Patient Perspective and Motivation in Telehealth
Original Editor - Oriana Catenazzi, Alicia Rebellato, Hannah Meredith, Aaron Kirk, Martin Fitheridge, Marco Zavagni Top Contributors - Tarina van der Stockt and Shaimaa Eldib
The Patient Perspective on Tele-rehabilitation[edit | edit source]
Much has been said about the demographic changes, including an aging population, increased life expectancy and a greater prevalence of chronic conditions, so far, putting increased strain on the healthcare system in Scotland, the UK and worldwide [1]. We know that there has been a lot of pressure on the health care service and systems to reduce the average hospital length of stay and getting patients home earlier. Consequently, in-home tele rehabilitation programmes are increasingly common as an alternative mode of service delivery [2].
Although there is evidence to date to show slow, but successful implementation and integration of home telehealth programmes, just what does the evidence say regarding the patient's perceptions of the services they are receiving as part of their healthcare? Below are two studies that use different methods of tele-rehabilitation intervention and evaluate the corresponding patient perspectives:
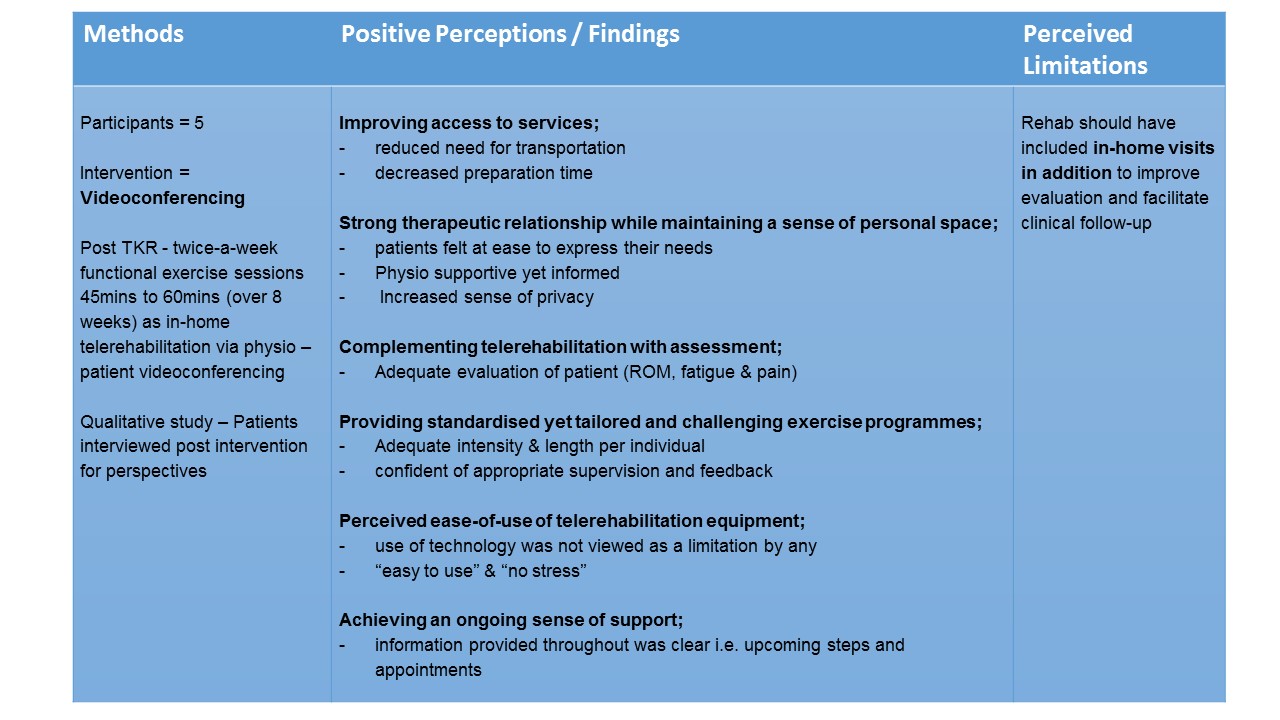
Dahlia et al 2013 “The Patient’s Perspective of in-Home Tele-rehabilitation Physiotherapy Services Following Total Knee Arthroplasty” - article available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3799503/pdf/ijerph-10-03998.pdf
Gale & Sultan 2013 “Telehealth as ‘peace of mind’: embodiment, emotions and the home as the primary health space for people with chronic obstructive pulmonary disorder” - article available from: http://www.sciencedirect.com/science/article/pii/S1353829213000129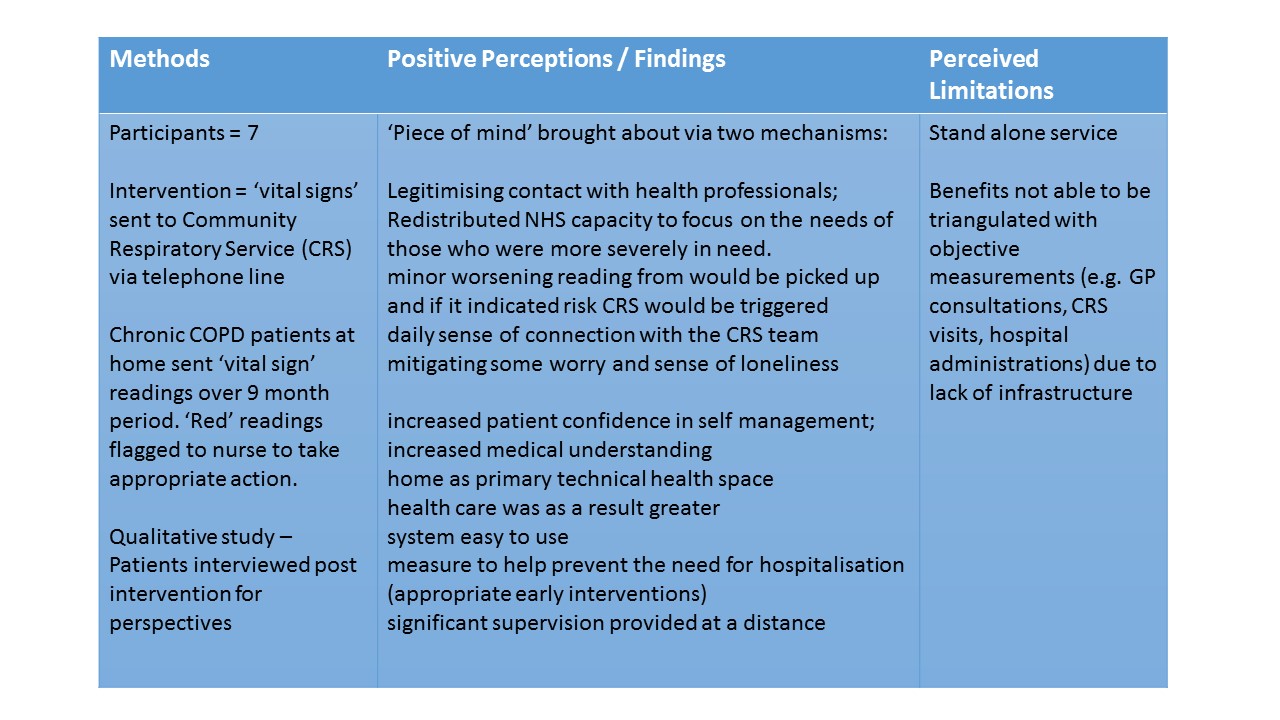
In the two studies above, the telerehabilitation concepts that have been evaluated may also be transferable to different services for conditions that benefit from community rehabilitation of home treatment or monitoring i.e. short and/or long term conditions, and those that result in restricted movement or mobility. Such conditions may include long term degenerative conditions, chronic diseases or musculoskeletal conditions.
Understanding the Patient[edit | edit source]
Recently the development and use of telehealth interventions for changing patient behaviours has greatly increased[3]. The use of mobile applications must take into account the physical and socio-psychological needs of health practitioners and patients. The user approaching a device is not purely interested in what the device does, but rather how the device makes them feel: the developer must remember that the application is developed focusing on the customer and is designed to satisfy all their needs[4]. The ability to access extensive and multifaceted programs provides health care professionals with the opportunity to deliver behavioural changing interventions that can be adapted to meet the patient’s characteristics, behaviours and environment [5]. In order to analyse the effectiveness of these interventions, health behaviour theories and models are used to guide the development and delivery of the intervention[3]. The Transtheoretical Model [6] and Self-Determination Theory (Deci and Ryan, 2000) have served as the basis for many health care interventions and it is important that the physiotherapist understands the underlying principles behind these theories. The use of health behaviour models and theories will assist the health care professional at the initiation stage of the intervention to meet their baseline characteristics of the patient and also during the intervention when behaviour change is taking place. To understand our patient fully it is necessary to examine their motivation, efficacy, and goals, then apply a theoretical model to our intervention.
Transtheoretical Model[edit | edit source]
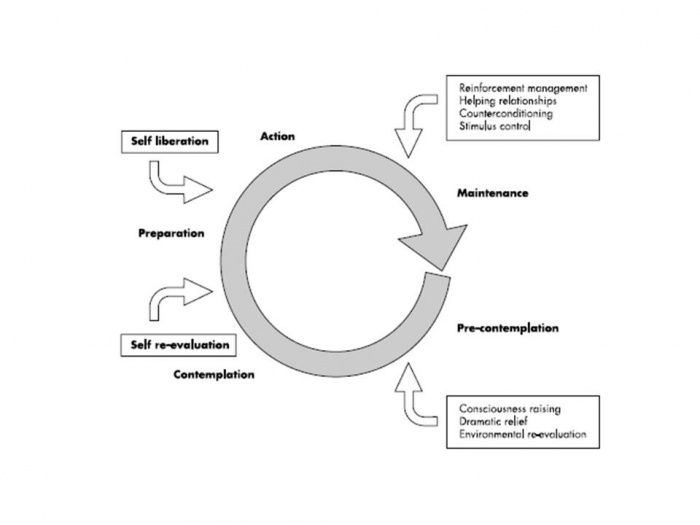
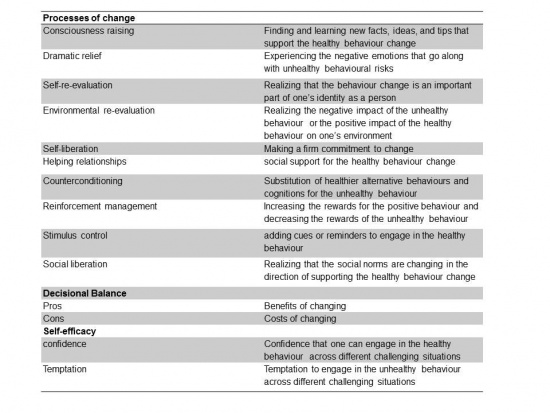
The TTM[7] consists of five stages related to behavioural change, pre-contemplation, contemplation, preparation are the motivational stages of the theory where the idea of changing behaviour varies from not at all too ready to change. These stages are followed by action and maintenance, during these stages the behaviour has been modified for less than six months and then established over the next six months. Depending on how the individual reacts to the process of change progression and regression between stages can occur. There are ten processes of change that need to be considered when changing behaviour and each can relate to a specific stage in the model these are the actions taken by the individual to develop a rationale for their changing behaviour it will help them overcome any potential barrier they may encounter in their pathway through the stages of change.
Prochaska et al. (1992)[7] proposed that the effectiveness of the process of change will vary according to the individual's stage of readiness to change. From a physiotherapy perspective the processes of change could affect an individual’s behaviour towards an intervention in numerous ways. For example, consciousness raising will make the patient more aware of why they are performing the intervention, Self-liberation will provide the individual with the belief that committing or recommitting to an intervention will lead to behavioural change and to act on that belief[9] and helping relationships such as the relationship between physio and patient will also help to facilitate change. These are just three of the ten processes of change and each process may have an impact on different stages of change. The aforementioned will affect the pre-contemplation, contemplation and action stages of the TTM.
Furthermore, within the TTM there are different measures of behaviour that affect the individual's progression through the stages[10]. These measures include decisional balance, self-efficacy and temptation. The decisional balance aspect of the theory involves weighing up the pros and cons of changing. The use of self-efficacy within this model was adapted from Bandura’s self-efficacy theory[11]. It is defined as the confidence the individual has in their ability to cope with situations where relapse is extremely likely. Temptation is the intensity of urges to engage in a specific behaviour when the individual is in a certain situation[9]. These concepts can be analysed by a temptation measure or a self-efficacy measure as both are similar in structure[12]. These outcome measures are particularly useful in that latter stages of change and beneficial establishing why a relapse has occurred ). If we examine the model as a whole, the stages of change are the central construct of the TTM, the processes of change are theorised as independent variables, and decisional balance, self-efficacy and temptations are hypothesized as intermediate dependent outcomes[10][13].
The TTM has been used in a telehealth setting previously via mobile phone interventions. Obermayer et al. (2004)[14] and Riley et al. (2008)[15] used text messaging (SMS) interventions to promote smoking cessation and found 25% difference in participants who managed to quit smoking after six weeks using the same intervention and a similar patient age group. Therefore using the TTM could be beneficial for specific patient groups within a physiotherapy setting as long as the intervention develops as the patient progress through the stages of the model in order to develop the desired behavioural change. The ICF framework takes into account all the biopsychosocial factors necessary for regaining health and is well established within physiotherapy practice. The use of behaviour change models, in particular the TTM, can work in harmony with the ICF framework and as suggested by Riley et al. (2008)[15] should be adapted to meet the needs of the individual over time. When a physiotherapist is implementing an intervention for a specific patient, the goals will be patient-centred. Therefore the physiotherapist must understand what the needs of the patient and investigate these needs further and establish the barriers and facilitators which may present themselves during the intervention[16]. Once the appropriate subjective and objective examinations have been implemented the correct application and choice of techniques is imperative and there must be an assessment of whether or not the intervention has been successful[16]. As the patient is moving through the stages of change the ICF model will be used at each stage to ensure patient-centred practice. It is important that we, as the physiotherapist look at all the biopsychosocial considerations before developing our clinical reasoning for a behavioural change intervention[17].
Self-Efficacy Theory[edit | edit source]
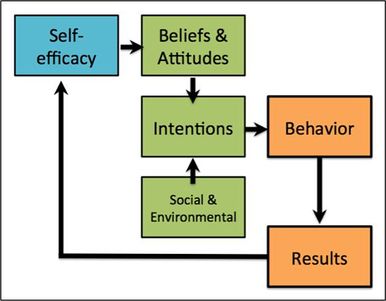
Self- efficacy theory was first proposed by Bandura (1982)[11] it refers to an individual's sense of confidence in their ability to execute a specific behaviour in different environments[18]. An individual’s level of self-efficacy will depend on the amount of perseverance and effort applied to a specific behaviour[11]. The individual's view of their efficacy may shape their actions, effort and attitude[19][20]. An essential component of self-efficacy theory is that the stronger the belief a person has in their ability to perform a set of actions, the more likely they are to comply and maintain participation throughout an intervention. However, those who have an inferior amount of self-efficacy could apply less effort and have an increased chance of relapsing when trying to change their behaviour[21]. Furthermore Bandura (1997)[18] suggest that a person's level of self- efficacy is based on personal beliefs rather than objective assessments. Therefore a person’s beliefs can often predict their behaviour more accurately than their capabilities. This can result in a behaviour level that does not match the individual's capabilities and could be why behaviour between individuals varies even when they have similar understanding and skills set[22]. It could then be argued that having self-efficacy alone could be sufficient enough to initiate a behavioural change[18].
There are many barriers to self-efficacy especially in the elderly and vulnerable populations that telehealth interventions are designed for. Misunderstanding the ageing process among older adults may result in restricted activity levels[23]. Lack of knowledge about the benefits of exercise may produce a dismissive attitude toward participation towards interventions involving physical activity[24]. More so, Supposed ill-health and symptoms related to physical disabilities associated with chronic disease are reasons behind dropping out of an intervention[25][26]. Within this population group, many of the barriers to activity are attitudinal and we must use the self-efficacy theory in order to provide appropriate interventions that instil confidence and belief in the individual to help them to modify their behaviour[22].
Existing literature has concluded that self-efficacy-based interventions to improve physical activity levels had a significant effect on outcome measures such as distance walked among older adults[27] and improvements in physical activity levels[28], but not in self-efficacy itself. This could indicate that self-efficacy is not necessary for bringing change in physical activity behaviour. This has been further emphasised by Calfas et al. (1997)[29] and McAuley et al. (1994)[30] who also used theory-based interventions and found no connection between self-efficacy and behavioural change. Another limitation with self-efficacy literature especially with physical activity interventions is the lack of reporting by the authors on the actual content of the intervention making it difficult to compare interventions and standardisation of behavioural change techniques[31].
Conversely, physical activity interventions aiming to improve self-efficacy have improved confidence and the individual's adherence to physical activity interventions[32][33]. Existing research confirms that self-efficacy beliefs are critical in the initial adoption of an exercise routine[22]. If the participant is able to believe that they can exercise under circumstances that could result in the relapsing behaviour it is more likely that they will take part in exercise intervention[34][35]. Therefore including self-efficacy theory in the design of physical activity intervention would be advantageous in guiding the participant towards adopting a new behaviour. Furthermore, In a systematic review by (Ashford et al. 2010)[31] they found that self-efficacy was increased when the parts of the intervention were performed by a peer prior to the participant taking part and therefore knowing that another person was able to perform the activity gave the participants increased confidence in their own capabilities.
In summary self-efficacy is a vital component of behavioural change, confidence in one’s ability to perform a certain behavioural change intervention. Looking at self-efficacy from a physiotherapy perspective it would apply the same principles as the physical activity interventions mentioned above. Influencing beliefs and establishing barriers to interventions could be influential when developing a telehealth intervention. Self-efficacy could be essential in patients complying with any intervention that may be beneficial to their health including mobile applications aimed at a specific injury, a health condition or chronic pain intervention.
Motivation[edit | edit source]
Motivation is a complex term and has been subjected to various definitions and approaches. Csikszentmihalyi[36] defines motivation as “a phenomenal experience being a sufficient reason for action”, which then lead Deci and Ryan[37] to further develop its content focusing on the “functional significance of events” as the main determinant for motivation.
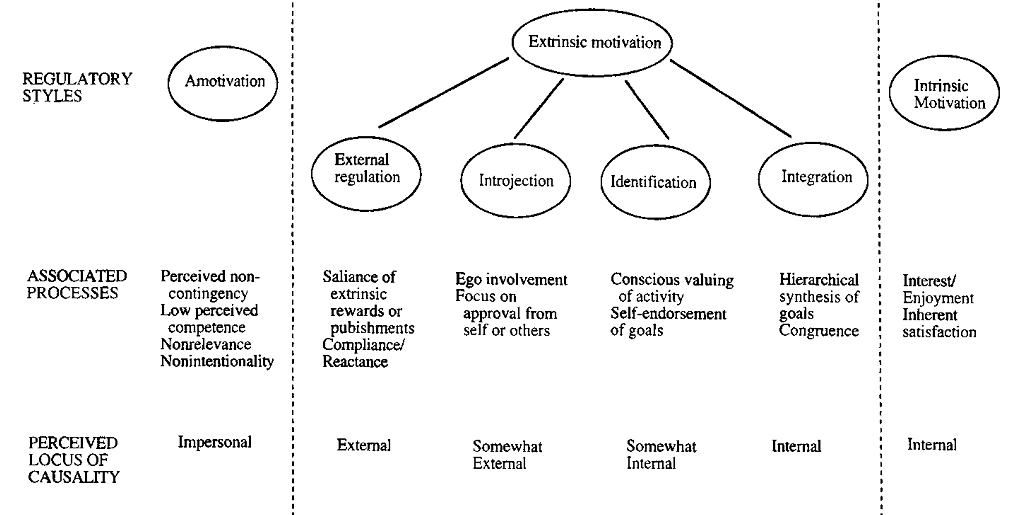
In Self-Determination Theory, Deci and Ryan[38] separate motivation into types, centred on the different goals that lead to the development of an action:
- Intrinsic motivation, which denotes the act of doing something because it is inherently interesting or enjoyable thus leading a person to act for the fun or challenge rather than because of external prods, pressures, or rewards. Spontaneous behaviours, which confer benefits to the organism, are not completed for any instrumental reason rather than constructive experience associated with exercising and empowering one’s capacities.
- Amotivation, which refers to the state of lacking an intention to act. Individuals who are amotivated (unmotivated) lack intentionality and sense of personal causation due to the fact that they are not valuing an activity, not feeling competent to do it, or not believing it will lead to the desired outcome.
- Extrinsic motivation, which denotes the act doing something because it leads to a separable outcome: social demands and roles that require individuals to assume responsibility for non-intrinsically stimulating duties. It can be further defined into four categories:
- External regulation, in which individuals perform tasks to satisfy an externally imposed demand.
- Introjection, in which individuals perform tasks in order to avoid guilt or anxiety or to enhance self-esteem.
- Identification, in which individuals identify the own importance of behaviour, accepting its rules as his or her own.
- Integration, in which individuals entirely assimilate rules and regulations and those are congruent with his or her own values and needs.
The motivation between individuals varies in amount, level (how much?) and orientation (what type?). The orientation of motivation refers to the essential attitudes and goals that lead to the development of a certain action (why are we doing this?). Research across various settings supports the role of communication in enhancing psychological functioning, self-regulation and intrinsic motivation.
The ideal situation is that an individual is able to self-monitor himself because he truly believes in the intervention and knows how this is intrinsically important for him/her[39] or because the enjoyment of the activity leads to the adoption of a certain lifestyle[40]. If neither self-consciousness or enjoyment could lead an individual to change its behaviour towards a healthier lifestyle, family encouragement and family cohesion could determine better outcomes within the rehabilitation setting[41].
Self-determination theory[edit | edit source]
Self-determination theory[42][43] is a macro‐theory of human motivation, personality development, and well‐being. The theory focuses especially on volitional or self‐determined behaviour and the social and cultural conditions that promote it[44]
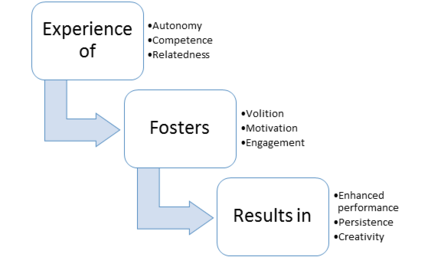
Ryan and Deci[42] propose three basic human needs involved in self-determination which motivate people to initiate behaviour:
- Autonomy, which is the perception of experiencing a sense of choice and psychological freedom in the initiation of activities,
- Competence, which is the ability to master challenges and the perception of being effective in dealing with the environment,
- Relatedness, which is the sense of being cared for and connected to other people
The quality of motivation is enhanced when any of these needs are satisfied, optimized if all three are satisfied and diminished if the person feels frustrated[45].
A person’s motivation for an activity is a dynamic and constant continuum which development is based on certain aspects. External factors reduce feelings of autonomy thus prompting a shift from autonomous to controlled motivation or amotivation. On the other side, several other factors promote autonomous motivation[46].
Motivational states exist along this SDT continuum with amotivation (a state in which there is no intention to act) being the bottom form of motivation and intrinsic motivation (a state in which an action is performed for purely joy and interest of the activity itself) being the top form.
Extrinsically motivated behaviors, cover the continuum between amotivation and intrinsic motivation, varying in the extent to which their regulation is self-determined. These include external regulation, introjected regulation, identified regulation and integrated regulation. Externally regulated motivation (i.e., the least self-determined form of extrinsic motivation) results in behaviors performed to obtain rewards (e.g., praise, monetary compensation) or to avoid negative consequences (e.g., criticism from others).
Goal Setting[edit | edit source]
The Aristotelic theory of final causality, in which every action is caused by a purpose, is the basic connection between Ryan and Deci[43] Self-Determination Theory and Locke[47] Goal-Setting theory.
“A Goal is the object or the aim of an action”[47]
Goals have both internal (ideas) and external (object or condition to which they refer) aspects.
Goals help individuals to serve their dispositional desires, channelling them in a more concrete direction to be satisfied in an effective and efficient manner: internal aspect guides action to attain the external, desired state[48]
Goals vary in content (the inner object) and intensity (the scope, focus of the selective process).
Locke[47] demonstrated the goals vary qualitatively (the goal content is what the person is seeking) and quantitatively (difficulty and specificity influence the content of a goal), summarizing that:
- The more difficult the goal, the greater the achievement.
- The more specific or explicit the goal, the more precisely performance is regulated.
- Goals that are both specific and difficult lead to the highest performance and commitment.
- Commitment to goals is attained when the individual is convinced that the goal is important and attainable.
To underline the importance of setting specific and difficult goals that, with feedback, lead to higher performance, Locke developed 5 fundamentals principles that constitute an effective goal setting:
- Clarity: Goals are measurable and unambiguous. There should be no misunderstanding regarding which behaviours will be rewarded.
- Challenge: Goals are challenges. If a task is too easy, don’t expect the accomplishment to be significant.
- Complexity: if Goals are highly complicated, make sure that the individual won’t fight in the face of overwhelming odds.
- Commitment: Goals acceptance implies effort, over time, towards the accomplishment.
- Feedback: provides knowledge on progress towards the Goals.
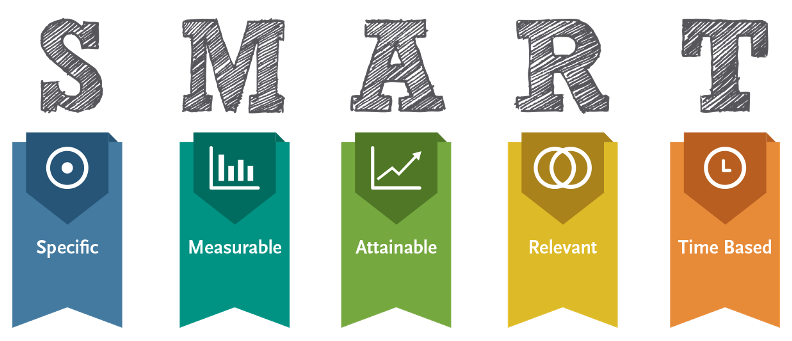
In 1981, Doran[49] published an article titled “There’s a S.M.A.R.T. way to write management’s goals and objectives” in which described new criteria on how to write meaningful objectives. The article underlined that goals, to be effective, should be relevant to the person involved, challenging but still achievable and realistic, and specific (in order to be measured):
S.M.A.R.T. goals are used every day in rehabilitation settings, even if difficult to develop and time-consuming[50]. In fact, despite the SMART acronym clearly derives from the Goal Setting Theory and it is routinely used by physiotherapists, there is little research on how to develop an optimal goal setting method for a patient. Using this simple acronym, some limitations could arise:
- Specific, but changeable!
- Measured, by the patient or by health carers or by both?
- Achievable, but may still be challenging!
- Relevant, to whom?
- Time, limited by who?
Clinical Implications[edit | edit source]
Maclean[51] investigated the role of motivation in clinical settings, stating its importance in determining patient outcomes and underlying the difficulties encountered when promoting its development. To increase a patient’s motivation, the authors suggest:
- Goal setting (clear and revisable), including patient feelings and point of views (which should be accepted and respected)
- Accept patient’s idiosyncrasies and worth patient’s value system
- Have a warm, approachable and competent manner
- Remind the patient that goals exist beyond the ward setting
- Do not stress the responsibility for motivation and recovery merely on the patient
Future research could focus on improving our telehealth behaviour interventions but also our theoretical and practical understanding of health behaviour change[3]. However, from the research associated with specific models as a theoretical basis for other types of intervention, there is generally an improvement in patient behaviour. In the development of applications is important that we can tailor the intervention to suit the individual and are able to SMART set goals, motivate and ensure progression through behaviour change models in the short term as well as in the long term.
Using Smartphone Applications in Physiotherapy[edit | edit source]
Following an understanding of what motivates patient behaviour and adherence to healthcare treatments discussed above, this section will look more specifically at factors that have an impact on the patient’s ability to respond and agree to treatment in the form of home exercise programmes (HEPs) as well as the potential for healthcare and physiotherapy smartphone applications to deepen the patient-physiotherapist relationship and improve overall rehabilitation of the patient in a musculoskeletal setting.
In an outpatient setting, a HEP is tailored to an individual patient and targets their specific problems, as identified by the Physiotherapist. This exercise schedule, modified with repetitions, sets and/or additional strengthening/ endurance components, is to be performed by the patient in their home environment between treatment sessions with the Physiotherapist. Continuation of training at home ensures that a patient will begin to improve and that their progress can be monitored throughout time. The continued tailoring of the HEP from each session by the physiotherapist must be complemented by the patient’s continued determination and trust in their shifting programme. The understanding and commitment between both the patient and their physiotherapist to achieve both short-term and long-term goals indicates a better outcome for the patient once they are back to (or potentially better than) their baseline. However, various reports monitoring patient compliance with and to a HEP show non-adherence rates to be as low as approximately 20% ([52]; [53]).
In addition to factors and models described above such as goal setting, self-efficacy, intrinsic and extrinsic motivation (self-determination theory) and the transtheoretical model there are other circumstances which can affect the ability of patients to respond positively to a home exercise programme. While demographics such as age and gender have been shown to have little effect on these rates ([52]), there are a few factors that have been discovered and discussed in the research that may affect compliance such as:
- Low levels of physical activity at baseline
- Anxiety, depression and pain
- Poor social support
- Greater perceived barriers to exercise
- Poor understanding about their condition
- Difficult to commit to the time needed to exercise
- High cost of treatment
Through a greater understanding of the patient perspective, Physiotherapists alongside the multi-disciplinary team can work to target and ensure that patients are kept on the right track and allow greater improvement of quality of life. However, with an adherence rate of 20% keeping most patients isolated from full recovery, what can we do to strengthen the patient-physiotherapist relationship?
This is where the potential of telerehabilitation comes in. Discussed in the beginning sections, telerehabilitation is the modernization of healthcare-related treatments and services. Mobile technologies are still fairly recent and just starting to emerge; therefore there is not a wealth of information or research on their use or advantages.
Further Considerations: Improved Communication [edit | edit source]
Facilitating Patient-Provider Relationship[edit | edit source]
Physiotherapy smartphone applications, which aim to support home exercise programs can help further engage the patient throughout treatment. In healthcare, the term compliance is often defined as the 'patient's behaviours (in terms of taking medication, following diets or executing lifestyle changes) that coincide with healthcare providers' recommendations for health and medical advice' [54]. As mHealth continues to evolve, it is predicted that it will provide the foundation to support self-management, health monitoring, self-directed learning and interactive patient-clinician communications into the future [55].
Utilising Reminder Services to Enhance Communication[edit | edit source]
There are several issues with therapeutic non-compliance, including two major clinical issues concerning the effect on treatment outcomes and increased financial burden for society [54]. A significant contributing factor to therapeutic non-compliance is the failure to attend scheduled appointments. Research has documented several characteristics contributing to this absenteeism including demographic variables, family responsibility, ethnicity and religion [56]. For the purpose of this discussion, we will only consider the most common reason for not attending appointments, which is forgetfulness ([57]; [58], [56]). If the reader would like to further follow up on reasons why outpatients fail to attend their scheduled appointments, please follow this link here. It has been implied that SMS (short message system) reminders can play a role in reducing non-attendance at outpatient clinics [58]. Additionally, researchers have tested the use of SMS across different preventative health behavior interventions and suggested its usefulness to provide patient education, appointment reminders, behavioural interventions, data acquisition and communication between patient and healthcare provider [59].
The message feature appears to benefit the physiotherapy practice, where the clinician is able to send 'push messages' to the patient's phone to inform them about available services, send promotions or links to their website. There is an option for the physiotherapist to incorporate personal comments on the patient program, which the patient receives on the application [60]. This application is clinic branded and offers the patient easily accessible contact details for the clinic through the main app page.
Several studies have shown the use of SMS reminders play a positive role in reducing non-attendance at out-patient clinics [57]. Literature focuses on the SMS feature found across many apps, but limited research is available concerning embedding reminders and messages in smartphone systems utilizing push notifications. For the purpose of this discussion, they will arguably apply similar outcomes, as they offer pop up reminder to attend an appointment. Research is also lacking into physiotherapy musculoskeletal outpatient clinics, as one review looked specifically across 10 major clinical domains including Activities of Daily Living, Alzeheimer's/Dementia care, Chemotherapy symptom management, palliative care management, congestive heart failure, chronic obstructive pulmonary disease, diabetes, falls and falls risk, osteoarthritis and dermatology [58]. SMS reminders appear to have a significant impact on adherence to appointments and would be relevant to physiotherapy musculoskeletal outpatient clinics. Additionally, the use of SMS and increased communication between the patient and physiotherapist can further benefit patient participation in a rehabilitation program.
Recent research has identified that text-messaging improves outcomes in an outpatient cardiovascular rehabilitation setting. In this study, text messages were sent 3-5 times weekly and consisted of heart-healthy tips, requests for weight and blood pressure input and minutes of exercise per day as well as medication adherence [61]. Results from this study indicated that the addition of SMS is cost-effective and significantly improves outcomes and compliance alongside a traditional cardiorehabilitaiton program [61]. Historically, SMS represents the most frequently used mobile phone feature in research focused on the role of mobile phones as a tool for encouraging and monitoring health, with much of this literature is specifically centered on diabetes management and weight loss [62]. Text messages were most often used to send motivational messages, educational information, social support and for self-monitoring [62]. It would be beneficial to identify research supporting these physiotherapy applications and the future ways that physiotherapy smartphone applications can incorporate messages to stimulate behavior change.
Facilitating Knowledge and Education Through Physiotherapist Communication[edit | edit source]
Another strong predictor on patient participation in healthcare is effective patient knowledge about their condition and course of action. Patient education is extremely important to enhance therapeutic compliance and healthcare providers should supply patients with adequate education about their treatment and disease [54]. [63].Education for patients is important as many patients describe not attending appointments because they perceived that their appointment was unnecessary. Providing clear information to patients is important since many patients appear to lack understanding over their own healthcare [56]. Communicating relevant information about the patient's condition can further engage the patient in his or her own treatment concerns and builds a greater understanding and partnership with the physiotherapist.
Communicating The Right Exercise Prescription[edit | edit source]
Finally, the importance of communicating the appropriate exercise prescription in an interactive manner is discussed. mHealth applications create new opportunities for patients to strengthen their relationship with their therapist, reinforce standing of the plan of care, confirm home exercise techniques and proactively address relevant concerns.
Rehabilitation professionals can utilize this information to better understand any relevant environmental factors affecting exercise adherence as well as utilizing this real-time data to receive patient feedback that is less subjective to recall bias in future appointments [55].
An important feature for patient participation in healthcare is accessibility and satisfaction with the healthcare facilities [54]. These physiotherapy applications help to promote healthcare facilities remotely in the patient's own environment. An important feature of the application is that is must be useful and usable, and this may link with adoption and frequent use of mobile application [62]. If the physiotherapist is able to communicate effectively with the patient about their condition, treatment and home exercise options using any of these applications, there will likely be improved patient participation and engagement with their rehabilitation process.
Key Points[edit | edit source]
Further considerations: Facilitating behaviour change[edit | edit source]
As a physiotherapist, it is imperative to create a trustworthy relationship with your patient and understand their psychosocial beliefs and behavior in order to effectively tailor a rehabilitation program for them. Importantly, patient's beliefs about the causes and meaning of illness as well as motivation following therapy are strongly related to their compliance with health care [64]. Unfortunately, effective strategies to promote behavior change in individuals with little or no motivation to change are relatively scarce[65]. These motivational states exist on a continuum between amotivation and intrinsic motivation, and it is up to the physiotherapist to identify what factors will help the patient engage in treatment.
For an individual who is intrinsically motivated, the use of physiotherapy smartphone applications may be enjoyable due to their inherent desire to challenge themselves. Apps may empower the patient to keep track of their own progress electronically, which they might enjoy.
However, intrinsic motivation may play more of a role in maintaining healthy behaviour following discharge from physiotherapy, when a patient may choose to continue preventative exercises or participate in an activity or sport for fun to keep healthy. However, these apps might further support individuals who are more extrinsically motivated since the applications create a direct partnership with the physiotherapist and allow these individuals to be externally regulated and tracked to support their motivation. Apps may allow the physiotherapist to monitor if the patient is accomplishing their program as well as the option to send text messages as additional reminders and motivation if required. Importantly, applications may provide the patient with educational resources, further allowing the patient to identify with their condition and the importance of their behavior to accomplish the rehabilitation program in order to improve. Mobile phone technology offers convenient real-time self-monitoring as well as timely delivery of feedback, which are two strategies to facilitate behavior change[62].
There are three basic human needs proposed for self-determination which motivate people to initiate behaviour: autonomy, competence and relatedness[42]. It can be argued that all three needs can be impacted by the use of these physiotherapy applications. Firstly, autonomy can be promoted by a physiotherapist-patient relationship where the patient is engaged with their condition and feels that it is their decision to use the smartphone home exercise program. Secondly, competence allows the patient to take the smartphone home exercise program into his or her own environment and feel mastery over their ability to complete the exercise. Lastly, relatedness allows the patient to feel cared for by the physiotherapist and connected through effective lines of communication that certain applications offer. General findings show that patients who have emotional support and help from not only family and friends but also their healthcare providers, are more likely to participate in treatment[64]. The use of smartphone applications may in fact increase the experience of these three domains, which will foster motivation and result in enhanced performance[42].
In addition to motivational constructs identified in the Self Determination theory, the first three phases of the Transtheoretical model are motivational in nature, and include proposed processes of change[7]. The physiotherapist can engage the patient to move through the stages with efforts such as reinforcement management, where the physiotherapist has monitored patient progress through the application and rewards the patient on making changes. The patient can also be impacted by consciousness raising, where the patient finds out more of the effects of the behavior by engaging in the home exercise program and reading up on literature about their condition. As previously mentioned, patient education is very important to enhance compliance [64] alongside the stage the patient is at in their readiness to change[7]. By applying these motivational aspects in various physiotherapy applications, patients will be more likely to change their behaviours during and after rehabilitation. The Transtheoretical Model is intrinsically linked to self-efficacy; see more below.
Self-Efficacy and Goal Setting[edit | edit source]
Self-efficacy is a major behavioural model focusing on the internal belief of a person in their ability to achieve a certain task. In this way, the more likely a person is to believe in themselves and their capacities, the more likely they are to succeed in their performance [66]. Self-efficacy is reinforced by previous successes in the past, which makes it easier for people to believe in and persevere through adverse events in their future. This theory is applicable to the patient-physiotherapist relationship and the patient’s motivation for and dedication to their home exercise program. Progress and feedback for rehabilitation can be tracked, monitored and discussed with patients to ensure that patients see their progress and ultimately improve their self-efficacy through completion of tasks. Encouragement to persevere can be provided by the physiotherapist if they feel as though a patient’s motivation to perform the home exercise program has dropped through text messages between the application or through e-mail. Reminders from the application may also prove helpful.
Goal setting will have a profound effect on compliance as it is intrinsically linked with self-efficacy. In-home exercise programmes, it is important the physiotherapist and the patient both work together to set and achieve goals which are specific, measurable, achievable, realistic and have a time-frame to work towards; in other words, these goals will be S.M.A.R.T.[49]. Similar to other models, goal setting is most effective when feedback is received by both the physiotherapist and the patient[47]; this ensures that both parties can understand what stage the patient is at in terms of rehabilitation and support them as required.
“A theory of goal setting and task performance”, developed by Locke et al. 1990, also discusses that these goals should follow five fundamental principles. Clarity is ensured by all four applications as a home exercise programme will either be created virtually, stored online, printed or emailed so the patient can go back to see the immediate short-term goals decided upon by the patient, or the patient alongside the physiotherapist. Goals also have to be challenging but not too complex; applications that will allow constant communication between the Physiotherapist and patient ensures that the task or exercise is attainable but not too simplistic for the patient to perform. Commitment is equally important and patient progress monitoring, as well as messaging, allows the physiotherapist to analyse and understand the patient’s growth over time so feedback can be communicated to the patient.
Currently, there is limited research measuring the usage of a health-related smartphone application and its effect on the behavior of users. The majority of health applications available for consumers are funded by commercial companies, which are disinclined to distribute their usage information in a competitive market [67]. Further research is necessary to help support the connections we have discussed between smartphone physiotherapy apps and behaviour change models.
References[edit | edit source]
- ↑ Gale, N., Sultan, H. Telehealth as ‘peece of mind’: embodiment, emotions and the home as the primary health space for people with chronic obstructive pulmonary disorder. Health and Place 2013; 21(): . http://www.sciencedirect.com/science/article/pii/S1353829213000129 (accessed 25 November 2015).
- ↑ Dahlia, K., Tousignant, M., Leclerc, N., Cote, A., Levasseur, M. The Patient’s Perspective of in-Home Telerehabilitation Physiotherapy Services Following Total Knee Arthroplasty. Public Health 2013; 10(): . http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3799503/pdf/ijerph-10-03998.pdf (accessed 25 November 2015).
- ↑ 3.0 3.1 3.2 Riley WT, Rivera DE, Atienza AA, Nilsen W, Allison SM, Mermelstein R. Health behavior models in the age of mobile interventions: are our theories up to the task? Translational behavioral medicine 2011;1(1):53-71.
- ↑ Ruiz EC, Hierro MG, Torres PM, Massoomi F, Brown ME, May-Russell S, et al. PHARMACY. 2012.
- ↑ PATRICK, K., RAAB, F., ADAMS, M. A., DILLON, L., ZABINSKI, M., ROCK, C. L. GRISWALD, W.G. AND NORMAN, G. J. (2009). A text message–based intervention for weight loss: randomized controlled trial. Journal of medical Internet research. vol.11, no.1.
- ↑ PROCHASKA, J. AND DICLEMENTE, C (1983). Stages and processes of self- change in smoking: toward an integrated model of change. Journal of consulting and clinical psychology. Vol.5. pp. 390-395.
- ↑ 7.0 7.1 7.2 7.3 PROCHASKA, J. O., DICLEMENTE, C. C., AND NORCROSS, J. C. (1992). In Search of How People Change: Applications to the Addictive Behaviors. American Psychologist. vol. 47, pp.1102–1114.
- ↑ ADAMS, J. AND WHITE, M. (2003). Are activity promotion interventions based on the transtheoretical model effective? a critical review. British Journal of Sports Medicine. vol.37, no.2. pp.106-114.
- ↑ 9.0 9.1 9.2 GLANZ, K., RIMER, B. K. AND VISWANATH, K. (2008). Health behavior and health education: theory, research, and practice. John Wiley & Sons.
- ↑ 10.0 10.1 VELICER, W. F, PROCHASKA, J. O., FAVA, J. L., NORMAN, G. J. AND REDDING, C. A. (1998). Smoking cessation and stress management: Applications of the transtheoretical model of behavior change. Homeostasis. Vol.38. pp. 216–233.
- ↑ 11.0 11.1 11.2 BANDURA, A. (1982). Self-efficacy mechanism in human agency. American psychologist. Vol. 37, no. 2. pp.122.
- ↑ VELICER, W. F., DICLEMENTE, C. C., ROSSI, J. S. AND PROCHASKA, J. O. (1990). Relapse situations and self-efficacy: An integrative model. Addictive Behaviors. vol. 15. PP. 271–283.
- ↑ DICLEMENTE, C. C. (2003). Addiction and change: How addictions develop and addicted people recover. Guilford: New York.
- ↑ OBERMAYER, J.L., RILEY, W.T., ASIF, O. AND JEAN-MARY J. (2004). College smoking-cessation using cell phone text messaging. J Amer Coll Health. vol. 53. pp. 71–78.
- ↑ 15.0 15.1 RILEY, W.T., OBERMAYER, J. AND, JEAN-MARY, J. (2008). Internet and mobile phone text messaging intervention for college smokers. J Amer Coll Health. vol.57. pp. 245–248.
- ↑ 16.0 16.1 HOMA, D. AND PETERSON, D. (2005) Using the international classification of functioning, disability and health (ICF) in teaching rehabilitation client assessment. Rehabil Educ. Vol. 19 pp. 119–28.
- ↑ JELSMA, J. AND SCOTT, D. (2011). IMPACT OF USING THE ICF FRAMEWORK AS AN ASSESSMENT TOOL FOR STUDENTS IN PAEDIATRIC PHYSIOTHERAPY: A PRELIMINARY STUDY. PHYSIOTHERAPY. VOL.97, NO. 1. PP. 47-54
- ↑ 18.0 18.1 18.2 BANDURA, A. (1997). Self-efficacy: The exercise of control. W.H. Freeman and Company: New York
- ↑ BANDURA, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review. vol. 84, no. 2. pp. 191–215.
- ↑ EYSENCK, H.J. (1978). Expectations as causal elements in behavioural change. Advances in Behaviour Research and Therapy. Vol. 1. pp. 171– 175.
- ↑ BANDURA, A. AND CERVONE, D. (1983). Self-evaluative and self-efficacy mechanisms governing the motivational effects of goal systems. Journal of Personality and Social Psychology. Vol.45. pp. 1017–1082.
- ↑ 22.0 22.1 22.2 LEE, L. L., ARTHUR, A. AND AVIS, M. (2008). Using self-efficacy theory to develop interventions that help older people overcome psychological barriers to physical activity: a discussion paper. International journal of nursing studies. vol.45, no.11. pp.1690-1699.
- ↑ LACHMAN, M., JETTE, A., TENNSTEDT, S., HOWLAND, J., HARRIS, B. AND PETERSON, E. (1997). A cognitive–behavioural model for promoting regular physical activity in older adults. Psychology Health and Medicine. Vol.2. pp. 251–261.
- ↑ KING, A.C., BLAIR, S.N., BILD, D.E., DISHMAN, R.K., DUBBERT, P.M., MARCUS, B.H., OLDRIDGE, N.B., PAFFENBARGER JR., R.S., POWELL, K.E. AND YEAGER, K.K. (1992). Determinants of physical activity and interventions in adults. Medicine and Science in Sports and Exercise. vol.24. pp. 221–236.
- ↑ CLARK, D.O. (1999). Identifying psychological, physiological, and environmental barriers and facilitators to exercise among older low-income adults. Journal of Clinical Geropsychology. Vol. 5. pp. 51–62.
- ↑ LIAN, W.M., GAN, G.L., PIN, C.H., WEE, S. AND YE, H.C. (1999). Correlates of leisure-time physical activity in an elderly population in Singapore. American Journal of Public Health. Vol. 89. pp.1578–1580.
- ↑ ALLISON, M.J. AND KELLER, C. (2004). Self-efficacy intervention effect on physical activity in older adults. Western Journal of NursingfckLRResearch. Vol. 26. pp. 31–46.
- ↑ ALLEN, J.K. (1996). Coronary risk factor modification in women after coronary artery bypass surgery. Nursing Research. Vol.45. pp.260–265.
- ↑ CALFAS, K. J., SALLIS, J. F., OLDENBURG, B. AND FRENCH, M. (1997). Mediators of change in physical activity following an intervention in primary care: PACE. Preventive Medicine. Vol. 26. pp. 297–304.
- ↑ MCAULEY, E., LOX, C., RUDOLPH, D. AND TRAVIS, A. (1994). Self-efficacy and intrinsic motivation in exercising middle-aged adults. Journal of Applied Gerontology. vol.13. pp.355–370.
- ↑ 31.0 31.1 ASHFORD, S., EDMUNDS, J. AND FRENCH, D. P. (2010). What is the best way to change self‐efficacy to promote lifestyle and recreational physical activity? A systematic review with meta‐analysis. British journal of health psychology. Vol.15. no.2. pp.265-288.
- ↑ DUNN, A.L., MARCUS, B.H., KAMPERT, J.B., GARCIA, M.E., KOHL III, H.W. AND BLAIR, S.N. (1999). Comparison of lifestyle and structured interventions to increase physical activity and cardiorespiratory fitness: a randomized trial. Journal of The American Medical Association. vol.281. pp.327–334.
- ↑ LEE, L.L., AVIS, M. AND ARTHUR, A. (2007). The role of self-efficacy in older people’s decisions to initiate and maintain regular walking as exercise—findings from a qualitative study. Preventive Medicine. vol.45. pp. 62–65.
- ↑ CLARK, D.O. (1996). Age, socioeconomic status, and exercise self-efficacy. Gerontologist. Vol. 36. pp.157–164
- ↑ SALLIS, J.F., PINSKI, R.B., GROSSMAN, R.M., PATTERSON. AND T.L., NADER, P.R. (1988). The development of self-efficacy scales for health-related diet and exercise behaviors. Health Education Research. vol.3. pp.283–292.
- ↑ Csikszentmihalyi M. Flow: The psychology of optimal performance. NY: Cambridge UniversityPress 1990
- ↑ Ryan RM, Deci EL. Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. Am Psychol 2000;55(1):68.
- ↑ Ryan RM, Deci EL. Intrinsic and extrinsic motivations: Classic definitions and new directions. Contemp Educ Psychol 2000;25(1):54-67.
- ↑ Teixeira PJ, Silva MN, Mata J, Palmeira AL, Markland D. Motivation, self-determination, and long-term weight control. Int J Behav Nutr Phys Act 2012;9(1):22.
- ↑ Cocosila M, Archer N. Adoption of mobile ICT for health promotion: an empirical investigation. Electronic Markets 2010;20(3-4):241-250.
- ↑ Rosland A, Heisler M, Piette JD. The impact of family behaviors and communication patterns on chronic illness outcomes: a systematic review. J Behav Med 2012;35(2):221-239.
- ↑ 42.0 42.1 42.2 42.3 Ryan R. Self determination theory and well being. Soc Psychol;84:822-848
- ↑ 43.0 43.1 Ryan RM, Deci EL. Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. Am Psychol 2000;55(1):68.
- ↑ Ryan R. Self determination theory and well being. Soc Psychol;84:822-848.
- ↑ Sanli EA, Patterson JT, Bray SR, Lee TD. Understanding self-controlled motor learning protocols through the self-determination theory. Frontiers in psychology 2012;3.
- ↑ Visser C. Self-determination theory meets solution-focused change: Autonomy, competence and relatedness support in action. InterAction-The Journal of Solution Focus in Organisations 2010;2(1):7-26.
- ↑ 47.0 47.1 47.2 47.3 Locke EA. Motivation through conscious goal setting. Applied and Preventive Psychology 1996;5(2):117-124.
- ↑ Deci EL, Ryan RM. Handbook of self-determination research. : University Rochester Press; 2002
- ↑ 49.0 49.1 Doran GT. There is a SMART way to write management’s goals and objectives. Manage Rev 1981;70(11):35-36.
- ↑ Bovend'Eerdt TJ, Botell RE, Wade DT. Writing SMART rehabilitation goals and achieving goal attainment scaling: a practical guide. Clin Rehabil 2009 Apr;23(4):352-361.
- ↑ Maclean N, Pound P. A critical review of the concept of patient motivation in the literature on physical rehabilitation. Soc Sci Med 2000;50(4):495-506.
- ↑ 52.0 52.1 DiMatteo RM. Variation in Patients’ Adherence to Medical Recommendations: A Quantitative Review of 50 Years of Research. Medical Care 2004; 42: 200-9.
- ↑ Dean SG, Smith, JA, Payne S, Weinman J. Managing time: An interpretative phenomenological analysis of patients’ and physiotherapists’ perceptions of adherence to therapeutic exercise for low back pain. Disability and Rehabilitation 2005; 27: 625-36.
- ↑ 54.0 54.1 54.2 54.3 Jin, J., Sklar, G., Oh, V., Li, S. Factors affecting therapeutic compliance: A review from the patient's perspective. Therapeutic and Clinical Risk Management 2008:4:269-286
- ↑ 55.0 55.1 Dicianno, B., Parmanto, B., Fairman, A., Crytzer, T., Yu, D., Pramana, G., Coughenour, D., Petrazzi, A. Perspectives on the evolution of mobile (mHealth) technologies and application to rehabilitation. Physical Therapy:2015:95:397-405
- ↑ 56.0 56.1 56.2 Collins, J., Santamaria, N., Clayton, L. Why outpatients fail to attend their scheduled appointments: a prospective comparison of differences between attenders and non-attenders. Australian Health Review 2003:1:52-63
- ↑ 57.0 57.1 Chen, Z., Fang, L., Chen, L., Dai, H. Comparison of an SMS messaging and phone reminder to improve attendance at a health promotion center: a randomized controlled trial. Journal of Zhejang University 2008:9:34-38
- ↑ 58.0 58.1 58.2 Geraghty, M., Glynn, F., Amin, M., Kinsella, J. Patient mobile telephone 'text' reminder: a novel way to reduce non-attendance at the ENT out-patient clinic. Journal of Laryngology & Oncology 2007:122:296-298
- ↑ Bouhaidar, C., Deshazo J., Puri, P., Gray, P., Robins, J., Salyer, J. Text messaging as an adjunct to the community-based weight management program. Computers, Informatics, Nursing 2013: 31: 469-476
- ↑ MyPhysio App. MyPhysio App home page. http://myphysioapp.com.au/home/ (accessed 4 Nov 2015).
- ↑ 61.0 61.1 Lounsbury, P., Elokda, A., Gylten, D., Arena, R., Clarke, W., Gordon, E. Text-messaging program improves outcomes in outpatient cardiovascular rehabilitation. IJC Heart&Vasculature 2015:7:170-175
- ↑ 62.0 62.1 62.2 62.3 Monroe, C., Thompson, D., Bassett, D., Fitzhugh, E., Raynor, H. Usability of mobile phones in physical-activity related research: a systematic review. American Journal of Health Education 2015:46:196-206
- ↑ PhysioAdvisor. PhysioAdvisor.com "Take control of your injury": home page. http://www.physioadvisor.com.au/ (accessed 4 Nov 2015)
- ↑ 64.0 64.1 64.2 JIN, J., SKLAR, G.E., MIN SEN OH, V., and CHUEN LI, S. Factors affecting therapeutic compliance: A review from the patient’s perspective. Journal of Therapeutics and Clinical Risk Management 2008; 4: 269-86.
- ↑ Hardcastle SJ, Hancox J, Hatter A, Maxwell-Smith C, Thorgersen-Ntoumani, Hagger MS. Motivating the unmotivated: how can health behavior be changed in those unwilling to change? Frontiers in Pyschology 2015; 6: 1-4.
- ↑ Bandura A. Self-Efficacy: Toward a unifying theory of behaviour change. Psychological Review 1977; 84: 191-215.
- ↑ Kirwan M, Duncan, MJ, Vandelanotte C, Mummery, WK. Using Smartphone Technology to monitor physical activity in the 10,000 Steps program: a matched case-control trial. J Med Internet Res 2012; 14: e55.
References[edit | edit source]
.