Chorea: Difference between revisions
No edit summary |
(added references) |
||
| Line 5: | Line 5: | ||
== Causes == | == Causes == | ||
They are predominantly of 2 types | They are predominantly of 2 types<ref name=":0">Termsarasab P. [https://journals.lww.com/continuum/Abstract/2019/08000/Chorea.9.aspx Chorea]. CONTINUUM: Lifelong Learning in Neurology. 2019 Aug 1;25(4):1001-35.</ref> | ||
* Acquired Causes | * Acquired Causes | ||
| Line 23: | Line 23: | ||
* '''Ballism'''- Variant of chorea which shows large-amplitude flinging movements involving proximal extremities. | * '''Ballism'''- Variant of chorea which shows large-amplitude flinging movements involving proximal extremities. | ||
* '''Athetosis'''-Slow writhing movements involving distal limbs sometimes may be facing. | * '''Athetosis'''-Slow writhing movements involving distal limbs sometimes may be facing. | ||
* '''Varying velocity of movements'''-quick velocity and low-amplitude movements accompanied by jerks. | * '''Varying velocity of movements'''-quick velocity and low-amplitude movements accompanied by jerks.<ref name=":0" /> | ||
{{#ev:youtube|RxWEilu-Mf4}} | {{#ev:youtube|RxWEilu-Mf4}} | ||
| Line 33: | Line 33: | ||
=== Differential Diagnosis === | === Differential Diagnosis === | ||
Specific diagnosis can be made on the basis of symptoms/clinical features experienced by the patient. These symptoms serves as diagnostic clues and are present as 3 body distributions and other crucial features. | Specific diagnosis can be made on the basis of symptoms/clinical features experienced by the patient. These symptoms serves as diagnostic clues and are present as 3 body distributions and other crucial features.<ref name=":0" /> | ||
1.On Forehead- [[Huntington Disease]]. | 1.On Forehead- [[Huntington Disease]]. | ||
| Line 71: | Line 71: | ||
== Multimodal Management == | == Multimodal Management == | ||
Chorea requires a Multidisciplinary Approach to be treated. | [[File:Mutimodal management chorea.jpg|right|frameless|387x387px]] | ||
Chorea requires a Multidisciplinary Approach to be treated.<ref>Feinstein E, Walker R. [https://link.springer.com/article/10.1007/s11940-018-0529-y An update on the treatment of chorea. Current Treatment Options in Neurology]. 2018 Oct;20(10):1-5.</ref> | |||
The team includes | The team includes | ||
| Line 83: | Line 84: | ||
* Genetic Counselor | * Genetic Counselor | ||
* Social worker | * Social worker | ||
=== Medical Management === | === Medical Management === | ||
1. '''Dopamine-depleting agents'''-Tetrabenazine, Deutetrabenazine, Valbenazine. | 1. '''Dopamine-depleting agents'''-Tetrabenazine, Deutetrabenazine, Valbenazine. | ||
| Line 100: | Line 98: | ||
== Physiotherapy Management == | == Physiotherapy Management == | ||
The management will be same as of Huntington's Disease. You can read it [https://www.physio-pedia.com/Huntington_Disease?utm_source=physiopedia&utm_medium=search&utm_campaign=ongoing_internal#Physiotherapy_Management here]. | |||
==References== | ==References== | ||
[[Category:Neurology]] | [[Category:Neurology]] | ||
[[Category:Neurological - Conditions]] | [[Category:Neurological - Conditions]] | ||
Revision as of 12:35, 25 August 2022
Introduction[edit | edit source]
The word Chorea has Greek origins meaning "to dance". It has a dance-like appearance due to the random and flowing quality of the movement. Chorea is a type of hyperkinetic movement disorder. The involuntary movements flow from one body area to another which cannot be predicted beforehand.
Causes[edit | edit source]
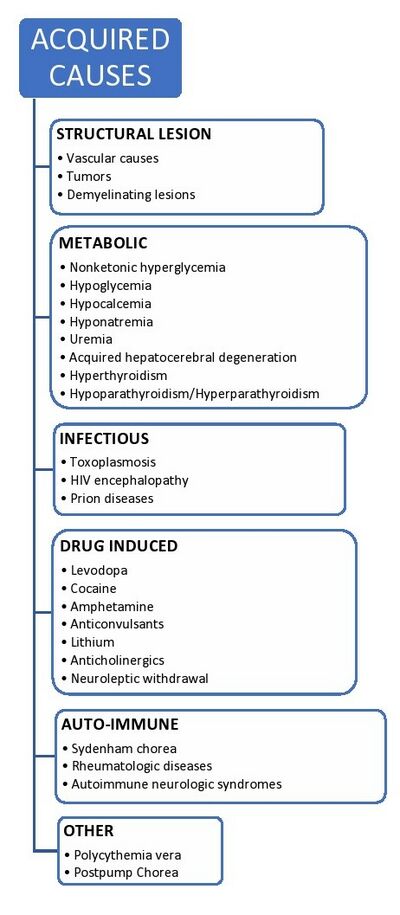
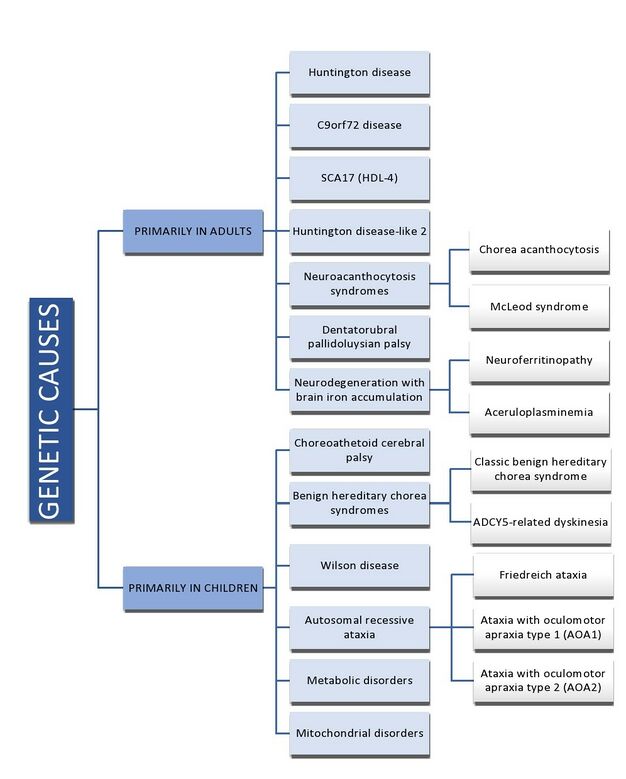
They are predominantly of 2 types[1]
- Acquired Causes
- Genetic Causes
Phenomenological Features[edit | edit source]
- Randomness
- Flowing Quality
- Parakinesia-Patients blend their chorea-induced movements with their own normal movements.
- Motor impersistence- the patient is unable to perform sustained motor activities.
- Ballism- Variant of chorea which shows large-amplitude flinging movements involving proximal extremities.
- Athetosis-Slow writhing movements involving distal limbs sometimes may be facing.
- Varying velocity of movements-quick velocity and low-amplitude movements accompanied by jerks.[1]
This video displays the dance-like movements performed by a patient.
Diagnosis[edit | edit source]
The phenomenological features mentioned above are observed to make a diagnosis of chorea.
Differential Diagnosis[edit | edit source]
Specific diagnosis can be made on the basis of symptoms/clinical features experienced by the patient. These symptoms serves as diagnostic clues and are present as 3 body distributions and other crucial features.[1]
1.On Forehead- Huntington Disease.
Wiggling of the eyebrows or activation of the frontalis muscle is present.
2. On Orobuccolingual region- Tardive Chorea, Acquired Hepatocerebral Degeneration ,Chorea-acanthocytosis, Lesch-Nyhan syndrome, PKAN(dystonia), Lubag Disease(dystonia).
Bonbon sign and problem of inappropriate intake of food is seen which cause biting of lips and tongue.
3.Localized to the contralateral subthalamic nucleus(hemichorea)- Nonketonic hyperglycemia, Polycythemia vera, Sydenham Chorea, Others.
Some disorders which are differentially diagnosed are given in the table below-
| Disorder/Symptom | Differentiating Factor from chorea |
|---|---|
| Dystonia | Predictable patterned movements |
| Dystonic Tremor | Irregular and jerky does not have a flowing quality like chorea |
| Myoclonic jerks | Randomness quality of chorea differs the two |
| Tics | Presence of premonitory urge and suppressibility |
| Stereotypies | Has stereotypic movement as if the video is running on a repetitive loop |
| Large amplitude cerebellar outflow tremor | Regular oscillation around the axis and activation of tremor with movements( postural and kinetic components) |
Multimodal Management[edit | edit source]
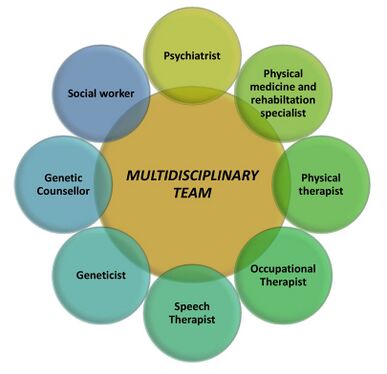
Chorea requires a Multidisciplinary Approach to be treated.[2]
The team includes
- Psychiatrist
- Physical medicine and Rehabilitation Specialist
- Physical therapist
- Occupational therapist
- Speech therapists
- Geneticist
- Genetic Counselor
- Social worker
Medical Management[edit | edit source]
1. Dopamine-depleting agents-Tetrabenazine, Deutetrabenazine, Valbenazine.
2. Dopamine D2 receptor-blocking agents-Haloperidol, Clozapine, Olanzapine.
3. Anticonvulsants- Valproic acid, Carbamazepine, Benzodiazepines, Levetiracetam.
4. Anti-glutamatergic agents-Amantadine, Riluzole.
5. Cannabinoids-Nabilone.
6. Deep Brain Stimulation
Physiotherapy Management[edit | edit source]
The management will be same as of Huntington's Disease. You can read it here.