Chronic Graft Versus Host Disease
Introduction[edit | edit source]
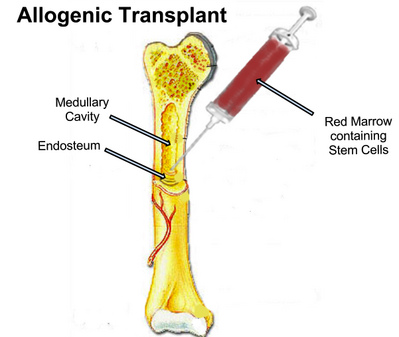
Graft versus host disease (GvHD) is a very common complication of bone marrow transplantations ( also known as allogeneic haematopoietic stem cell transplantation). Anti-rejection drugs have decreased the incidence, however it still occurs regularly.[1]
GvHD cause significant damage to the tissues affected, directly contributing to functional impairment. Treatment typically involves high-dose corticosteroids to suppress the immune system which can be destructive. Rehabilitation often is required to restore function and quality of life.[2]
Pathology[edit | edit source]
Graft versus host disease presents either early/acute (<100 days) or late/chronic (>100 days) post bone marrow transplantation, being a major complication. The skin, gastrointestinal tract (in particular the small bowel), and liver are the organs most often affected.[1]
How is GVHD Diagnosed?[edit | edit source]
A clinical diagnosis is usually made. Typically diagnosis includes the following:
- Immunologically competent cells present in the graft.
- The recipient has transplantation alloantigens appearing foreign to the graft and hence stimulate it antigenically.
- The recipient cannot mount an effective immunologic reaction against the graft, or enough time is allowed for the graft to manifest an immune response.[3]
Treatment[edit | edit source]
Treatment for GVHD is determined by the severity of symptoms and organs involved. Treatment options are based on immunosuppression with corticosteroids being the most commonly used treatment.[3]
What Are the Clinical Manifestations for cGVHD?[edit | edit source]
Acute GVHD typically involves the skin, gastrointestinal tract, and liver. It may involve the lungs, kidneys, eyes, and hematopoietic system. Decreased responsiveness to active immunization may also occur.
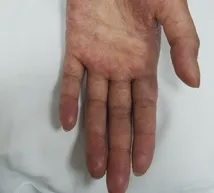
- Skin manifestation commonly arise as pruritic or painful maculopapular rash, first involving the palms, soles shoulders, and nape of the neck.
- GI symptoms usually include diarrhea and abdominal pain, but mucositis, mucosal ulceration, nausea, and vomiting. Liver involvement usually include abnormal liver function tests with elevated bilirubin and alkaline phosphatase levels.
Chronic GVHD has a presentation similar to collagen vascular disorders and systemic sclerosis. Death may occur due to recurrent infections (as a complication of immunosuppression).[3]
Physiotherapy[edit | edit source]
In put from the physiotherapist team may occur in the rehabilitation phase. Rehabilitation interventions may be required to manage complications such as reduced cardiopulmonary function, steroid-induced myopathy or bone and joint destructionPhysiotherapy can help client maintain a good quality of life.
Treatment may include:
- Increasing muscle strength
- Improving balance
- Increasing flexibility
- Reducing risk of falls
- Preventing development of muscular and joint contractures
- Providing equipment for mobility eg walking aids, orthoses, callipers and wheelchairs
- Advising on moving and handling techniques and equipment.[4]
References[edit | edit source]
- ↑ 1.0 1.1 Radiopedia Graft versus host disease Available: https://radiopaedia.org/articles/graft-versus-host-disease(accessed 28.1.2023)
- ↑ Smith SR, Asher A. Rehabilitation in chronic graft-versus-host disease. Physical Medicine and Rehabilitation Clinics. 2017 Feb 1;28(1):143-51.Available: https://www.sciencedirect.com/science/article/abs/pii/S1047965116300717?via%3Dihub (accessed 29.1.2023)
- ↑ 3.0 3.1 3.2 Vaillant AA, Modi P, Mohammadi O. Graft versus host disease. InStatPearls [Internet] 2022 Jul 8. StatPearls Publishing.Available:https://www.ncbi.nlm.nih.gov/books/NBK538235/ (accessed 28.1.2023)
- ↑ Manchester Physio Myopathies Available from:https://www.manchesterneurophysio.co.uk/adults/conditions-we-treat/orthopaedic-msk-conditions/myopathy/physiotherapy-treatment-for-myopathies.php (last accessed 22.11.2020)