Sever's Disease
Definition/Description[edit | edit source]
The term was coined by James Warren Sever in 1912. One of the most common causes of heel pain among children between the ages of 10 to 12 years. Also known as calcaneal apophysitis or calcaneoapophysitis, this condition is the painful inflammation of the calcaneal apophysis caused by repetitive microtrauma on the unossified apophysis due to traction of the achilles tendon. Other common traction injuries are Iliac apophysitis, medial epicondyle apophysitis or Little League elbow, inferior pole of patella apophysitis or Sinding-Larsen-Johansson syndrome, tibial tubercle apophysitis or Osgood-Schlatter disease, and fifth metatarsal apophysitis.
Clinically Relevant Anatomy[edit | edit source]
The calcaneal apophysis refers to the back part of the posterior aspect of the calcaneus , where the Achilles tendon inserts. This area contains the open growth plate called physis. The closure of the calcaneus growth plate typically occurs around the age of 14.[1] Until that time, new bone is forming at the calcaneal physis. When this growth plate is irritated, it undergoes stress that leads to inflammation. The primary explanation for Sever's injury involves excessive mechanical strain caused by repeated impact pressure and shear forces on the still-developing growth plate of the calcaneus.[1]
Apophysis have a higher composition of fibrocartilage. The calcaneal apophysis usually appears in children around 7-9 years old and fuses between the ages 15–17 years of age. The Achilles Tendon inserts to the lower, posterior and slightly medial aspect of the calcaneus. The calcaneal growth plates are subjected to high stress from the plantar aponeurosis and the Achilles tendon.[2]
Etiology/Risk Factors[edit | edit source]
Sever’s disease is an osteochondrosis caused by overload. This C-shaped growth zone becomes inflamed secondary to repetitive traction stress of the Achilles tendon.
Risk factors may include:
- High physical and sporting activities especially those involving repetitive running and jumping
- Heel cord tightness
- Weak ankle dorsiflexion
- Poorly cushioned or worn out athletic shoes
- Running on hard surfaces
- Biomechanical factors such as genu varum, forefront pes cavovarus or pes planus[3][4]
- Obesity[5]
- Greater waist circumference and increased height[5]
Epidemiology[edit | edit source]
Sever's disease is an overgrowth syndrome similar to Osgood-Schlatter disease. Growth is directly proportional to the amount of stress placed on the calcaneal growth plates.
Active children and adolescents, particularly during the pubertal growth spurt or at the beginning of a sport season (e.g. gymnasts, basketball and football players) often suffer from this condition[6][7]. This disease occurs most commonly during the early part of the growth spurt. A boy-to-girl ratio is 2-3:1.[7] It occurs only in the growing children and never occurs after puberty[8].
Characteristics/Clinical Presentation[edit | edit source]
This syndrome can occur unilaterally or bilaterally[9]. The incidence of bilaterally is approximately 60%[3].
Common signs and symptoms:
- Pain is usually absent when the child gets up in the morning[7].
- Increased pain with weight bearing, running or jumping[6][7]
- Tenderness on medial and lateral heel compression.[8]
- No erythema, swelling or skin changes found.[8]
- Can be associated with other foot malalignments.
- The child may limp at the end of physical activity[2][7].
- Limited ankle dorsiflexion range secondary to tightness of the Achilles tendon. The pain gradually resolves with rest. All the sporting activities including running should be discontinued while the child has heel pain.
Differential Diagnoses[edit | edit source]
Posterior heel pain can occur due to
- Achilles Tendinopathy
- Haglund's Deformity
- Retrocalcaneal Bursitis
- Calcaneal stress Fracture
- Heel spur
- Heel pad syndrome
Diagnostic Procedures[edit | edit source]
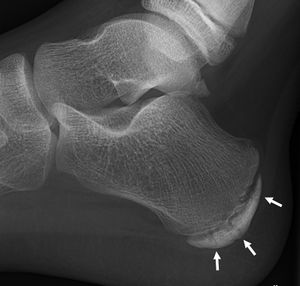
Radiography[edit | edit source]
Most of the time radiographs are not helpful because the calcaneal apophysis is frequently fragmented and dense in normal children. But they can be used to exclude other traumas.
Ultrasonography[edit | edit source]
Diagnostic Ultrasound could show the fragmentation of secondary nucleus of ossification of the calcaneal growth plate. This is a safe diagnostic tool since there is no radiation. This diagnostic tool can also be used to exclude Achilles tendinopathy and/or retrocalcaneal bursitis[10].
MRI[edit | edit source]
MRI showed signal changes in posterior calcaneal epiphysis, and can help localize inflammation to apophysis[11].
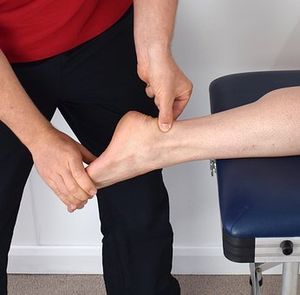
Examination[edit | edit source]
- Tenderness on palpation.
- Passive dorsiflexion test of the ankle: shows a decrease in dorsiflexion. This test may also provoke a painful reaction.
- Squeeze test: Mediolateral compression of the calcaneal growth plate to elicit pain in Sever’s disease[2]. Performed over the lower one-third of the posterior calcaneus. This test is the most important to diagnose calcaneal apophysitis.
- Standing tiptoe aggravates the heel pain.
- Biomechanical abnormalities: pes valgoplanus, forefoot varus, rear foot varus, pes cavus, pes planus, and hallux valgus.
- Swelling and other skin changes are indicators for different pathologic conditions and are uncommon for Sever’s disease. Although there could be mild swelling.
- Gait may be normal; the patient may walk with a limp or exhibit a forceful heel strike.
- Overweight
Physical Therapy Management[edit | edit source]
As the condition is self-limiting, it resolves as the child matures. Treatment depends on the severity of the child’s symptoms. During the active phase, the patient’s activity level should be limited only by pain.
Treatment:
- Relative Rest and/or cessation of sports[7].
- Cryotherapy[7].
- Taping: Taping the foot around the arch and heel area has been noted to reduce pain caused by Sever’s disease and ambulation.[1]
- Silicone heel cup with medial arch support cushions the affected area for shock absorption and helps in reducing pain.
- Orthoses can be prescribed to correct secondary foot malalignments, such as foot in valgus position can disrupt the Windlass mechanism which is important for normal gait.[7]
- Stretching of Triceps Surae, Plantar fascia to improve dorsiflexion and strengthening of extensors[7]
- Gentle mobilizations to the subtalar joint and forefoot area[12]
- Electrical stimulation in the form of Russian stimulation sine wave modulated at 2500 Hz with a 12 second on time and an 8 second off time with a 3 second ramp[12]
- Ultrasound, nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen can also be used to decrease the pain and inflammation in individuals with server's disease. [1]
- Corticosteroid injections are not recommended.
- Ketoprofen Gel as an addition to treatment.
Symptoms usually resolve in a few weeks to 2 months after therapy is initiated[6][7][9].
Resources[edit | edit source]
Complications[edit | edit source]
The long-term effect on the heel related to Sever's disease has not been well studied.[1] There have been no long-term effects aasociated with Sever's disease. [1]However, the disease may reappear frequently during periods of growth and non-compliance with treatment plans, but symptoms generally resolve after the closure of the apophysis when the patient reaches skeletal maturity.[1] [3]The following are potential complications linked to individuals suffering from this disease:
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Ramponi DR, Baker C. Sever’s Disease (Calcaneal Apophysitis). Adv Emerg Nurs J. 2019;41(1):10–4.
- ↑ 2.0 2.1 2.2 Scharfbillig RW, Jones S, Scutter SD. Sever’s disease: what does the literature really tell us? Journal of the American Podiatric Medical Association. 2008 May;98(3):212-23.
- ↑ 3.0 3.1 3.2 Smith JM, Varacallo M. Sever Disease. [Updated 2021 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021
- ↑ McSweeney SC, Reed L, Wearing S. Foot Mobility Magnitude and Stiffness in Children With and Without Calcaneal Apophysitis. Foot Ankle Int. 2018 May;39(5):585-590.
- ↑ 5.0 5.1 James AM, Williams CM, Luscombe M, Hunter R, Haines TP. Factors Associated with Pain Severity in Children with Calcaneal Apophysitis (Sever Disease). J Pediatr [Internet]. 2015;167(2):455–9.
- ↑ 6.0 6.1 6.2 Launay F. Sports-related overuse injuries in children. Orthopaedics & Traumatology: Surgery & Research. 2015 Feb 1;101(1):S139-47.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 7.8 7.9 James AM, Williams CM, Haines TP. Effectiveness of interventions in reducing pain and maintaining physical activity in children and adolescents with calcaneal apophysitis (Sever’s disease): a systematic review. Journal of Foot and Ankle Research. 2013 Dec 1;6(1):16.
- ↑ 8.0 8.1 8.2 Micheli LJ, Ireland ML. Prevention and management of calcaneal apophysitis in children: an overuse syndrome. J Pediatr Orthop. 1987 Jan 1;7(1):34-8.
- ↑ 9.0 9.1 Elengard T, Karlsson J, Silbernagel KG. Aspects of treatment for posterior heel pain in young athletes. Open access journal of sports medicine. 2010;1:223.
- ↑ Hosgoren B, Koktener A, Dilmen G. Ultrasonography of the calcaneus in Sever's disease. Indian pediatrics. 2005 Aug 1;42(8):801.
- ↑ Idrissi MO. Sever’s disease. Sch J App Med Sci. 2021 May;5:684-5.
- ↑ 12.0 12.1 Leri JP. Heel pain in a young adolescent baseball player. Journal of Chiropractic Medicine. 2004 Mar 1;3(2):66-8.
- ↑ David Piskulic. Case Study Sever's disease. Medbridge. Available from https://www.youtube.com/watch?v=A6Ffiotje2w
- ↑ Kumar S, Jain N, Karpe P, Limaye R. Osteomyelitis complicating Sever‘s disease: A report of two cases. J Clin Orthop Trauma [Internet]. 2020;11(2):310–3.
- ↑ Belikan P, Färber LC, Abel F, Nowak TE, Drees P, Mattyasovszky SG. Incidence of calcaneal apophysitis ( Sever ’ s disease ) and return ‑ to ‑ play in adolescent athletes of a German youth soccer academy : a retrospective study of 10 years. J Orthop Surg Res [Internet]. 2022;9:1–6.