Beta-blockers in the Treatment of Hypertension
Introduction[edit | edit source]
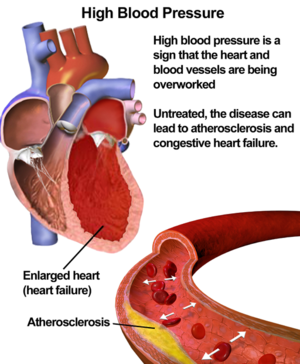
Beta‐blockers refer to a mixed group of drugs with diverse pharmacodynamic and pharmacokinetic properties. They have shown long‐term beneficial effects on mortality and cardiovascular disease (CVD) when used in people with heart failure or acute myocardial infarction.
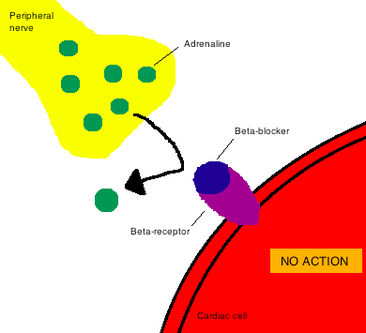
Beta receptors (tiny proteins) sit on the outer surface of many cells. There are three main types.
- Beta-1 receptors are found almost exclusively in heart cells.
- Beta-2 receptors reside mostly in lung and blood vessel cells, though heart cells also have some.
- Beta-3 receptors are located on fat cells[1].
Beta blockers are medications that have beta-adrenergic blocking properties, meaning they block sympathetic nervous system activity and effect Vagal tone . See link for full description of beta Blockers.
Evidence[edit | edit source]
Cochrane review findings 2017
- Beta‐blockers were not as good at preventing the number of deaths, strokes, and heart attacks as other classes of medicines such as diuretics, calcium‐channel blockers, and Angiotensin Inhibitors and Blockers.
- People given beta‐blockers are more likely to have side effects and stop treatment than people taking renin‐angiotensin system inhibitors, but there may be little or no difference in side effects between beta‐blockers and diuretics or calcium‐channel blockers.
- Beta‐blockers may reduce the number of strokes, an effect which appears to be similar to that of diuretics. However, beta‐blockers may not be as good at preventing strokes as renin‐angiotensin system inhibitors or calcium‐channel blockers.
- Beta‐blockers may make little or no difference to the number of heart attacks among people with high blood pressure.[2]
See also Pharmacological Management of Hypertension
References[edit | edit source]
- ↑ Harvard Edu. Beta Blockers: Jack of all trades Available from: https://www.health.harvard.edu/heart-health/beta-blockers-cardiac-jacks-of-all-trades(accessed 4.6.2021)
- ↑ Wiysonge CS, Bradley HA, Volmink J, Mayosi BM, Opie LH. Beta‐blockers for hypertension. Cochrane database of systematic reviews. 2017(1).Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5369873/ (accessed 5.6.21)