Transverse Myelitis
Original Editor - Wendy Walker
Top Contributors - Wendy Walker, Admin, Naomi O'Reilly, Mason Trauger, WikiSysop, Kim Jackson, Claire Knott and Kehinde Fatola
Introduction[edit | edit source]
Transverse Myelitis (TM), AKA Acute Transverse Myelitis (ATM) is a rare neurological disorder of the spinal cord, caused by inflammation and occurring across one spinal segment, leading to severe motor, sensory and autonomic dysfunction[1].
The term Transverse Myelitis (TM) was first coined in 1948 by Dr Suchett-Kaye, an English neurologist. He uses this to describe a case of rapidly progressive paraparesis with a thoracic sensory level, occurring as a post-infectious complication of pneumonia.
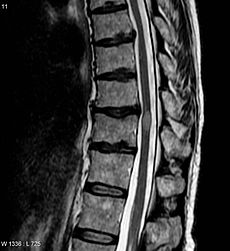
In the MRI scan opposite, the TM lesion is the lighter, oval shape at center-right.
Epidemiology[edit | edit source]
The incidence of TM is 1 (severe) to 8 (mild) cases/million per year[2]. It occurs in adults and children, in both genders, and in all races. A peak in incidence rates (the number of new cases per year) appears to occur between 10 and 19 years and 30 and 39 years.
Mechanism of Injury / Pathological Process[edit | edit source]
The mechanism of injury is inflammation of the spinal cord causing damage to the myelin sheath of the nerves.
Clinical Presentation[edit | edit source]
- Sensory, motor, or autonomic dysfunction attributable to the spinal cord
- Bilateral signs and/or symptoms
- Clearly defined sensory level
The symptoms of TM include muscle weakness, paralysis, parasthesia, neuropathic pain, spasticity, as well as bladder, bowel and sexual dysfunction.
In some cases, symptoms progress over hours whereas in other instances, the presentation is over days. Neurologic function tends to decline during the 4-21 day acute phase, while eighty-percent of cases reach their maximal deficit within 10 days of symptom onset. At its worst point, 50% of individuals have lost all movements of their legs, 80-94% experience numbness, paresthesias or banding or girdling, and almost all have some degree of bladder dysfunction.
There is tremendous variability in the presentation of symptoms, which are based on the level of the spinal cord affected and on the severity of the damage to the myelin and the neurons in the spinal cord.
Although some people recover from transverse myelitis with minor or no residual problems,[2] the healing process may take months to years.[3] Others suffer permanent impairments that affect their and ability to perform ordinary tasks of daily living. Most people will have only one episode of transverse . A small percentage (10-20%) may have a recurrence.
Diagnostic Procedures[edit | edit source]
MRI and/or CT scanning are invariably used in diagnosing TM. Up to 40% of cases have no findings on MRI[4]. Lumbar puncture is used to look for surrogate markers for inflammation in the cerebrospinal fluid (CSF).
Differential Diagnosis[edit | edit source]
The most common aetiologies to be distinguished from idiopathic acute transverse myelitis are:
- Multiple Sclerosis
- Guillain Barre Syndrome
- Disc herniation
- Parainfectious myelitis
- Neuromyelitis optica (Devic's disease)
- Myelitis related to systemic disease, such as systemic lupus erythematosis
- Compression of spinal cord caused by trauma eg. vertebral fractures
- Epidural or subdural hematoma
- Epidural and/or paraspinal abscess
- Tumour
Medical Management[edit | edit source]
Treatments are intended to reduce spinal cord inflammation and alleviate symptoms:
- Corticosteroids given intravenously
- Plasmapheresis - for moderate to severe cases, or those who do not respond to steroids after 3-5 days
- Immunosuppresant medication
Physiotherapy[edit | edit source]
- Stretching programme – to prevent contractures
- Strengthening
- Transfers
- Gait training
- Wheelchair training
- Reduce risk of pressure ulcers
- Aid control of spasticity
- Pain reduction/management
Bladder Problems[edit | edit source]
Bladder function is almost always at least transiently impaired in patients with TM.
Early stage, 1st 6-12 weeks:[edit | edit source]
Immediately after the onset of TM, there is frequently a period of transient loss or reduction of neural activity below the involved spinal cord lesion; this is known as “spinal shock,” and generally lasts approximately 6 to 12 weeks, although it can persist for 6 months or more.
Later stage, post spinal shock:[edit | edit source]
At this stage, two general problems can affect the bladder.
- The bladder can become overly sensitive, and empty after only a small amount of urine has collected, OR
- the bladder comes relatively insensitive, and thus becomes over extended and tends to overflow.
An overly distended bladder increases the likelihood of urinary tract infections and, in time, may threaten the health of the kidneys. Depending on the dysfunction, treatment options include timed voiding, medicines, external catheters for males (a catheter connected to a condom), padding for women, intermittent internal self-catheterization,[5] an indwelling catheter, Botox,[6] or electrical stimulation.[7] Surgical options may be appropriate for some people.[8]
Prognosis[edit | edit source]
Some case series have estimated that approximately one third of patients recover with few or no lasting effects; another third have a moderate degree of residual disability, and one third remain severely disabled.[9][10]
Resources[edit | edit source]
- The Transverse Myelitis Association is the world-wide organisation for TM and related rare autoimmune neurological diseases. This organisation is based in the USA and has close associations to medical and research communities specialising in neurological disorders. Their website is a good source of scientific information and articles on symptoms, treatments.
- The TM Society is a small UK based charity which offers information and support; they hold support group meetings throughout the UK, and also provide a telephone support service, answering questions on TM from patients, relatives or carers.
- Case Report: Physiotherapy management of acute transverse myelitis in a pediatric patient in a Nigerian hospital
References[edit | edit source]
- ↑ Proposed diagnostic criteria and nosology of acute transverse myelitis. Neurology. 2002;59 (4): 499-505
- ↑ 2.0 2.1 Berman M, Feldman S, Alter M, Zilber N, Kahana E. Acute transverse myelitis: incidence and etiologic considerations. Neurology 1981;31:966–971
- ↑ NIH. Transverse Myelitis Fact Sheet. Accessed https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Transverse-Myelitis-Fact-Sheet 5 March 2018
- ↑ 8. Scotti G, Gerevini S. Diagnosis and differential diagnosis of acute transverse myelopathy. The role of neuroradiological investigations and review of the literature. Neurol. Sci. 2001;22 Suppl 2 : S69-73
- ↑ Jamison J, Maguire S, McCann J. Catheter policies for management of long term voiding problems in adults with neurogenic bladder disorders. Cochrane Database Syst Rev. 2013 Nov 18
- ↑ Frenkl TL, Rackley RR. Injectable neuromodulatory agents: botulinum toxin therapy. Urol Clin North Am. 2005 Feb. 32(1):89-99
- ↑ Utomo E, Groen J, Blok BF. Surgical management of functional bladder outlet obstruction in adults with neurogenic bladder dysfunction. Cochrane Database Syst Rev. 2014 May 24. 5:CD004927
- ↑ McGuire EJ, Savastano JA. Urodynamics and management of the neuropathic bladder in spinal cord injury patients. J Am Paraplegia Soc 8 (1985), pp. 28–32
- ↑ Berman M, Feldman S, Alter M, Zilber N, Kahana E. Acute transverse myelitis: incidence and etiologic considerations. Neurology 31(8):966-971, 1981
- ↑ Transverse Myelitis Consortium Working Group (TMCWG). Proposed diagnostic criteria and nosology of acute transverse myelitis. Neurology 59(4):499-505, 2002