Diagnostic Imaging of the Shoulder
Original Editor - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Rucha Gadgil, Admin, Wanda van Niekerk and Lucinda hampton
Introduction[edit | edit source]
Crowell et al [1] suggest that the relationship between musculoskeletal imaging and physiotherapy practice can broadly be divided into three areas:
- imaging as an aid to clinical diagnosis;
- imaging as an aid to injury management rehabilitation and, finally,
- imaging as an aid to treatment accuracy, specifically ultrasound-guided injections.
Diagnostic Imaging can be a useful resource for shoulder conditions and where used appropriately can be an invaluable tool for physiotherapists. Imaging such as MRI, X-ray, CT Scans, and Bone Scans are prime examples of practical diagnostic imaging that facilitates accurate diagnosis, prognosis, intervention, and assessment of injuries and dysfunction that physiotherapists' address daily. Unnecessary imaging will not only potentially squander financial resources, increase the failure rate of conservative physiotherapy and and increase potential for premature surgery, so it is key to understand and recognise when imaging is appropriate.[2] Some researchers have suggested the increase in use of diagnostic imaging including x-ray, diagnostic ultrasound and magnetic resonance imaging (MRI) for shoulder pathology is possibly related to the challenges in classification of shoulder pain and low levels of practitioner confidence in making an accurate clinical diagnosis, specifically a pathoanatomic diagnosis. [3][4][5]
While there are a number of studies which indicate diagnostic imaging is underutilized such as x-rays identifying fractures or bone scans identifying osteoporosis[6], there are also many more studies which suggest over utilization of imaging, such as X-rays or MRI for acute and uncomplicated shoulder pain.[7] While a thorough history and physical examination are the most important instruments in evaluating shoulder pain, musculoskeletal imaging can be an important adjunct.[8]
There may also be an expectation from patients in relation to the needs for imaging studies, many who often demand investigations believing it is necessary for adequate diagnosis and management of shoulder pathology, which can present a multitude of problems for the physiotherapist in managing these expectations and advising or educating patients around the diagnostic imaging and its role.[9] Conservative treatment can be impacted as a result of patient expectations following findings on diagnostic imaging e.g. perception that if a tear is there then physiotherapy has no role to play. Cuff and Littlewood [10] highlight a wide range of factors that influence patient beliefs about the cause of their shoulder pain, but suggest the information they receive from healthcare professionals has the strongest influence, hence, the language and terminology we use is key to achieving good clinical outcomes. Successful physiotherapy management of shoulder pain is often impacted by the patients expectations about how effective they believe physiotherapy to be and has been shown to be the strongest predictor of future surgical intervention in people with shoulder pain and associated rotator cuff tear. [10]
If the patient perceives their problem as one not amenable to physiotherapy following diagnostic imaging, for example an osteophyte (bone spur) impinging on their rotator cuff, the opportunity to achieve a satisfactory outcome might be compromised." [10]
In the evaluation of shoulder pain, the role of diagnostic imaging is to guide clinical management, and can be useful in identifying when operative treatment may be required, and where required can be used further to plan the surgical approach whether it be open or arthroscopic. Currently magnetic resonance imaging (MRI) and ultrasound are the most commonly used cross-sectional imaging modalities in the diagnostic work-up of shoulder pain. [11] Where a thorough and detailed subjective and objective physical assessment has been completed, imaging in some cases may aid in confirming diagnosis, but diagnostic imaging findings can also lead to misdiagnosis if not reviewed in the overall context of the patients symptoms and physical exam findings. As such shoulder examination and development of adequate differential diagnosis is therefore key to establish if advanced imaging is required.
Direct access to physical therapy evaluation and intervention has the potential to reduce costs and improve outcomes in musculoskeletal medicine. The results of multiple studies show that direct access to physical therapy is associated with improved patient outcomes and decreased costs, with minimal risk of harm to the patient.[1][2][3][4][5][6] The diagnostic accuracy of a physical therapists clinical examination has been shown to be the equivalent of orthopedic surgeons and well above non-orthopedic providers when compared to an MRI diagnosis.[3] Direct-access to physical therapy is associated with decreased rates of diagnostic imaging. Additionally, numerous case reports describe the appropriate identification of patients whose pathology lies outside the scope of physical therapy by physical therapists operating in a direct-access setting..[1][6]
Traditionally it was assumed that the utilisation of advanced imaging modalities would provide additional benefits and increase diagnostic accuracy, however as highlighted by Jarvie et al [9] there are many studies which now refute this and suggest the use of additional advanced imaging has minimal impact on the care patients receive. [9] We will review the options and principles of shoulder investigations as they can play a role in the effective management in some shoulder conditions. There are many different types of imaging and each type is used for a specific purpose. For shoulder related problems the main forms of imaging include X-rays (Plain Radiography), Ultrasound, computed tomography (CT) and MRI Scans although direct access to these types of testing vary dramatically worldwide, and even within countries
Imaging Options[edit | edit source]
X-Ray (Pain Radiography)[edit | edit source]
Plain X-rays can be important in the diagnosis of some shoulder conditions, with a good overview provided by routine views which should include a true Antero-Posterior view in the scapular plane (Grashey View) with the arm in maximal internal-rotation, with the arm in External Rotation and Axillary View and Y View (less important). In the context of traumatic injuries or the unstable shoulder, x-rays allow the identification of any dislocations / subluxations and associated fractures, which are more frequent in older patients, such as: tuberosities, surgical or anatomical humeral neck and coracoid and patients should be referred for immediate x-ray if there is any suspicion of these injuries.[12]
The conditions that can be identified on Plain Films include;
- Calcific Teninopathy
- Glenohumeral Joint ARthritis
- Scelrosis of Anterior ad Lateral Acromion
- Sclerosis of the Greater Tuberosity
- Proximal Humeral Head Translation
- Fractures
Indications for X-ray[edit | edit source]
To detect or exclude pathology when diagnosis is obscure and thus contribute to decisions regarding further management. Consider an x-ray and discussion with the patients GP if the patient has; [13]
- Exquisite Pain - Exclude Acute Calcific Tendonitis;
- Subacromial Pain (ONLY if suspect a structural deformity or is unresponsive to treatment);
- History of Trauma - Exclude Fracture and / or Dislocation / Subluxation;
- Possibility of Metastases, particularly in patients with a previous history of Cancer (Breast or Lung)
- AC Joint Pain - Persistent pain with continued functional impairment;
- Older Person with a stiff, painful shoulder +/- crepitus.
"X-ray is currently considered an indicated imaging modality for diagnosing adhesive capsulitis and ruling out an intrinsic cause for motion loss (e.g., glenohumeral arthritis)." [9]
"X-ray studies are also considered indicated for suspected instability to identify concentric reduction and the absence of fracture or bone loss." [9]
Ultrasound[edit | edit source]
Musculoskeletal ultrasound has evolved as a useful and powerful tool for both diagnosis and treatment of shoulder pain, as it provides both static and dynamic visualization of structures surrounding the shoulder including the lateral third of the acromion, the subacromial/subdeltoid bursa, supraspinatus tendon, and the head of the humerus.and their biomechanical relationships.[14] A sensitivity level of 79% and a specificity of 94% was found in a meta-analysis of five studies (311 Shoulders), which used ultrasound to diagnose Rotator Cuff related disorders, so can be considered a valuable investigation for rotator cuff related shoulder pain where indicated. [15] Similarily Henderson et al [16] show that shoulder ultrasound had high diagnostic value for subacromial bursitis, while Ottenheijm et al [17] report a sensitivity and specificity of 79-81 and 94-99%, respectively, when compared to arthroscopy or MRI when detecting bursitis, as do Le Corroller et al [18] who showed a sensitivity and specificity of 96% and 90%, respectively, when compared to MRA. [14]
"High resolution ultrasound, completed by an experienced operator, is a reliable, non-invasive technique for imaging the rotator cuff and adjacent muscles, the bursae, and the long head of biceps muscle." [19]
MRI[edit | edit source]
MRI allows for multiplaner, non-invasive examination of the shoulder. Currently there are many debates surrounding the use of MRI with many studies questioning the clinical relevance of the findings seen on MRI, which have been shown to not always correlate well with surgical findings. [20][21] These studies suggest that the findings on shoulder MRI may not always be clinically relevant. [22] Baudi et al [12] suggest that MRI is considered the gold standard for the evaluation of soft-tissue injuries in the unstable shoulder. MRI can also be used to evaluate bony injuries in detail, as yet it is still unclear whether MRI is more accurate at detecting shoulder related disorders compared with Ultrasound, specifically in relation to Rotator Cuff or Subacromial Related Shoulder Pain, but both have been shown to be equally effective in the detection of partial or full thickness rotator cuff tears [23]. Onward referral to a specialist rather than requesting a MRI may often be a much better management strategy due to the cost implications for shoulder MRI. [24] . Magnetic resonance arthrography (MRA) in particular has shown high sensitivity (86-91%) and high specificity (86- 98%) for the capsulo-ligamentous complex, labral and cartilaginous structures.[12]
Arthrography[edit | edit source]
Arthrography is when the joint is injected with a dye and is generally combined with CT or MR to provide detailed anatomical information of the Shoulder Joint including strong detail of the Capsular Attachments, Labrum and can very clearly highlight small avulsion fractures of the Glenoid Rim (Bankart Lesions) and Humeral Head (Hills-Each Lesion).[19] Magnetic resonance arthrography (MRA) has shown high sensitivity (86-91%) and high specificity (86- 98%) for capsulo-ligamentous complex, labral and cartilaginous structures.[12]
Summary[edit | edit source]
The high prevalence of asymptomatic pathology on imaging complicates the interpretation of imaging with respect to symptoms even when radiological imaging investigations are available. Imaging findings such as tendon tears and bursal thickening, often diagnosed as bursitis, are as common in individuals with no shoulder pain, as they are in those with shoulder pain. One study suggest as much as 96% of individuals without any shoulder pain or loss of function were found to have imaging changes, such as tears, and bursal thickening.[10] This suggests that what can be seen in imaging is not always the cause of the problem, and in many cases imaging findings do not tell you what structure is specifically causing the pain. Cadogan et al [15] suggest that problems associated with the pathoanatomic approach to the clinical diagnosis of shoulder pain often utilised in primary care can lead the practitioner to inaccurate diagnosis, often resulting in inappropriate treatment interventions that may adversely affect patient outcome and result in inappropriate use of healthcare resources, and higher incidences of failed conservative treatment.[15]
Currently in many cases MRI often represents a more universally accepted imaging modality, which may be due to ease of use with the ability for imaging to be evaluated by more than one radiologist. Ultrasound on the other hand, can be slightly more challenging to perform and is operator dependent, requiring a skilled individual.[25]
It is important to consider that diagnostic imaging findings in the acute setting in many cases will not actually change the management of the injury, so knowing and recognising when diagnostic imaging is required is key.[8][22][23] Keeping that in mind, current research suggests that Ultrasound is a valuable for rotator cuff related and subacromial related shoulder pain, in particular complete or incomplete ruptures of the Rotator Cuff, and is more cost effective than use of MRI.[25] MRI on the other hand is indicated when there is question of an abnormality related to the labrum, articular cartilage, bone marrow, or deep soft tissues and is much more accurate when evaluating for Hill-Sachs Lesions or bony Bankart Lesions, while MR Arthrography is far superior when looking for labral capsular ligamentous complex lesions.[25] Ultrasound has some advantages over MRI in particular when imaging around hardware, for detecting foreign bodies, or when there is need to perform a dynamic maneuver to elicit pathology, or for guiding procedures such as injection. Ultrasound is indicated also if the patient has a pacemaker, has a non-MRI-compatible metal implant, or is claustrophobic.[11] When clinical examination findings suggest the need for diagnostic imaging relation to the rotator cuff Levine et al suggests the choice between MRI and ultrasound is influenced by access to imaging, radiologist experience, referring physician preference, MRI contraindications, and patient choice.[11]
Physical therapists operating as musculoskeletal primary care providers in a direct-access sports physical therapy clinic appropriately ordered advanced diagnostic imaging in over 80% of cases. They ordered MRI/MRA in only 8% of all new evaluations, suggesting judicious use of advanced imaging.
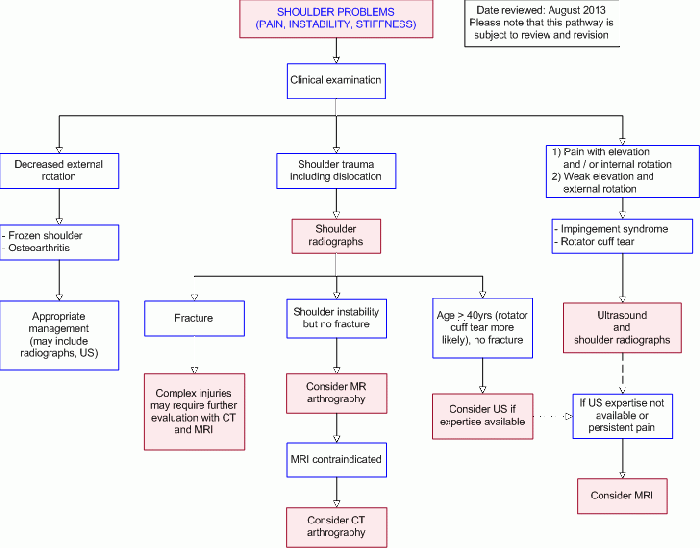
The following pathway provides guidance on the imaging of adult patients with new onset traumatic and non-traumatic shoulder pain or instability.
Resources[edit | edit source]
If you are interested in learning more about diagnostic imaging take a look at these resources for the shoulder
Diagnostic Imaging Pathways - Shoulder (Pain or Instability)[edit | edit source]
The Diagnostic Imaging Pathways website is an evidence-based and consensus-based education and decision support tool for clinicians. It guides the choice of the most appropriate diagnostic examinations in the correct sequence in a wide range of clinical scenarios. Guidance is summarised in flow charts (diagnostic algorithms) and these are supported by appropriate documentation and links to other sources of information and evidence where possible. Each pathway is designed to assist clinicians in situations when faced with a large array of possible diagnostic tests and examinations. However, it is recognised that diagnostic practice may differ from a particular pathway depending on local availability of equipment and expertise, as well as the experience of individual clinicians. Therefore each pathway is neither a rigid set of rules, nor a substitute for clinical assessment, and individual patient circumstances should always be considered.
Norwich Image Interpretation Course: Shoulder[edit | edit source]
The Norwich Image Interpretation Course is aimed primarily at radiographers who provide a preliminary clinical evaluation service to A&E, however it will also benefit those keen to review image interpretation skills. It is anticipated that by reading through each module and referring to the associated images provided, the user will become more accurate in their interpretation skills. You also have an option at the end of each module there is an online self-test which is designed to assess the concepts taught.
They also have a pathology image gallery which can aid with reviewing image interpretation skills when viewing pathologies. These pathologies may arise incidentally when looking at trauma radiographs, or may be encountered when reviewing images from GP or Rheumatology referrers.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Crowell MS, Dedekam EA, Johnson MR, Dembowski SC, Westrick RB, Goss DL. DIAGNOSTIC IMAGING IN A DIRECT-ACCESS SPORTS PHYSICAL THERAPY CLINIC: A 2-YEAR RETROSPECTIVE PRACTICE ANALYSIS. International journal of sports physical therapy. 2016 Oct;11(5):708.
- ↑ 2.0 2.1 Van Tulder MW, Tuut M, Pennick V, Bombardier C, Assendelft WJJ. Quality of primary care guidelines for acute low back pain. Spine. 2004;29(17):E357-62. Available at: http://www.ncbi.nlm.nih.gov/pubmed/15534397.
- ↑ 3.0 3.1 3.2 Cadogan A, McNair PJ, Laslett M, Hing WA. Diagnostic Accuracy of Clinical Examination and Imaging Findings for Identifying Subacromial Pain. PloS one. 2016 Dec 9;11(12):e0167738.
- ↑ 4.0 4.1 Awerbuch MS. The clinical utility of ultrasonography for rotator cuff disease, shoulder impingement syndrome and subacromial bursitis. Med J Aust. 2008;188(1):50–3. pmid:18205566
- ↑ 5.0 5.1 Johal P, Martin D, Broadhurst N, Johal P, Martin D, Broadhurst N. Managing shoulder pain in general practice—assessment, imaging and referral. Aust Fam Physician. 2008;37(4):263–5. pmid:18398526
- ↑ 6.0 6.1 6.2 Freeborn DK, Shye D, Muttooty JP, Eraker S, Romeo J. Primary Care Physicians ’ Use of Lumbar Spine. Journal of General Internal Medicine.3-9.
- ↑ Carey TS, Garrett J, Back C, Project P. Patterns of Ordering Diagnostic Tests for Patients with Acute Low Back Pain. Medicine. 1996.
- ↑ 8.0 8.1 McMahon KL, Cowin G, Galloway G. Magnetic resonance imaging: the underlying principles. The Journal of orthopaedic and sports physical therapy. 2011;41(11):806-19. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21654095. Accessed March 16, 2012.
- ↑ 9.0 9.1 9.2 9.3 9.4 Jarvie GC, Pike JM, Goel DP. Diagnoses and imaging utilization for common shoulder disorders by referring physicians in British Columbia. How would you like to die?. 2017 May:222.
- ↑ 10.0 10.1 10.2 10.3 Cuff A, Littlewood C. Subacromial Impingement Syndrome - What does this mean to and for the Patient? A Qualitative Study. Musculoskeletal Science and Practice. Elsevier Ltd; 2017 Oct 17;:1–14.
- ↑ 11.0 11.1 11.2 Levine BD, Motamedi K, Seeger LL. Imaging of the shoulder: a comparison of MRI and ultrasound. Current sports medicine reports. 2012 Sep 1;11(5):239-43.
- ↑ 12.0 12.1 12.2 12.3 Baudi P, Rebuzzi M, Matino G, Catani F. Imaging of the Unstable Shoulder. Open Orthopaedics J. 2017 Aug 31;11(Suppl-6, M7):882–96.
- ↑ Bussières AE, Peterson C, Taylor JA. Diagnostic imaging guideline for musculoskeletal complaints in adults—an evidence-based approach—part 2: upper extremity disorders. Journal of manipulative and physiological therapeutics. 2008 Jan 31;31(1):2-32.
- ↑ 14.0 14.1 Saulle M, Gellhorn AC. Approach to the diagnosis of shoulder pain using physical exam and ultrasound: an evidence-based approach. Current Physical Medicine and Rehabilitation Reports; 2017 Mar 30;:1–11.
- ↑ 15.0 15.1 15.2 Roy, J. S., Brae ̈n, C., Leblond, J., Desmeules, F., Dionne, C. E., MacDermid, J. C., ... Fre ́mont, P. (2015). Diagnostic accuracy of ultrasonography, MRI and MR arthrography in the characterisation of rotator cuff disorders: A systematic review and meta-analysis. British Journal of Sports Medicine, 49(20), 1316–1328. doi: 10.1136/bjsports-2014- 094148
- ↑ Henderson RE, Walker BF, Young KJ. The accuracy of diagnostic ultrasound imaging for musculoskeletal soft tissue pathology of the extremities: a comprehensive review of the literature. Chiropr Man Therap. 2015;23:31.
- ↑ Ottenheijm RP, Jansen M, Staal JB, van den Bruel A, Weijers RE, de Bie RA, et al. Accuracy of diagnostic ultrasound in patients with suspected subacromial disorders: a systematic review and meta- analysis. Arch Phys Med Rehabil. 2010;91(10):1616–25
- ↑ Le Corroller T, Cohen M, Aswad R, Pauly V, Champsaur P. Sonography of the painful shoulder: role of the operator’s experi- ence. Skelet Radiol. 2008;37(11):979–86.
- ↑ 19.0 19.1 Brukner P. Brukner & Khan's clinical sports medicine. North Ryde: McGraw-Hill; 2012.
- ↑ Wnorowski DC, Levinsohn EM, Chamberlain BC, McAndrew DL. Magnetic resonance imaging assessment of the rotator cuff. Is it really accurate? Arthroscopy 1997;13:710-9.
- ↑ Tortensen ET, Hollinshead RM. Comparison of magnetic reso- nance imaging and arthroscopy in the evaluation of shoulder pathology. J Shoulder Elbow Surg 1999;8:42-5.
- ↑ 22.0 22.1 Bradley MP, Tung G, Green A. Overutilization of shoulder magnetic resonance imaging as a diagnostic screening tool in patients with chronic shoulder pain. Journal of shoulder and elbow surgery. 2005 Jun 30;14(3):233-7.
- ↑ 23.0 23.1 Gazzola, S., & Bleakney, R. R. (2011). Current imaging of the rotator cuff. Sports Medicine and Arthroscopy Review, 19(3), 300–309. doi: 10.1097/JSA.0b013e3182189468
- ↑ Leung R. Common Sports-related Shoulder Injuries. InnovAiT. 2017 Jan;10(1):30-8.
- ↑ 25.0 25.1 25.2 Pavic R, Margetic P, Bensic M, Brnadic RL. Diagnostic Value of US, MR and MR Arthrography in Shoulder Instability. Injury. 2013 Sep 30;44:S26-32.