Duchenne Muscular Dystrophy
Original Editor - Rachael Lowe
Top Contributors - Pacifique Dusabeyezu, Alyssa Aquino, Rachael Lowe, Kim Jackson, Nikhil Benhur Abburi, Rucha Gadgil, Admin, Shaimaa Eldib, Laura Ritchie, Faye Underwood, WikiSysop, Vidya Acharya, Lucinda hampton, Audrey Brown, 127.0.0.1, Evan Thomas, Naomi O'Reilly and Michelle Lee
Introduction[edit | edit source]
Duchenne muscular dystrophy (DMD) is a progressive genetic condition which affects the muscles, causing muscle weakness. It is a serious condition which starts in early childhood. The muscle weakness is not noticeable at birth, even though the child is born with the gene which causes it. The muscle weakness develops gradually, usually becomes evident between the age of three and five years and functional level is maintained between three and six years in these children. Symptoms are mild at first but become more severe as the child gets older.
Duchenne muscular dystrophy, the most common type, is one of more than 20 muscular dystrophies. The incidence of DMD globally is every 1/3500 male births[1] That means that there is approximately 2400 individuals living with DMD in the UK alone[2].
| Type | Prevalence | Common Symptoms |
|---|---|---|
| Duchenne Muscular Dystrophy | 1 in 3,500 | • Difficulty walking, running or jumping
• Difficulty standing up • Learn to speak later than usual • Unable to climb stairs without support • Can have behavioural or learning disabilities |
| Facioscapulohumeral Muscular Dystrophy | 1 in 7,500 | • Sleeping with eyes slightly open
• Cannot squeeze eyes shut tightly • Cannot purse their lips |
| Myotonic Dystrophy | 1 in 8000 | • Muscle stiffness
• Clouding of the lens in the eye • Excessive sleeping or tiredness • Swallowing difficulties • Behavioural and learning disabilities • Slow and irregular heartbeat |
| Becker Muscular Dystrophy | Varies;
1 in 18,000 – 1 in 31, 000 |
• Learn to walk later
• Experience muscle cramps when exercising |
| Limb-Girdle Muscular Dystrophy | Estimated to be in a range of 1 in 14,500 – 1 in 123,000 | • Muscle weakness in hips, thighs, and arms
• Loss of muscle mass in these same areas • Back pain • Heart palpitations / irregular heartbeats |
| Oculopharyngeal Muscular Dystrophy | 1-9 in 100,000 | • Does not usually appear until age 50-60
• Dropped eyelids • Trouble swallowing • Gradual restriction of eye movement • Limb weakness, especially around shoulders and hips |
| Emery-Dreifuss Muscular Dystrophy | 1 in 100,000 | • Develop symptoms in childhood and adolescence
• Muscle weakness • Trouble on stairs • Tendency to trip • Slow, irregular heartbeat |
All types of muscular dystrophies are caused by faults in genes (the units of inheritance that parents pass on to their children) which result in progressive muscle weakness due to muscle cells breaking down and gradually becoming lost. The Duchenne type dystrophy is an X-linked genetic disorder affecting primarily boys (with extremely rare exceptions, For example: Females with Turner's syndrome) and a problem in this gene results in a defect in a single important protein in muscle fibers called dystrophin. It is named after Dr. Duchenne de Boulogne, who worked in Paris in the mid-19th century, who was one of the first people to study the muscular dystrophies.
The females are typically the carriers(those with a DMD mutation on one X chromosome) for the disease and they are usually asymptomatic but, in rare cases, resemble Becker muscular dystrophy (BMD).[9] However, 2-20% of carriers have clinically evident muscle weakness and weakness is usually mild to moderate, and asymmetric. Some carriers report myalgia or cramps without weakness.[10][11] The son of carrier mother has a 50% chance of inheriting the defective gene from his mother while the daughter of carrier mother has also a 50% chance of being a carrier or having two normal copies of the gene.
Clinically relevant anatomy[edit | edit source]
Dystrophin is responsible for connecting the cytoskeleton of each muscle fiber to the underlying basal lamina. The absence of dystrophin stops calcium entering the cell membrane, which affects the signalling of the cell. Water then enters the mitochondria, causing the cell the burst. In a complex cascading process that involves several pathways, increased oxidative stress within the cell damages the sarcolemma resulting in the death of the cell. Muscle fibers undergo necrosis and are replaced with connective tissue.
Small amounts of dystrophin are also made in nerve cells (neurons) in specific parts of the brain, including the hippocampus. The hippocampus is the part of the brain involved in learning and memory, as well as emotions. The non-progressive memory and learning problems, as well as social-behavioural problems in some people with DMD, are most likely linked to loss of dystrophin in the neurons of the hippocampus and other parts of the brain where dystrophin is normally produced in small amounts. However, studies are being carried out to find out why only a small number of individuals with DMD are affected by this.[12]
Mechanism of Injury / Pathological Process[edit | edit source]
The cause of DMD is a mutation in the gene that encodes the 427-kDa cytoskeletal protein dystrophin, which affects the muscles. People with DMD have a shortage of dystrophin in their muscles. The lack of dystrophin leads to muscle fiber damage and a gradual weakening of the muscles.
Clinical Presentation[edit | edit source]
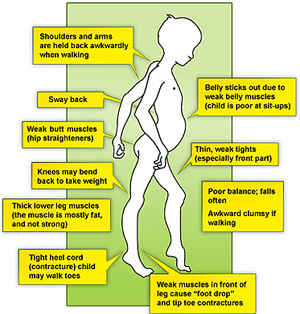
The muscle weakness is mainly in the 'proximal' muscles, which are those near the trunk of the body and around the hips and the shoulders. Weakness typically starts proximally in the lower extremities, then moves distally. Weakness in the upper extremities tends to appear later[1]. This means that fine movements, such as those using the hands and fingers, are less affected than movements like walking.
The symptoms usually start around age 1-3 years, and may include:
- Difficulty with walking, running, jumping and climbing stairs. Walking may look different with a 'waddling' type of walk. The boy may be late in starting to walk (although many children without DMD also walk late).
- When you pick the child up, you may feel as if he 'slips through your hands', due to the looseness of the muscles around the shoulder(Proximal shoulder girdle muscle weakness). This is called "Meryon's sign".
- Toe-walking, In this gait pattern, children walk on their toes with feet apart to help maintain balance, with an increased curve in the lower back.
- Frequent falls between the ages of 3 and 5 years.[13]
- The calf muscles may look bulky, although they are not strong.This is called Pseudohypertrophy of calf muscles.
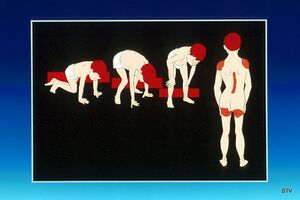
- As he gets older, the child may use his hands to push on the thighs to achieve standing position, looking as if he is 'climbing up his legs'. This is called Gower maneuver or "Gower's sign".This is maneuver indicates weekness of the thigh muscles.[13]
- Some boys with DMD also have a learning difficulty. Usually, this is not severe.
- Sometimes, a delay in development may be the first sign of DMD. The child's speech development may also be delayed. Therefore, a boy whose development is delayed may be offered a screening test for DMD. However, DMD is only one of the possible causes of developmental delay and there are many other causes not related to DMD.
- Contractures are a classic finding in DMD[14]. It develops when muscle fibers, which are normally stretchy, are replaced by hardened, non-stretchy tissue[14]. Contractures are seen as a major cause of disability as they prevent normal movement.[15] For children with DMD, contractures occur often in the legs, especially the calf and muscles around the hip.
- Progressive enlargement of heart
- Some boys with DMD develops lumbar lordosis. This is due to muscle imbalance
| [16] | [17] |
Diagnostic Procedures[edit | edit source]
Initial diagnosis in families without genetic history typically occurs around five years of age, although it may be suspected because of the child's symptoms (above) as they are often seen earlier. When looking for signs of DMD, it is important to watch the child running and getting up from the floor as muscle weakness is more noticeable during these activities.
Gower’s Sign is a very common physical finding in individuals with Duchenne’s[18]. It involves using their hands to ‘climb’ up their legs in order to stand up[18]. It is due to a weakness in the child’s hip muscles[18].
Tests are needed before DMD can be diagnosed. The first step in making the diagnosis is a blood test which tests for creatine kinase. Children with DMD have a very high level of creatine kinase (about 10-100 times normal). Therefore, if a child's creatine kinase level is normal, DMD can be ruled out. If the creatine kinase level is high, further tests are needed to see whether it is due to DMD or to some other condition.
The next step in diagnosing DMD involves either a muscle biopsy and/or genetic tests:
- A muscle biopsy involves taking a small sample of a muscle under local anaesthetic. The sample is examined under a microscope using special techniques to look at the muscle fibers and dystrophin protein.This is only if genetic testing is not able to accurately provide the diagnosis.
- Genetic tests are done using a blood sample. The DNA in the blood is tested to look at the dystrophin gene. This test can diagnose most cases of DMD.
Muscle MRI is usually not performed in DMD for diagnosis, but may be a useful noninvasive tool to evaluate progression of muscle involvement over time. Abnormalities in signal are seen on T1 and T2 images, with initial selective involvement of the gluteus maximus, adductor magnus, quadriceps, biceps femoris, rectus femoris and gastrocnemius muscles.[19]
Prognosis[edit | edit source]
Unfortunately there's no cure for Duchenne muscular dystrophy the aim of treatment is to control symptoms and improve the quality of life. Most patients become wheelchair dependent around 10–12 years of age and need assisted ventilation at around 20 years of age. With optimal care, most patients with DMD die between 20 and 40 years of age from cardiorespiratory complications[20][21]
Duchenne muscular dystrophy (DMD) is a progressive, disabling and life-limiting disorder that will affect the lives of patients and their families. Some quality of life studies(QOL) in patients with DMD have reported a reduced QOL whereas others have found no differences compared with healthy individuals[22]
According to PPMD(Parental Project Muscular Dystrophy), the advanced therapy now permits patients with DMD to attain their adulthood for 30 years.
Outcome Measures[edit | edit source]
Outcome measures for an individual with DMD vary according to the progression of the disease.
Outcome measures to quantify disease progression include:
- 6‐minute walking test
- North Star ambulatory assessment scale,
- Time taken to climb four steps
- Vignos functional rating scale[23]
- Time taken to rise from the floor
- Performance of upper limb.
One of the limitations of the above measures is that they target either ambulant or non‐ambulant patients[24]. However, as the disease progresses, the outcome measures change, making it difficult to use a single outcome measure to analyze the patient. Studies are being carried out to create a uniform measure for muscular dystrophy conditions.
(see Outcome Measures Database)
Management / Interventions[edit | edit source]
Multidisciplinary management of symptoms is currently the standard of treatment for DMD, with interventions primarily focused on delaying disease progression with approaches that focuses on anticipatory and preventive measures as well as active interventions to address the primary and secondary aspects of the disorder. Initially, around the time of diagnosis, genetic counseling and psycho-social support for the boy and family members are important,The family can do many things to help the child live more fully and happily. The goal of the family is to help the child be as active and happy as possible,and to adjust his increasing limitations.[25]
Medical Management[edit | edit source]
As there is no cure for Duchenne muscular dystrophy, there are ways to help improve the individual’s quality of life and provide help for the stage they are in.
Mobility aids will be given to help the child be as independent as possible. These can include a walker in the beginning phases and can progress to a motorized wheelchair. In-home hoists are useful for the carers when they need help to transfer the child. Standing frames also become useful when the child can no longer stand on their own. This helps the child gain the benefits of standing, such as increased bone density, and stretching the muscles even if the child cannot stand on their own. Knee-ankle-foot orthosis (KAFOs) may be used as well. KAFOs have been found to prolong the child’s independent mobility[26]. These should be used alongside mobility aids, such as a zimmer frame. Staying as active as possible is recommended as bedrest can make the muscle-weakening worse[27].
Steroids are commonly prescribed for children with DMD and are the only palliative treatment.[28]. Steroids have been shown to increase the child’s muscle strength and functional ability[29]. Steroids may help delay the child from becoming wheelchair dependent, however, there may be side effects[29]. Another group of medications that have been shown to be helpful are Beta-Blockers[30]. Heart and respiratory function slowly decline in these children and these drugs are used to help manage both these problems[31].
Some families may consider surgery for their child. Common surgeries for children with DMD include foot surgery, insertion of a feeding tube, and spinal surgeries to correct scoliosis, which may occur from being wheelchair dependent. There are many facts to consider before surgery, such as the effect general anaesthesia has on the cardiac and respiratory systems, which are already compromised in children with DMD[32]. Families need to weigh the advantages of the surgery with the risk before making a decision. For example, evidence has been found that surgery to correct scoliosis has improved respiratory function[33], and it also improves the cosmetic appearance and comfort of the child. [34]
Controlling and managing symptoms as multidisciplinary team and access to non-invasive ventilation increases chances of survival into adulthood. For optimal management, a multidisciplinary care team who may be involved in the care include Neurologist, Cardiologist, Orthopedist, Pulmonologist, Medical Geneticist, Physical therapist, and Occupational therapist.[35][36][37] Males with DMD, with proper management and intervention, can now be expected to live into their 30's and 40's.
Preschool Age[edit | edit source]
Usually, at this stage, the child will be well and not need much treatment. Management entails:
- Provided information about DMD and patient support groups.
- Referral to a specialist team (for example, a paediatrician or neurologist, physiotherapist, and a specialist nurse) to monitor child health.
- Advice about the right level of exercise.
- Genetic advice for the family.
Management in Age 5-8 Years[edit | edit source]
Between the ages of 6-11, there is a steady decline in muscle strength and by the age of 12, most children are wheelchair bound[38]. There are further complications surrounding children being dependent on wheelchairs, such as scoliosis and respiratory problems[39].Thus monitoring spinal alignment and giving these boys manual wheelchair as walking becomes difficult may be helpful in preventing deformity and preserving independent mobility.[40] Some support may be needed for the legs and ankles through night-time ankle splints or with knee-ankle-foot orthoses. There is no evidence of significant benefit from any intervention for increasing ankle range of motion[41].
Treatment with corticosteroids can help to maintain the child's muscle strength in boys with DMD when their motor development stops or starts to decline. This involves taking medication such as prednisolone or deflazacort as a long-term treatment, either continuously or in repeated courses.[42]
Management in 8 Years-Late Teenage Years[edit | edit source]
At some time after the age of 8 years, the child's leg muscles become significantly weaker. Walking gradually gets more difficult, and a wheelchair is needed. The age at which this happens varies from person to person, but it is often around age 9-11 years.
With corticosteroid treatment, some patients with DMD can walk for longer. An RCT[43] in Duchenne muscular dystrophy children aged 6 to 10 years suggests that bicycle ergometer and treadmill training along with physical therapy treatment program significantly improves functional walking capacity (6-minute walk test) and balance (measured on Biodex Stability System). The physical therapy treatment program included gentle stretching, isometric muscle contraction (of quadriceps, hamstrings, anterior tibial group, calf muscles, biceps, triceps muscles), gait and balance exercise training. Besides, the results of the study found treadmill training effectively improved walking capacity and balance over bicycle ergometer in Duchenne muscular dystrophy children.[43]
Complications tend to begin once the child becomes wheelchair dependent, so it is important to monitor the child's health and to treat any complications early. Practical support and equipment will be needed at this stage, through wheelchairs and adaptations to the child's home and school. Counseling and emotional support for the child and family may also be helpful.
Management in Late Teenage Years-Twenties[edit | edit source]
At this stage, muscle weakness becomes more problematic. Increasing help and household and community adaptations are needed. Complications such as chest infections are likely to increase, so more medical monitoring and treatment are required.
Physiotherapy Management[edit | edit source]
Physiotherapy is essential to the management of Duchenne muscular dystrophy. Physiotherapists work with the parents and provide them with information and manual skills that will be helpful for the child. It is important to identify the following impairments, activity limitations, or participation restrictions to be addressed by physical therapy in:
- Impaired strength and range of motion
- Decreased functional mobility, transfers and gait.
- Limitation in functional abilities
- Impaired respiratory function
- Apparent or potential spinal deformities
- Emotional trauma of the individual and the family (The most important thing as physical therapist is to provide education and support for the family while managing the child's impairments).
- Need for adaptive equipment.
The physical therapy goals are to prolong function by maintaining capacity of the child for activities of daily living (ADL) and to involve the child in play, to prevent deformity, to control discomfort and to assist in supporting the family.[13]
Range of motion[edit | edit source]
There is high chances of developing muscle contractures in children's with DMD and every effort should be made to maintain range of motion at all joints. Contractures are one of the major side effects that is addressed through a stretching exercises routine. It can also be taught to the parents[44].Special attention should be given specifically to gastrocnemius-soleus complex and the tensor fasciae latae because tightness in these muscles results in gait deviations and widened base of support.[13]
Physiotherapists advise parents on the need for orthoses, such as AFOs or KAFOs, and refer them to a pediatrics orthotist[45]. They will also help families choose what mobility aids and equipment the child might need.
Respiratory function[edit | edit source]
Respiratory function should be targeted for aggressive management in patients with DMD. Breathing exercises and range of motion should be part of home exercise program. Flexion of the arms or legs should be paired with inspiration, whereas extension can be linked with expiration. Diaphragmatic breathing is more efficient than use of accessory muscles and therefore should be emphasized along with lateral basal expansion.[13] In the early stages of the condition, the physiotherapist will be involved in helping keep the child active. During later stages of the condition, respiratory issues are addressed[45].
Muscle weakness[edit | edit source]
Due to the wasting of the muscle caused by the lack of dystrophin and proximal muscle weakness(most clearly apparent in shoulder and pelvic girdle) in DMD patients, they struggle with many everyday activities. Physiotherapists can help with the management of presenting neuro-musculoskeletal problems. They can help slow the regression of range of motion, muscle strength, and daily function, and work to improve gait pattern and posture/alignment [46]. Physiotherapy can also address the pain that the patient may be experiencing. As the patient's walking and standing abilities decline, the physiotherapist may choose to implement a standing program [47].
Physiotherapists will monitor the child’s posture in sitting, lying and standing[48]. They can inform the parents of ways to help the child sit, stand, and lie in optimal positions using pillows or splints. A sleep system and night splints may be recommended for nighttime to help maintain the child’s posture over a long period of time[45].
Many physiotherapists use the NorthStar Ambulatory Assessment in order to objectively monitor the child’s progression. Initiated in 2003, it is a tool designed specifically for children with DMD and has the child perform up to 17 activities, including standing, head-raising, hopping, and running[49]. This assessment is used only for children who are still able to walk. It is standardized with each child given the same instructions and their ability to complete a task given a score of 0-2[50]. It is easy to administer and can be completed in approximately 10 minutes[49]. These are useful when consulting with other medical practitioners and for assessing the child's physical condition.
Pharmacology[edit | edit source]
In the ambulant stage, chronic corticosteroid treatment is an accepted practice. Glucocorticoid, a type of corticosteroid, is a standard of care among DMD patients. The use of steroids has been shown to help improve muscle strength and function, delay the loss of ambulation, and help maintain cardiac and respiratory function. Due to the fact that it helps with muscle strength, cortical steroids also reduce the risk of scoliosis.[51]
Treatment plans may vary, with some patients taking steroids every day or every other day. Different dosages may also be taken.
As with all medications, there are side effects which should be taken under consideration when treating the patient. Examples of known side effects are:
- Cushingoid features
- Weight gain and growth inhibition
- Impaired fat and glucose metabolism
- Fluid retention and hypertension
- Osteoporosis with increased risk of vertebral fractures
- Cataracts[51]
Respiratory Care[edit | edit source]
Respiratory function should be routinely checked in DMD patients. This allows physicians to monitor who may need help with assisted coughing and ventilation in the future. Evaluation of respiratory functions include:
- Spirometric measurements of FVC, FEV, and maximal mid-expiratory flow rate
- Maximum inspiratory and expiratory pressure
- Peak cough flow
Carbon dioxide levels should also be monitored[52]
Airway clearance is of importance to prevent atelectasis and pneumonia. A variety of manual techniques can be used in clinical practice to help clear the patient's airways. Manually assisted coughing techniques are especially useful in patients who have a low cough peak flow rate (below 160 L/min) because self-clearance of their airways are not adequate. Expiratory force can also be increased by applying pressure to the patient's upper abdomen during their natural cough. Other manual techniques include air stacking, glossopharyngeal breathing, and positive pressure application [52].
Along with manual techniques, mechanical techniques and mucus mobilization devices may also prove useful[52].
Complications[edit | edit source]
Anaesthetics[edit | edit source]
People with DMD need extra care if they have a general anaesthetic. Certain anaesthetic medicines can cause harmful reactions for people who have DMD. Also, extra care for the chest and breathing is needed. It is important to have a pre-operative assessment and a senior anaesthetist providing anaesthetic care.
Patients with DMD are thought to have increased risk of malignant hyperthermia, or at least malignant hyperthermia-like reactions if exposed to inhalational anesthetics such as halothane, or succinylcholine.[53][54]
Osteoporosis[edit | edit source]
People with DMD may develop osteoporosis due to a lack of mobility and steroid treatment. Loss of bone mineral density begins even when boys are still ambulant[55][56]and continues to diminish with age.It is important to prevent osteoporosis for as long as possible. A good intake of vitamin D and calcium can help. Sometimes a blood test to check vitamin D levels is advised, and vitamin D supplements may be offered.
Joint and Spinal Complications[edit | edit source]
Muscle weakness can result in joint contractures. In DMD, it is often the ankle joint and Achilles' tendon which become tight. This can be treated either using orthotic devices or by surgical release of the tendon.
Scoliosis develops in almost all children with DMD, and impacts on respiratory vital capacity and mainly occurs due to muscle weakness.[57] Usually this happens at the beginning of the second decade of life, after the patient has lost ambulation[52]. Scoliosis can cause discomfort and is detrimental for posture and breathing. A spinal brace or spinal surgery are the recommended interventions. Surgery has been shown to improve function and quality of life[58]. Surgery should be done while the patient still has sufficient lung function and before cardiomyopathy becomes a major risk factor when putting the patient under anaesthesia[52]
Nutrition and Digestion[edit | edit source]
Some children with DMD are prone to being overweight, especially if taking steroid treatment. Teenagers and adults with DMD may also be underweight, due to loss of muscle bulk. Dietary advice can be helpful in these situations.
Constipation(hard, difficult stool) can be a symptom for anyone who is not mobile. This can be treated with laxatives,drinking a lots of liquids, eating fruits and vegetables and a high fiber diet.[35]
In the later stages of DMD (as a young adult and older), people with DMD may have pharyngeal weakness that leads to dysphagia and difficulty with chewing. These individuals need a careful assessment and nutritional advice or supplements. If the problem is severe, then a gastrostomy may be needed. [59]
Chest and Breathing Complications[edit | edit source]
During the teenage years, the breathing muscles weaken, causing shallow breathing and a less effective cough mechanism which can lead to chest infections. All individuals with DMD will present with restrictive lung disease[1]. Clearance techniques and non-invasive ventilation may help.
As the breathing muscles get weaker, oxygen levels in the blood may be reduced. Reduced oxygen levels are reduced even more so while sleeping. Because this develops gradually, the symptoms may not be obvious. Possible symptoms of low oxygen are tiredness, irritability, morning headaches, night time waking, and vivid dreams.
Vital capacity will increase as in a normal individual until the age of ten. After the age of ten, an individual's vital capacity will decrease by approximately 8-12% each year[1].
It is helpful if breathing problems are detected and treated early. Patients with DMD will usually be offered regular lung function tests once they start to have significant muscle weakness.
Cardiac (Heart) Complications[edit | edit source]
Teenagers and adults with DMD may develop cardiomyopathy. Cardiomyopathy generally develops around the age of 10 and by the age of 18 all individuals with DMD will present with cardiomyopathy [1]. In dilated cardiomyopathy, it becomes difficult for the heart to pump blood to the body because the chambers have become enlarged and the heart wall has thinned [1].
With DMD, cardiomyopathy does not usually cause much in the way of symptoms. Possible symptoms are tiredness, leg swelling, shortness of breath, or an irregular heartbeat. Cardiomyopathy can be helped by medication, which seems to work best if started at an early stage before symptoms are noticeable. So people with DMD are usually offered regular heart check-ups involving an ECG, starting from early childhood.
Intellectual disability[edit | edit source]
Intellectual disability is seen in 30% of boys with DMD, with the average intelligence quotient (IQ) being 85, normally distributed one standard deviation below the population norms.[60] [61][62]Verbal IQ is more impaired than performance IQ.[63][64]Intellectual disability is not correlated with the severity of weakness.Boys with DMD also have a higher incidence of attention deficit hyperactivity disorder (ADHD).It was found that the risk of ADHD was higher in carriers of mutations in brain-expressed dystrophin isoforms expressed in the brain and are known to be associated with higher risk of cognitive impairment.[65]
Differential Diagnosis[edit | edit source]
Differential diagnosis for DMD involves other types of muscular dystrophy—particularly Becker's Muscular dystrophy, which is similar but progresses more slowly. The age of onset is usually later and clinical involvement more mild. Muscle biopsy can be used as a standard for differentiating Becker's and Duchene's dystrophy.
In other myopathies, Creatinine Kinase levels are usually lower than those in DMD. Identification of deletion or mutation of relevant genes with DNA analysis confirms the diagnosis.
Polymyositis- Diagnosis is established by characteristic muscle biopsy findings of inflammation, including mono nuclear invasion of non-necrotic muscle, CD8+ cytotoxic/suppressor T cells, macrophages, and absence of peri-fascicular atrophy of dermatomyositis. Usually, polymyositis affects proximal and limb-girdle muscles.
Neurological causes of muscle weakness - eg, spinal cord lesions, spinal muscular atrophies, motor neurone disease, multiple sclerosis. These conditions are likely to have additional features, such as sensory loss, upper motor neuron lesion signs, or muscle fasciculation.
Increased transaminases (aspartate aminotransferase and alanine aminotransferase, which are produced by muscle as well as liver cells). The diagnosis of DMD should thus be considered before liver biopsy in any male child with increased transaminases[66].
Resources[edit | edit source]
- Diagnosis and management of Duchenne muscular dystrophy, part 1: diagnosis, and pharmacological and psychosocial management
- Diagnosis and management of Duchenne muscular dystrophy, part 2: implementation of multidisciplinary care
- Case Study
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Yiu E, Kornberg A. Duchenne Muscular Dystrophy. Neurology India 2008;56(3):236-247.
- ↑ Muscular Dystrophy UK. Muscular Dystrophy UK Fighting Muscle-wasting Conditions. http://www.musculardystrophyuk.org/about-muscle-wasting-conditions/?gclid=CjwKEAjwpYeqBRDOwq2DrLCB-UcSJAASIYLjj2w3LQ3hI43XFhdWOw7wXT-6OFurebTSskU9ckZCdhoCZwfw_wcB (Accessed 28 April 2009)
- ↑ Tecklin, J.S., 2006. Pediatric physical therapy / [editied by] Jan S. Tecklin. Philadelphia : Lippincott Williams and Wilkins, 2008; 4th ed.
- ↑ Centers for disease control and prevention., 2014. Facts About Muscular Dystrophy [online]. [viewed 2 October 2014]. Available from: http://www.cdc.gov/ncbddd/musculardystrophy/facts.html
- ↑ Orphanet., 2007. Duchenne and Becker Muscular Dystrophy [online]. [viewed 6 October 2014]. Available from: http://www.orpha.net/consor/cgi-bin/OC_Exp.php?Lng=EN&Expert=262
- ↑ FSH society: Facioscapulojumeral muscular dystrophy., 2010. About FSHD [online]. [viewed 5 October 2014]. Available from: https://www.fshsociety.org
- ↑ NHS., 2013. Muscular Dystrophy – Types [online]. [viewed 3 October 2014]. Available from: http://www.nhs.uk/Conditions/Muscular-dystrophy/Pages/Symptoms.aspx
- ↑ Suominen, T., Bachinski, L., Auvinen, S., Hackman, P., Baggerly, K., Angelini, C., Peltonen, L., Krahe, R. and Udd, B., July 2011. Population frquency of myotonic dystrophy: higher than expected frequency of myotonic dystrophy type 2 (DM2) mutation in Finland.vol. 19, no. 7 pp. 776-82 Available from: http://www.ncbi.nlm.nih.gov/pubmed/21364698
- ↑ Duan D, Goemans N, Takeda S, Mercuri E, Aartsma-Rus A. Duchenne muscular dystrophy. Nature Reviews Disease Primers. 2021;7(1):13.
- ↑ Hoogerwaard EM, Bakker E, Ippel PF, Oosterwijk JC, Majoor-Krakauer DF, Leschot NJ, et al . Signs and symptoms of Duchenne muscular dystrophy and Becker muscular dystrophy among carriers in The Netherlands: A cohort study. Lancet 1999;353:2116-9.
- ↑ Norman A, Harper P. A survey of manifesting carriers of Duchenne and Becker muscular dystrophy in Wales. Clin Genet 1989;36:31-7.
- ↑ Rae MG, O'Malley D. Cognitive dysfunction in Duchenne muscular dystrophy: a possible role for neuromodulatory immune molecules. J Neurophysiol. September 1 2016; 116(3):1304-15. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5023417/.
- ↑ 13.0 13.1 13.2 13.3 13.4 Tink Martin, Mary Kessler. Neurological Intervention for Physical Therapy, 4ed. Elsevier. 2020
- ↑ 14.0 14.1 Medlineplus., 2014. Contracture deformity [online]. [viewed 2 October 2014]. Available from: http://www.nlm.nih.gov/medlineplus/ency/article/003185.htm
- ↑ Hyde, S.A., Floytrup, I., Glent, S., Kroksmark, A., Salling, B., Steffensen, B.F., Werlauff, U. and Erlandsen, M., 2000. A randomized comparative study of two methods for controlling Tendo Achilles contracture in Duchenne muscular dystrophy. Neuromuscular Disorders. , vol. 10, no. 4, pp. 257-263.
- ↑ Armando Hasudungan. Muscular Dystrophy - Duchenne, Becker and Mytonic. Available from: http://www.youtube.com/watch?v=o1uhhpjmzkw[last accessed 31/01/21]
- ↑ ilm kidunya. Duchenne Muscular Dystrophy by Dr Khalid Jamil Akhtar. Available from: http://www.youtube.com/watch?v=vbz6UG4iHhs [last accessed 25/05/13]
- ↑ 18.0 18.1 18.2 Wallace, G.B. and Newton, R.W., 1989. Gowers' sign revisited. Archives of Disease in Childhood. Sep, vol. 64, no. 9, pp. 1317-1319.
- ↑ Mercuri E, Pichiecchio A, Allsop J, Messina S, Pane M, Muntoni F. Muscle MRI in inherited neuromuscular disorders: Past, present, and future. J Magn Reson Imaging 2007;25:433-40.
- ↑ Mercuri, E., Bonnemann, C. G. & Muntoni, F. Muscular dystrophies. Lancet 394, 2025–2038 (2019). Comprehensive overview of the clinical and genetic aspects of muscular dystrophies.
- ↑ Elisa Panero, Rossella D’Alessandro, Ilaria Cavallina, Chiara Davico, Tiziana Mongini, Laura Gastaldi, Federica Ricci, Wearable Inertial Devices in Duchenne Muscular Dystrophy: A Scoping Review, Applied Sciences, 10.3390/app13031268, 13, 3, (1268), (2023).
- ↑ Pangalila, R. F. et al. Prevalence of fatigue, pain, and affective disorders in adults with duchenne muscular dystrophy and their associations with quality of life. Arch. Phys. Med. Rehabil. 96, 1242–1247 (2015).
- ↑ Autonomic Modulation in Duchenne Muscular Dystrophy during a Computer Task: A Prospective Control Trial - Scientific Figure on ResearchGate. Available from: https://www.researchgate.net/figure/Description-individuals-with-DMD-by-Vignos-Scale_tbl1_312845703 [accessed 27 Apr, 2023]
- ↑ Outcome measures in Duchenne muscular dystrophy: sensitivity to change, clinical meaningfulness, and implications for clinical trials Joana Domingos Francesco Muntoni https://doi.org/10.1111/dmcn.13634
- ↑ Werner D. Disabled Village Children: A Guide for Community Health Workers, Rehabilitation Workers, and Families 10th Updated printing 2022. California: Hesperian Health Guides,2022.p109-112.
- ↑ Garralda, M.E., Muntoni, F., Cuniff, A. and Caneja, A.D., 2006. Knee–ankle–foot orthosis in children with duchenne muscular dystrophy: User views and adjustment. European Journal of Paediatric Neurology. , vol. 10, no. 4, pp. 186-191.
- ↑ Medlineplus., 2014. Duchenne Muscular Dystrophy [online]. [viewed 3 October 2014]. Available from: http://www.nlm.nih.gov/medlineplus/ency/article/000705.htm
- ↑ Muntoni, F., Fisher, I., Morgan, J.E. and Abraham, D., 2002. Steroids in Duchenne muscular dystrophy: from clinical trials to genomic research. Neuromuscular Disorders. , vol. 12, pp. S162-S165.
- ↑ 29.0 29.1 Angelini, C. and Peterle, E., 2012. Old and new therapeutic developments in steroid treatment in Duchenne muscular dystrophy. Acta Myologica : Myopathies and Cardiomyopathies : Official Journal of the Mediterranean Society of Myology / Edited by the Gaetano Conte Academy for the Study of Striated Muscle Diseases. May, vol. 31, no. 1, pp. 9-15.
- ↑ Ogata, H., Ishikawa, Y.and Minami, R., 2009. Beneficial effects of beta-blockers and angiotensin-converting enzyme inhibitors in Duchenne muscular dystrophy. Journal of Cardiology. , vol. 53, no. 1, pp. 72-78.
- ↑ Matsumura, T., 2014. Beta-blockers in Children with Duchenne Cardiomyopathy. Reviews on Recent Clinical Trials. , vol. 9, no. 2, pp. 76-81.
- ↑ Sethna, N.F., Rockoff, M.A., Worthen, H.M. and Rosnow, J.M., 1988. Anesthesia-related complications in children with Duchenne muscular dystrophy. Anesthesiology. , vol. 68, no. 3, pp. 462-464.
- ↑ Galasko, C.S., 1993. Medical management of Duchenne muscular dystrophy. BMJ (Clinical Research Ed.). Mar 27, vol. 306, no. 6881, pp. 859.
- ↑ Karol, L.A., 2007. Scoliosis in patients with Duchenne muscular dystrophy. The Journal of Bone & Joint Surgery. , vol. 89, no. suppl_1, pp. 155-162
- ↑ 35.0 35.1 Duan, D., Goemans, N., Takeda, S. et al. Duchenne muscular dystrophy. Nat Rev Dis Primers 7, 13 (2021).
- ↑ Birnkrant DJ, Bushby K, Bann CM, Alman BA, Apkon SD, et al. Diagnosis and management of Duchenne muscular dystrophy, part 2: respiratory, cardiac, bone health, and orthopaedic management.. Lancet Neurol. 2018; 17(4):347-361. https://pubmed.ncbi.nlm.nih.gov/29395990.
- ↑ Birnkrant DJ, Bushby K, Bann CM, Apkon SD, Blackwell A et al. Diagnosis and management of Duchenne muscular dystrophy, part 3: primary care, emergency management, psychosocial care, and transitions of care across the lifespan. Lancet Neurol. 2018; 17(5):445-455. https://pubmed.ncbi.nlm.nih.gov/29398641.
- ↑ Prosensa., 2014. DMD - Duchenne Muscular Dystrophy [online]. [viewed 3 October 2014]. Available from: http://www.prosensa.eu/hc-professionals/duchenne-muscular-dystrophy
- ↑ Lord, J., Berham, B., Varzos, N., Cooper, D., Lieberman, J.S. and Fowler, W.M., 1990. Scoliosis associated with Duchenne muscular dystrophy. Archives of Physical Medicine and Rehabilitation. Jan, vol. 71, no. 1, pp. 13-17.
- ↑ Tink Martin, Mary Kessler. Neurological Intervention for Physical Therapy, 4ed. Elsevier. 2020
- ↑ Rose KJ, Burns J, Wheeler DM, North KN. Interventions for increasing ankle range of motion in patients with neuromuscular disease. Cochrane Database Syst Rev. 2010 Feb 17;2:CD006973.fckLR.
- ↑ Birnkrant, D. J. et al. Diagnosis and management of Duchenne muscular dystrophy, part 1: diagnosis, and neuromuscular, rehabilitation, endocrine, and gastrointestinal and nutritional management. Lancet Neurol. 17, 251–267 (2018). Part 1 of a three-part standard-of-care document for DMD.
- ↑ 43.0 43.1 Abd El Aziz AS, Abd ElAziz HG, Ali MS. Efficacy of two intervention approaches on functional walking capacity and balance in children with Duchene muscular dystrophy. Journal of Musculoskeletal & Neuronal Interactions. 2021;21(3):343.
- ↑ Bushbyb, K., Finkel, R., BirnkrantI, D.J., Case, L.E., Clemens, P.R., Cripe, L., Kaul, A., KinnetI, K., Mcdonalds, C. and Pandya, S., 2010. Diagnosis and management of Duchenne muscular dystrophy, part 2: implementation of multidisciplinary care. The Lancet Neurology. , vol. 9, no. 2, pp. 177-189.
- ↑ 45.0 45.1 45.2 Di Marco, M., YirrellI, J., Tewnion, J., KeddieE, A., Melville, P. and Harrison, L. DMD Scottish Physiotherapy Managment Profile. Available from: http://www.smn.scot.nhs.uk/DMD%20management%20profile%20-%20version%2020b).pdf
- ↑ Tay S, Lin J. Current strategies in management of Duchenne Muscular Dystrophy: Allowing patients to live with hope. Annals of the Academy of Medicine 2012;41(2):44-6.
- ↑ Bushby K et al. Diagnosis and management of Duchenne muscular dystrophy, part 2: implementation of multidisciplinary care. The Lancet Neurology 2010;9(2):177.
- ↑ Muscular dystrophy campaign., 2009. A Home Exercise Book: Physiotherapy management for Duchenne muscular dystrophy [online]. [viewed 7 October 2014]. Available from: http://www.muscular-dystrophy.org/assets/0001/1477/Physio_booklet_web.pdf
- ↑ 49.0 49.1 Mazzone, E., Messina, S., Vasco, G., Main, M., Eagle, M., D’Amico, A., Doglio, L., Politano, L., Cavallaro, F. and Frosini, S., 2009. Reliability of the North Star Ambulatory Assessment in a multicentric setting. Neuromuscular Disorders. , vol. 19, no. 7, pp. 458-461.
- ↑ Muscular dystrophy campaign. North Star Ambulatory Assessment [online]. [viewed 8 October 2014]. Available from: http://www.muscular-dystrophy.org/assets/0000/6388/NorthStar.pdf
- ↑ 51.0 51.1 Goemans N, Buyse G. Current treatment and management of dystrophinopathies. Neuromuscular Disorders 2014;16(5):1-13
- ↑ 52.0 52.1 52.2 52.3 52.4 Finder JD et al. Respiratory care of the patient with Duchenne muscular dystrophy: ATS consensus statement. Am J Respir Crit Care Med 2004;170(4):456-65.
- ↑ Kelfer HM, Singer WD, Reynolds RN. Malignant hyperthermia in a child with Duchenne muscular dystrophy. Pediatrics 1983;71:118-9.
- ↑ Wedel DJ. Malignant hyperthermia and neuromuscular disease. Neuromuscul Disord 1992;2:157-64.
- ↑ Larson CM, Henderson RC. Bone mineral density and fractures in boys with Duchenne muscular dystrophy. J Pediatr Orthop 2000;20:71-4.
- ↑ Aparicio LF, Jurkovic M, DeLullo J. Decreased bone density in ambulatory patients with duchenne muscular dystrophy. J Pediatr Orthop 2002;22:179-81.
- ↑ Smith AD, Koreska J, Moseley CF. Progression of scoliosis in Duchenne muscular dystrophy. J Bone Joint Surg Am 1989;71:1066-74
- ↑ Takaso M, Nakazawa T, Imura T, Okada T, Fukushima K, Ueno M, Takahira N, Takahashi K, Yamazaki M, Ohtori S, Okamoto H, Okutomi T, Okamoto M, Masaki T, Uchinuma E, Sakagami H.fckLRSurgical management of severe scoliosis with high risk pulmonary dysfunction in Duchenne muscular dystrophy: patient function, quality of life and satisfaction. Int Orthop. 2010 Feb 16. [Epub ahead of print]
- ↑ Katharine Bushby, Richard Finkel, David J Birnkrant, Laura E Case, Paula R Clemens, Linda Cripe, Ajay Kaul, Kathi Kinnett, Craig McDonald, Shree Pandya, James Poysky, Frederic Shapiro, Jean Tomezsko, Carolyn Constantin, Diagnosis and management of Duchenne muscular dystrophy, part 2: implementation of multidisciplinary care.
- ↑ Leibowitz D, Dubowitz V. Intellect and behaviour in Duchenne muscular dystrophy. Dev Med Child Neurol 1981;23:577-90.
- ↑ Cotton S, Voudouris NJ, Greenwood KM. Intelligence and Duchenne muscular dystrophy: Full-scale, verbal and performance intelligence quotients. Dev Med Child Neurol 2001;43:497-501.
- ↑ Anderson JL, Head SI, Rae C, Morley JW. Brain function in Duchenne muscular dystrophy. Brain 2002;125:4-13.
- ↑ Leibowitz D, Dubowitz V. Intellect and behaviour in Duchenne muscular dystrophy. Dev Med Child Neurol 1981;23:577-90.
- ↑ Karagan NJ, Richman LC, Sorensen JP. Analysis of verbal disability in Duchenne muscular dystrophy. J Nerv Ment Dis 1980;168:419-23.
- ↑ Pane M, Lombardo ME, Alfieri P, D'Amico A, Bianco F, Vasco G, Piccini G, Mallardi M, Romeo DM, Ricotti V, Ferlini A, Gualandi F, Vicari S, Bertini E, Berardinelli A, Mercuri E. Attention deficit hyperactivity disorder and cognitive function in Duchenne muscular dystrophy: phenotype-genotype correlation. J Pediatr. 2012 Oct;161(4):705-9.e1.
- ↑ Oxford Med Online Duchenne Muscular Dystrophy (4 ed.) Alan E. H. Emery, Francesco Muntoni, and Rosaline C. M. Quinlivan 0.1093/med/9780199681488.003.0005