Communication to Improve Health Outcomes
Original Editor - Robyn Holton, Frank Ryan, Shawn Swartz, Elaine McDermott, Noel McLoughlin, Zeeshan Mundhas
Top Contributors - Kim Jackson
Introduction[edit | edit source]
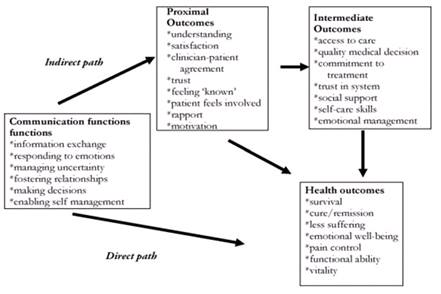
Communication in healthcare is vital and research has shown the interaction between practitioners and patient's can have an impact on health outcomes. To understand why communication may lead to better improved health outcomes researchers have identified pathways through which communication influences health and well being and can be simplified as proposed by Street[1].
Direct Pathways[edit | edit source]
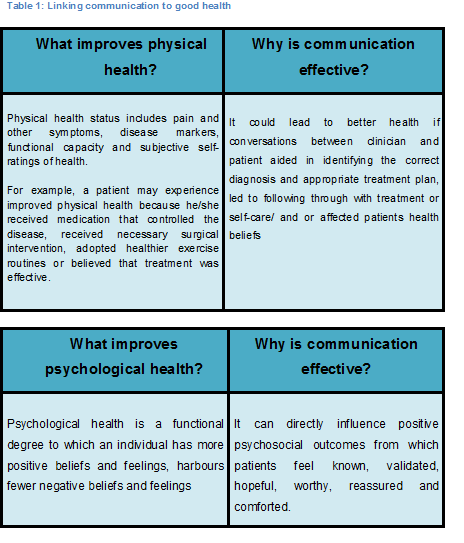
Talk may be therapeutic, meaning, a physiotherapist who validates the patients perspective or expresses empathy may help a patient experience improved psychological well being. Leading to the patient experiencing fewer negative emotions (e.g. fear and anxiety) and more positive ones (e.g., hope, optimism and self-worth).
Non-verbal behaviours such as touch or tone of voice may directly enhance well-being by lessening anxiety or providing comfort[2][3][4]
Indirect Pathways[edit | edit source]
In most cases, communication affects health through a more indirect or mediated route through proximal outcomes of the interaction, such as;
- Satisfaction with care
- Motivation to adhere
- Trust in the clinician and system
- Self-efficacy in self care
- Clinician - patient agreement
- Shared understanding
This could affect health or that could contribute to the intermediate outcomes (e.g., adherence, self-management skills, social support that lead to better health[5].
A physiotherapists clear explanation and expression of support could lead to greater patient trust and understanding of treatment options[1]. This in turn may facilitate patient adherence to recommended therapy, which in turn improves the particular health outcome. Increased patient participation in the consultation could help the physiotherapist better understand the patient’s needs and preferences as well as discover possible misconceptions the patient may have about treatment options[1]. The physiotherapist can then have the opportunity to communicate risk information in a way that the patient understands. This could lead to mutually agreed upon, higher quality decisions that best match the patients circumstances[1].
An article by Street et al.[1] explores these pathways to further broaden your knowledge. A link to this article can be found in ‘Further Reading’ section below.
Communication During Examination and Assessment[edit | edit source]
The medical interview, particularly the subjective assessment, will determine the quantity, quality and accuracy of data that the physiotherapist will elicit. In turn, this will affect both the approach to the problem and the consequent care of the patient[6]. Ensuring that we communicate effectively will directly influence the patients behaviour and well being for:
- Satisfaction with care[7]
- Adherence to treatment plans[7]
- Recall and understanding of the information given[7]
- Coping with the diagnosis[7]
- Quality of life and even state of health[7]
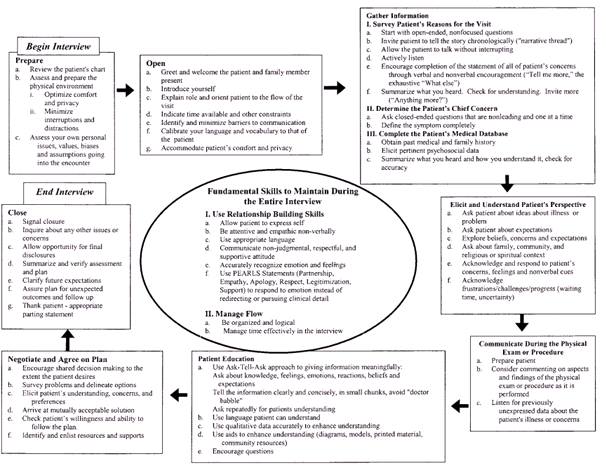
The Macey Model of Doctor-patient Communication is a communication skills model that illustrates fundamental processes applicable to every meeting between physician and patient, and represents a complete set of core skills[6].
Although this tool was developed for doctors, the model provides an overall framework for systematically teaching vital communication elements[6].
Improving Understanding[edit | edit source]
Miscommunication between patients and physiotherapists is often documented when it comes to diagnosis explanation and treatment advice [8] [9]. Patients will describe symptoms in “lay” terms while physiotherapists often return feedback based on biomedical symptoms and processes of the condition using medical terms without taking into account the gap in the level of knowledge on the subject between the patient and themselves[8] [9]. Research believes that this may be because some therapists forget to account for the difference in literacy levels between themselves and their patient, or they don’t know how to describe a condition outside of the medical model they have been taught during training.[10] .
Studies show that literacy levels in some countries can be as low as age 10 [11]. According to the Organisation for Economic Co-operation and Development,[12] the UK is now ranked 22nd in a study of 24 EU countries in terms of literacy with a national literacy age of 10 years old.
In addition to this English is not everyone’s first language. According to the 2011 UK census 92% of residents acknowledged English as their first language and of the 8% remaining (3.3 million people), only 79% claimed they could speak English well or very well [13]. Both of these factors may cause difficulty and confusion when trying to speak to a patient about their diagnosis and to make an informed decision around treatment options.
Understand Your Patient[edit | edit source]
In order to understand your patient, it is important to respect their background, culture and learning style. By getting a better understanding of patient’s learning styles and acknowledging the difference between lay and medical terminology, we can provide effective education which, in return, may increase the compliance and cooperation of patients[9]. Before educating the patient it is crucial that the following aspects are assessed:
- Patient's needs
- Patient's concerns
- Patient's motivation and readiness to learn
- Patient's preferences
- Patient's support network
- Patient's barriers and limitations to learning (mental health status, learning difficulties)[14]
Patient behaviour is determined by several factors such as family and work commitments[14] . Patients will often weigh up these factors and consider various options before settling on the choice most suitable to their personality and lifestyle [14].
Learning is defined as a process in which knowledge is created through the transformation of experience [15] [16]. Individuals use learning to manage and adapt to everyday situations, giving rise to different types of learning styles[15] [16]. Through various research and studies, learning styles have been organised and categorized into levels, suggesting an individual’s capacity for flexible and adaptive model learning [15] [16]. These levels are ranked in descending order of stability and are listed as:
For instructional preference. Patterson (2003) [17]proposed three types of learning styles: Visual, Auditory & Kinesthetic. However, Kolb suggested that learning is based on four stages. This commonly used learning theory model explains four stages of experiential model (1984)[18]. The ideology is that individual’s transition from phase to phase in their learning process[15] [16]. However, very little research is available on the application of teaching models to a healthcare setting perspective.
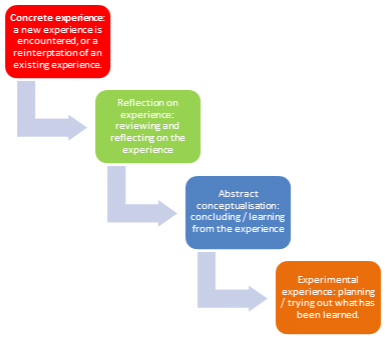
Kolb’s four stages of experiential model:
- Concrete experience: The patient learns of their diagnosis for the first time from the physio or they could have some previous knowledge or experience of the condition, possibly from news articles or friends or family members with experience or knowledge of the condition. This stage helps the patient to grasp what their diagnosis and prognosis is
- Reflection on experience: The patient will go away and review and reflect on the experience and their understanding of their diagnosis.
- Abstract conceptualisation: The patient learns from the experience of their treatment and diagnosis.
- Experimental experience: The patient will plan and adapt to the arising situation and try out what has been learned in terms of education and treatment.
Improving Communication[edit | edit source]
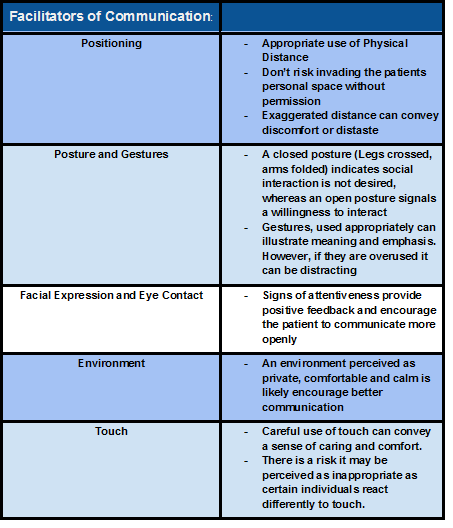
Several key factors need to be considered when looking at ways to improve communication and patient experience[19]. This will help them to relax, speak openly, listen, and most importantly remember what is being said. Together these important factors will empower the client and have a positive impact on health outcomes:
- Positioning
- Posture and Gestures
- Facial Expression and Eye Contact
- Environment
- Touch
Strategies to Aid Information Recall[edit | edit source]
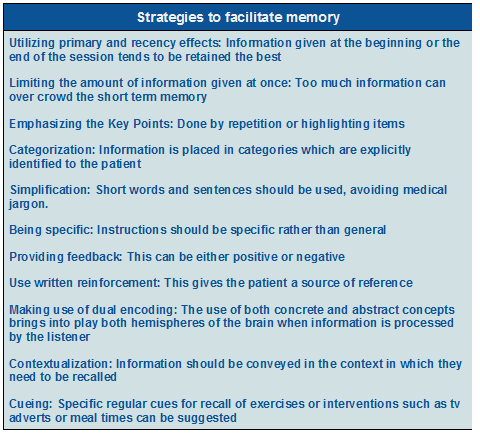
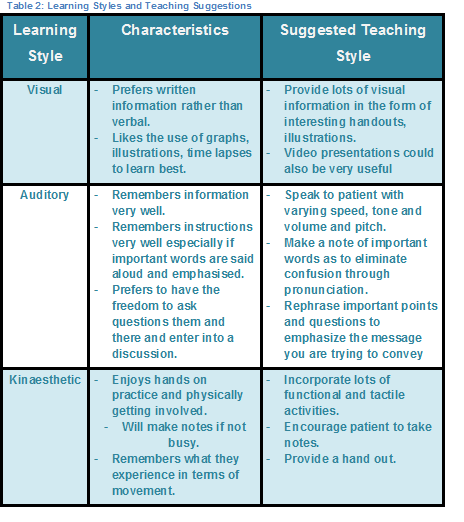
An important feature of effective communication is the ability of the patients to retain the information that is imparted[19]. Extensive research has been conducted within health care on factors which may hinder or facilitate memory and therefore, the degree of adherence. The following table summarizes some techniques which can help maximise the information patients retain and recall. However, it is important to stress that these techniques should not be seen as a substitute for interpersonal skills and attitude that helps to create a good relationship with the patient, as this is a prerequisite for good communication[19].
Explaining Diagnosis[edit | edit source]
The ethos of a physiotherapist defines what good occupational practices should be [20]. General principles cover an evaluation of an adequate attitude i.e. respectable coexistence and behaviour with respect to others, as well as normal social relationships and a positive attitude towards oneself and the surrounding world[20]. A physiotherapist should possess skills of empathetic understanding of patient circumstances and how to respect patients feelings and sensations. Kindness, engagement in the recognition of a patient's individual life situation, as well as his/her personality traits, allow the physiotherapist the ‘maximisation’ of their techniques of providing assistance to a patient[20].
Bad news in the healthcare context can refer to any information that creates a negative view of a person’s health[21]. Communicating bad news can be mishandled with potentially distressing results for clinicians and especially patients. Yet few health care professionals have received formal training in this area and it is evident that many feel ill prepared to perform the task of communicating bad news effectively[21].
Dealing with difficult situations is challenging and requires important communication skills on behalf of the physiotherapist. Besides the moral, ethical and social obligations of conveying this type of information in a sensitive and accurate manner, it can also be medico-legal responsibility[22]. Poorly communicated diagnosis can generate feelings of mistrust, anger, fear and blame[22]. A physiotherapist’s ability to effectively communicate is typically learned through trial and error or observation of more senior staff[22].
Use of Metaphors in Explaining Diagnosis[edit | edit source]
“The medical profession has for a long time largely neglected the influence that language itself has in shaping and conceptualising medical practice”.[23] Why is this? Over the past 3 decades there has been a growing body of evidence that has looked at the role of metaphors in healthcare[23]. Historically metaphors were thought of being misleading and potentially counter productive for cognitive reconceptualising[24]. Contemporary literature is much more welcoming of metaphors, especially within pain management. Now the research debate has shifted toward how metaphors should be applied in clinical practice rather than if metaphors are true or not. [23] [25]We know that each and every patient that is seen comes with a very individual set of life experiences and different ways of shaping understanding of their “impairments". [23] Language and more specifically metaphors can aid in this process to promote advancement of a more meaningful understanding of diagnoses, avoidance of persistent pain, and self management strategies.[23] [26] Despite these potential benefits, physiotherapists need to be aware of the chance of misinterpretations some patients might take from these metaphors.
In clinical practice physiotherapists must keep treatment "patient centered" and address the unique needs of each individual patient.[25] Due to the often complex idiosyncratic nature of bio-psycho-social pain, physiotherapists often use metaphors to try and create an “unique” reconceptualisation of what is really going on with the patients body.[27] If we examine metaphors separate from the healthcare environment we know that metaphors can facilitate new ways of visualising the world and how we act within it. As a child we are always using our imagination or past experiences to create meaning of new experiences we face on a everyday basis. Physiotherapists must aid the patient to find meaning in the dialogue of personal, cultural, and physical experiences that have made up their lives.[28] [25]
Now if we integrate pain for example into this situation we can argue that pain is essentially an interpretation by that individual, it can be said that the only way to adequately understand pain is through metaphor itself.[25] Ideally a set of metaphors that address the neurobiological contexts as well as the sociocultural contexts of their lives without looking at them dualistically but instead cohesively.[23] Over the years the use of metaphors have been looked at by many different research papers and some that are continually being used in practice produce poor patient outcomes. Below are some commonly-used Metaphors in Practice:
- The Body is a Machine
- This often implies that the patients are handing over their bodies to a health professional to locate the damage and administer treatment to repair the damage. Much like a car garage.
- Encourages us to think in a dualistic way (biomedical versus biopsychosocial), although if we recognise that social interaction, self interpretation and meaning are important; we must look for more adequate metaphors.[23]
- Medicine is War/ Military Metaphors[23][25][29]
- Can imply that the patients are being passive and the doctors are warriors.
- Allows patients and clinicians to think that the patient has failed rather than the treatment.
- These metaphors can also lead some clinicians to think of themselves as a poor “soldier” and decrease confidence.
- Military metaphors can direct pain reconceptualisation away from bio-psycho-social evidence and think the war can be won with biomedical means of treatment.
- Brain as a Computer
- This metaphor can sometimes help patients understand some of the complexities of neurobiology, but downplays the idiosyncratic and adaptive properties of the CNS. [25]
- Journey Metaphor
- Some other metaphors paint a more adequate picture for patients and have been successful in practice, especially for patients with consistent pain.
- Contrary to military metaphors, journey metaphors have destinations but in journeys there isn’t just one way to get to that destination. Patients and clinicians have the ability to adjust and try out different avenues. It has been proposed by Reisfield & Wilson [30] that journey metaphors offer “different roads to travel, various avenues to explore and always there are exits to take.”
- Journey metaphors rightfully shift the focus away from failure or success and focus on personalised adaptive exploration .[31]
Advice and Caution[edit | edit source]
As mentioned before there should be certain caution’s and encouraging tips to think about when delivering metaphors in clinical practice. “When Should We Use, and Not Use, Metaphors?” Well that all depends on who is seeking medical help and how the metaphors are going to be used. There isn’t one metaphor that is good or bad, one metaphor might work great with one patient and be harmful or insignificant to another patient.[23] This is when clinicians must open our toolkit and take out their clinical appraisal skills. Therapists must look at “What Patient Has the Condition, Not What Condition Does the Patient Have?” Physiotherapists must be aware of the potential of imposing our own bias on our patients, this is precisely why communication should be looked at in a dialogical manner[23][25].
Through a dialogical approach to assessment we can better understand our patients and through that subjective information co-construct more meaningful metaphors .[23] “Thacker & Mosley have argued that clinician dominant questioning can negate the critical need for the patients to have their psychological, social and philosophical stories heard.” [32]
Its important that we as clinicians understand and appreciate both the power and subtlety that language can possess .[23] The debate shouldn’t be looking at what metaphor is the truest in all senses, this is irrelevant because metaphors aren’t true or false they are useful or not in various contexts.[23]
Conclusion[edit | edit source]
So much of our practice is not just based on our clinical skills but also our ability to communicate and engage our clients. How we communicate can impact the patient and influence their health both physically and psychologicallyReferences[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Street Jr RL, Makoul G, Arora NK, Epstein RM. How does communication heal? Pathways linking clinician–patient communication to health outcomes. Patient education and counseling. 2009 Mar 1;74(3):295-301.
- ↑ Henricson M, Ersson A, Määttä S, Segesten K, Berglund AL. The outcome of tactile touch on stress parameters in intensive care: a randomized controlled trial. Complementary therapies in clinical practice. 2008 Nov 1;14(4):244-54.
- ↑ Knowlton GE, Larkin KT. The influence of voice volume, pitch, and speech rate on progressive relaxation training: application of methods from speech pathology and audiology. Applied psychophysiology and biofeedback. 2006 Jun 1;31(2):173-85.
- ↑ Weze C, Leathard HL, Grange J, Tiplady P, Stevens G. Evaluation of healing by gentle touch in 35 clients with cancer. European journal of oncology nursing. 2004 Mar 1;8(1):40-9.
- ↑ Stewart MA. Effective physician-patient communication and health outcomes: a review. CMAJ: Canadian Medical Association Journal. 1995 May 1;152(9):1423.
- ↑ 6.0 6.1 6.2 Kalet A, Pugnaire MP, Cole-Kelly K, Janicik R, Ferrara E, Schwartz MD, Lipkin Jr M, Lazare A. Teaching communication in clinical clerkships: models from the macy initiative in health communications. Academic Medicine. 2004 Jun 1;79(6):511-20.
- ↑ 7.0 7.1 7.2 7.3 7.4 Ong LM, Visser MR, Lammes FB, De Haes JC. Doctor–patient communication and cancer patients’ quality of life and satisfaction. Patient education and counseling. 2000 Sep 1;41(2):145-56.
- ↑ 8.0 8.1 Gill VT, Maynard DW. Explaining illness: Patients' proposals and physicians' responses. Studies in Interactional Sociolinguistics. 2006;20:115.
- ↑ 9.0 9.1 9.2 Donovan J. Patient education and the consultation: the importance of lay beliefs. Annals of the Rheumatic Diseases. 1991 Jun;50(Suppl 3):418..
- ↑ Sullivan RJ, Menapace LW, White RM. Truth-telling and patient diagnoses. Journal of medical ethics. 2001 Jun 1;27(3):192-7.
- ↑ Weiss BD, Reed RL, Kligman EW. Literacy skills and communication methods of low-income older persons. Patient Education and Counseling. 1995 May 1;25(2):109-19.
- ↑ Schleicher A. Education at a glance 2014. Organisation for economic co-operation and development. 2014. , [accessed on 10 May 2020]
- ↑ Office for National Statistics. 2011 Census: Key Statistics for England and Wales, March 2011. Statistical Bulletin. 2012. [Accessed 10 May 2020]
- ↑ 14.0 14.1 14.2 Strömberg A. The crucial role of patient education in heart failure. European journal of heart failure. 2005 Mar;7(3):363-9.
- ↑ 15.0 15.1 15.2 15.3 15.4 Cassidy* S. Learning styles: An overview of theories, models, and measures. Educational psychology. 2004 Aug 1;24(4):419-44.
- ↑ 16.0 16.1 16.2 16.3 16.4 Hauer P, Straub C, Wolf S. Learning styles of allied health students using Kolb's LSI-IIa. Journal of Allied Health. 2005 Sep 1;34(3):177-82.
- ↑ PATTERSON, D. J. (2003). Learning Styles. Journal of Adventist Education Summer, vol. 39.
- ↑ KOLB, D. A. (1984). Experiential learning: Experience as the source of learning and development (Vol. 1). Englewood Cliffs, NJ: Prentice-Hall.
- ↑ 19.0 19.1 19.2 Pryor JA, Prasad AS. Physiotherapy for respiratory and cardiac problems: adults and paediatrics. Elsevier Health Sciences; 2008 Mar 6.
- ↑ 20.0 20.1 20.2 Standards of Proficiency - Physiotherapists. (2013). Health and Care Professions Council (HCPC).
- ↑ 21.0 21.1 Walsh RA, Girgis A, Sanson-Fisher RW. Breaking bad news 2: What evidence is available to guide clinicians?. Behavioral Medicine. 1998 Jan 1;24(2):61-72.
- ↑ 22.0 22.1 22.2 Colletti L, Gruppen L, Barclay M, Stern D. Teaching students to break bad news. The American journal of surgery. 2001 Jul 1;182(1):20-3.
- ↑ 23.00 23.01 23.02 23.03 23.04 23.05 23.06 23.07 23.08 23.09 23.10 23.11 23.12 Loftus S. Pain and its metaphors: A dialogical approach. Journal of Medical Humanities. 2011 Sep 1;32(3):213-30.
- ↑ Sontag S. Illness as metaphor and AIDS and its metaphors. Macmillan; 2001 Aug 25.
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 25.6 Stewart M. The road to pain reconceptualisation: Do metaphors help or hinder the journey?. Pain and Rehabilitation-the Journal of Physiotherapy Pain Association. 2014 Jan 1;2014(36):24-31.
- ↑ Bedell SE, Graboys TB, Bedell E, Lown B. Words that harm, words that heal. Archives of internal medicine. 2004 Jul 12;164(13):1365-8.
- ↑ Sullivan MD. Pain in language: from sentience to sapience. InPain Forum 1995 Mar 1 (Vol. 4, No. 1, pp. 3-14). Churchill Livingstone.
- ↑ Gifford L. Topical Issues in Pain 2: Biopsychosocial assessment and management Relationships and pain. AuthorHouse; 2013 Sep 9.
- ↑ Louw A, Diener I, Butler DS, Puentedura EJ. The effect of neuroscience education on pain, disability, anxiety, and stress in chronic musculoskeletal pain. Archives of physical medicine and rehabilitation. 2011 Dec 1;92(12):2041-56.
- ↑ Reisfield GM, Wilson GR. Use of metaphor in the discourse on cancer. Journal of clinical oncology. 2004;22(19):4024-7.
- ↑ Hartley T. Cutting edge metaphors. J Assoc Surg GB Irel. 2012 Sep;37:26-9.
- ↑ Yelland, M. (2011). What do patients really want?. International Musculoskeletal Medicine, 33(1), pp.1-2.