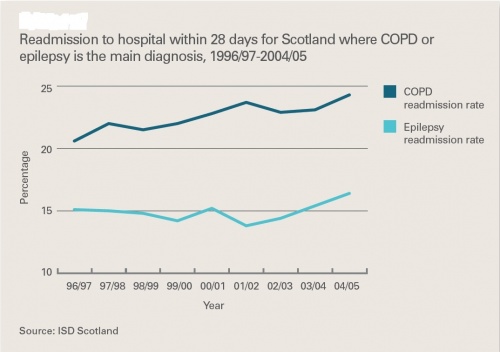
COPD’s direct per-annum cost to NHS Scotland is estimated at £100 million. inpatient stays have shown a steady downward trend, however, readmission rates have been rising over the same period, as seen in Figure 6 [20].
NICE COPD guidelines [8] suggest that average COPD patient per-annum costs to the NHS scale with severity accordingly:
- Mild COPD: £150
- Moderate COPD: £308
- Severe COPD: £1307
Figure 6: Readmission to hospital within 28 days for Scotland where COPD or epilepsy is the main diagnosis, 1996/97 to 2004/05 [20]
Based on the national average expense of £1036 per paitent per year it suggest that most known patients in Scotland have moderate- severe COPD. This cost suggests that there is evidence for pulmonary rehabilitation to potentially generate large indirect savings by decreasing readmission rates, thus, freeing up hospital beds [20].
Guidelines [edit | edit source]
National Clinical Guideline Centre, 2010 [edit | edit source]
The National Institute for Clinical Excellence (NICE) states in its 2010 guidelines for COPD management [8] that pulmonary rehabilitation is evidentially sound for:
- Eliciting meaningful improvements to health-related quality of life, functional and maximum exercise capacity in COPD patients
- Reducing dyspnoea
- Decreasing total hospitalisation days and total incidences of hospitalisation required for COPD patients in the years following a comprehensive pulmonary rehabilitation versus the year prior to rehabilitation
- Cost-effectiveness in terms of cost per quality of life-adjusted year (QALY) gained versus conventional treatment.
- Having a significantly greater effect on the above outcomes than bronchodilator drugs
It was also recommended that referral to pulmonary rehabilitation be considered at all stages of disease progression; as soon as symptoms are present and not at predetermined impairment levels.
Additionally, it was noted that patients previously hospitalised for acute COPD exacerbation showed a tendency towards significant benefits from early pulmonary rehabilitation (within 1 month post-discharge), compared to patients receiving standard care modalities or no rehabilitation during this period. Evidential quality was low in the systematic review examined, but it was determined that there was no reason why patients who had a recent COPD exacerbation should not be considered for pulmonary rehabilitation [8].
NHS Lothian, 2011 [edit | edit source]
The NHS Lothian COPD Guidelines [22] concur broadly with the NICE 2010 Guidelines [8], agreeing that there is sufficient evidence that it is evidentially sound in its purported benefits to all COPD patients, and particularly those with severe to extremely severe COPD, or those scoring ≥ 3 on the Medical Research Council (MRC) breathlessness scale.
As with the NICE 2010 Guidelines, this guideline acknowledges that pulmonary rehabilitation:
- Improves exercise tolerance
- Improves Quality of Life
- Reduces symptoms
- Reduces number of exacerbations
- Reduces hospital admissions
Given that pulmonary rehabilitation is available in all Community Health Partnerships (CHPs) throughout Lothian, this guideline recommends that all patients with repeated exacerbations or who are hospitalised for exacerbations be fast-tracked for pulmonary rehabilitation [22].
NHS Quality Improvement Scotland, 2010 [edit | edit source]
It acknowledges both the benefits of pulmonary rehabilitation on COPD patients with regard to improving health-related quality of life, exercise capacity and breathlessness, particularly in the wake of acute exacerbation.[23]
In summary, multiple major sources of clinical standards and guidelines agree that pulmonary rehabilitation is an effective treatment modality for:
- Improving health-related quality of life outcomes in patients
- Modulating symptoms,
- Reducing incidences of exacerbation
- Reduce hospital readmission
- Reduce the need for medication
Pulmomary rehabilitation is a method of doing so in a safe, timely and cost-effective manner [23].
Patients' Experience of Pulmonary Rehabilitation Classes[edit | edit source]
The following are patients’ accounts of what life was like before starting a pulmonary rehabilitation programme for COPD, called Breath Smart, and how the rehabilitation classes have affected them. We feel that the improvements they report to their quality of life is another reason for why we should have more pulmonary rehabilitation classes. They have all given written consent for their stories and/or name to be shared on physiopedia.
Patient A’s Story: Back before I started at Breath Smart I couldn’t do a lot. I was heavily dependent on oxygen and practically house bound. I couldn’t use the stairs or do my gardening or go to the shops. I was actually wheeled into my 1st class at breath smart because I couldn’t walk far at all. I must have been in hospital 8 or 9 times the year before I started these classes. I’ve been coming twice a week for just over a year and now I don’t use any oxygen at all and I will gladly take the stairs without any trouble. I haven’t been admitted to hospital once this year. I can now use the treadmill for 25mins at a time at a speed of 5.5km/hr and an incline of 3.5. I never thought this would be possible. Breath Smart has given me back my freedom I can’t begin to explain the changes it has made to my life. I am however still smoking. If I was able to improve this much while still smoking I can only imagine how much better I would be if I could give them up but I haven’t been able to as of yet.
Anne’s Story: Before starting Breath Smart I spent a lot of time in hospital, my breathing was very bad and my general health was very bad also. I used an awful lot of oxygen. Confidence was a big problem. It was hard to know what to do, that was very very difficult. I had been very very active all my life and then everything came to a standstill. My consultant suggested I come to Breath Smart. I’m here 2 years now, and the difference in my life is huge! I couldn’t even start to tell people how much of a difference it has made to my life, but I do tell people. My family have all seen the difference it has made to my life. I’m more active. Coming to breath smart gives you an incentive, it gives you the confidence, the people here are professional you trust them, I trust everyone here they are very very good, they explain to you and tell you if you are doing too much or doing too little. This is the 1st year that I haven’t been in hospital since I was diagnosed.
Option Appraisal[edit | edit source]
In order to establish the most effective setting for our pulmonary rehabilitation programme we evaluated hospital, community and home settings using existing evidence. Choosing the right setting for the pulmonary rehabilitation programme is vital for ensuring the success of the programme. The correct setting can have a positive effect on patient uptake and adherence positively influencing the health of COPD patients reducing exacerbations and hospital admissions and in turn reduce NHS spending on treating COPD.
A recent survey highlighted that pulmonary rehabilitation is only available in 25% of U.K. hospitals [9] limiting the number of COPD patients that can benefit. There are a variety of settings in which pulmonary rehabilitation services for patients with COPD can be provided. Traditionally services were based in hospital inpatient and outpatient settings, but there is growing interest in developing services in community and home settings making it easier for patients to attend and carry out. As pulmonary rehabilitation programmes have been long established in hospital based settings it is the standard comparison for any other potential pulmonary rehabilitation programme settings.
Location is stated as a core element in the full clinical guideline on COPD, it states that for pulmonary rehabilitation programmes to be effective and to improve compliance, they should be held at times that suit participants, in buildings that are easy for participants to get to and have good access for people with disabilities [8].
Hospital[edit | edit source]
Table 1: Advantages and disadvantages to pulmonary rehabilitation in a hospital setting
| Advantages |
Disadvantages |
| Peer support | Difficulty parking – possible |
| No external costs, i.e. rent | Busy environment |
| Patients may deem hospital appointments more important | Lack of available, purposeful space |
| Qualified medical staff | Limited exercise equipment |
| Safe, controlled environment | May associate hospital with acute illness |
| Medical equipment available | Increased chance of contracting an infection |
| Exercise equipment available | Costly, even in outpatient setting |
| Cost comparison found most efficient form of delivery | Suffer from high drop out rates with 20% not completing the programme |
| Found to be effective in improving exercise tolerance and QoL | Patients discouraged because of frequent journeys to hospital |
| Patients often have difficulty getting to a hospital |
Compiled from [24][25][9][26][27][28][29][30]
Community[edit | edit source]
Table 2: Advantages and disadvantages of pulmonary rehabilitation in a community setting
| Advantages | Disadvantages |
| Peer support | External costs i.e. rent, travel expenses, equipment, resources |
| Motivational environment encouraging compliance | Patients may want to take part more anonymously |
| Familiar, friendly atmosphere | |
| Low drop out rates | |
| Sufficient amount of exercise equipment | |
| Available, purposeful space | |
| More involved within the community | |
| Qualified physiotherapists | |
| Relaxed atmosphere so patients feel more comfortable raising questions/issues | |
| Influence patients participation in physical activity | |
| Greater choice of venue making it more accessible | |
| Local ownership | |
| Found to be effective in improving exercise tolerance and QoL |
Home[edit | edit source]
Table 3: Advantages and disadvantages of pulmonary rehabilitation in a home setting
| Advantages | Disadvantages |
| Cost effective | Safety |
| No supervision | Adherence |
| Patient may feel safer and more comfortable exercising in own home | Information clear and well instructed? Patient understands and carries out correctly? |
| Can do it at time that suits patient | No supervision |
| Improved exercise tolerance | No peer support |
| Any issues that arise may not be addressed immediately | |
| Feasibility of resources and equipment – cost, availability | |
| Practicalities of having equipment in home i.e. space |
Compiled from [26][24][31][28]
Following a review of the evidence a community setting was chosen for the pulmonary rehabilitation programme. Evidence showed pulmonary rehabilitation provided in a community setting has comparable benefits to that produced in a more customary hospital-based setting, with both settings producing significant improvements in exercise capacity and quality of life [26][28][25] . The choice of venue has been found to be determined by local factors of convenience, current availability of resources and incremental costs as supported by Waterhouse et al. [25]. When health economic analysis was considered by Waterhouse et al. [25] it revealed that neither hospital nor community based programmes were preferential. Benefits of having the class in a community setting aided attendance and compliance helping not only patients but in the long run saving the NHS money by preventing exacerbations and reducing hospital admissions.
Evidence suggests that there appears to be no clinical or cost benefit of community based pulmonary rehabilitation programmes over hospital based pulmonary rehabilitation and that the venue may be best determined by local access preferences and transport links reinforcing current NICE recommendations [8].
Proposed Class Structure[edit | edit source]
Table 4: Proposed Class Structure
| Structure |
Additional Information |
| 2 supervised classes a week with 1 hour of exercise per class for 10 weeks |
Rolling classes Encouragement to do at least 2 home exercise sessions, recorded in helath check sheets (see SecondWind:appendix 1) If a patient feels the need they can return for a top-up session |
| Health Check |
See SecondWind:appendix 1 |
| Warm-up | |
| Cardiovascular Exercise |
To be recorded on exercise sheets (see SecondWind:appendix 2) Intensity: 4-6 on dyspnoea scale (see SecondWind:appendix 3) Duration: Building up to 30mins |
|
Strengthening Exercise For Upper and Lower Limbs |
To be recorded on exercise sheets (see SecondWind:Appendix 5) 2-4 sets 6-12 reps 50-80% of 1RM |
| Cool down | |
| Health checks | |
| Education and Refreshments | Short education session and time for participants to ask questions* |
Education topics to include, but not limited to;
- COPD
- Medications
- Smokign Cessation
- Pacing
- Goal Setting
- Breathlessness Management
- Chest clearance
- Benifit of Exercise
- Nutrition
Evidence To Support Our Proposed Class Structure[edit | edit source]
Eligibility for the proposed pulmonary rehabilitation program shall be in line the NICE COPD guideline [8]. This states that “pulmonary rehabilitation should be offered to all patients who feel functionally disabled by COPD” [8].
“The opportunity for structured, on-going exercise with peer and professional support, in a suitable venue, is perceived as important to people with COPD in facilitating a physically active lifestyle following pulmonary rehabilitation” [11].
According to General Practice Airways group's sharing of best practice meeting [32] and the American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation [33], at least one supervised session is required per week for effective pulmonary rehabilitation. It has also been suggested that two supervised sessions per week may have a better impact on health-related quality of life compared to one supervised session [34].Group sessions would be interspersed with exercise sessions which participants would do in their own time at home or in a local leisure facility. It is suggested that a minimum of four home sessions are completed per week [32]. Therfore, to make this program as cost effective as possible, we suggest that it should contain two weekly exercise classes, and two home sessions, as opposed to a number of individually supervised rehabilitation sessions which would be labour and cost intensive.
As recommended by the American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation [33], a minimum of twenty exercise sessions would be included in this pulmonary rehabilitation program at a frequency of at least three per week. According to the NICE COPD guideline [8], duration of initial pulmonary rehabilitation should be between six and 12 weeks. To conform to both of these guidelines, we propose a 10 week pulmonary rehabilitation program consisting of two supervised sessions per week.
Although exercise of varied intensity has been shown to be beneficial for people with COPD, high intensity exercises would be encouraged in this rehabilitation program for greater physiological effects [33]. In addition to the traditional lower limb training normally included in pulmonary rehabilitation, such as walking or cycling, upper limb exercises, such as arm ergometer or hand weight exercises, will be included as a number of beneficial effects have been noted including reduce ventilatory requirements while using the arms [35][36].
In addition to the structured exercise class, an essential educational component will be included in the pulmonary rehabilitation program [32]. This would include teaching participants the importance of exercise, which is of specific importance as many individuals with COPD elect not to take up a referral to pulmonary rehabilitation as they think they would not experience any health benefits. Ensuring good attendance at pulmonary rehabilitation requires consideration of how information regarding its proven benefits can be conveyed to participants [37]. It is also important to supply the participants with information on how to transfer exercise into environments outside the class, such as their home, as this will be required for between supervised sessions and once they have completed the program [33]. Information on relaxation, anxiety management, medication and self-management [32], including an action plan for exacerbations [33], would also be included as this seen as being essential in an effective pulmonary rehabilitation program.
Financing[edit | edit source]
Fixed Expenses[edit | edit source]
Below is a table indicating the fixed costs of the SecondWind class by year and by month.
Table 5: Fixed Expenses
| Expenses | Yearly | Monthly |
| Venue | 3600 | 300 |
| Staff (Band 5 Physiotherapist) | 2027.52 | 168.96 |
| Staff (Physiotherapist Assistant) | 1110.24 | 92.52 |
| Personal Indemnity Insurance | Covered by CSP Membership | Covered by CSP Membership |
| Total | £6737.76 | £561.48 |
To calculate the staffing costs we used the following stepped equation:
1. Number of workable hours per year
- Number of weeks per year X hours worked per week
- 52 X 37.5= 1950
2. Number of hours worked per year
- Number of workable hours per year– (Holiday + bank holiday hours)
- 1950 – [(27 X 7.5) + (8 X 7.5)]
- 1950 – (203 + 60)
- 1950 – 263
- 1687
3. Cost per hour for staff
- (Salary + Employers Contribution to National Insurance [13.08% for 2012-2013]) ÷ Hours worked per year
- Physiotherapist = 21,000 + 2750= 22750, 22750 ÷ 1687 = 14.08.
- Physiotherapist Assistant= 11500 + 1504.2 = 13004.2, 13004.2 ÷ 1687 = 7.71
4. Monthly Cost
- Cost per hour X hours per week X hours per month
- 2 class per week @ 1.5hr each = 3hrs per week
5. Yearly Cost
- monthly cost X 12
Variable Expenses[edit | edit source]
Below is a table indicating the variable costs of the SecondWind class by year and by month.
Table 6: Variable Expenses
| Expenses | Once off | Yearly | Monthly |
| Stationary | |||
| Printer | 49.99 | 16.66 | 1.39 |
| Tea and Coffee | 96 | 8 | |
| Paper Cups | 48 | 4 | |
| Plastic Spoons | 24 | 2 | |
| Milk | 96 | 8 | |
| Total | £49.99 | £340.68 | £28.39 |
The cost of the printer was worked out as follows:
1. Yearly cost
- Cost of printer (priced at PC World) ÷ 3 (estimated minimal life expectancy)
2. Monthly cost
- Yearly cost ÷ months per year
Capital Expenses[edit | edit source]
Below is a table indicating the capital costs of the SecondWind class by year and by month.
Table 7: Capital Expenses
| Expenses | Once Off | Yearly | Monthly |
| Blood Pressure Monitor X 4 | 160 | 53.33 | 4.44 |
| Pulse Oximeter | 198 | 66 | 5.50 |
| Total | £358 | £119.33 | £9.94 |
The cost of all capital equipment was worked out as follows:
1. Three quotes were explored and the average cost was taken
2. Yearly Cost
- Cost of item ÷ 3 (estimated minimal life expectancy)
3. Monthly cost
- Yearly cost ÷ months per year
Overhead Cost[edit | edit source]
Fixed Expenses + Variable Expenses
Yearly overheads = £7078.44
Monthly overheads = £589.87
Start Up Costs[edit | edit source]
Capital expenses + 1st 3 month’s overheads
358 + (589.87 X 3)
358 + 1769.61
£2127.61
Cost of Service per Participant[edit | edit source]
(Overhead costs + Capital expenses) ÷ Number of participants
Yearly
(7078.44 + 119.33) ÷ 16
£449.86 per participant per year
Monthly
(589.87 + 9.94) ÷ 16
£37.49 per participant per year
Risk Analysis[edit | edit source]
SWOT[edit | edit source]
To analyse the risks of our class being sucessful or not we performed a SWOT analysis looking at our Strengths, Weaknesses, Opportunities and Threats.
Strengths When exploring the strengths of our proposed pulmonary rehabilitation classes we first assessed the strengths associated with the location of our class. They are as follows;[edit | edit source]
- The setting of a local gym is easy to access which may increase adherence to classes
- Being placed in the community may, potentially, cause less anxiety for participants than a hospital setting.
- The gym has more available space than most hospitals, thus, a greater capacity for participants.
- Since the rehabilitation program is not being run in the hospital, there is a lower chance of participants acquiring healthcare related infections.
This is followed by the strengths associated with our staff which include;
- Our program will have qualified staff including first aiders who are trained in defibrillator use.
- The physiotherapist will have cardiorespiratory education as part of their degree and experience in respiratory care. They will be able to provide answers to questions patients may have.
And finally the strengths of the class itself which include;
- Evidence shows that pulmonary rehabilitation gives numerous benefits to participants including improved quality of life
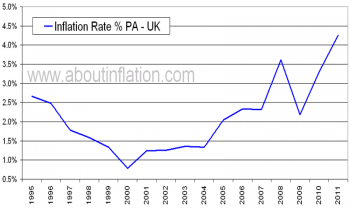
- There is an increasing body of evidence that pulmonary rehabilitation decreases long term costs to NHS. As Figure 7 and 8 demonstrate, the NHS, in real terms, is receiving less money. Therefore, projects like our proposed class would assist in maximising uitity for resources invested.
- The group exercise setting provides peer support which have been shown to benefit this population of people by helping to decreases feelings of isolation and increase confidence
- Top-up sessions available for patients who require further assistance to adhere to exercise
- The class are free for participants therefore, those effected by inablility to work do not have to worry about how they will pay for the class, this may encourage more participants to take part.
Figure 7: UK Health Budget And Spending (adapted from [38][39]) Figure 8: UK Inflation Rates [40]
Weaknesses[edit | edit source]
- Some participants may find a gym to initially be an intimidating setting. However, they will be provided with information explaining that they will be exercising with other people who are of a similar age and have the same condition.
- Exercise is an undesirable activity for some participants, especially in people with COPD where breathlessness may be an issue. However, they will be provided education on the benefits of exercise and what to expect from the classes.
Opportunities[edit | edit source]
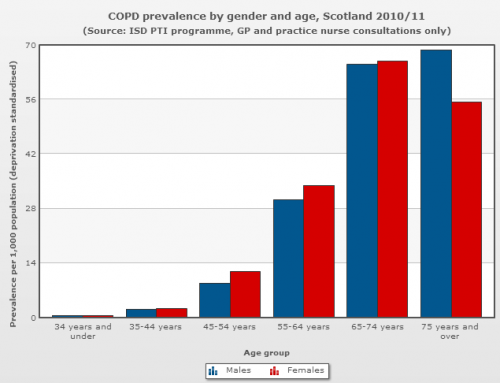
- There is a large prevalence and incidence of COPD, as indicated by Figure 9, which provides a large pool of participants who may take part in our classes.
- Increased referrals to the program will reduce demands on NHS’s limited resources. Refer back to figure 5 and 6
- Greater exposure of pulmonary rehabilitation in the community will increase public awareness of this treatment option
Figure 7: COPD prevalance by gender and age, Scotland 2010/11 [41]
Threats[edit | edit source]
The primary threats to our propossed classes are other pulmonary rehabilitation classes:
- Some gyms run pulmonary rehabilitation classes. However, these are 1 to 1 sessions with a gym instructor so there is a lack of peer and group support. In addition, this rehabilitation program will have all the material delivered by health professionals with experience in respiratory care.
- Pulmonary rehabilitation is also often held in the hospital. We feel that our program setting is less intimidating and carries fewer negative connotations. There is also the additional benefit of more car parking facilities than what is available at most hospitals.
Health and Safety[edit | edit source]
To address the issues sourrounding the health and safety risks we compiled a risk assessment form for the classes. Please refer to SecondWind:Appendix 6.
Evaluation of Programme[edit | edit source]
To evaluate the success of our programme, the following outcome measures will be monitored:
NHS Costs[edit | edit source]
- Patient healthcare utilisation frequency: Changes in per-patient rate of consultations, hospitalisations, drug prescriptions and other use of healthcare will be indicative of any savings accrued by the NHS. This outcome will be assessed via a healthcare utilisation questionnaire administered at three intervals; prior to commencement of treatment, 6 months post-programme and 1 year post-programme.
Patient Improvements[edit | edit source]
Functional improvements in patients will be determined by pre and post programme measurements based on the following:
- Shuttle walk test
- 10 RM test of major upper limb and lower limb muscle groups
- Quality of life questionnaire .
These baseline measures will be used to individualise the participants exercise programmes.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 NHS. Chronic Obstructive Pulmonary Disease 2012; Available at: http://www.nhs.uk/Conditions/Chronic-obstructive-pulmonary-disease/Pages/Introduction.aspx. Accessed October/18th, 2012.
- ↑ 2.0 2.1 British Lung Foundation. COPD. 2012; Available at: http://www.blf.org.uk/Conditions/Detail/COPD#overview. Accessed October/20th, 2012.
- ↑ 3.0 3.1 3.2 NHS Lothian. Lothian Pulmonary Rehabilitation Audit. 2009; Available at: http://www.lothianrespiratorymcn.scot.nhs.uk/wp-content/uploads/2010/08/Pulmonary-Rehabilitation-Service-Audit-2009-v1.0.pdf. Accessed October/20th, 2012.
- ↑ Willgoss T, Yohannes A, Goldbart J, Fatoye F. COPD and anxiety: its impact on patients' lives. Nurs Times 2011 Apr 19-May 2;107(15-16):16-19.
- ↑ Stahl E, Lindberg A, Jansson SA, Ronmark E, Svensson K, Andersson F, et al. Health-related quality of life is related to COPD disease severity. Health Qual Life Outcomes 2005 Sep 9;3:56.
- ↑ 6.0 6.1 6.2 National Clinical Guideline Centre. COPD Costing report: Implementing NICE guidelines 2011; Available at: http://www.nice.org.uk/nicemedia/live/13029/53292/53292.pdf. Accessed October/18th, 2012.
- ↑ Department of Health. Action plan for respiratory disease treatment published. 2012; Available at: http://www.dh.gov.uk/health/2012/05/nhs-companion-copd/. Accessed October/21st, 2012.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 8.12 8.13 National Clinical Guideline Centre. Chronic obstructive pulmonary disease, Management of chronic obstructive pulmonary disease in adults in primary and secondary care. 2010; Available at: http://guidance.nice.org.uk/CG101/Guidance/pdf/English. Accessed October/15th, 2012
- ↑ 9.0 9.1 9.2 9.3 British Thoracic Society. Standards of Care Committee on Pulmonary Rehabilitation. Thorax 2001;56:827-834.
- ↑ Global Initiative For Chronic Obstructive Lung Disease. Global Strategy for the diagnosis, management, and prevention of Chronic Obstructive Pulmonary Disease (Revised 2011). Global Initiative For Chronic Obstructive Lung Disease 2011:1-80.
- ↑ 11.0 11.1 Hogg L, Grant A, Garrod R, Fiddler H. People with COPD perceive ongoing, structured and socially supportive exercise opportunities to be important for maintaining an active lifestyle following pulmonary rehabilitation: a qualitative study. Journal of Physiotherapy 2012 9;58(3):189-195.
- ↑ 12.0 12.1 Ries AL, Bauldoff GS, Carlin BW, Casaburi R, Emery CF, Mahler DA, et al. Pulmonary Rehabilitation: Joint ACCP/AACVPR Evidence-Based Clinical Practice Guidelines. Chest 2007 May;131(5 Suppl):4S-42S.
- ↑ Griffiths TL, Burr ML, Campbell IA, Lewis-Jenkins V, Mullins J, Shiels K, et al. Results at 1 year of outpatient multidisciplinary pulmonary rehabilitation: a randomised controlled trial. Lancet 2000 Jan 29;355(9201):362-368.
- ↑ Griffiths TL, Phillips CJ, Davies S, Burr ML, Campbell IA. Cost effectiveness of an outpatient multidisciplinary pulmonary rehabilitation programme. Thorax 2001 October 01;56(10):779-784.
- ↑ 15.0 15.1 15.2 Crawford R, Emmerson C. NHS and social care funding: the outlook to 2021/22. Institute for Fiscal Studies 2012;July:1-32.
- ↑ The Scottish Government. Scottish Spending Review 2011 and Draft Budget 2012-13. 2011; Available at: http://www.scotland.gov.uk/Resource/Doc/358356/0121130.pdf. Accessed November/16, 2012.
- ↑ BBC. Commmissioning Success. 2012; Available at: http://commissioningsuccess.com/2012/07/nhs-budget-squeeze-could-last-a-decade/. Accessed October/20th, 2012.
- ↑ Khdour MR, Agus AM, Kidney JC, Smyth BM, Elnay JC, Crealey GE. Cost-utility analysis of a pharmacy-led self-management programme for patients with COPD. Int J Clin Pharm 2011 Aug;33(4):665-673.
- ↑ 19.0 19.1 Britton M. The burden of COPD in the U.K.: results from the confronting COPD survey. Respir Med 2003 3;97, Supplement C(0):S71-S79.
- ↑ 20.0 20.1 20.2 20.3 20.4 Audit Scotland. Managing long-term conditions. 2007; Available at: http://www.audit-scotland.gov.uk/docs/health/2007/nr_070816_managing_long_term.pdf. Accessed October/15, 2012.
- ↑ 21.0 21.1 ISD Scotland. Estimated numbers of consultations, by staff type. 2011; Available at: http://www.isdscotland.org/Health-Topics/General-Practice/Publications/2011-11-29/PTI_Nov11_charts_consultations_COPD.xls. Accessed November/13th, 2012.
- ↑ 22.0 22.1 NHS Lothian. Chronic Obstructive Pulmonary Disease (COPD) Guideline. Lothian Respiratory (COPD) MCN 2011;August:1-18.
- ↑ 23.0 23.1 NHS Quality Improvement Scotland. Healthcare Improvement Scotland COPD services - Clinical Standards, Edinburgh. NHS Quality Improvement Scotland 2010.
- ↑ 24.0 24.1 24.2 Ward JA, Akers G, Ward DG, Pinnuck M, Williams S, Trott J, et al. Feasibility and effectiveness of a pulmonary rehabilitation programme in a community hospital setting. Br J Gen Pract 2002 Jul;52(480):539-542.
- ↑ 25.0 25.1 25.2 25.3 25.4 Waterhouse JC, Walters SJ, Oluboyede Y, Lawson RA. A randomised 2 x 2 trial of community versus hospital pulmonary rehabilitation, followed by telephone or conventional follow-up. Health Technol Assess 2010 Feb;14(6):i-v, vii-xi, 1-140.
- ↑ 26.0 26.1 26.2 Maltais F, Bourbeau J, Shapiro S, Lacasse Y, Perrault H, Baltzan M, et al. Effects of home-based pulmonary rehabilitation in patients with chronic obstructive pulmonary disease: a randomized trial. Ann Intern Med 2008 Dec 16;149(12):869-878.
- ↑ Slovic P, Finucane ML, Peters E, MacGregor DG. Risk as Analysis and Risk as Feelings: Some Thoughts about Affect, Reason, Risk, and Rationality. Risk Analysis 2004;24(2):311-322.
- ↑ 28.0 28.1 28.2 Guëll MR, Lucas P, Gáldiz JB, Montemayor T, González-Moro JMR, Gorostiza A, et al. Home vs hospital-based pulmonary rehabilitation for patients with chronic obstructive pulmonary disease: A Spanish multicenter trial. Archive Bronconeumol 2008;44(10):512-518.
- ↑ Fischer MJ, Scharloo M, Abbink JJ, Thijs-Van A, Rudolphus A, Snoei L, et al. Participation and drop-out in pulmonary rehabilitation: a qualitative analysis of the patient's perspective. Clin Rehabil 2007 Mar;21(3):212-221.
- ↑ Strijbos JH, Postma DS, van Altena R, Gimeno F, Koeter GH. A comparison between an outpatient hospital-based pulmonary rehabilitation program and a home-care pulmonary rehabilitation program in patients with COPD. A follow-up of 18 months. Chest 1996 Feb;109(2):366-372.
- ↑ Zakrisson A, Engfeldt P, Hägglund D, Odencrants S, Hasselgren M, Arne M, et al. Nurse-led multidisciplinary programme for patients with COPD in primary health care: a controlled trial. Primary Care Respiratory Journal 2011 December;20(4):427-433.
- ↑ 32.0 32.1 32.2 32.3 Backley J, Bloom J, Bott J, Jones R, Langley C, Singh S, et al. A summary of recommendations of the pulmonary rehabilitation in the community- sharing best practice meeting. General Practice Airways Group 2005:30/10/12.
- ↑ 33.0 33.1 33.2 33.3 33.4 Nici L, Donner C, Wouters E, Zuwallack R, Ambrosino N, Bourbeau J, et al. American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation. American Journal of Respiratory and Critical Care Medicine 2006 June 15;173(12):1390-1413.
- ↑ Liddell F, Webber J. Pulmonary rehabilitation for chronic obstructive pulmonary disease: a pilot study evaluating a once-weekly versus twice-weekly supervised programme. Physiotherapy 2010 3;96(1):68-74.
- ↑ Couser JI, Martinez FJ, Celli BR. Pulmonary rehabilitation that includes arm exercise reduces metabolic and ventilatory requirements for simple arm elevation. CHEST Journal 1993 January 1;103(1):37-41.
- ↑ Epstein SK, Celli BR, Martinez FJ, Couser JI, Roa J, Pollock M, et al. Arm training reduces the VO2 and VE cost of unsupported arm exercise and elevation in chronic obstructive pulmonary disease. J Cardiopulm Rehabil 1997 May-Jun;17(3):171-177.
- ↑ Keating A, Lee AL, Holland AE. Lack of perceived benefit and inadequate transport influence uptake and completion of pulmonary rehabilitation in people with chronic obstructive pulmonary disease: a qualitative study. Journal of Physiotherapy 2011 9;57(3):183-190.
- ↑ HM Treasury. UK budgets 2009-2012. 2012; Available at: http://www.hm-treasury.gov.uk/home.htm. Accessed September/18th, 2012.
- ↑ HM Treasury. UK budgets 1998-2008. 2008; Available at: http://webarchive.nationalarchives.gov.uk/+/http:/www.hm-treasury.gov.uk/budget/budget_04/bud_bud04_index.cfm. Accessed September/18th, 2012.
- ↑ About Inflation. UK Inflation Rate Historical chart. 2011; Available at: http://www.aboutinflation.com/inflation-rate-historical/uk-inflation-rate-historical-chart. Accessed November/15th, 2012.
- ↑ The Scottish Public Health Observatory. Chronic obstructive pulmonary disease (COPD): primary care data. 2012; Available at: http://www.scotpho.org.uk/health-wellbeing-and-disease/chronic-obstructive-pulmonary-disease-copd/data/primary-care-data. Accessed November/13th, 2012.
Appendices[edit | edit source]
Appendix 1 - Sample Pre-Exercise Health Check Sheet[edit | edit source]
File:Pre-exercise health check.pdf
Appendix 2 - Sample Aerobic Exercise Recording Sheets[edit | edit source]
File:Exercsie class sheets.pdf
Appendix 3 - Rate of Preceived Dyspoena[edit | edit source]
File:Rate of Perceived Dyspnea.pdf
Appendix 4 - Measure Outcome for Quality Of Life[edit | edit source]
Appendix 5 - Sample Recording Sheet for Strengthening Exercises[edit | edit source]
File:Strengthening exercise recording sheet.pdf
Appendix 6 - Pulmonary Rehabilitation Programme Risk Assessment[edit | edit source]