Heat Illness in Sports
Original Editor - Puja Gaikwad
Top Contributors - Puja Gaikwad, Lucinda hampton, Kim Jackson, Wanda van Niekerk, Kapil Narale and Shaimaa Eldib
Introduction[edit | edit source]
Exertional heat-related illness (EHRI) is comprised of several states that afflict physically active persons when exercising during conditions of high environmental heat stress. If not treated EHRI in the extreme cases can be life threatening. Exertional heat stroke (ie a core body temperature of >40 ° C and mental status changes) is the most severe form of EHRI, and calls for immediate treatment (rapid body cooling) to reduce morbidity and mortality.
EHRI consists of a spectrum of conditions that range from mild (heat oedema, heat rash) to life-threatening (heat stroke). Deaths from sports-related heat stroke appear to be increasing, with eg football players at high risk.[1]
Types of Heat Illness[edit | edit source]
Heat illness is classified into two types:
- Classic heat illness is directly related to the environment and the way the environment is affecting one’s ability to dissipate heat. These factors include a rise in temperature and humidity, strong direct sun exposure, and still air. [2]
- Exertional heat illness (EHI) is primarily caused by an individuals' own heat production and can occur in all types of weather.
It should be noted that the treatment and identification do not change between these two types of heat illness but illustrates the fact that athletes should be aware of the signs of heat illness even in cooler and less humid climates.[3]
Levels of Heat Illness[edit | edit source]
Heat-related illnesses start out mildly uncomfortable and progress all the way to life-threatening. The conditions are, from least serious to most serious: heat oedema, heat rash, heat syncope, heat cramps, heat exhaustion and heatstroke.[2][3][4]
- Heat Oedema and Heat Rash: Heat oedema and heat rash are both the mildest sorts of heat illness. Heat oedema may occur as the body tries to dissipate heat by vasodilation and a shift of blood flow to the skin. This mostly happens in the lower extremities as fluid creates inflammation in the feet and ankles. Heat rash (also known as prickly heat or miliaria Rubra) is a pinpoint red rash that forms on the skin that was covered by clothing. This generally occurs in areas that have a higher concentration of heat glands, such as the trunk and groin, and is caused by the rise in sweat saturating the clothing and skin surface clogging sweat ducts.[3]
- Heat Syncope: Heat syncope, or fainting caused by heat, can happen during excessive heat exposure because blood is being shunted to the skin and extremities.[4] Rapid changes in body position (frequently seen in sitting to standing, or bending over and standing back up) may lead to a temporary change in blood pressure that causes an individual to faint. Most athletes recover quickly once laid flat, which allows blood flow to normalise. That being said, falling due to a rapid loss of consciousness could lead to a concussion, and an athlete who faints due to heat should be evaluated before being allowed to continue training or competing.[3]
- Heat Cramps: Heat cramps or muscle spasms have been notoriously linked with dehydration and electrolyte imbalances over the years. However, exercise-associated muscle cramps are more commonly related to a wider range of variables like fatigue and muscular imbalances. Although harmful to performance, exercise-associated muscle cramps are generally harmless to our health and most ordinarily occur on one side of the body. If experiencing bilateral, or both sides, cramping or full body cramping, this is often linked to a more serious condition like extreme dehydration or hyponatremia (depleted electrolytes from excessive water consumption) and should be immediately addressed by a physician or the medical team at the event.[5]
- Heat Exhaustion: Heat exhaustion should be taken seriously and managed quickly because it can advance to severe and potentially life-threatening conditions like heat stroke. Heat exhaustion classically presents with fatigue, dizziness, excessive sweating, nausea, vomiting, headache, fainting, weakness, and cold, clammy skin. An athlete with exhaustion typically still has normal cognitive and neurological function. They should be able to answer questions about their condition, where they are, who they are, etc.[6][7]
- Heat Stroke: Heatstroke is characterized by a core body temperature >104°F (40°C) with altered central nervous system functions such as irritability, confusion, combativeness, or maybe worse, loss of consciousness. Hot and dry skin is a sign of heat stroke, but it is important to understand an athlete may be sweating and still have heat stroke. The altered CNS function is the hallmark difference between heat exhaustion and heat stroke, but when unsure, treat the situation as if the athlete has heat stroke. Athletes showing signs of heat stroke have to be treated by medical professionals as soon as possible. It should be stressed that heat stroke is incredibly severe and may cause death if not treated quickly.[6][8][9]
Criteria for Diagnosis of Heat Illness[edit | edit source]
| Condition | Core Temperature °F (°C) Associated Symptoms | Associated Signs | |
| Heat oedema | Normal | None | Mild oedema in dependant areas (ankles, feet, hands) |
| Heat rash | Normal | Pruritic rash | Papulovesicular skin eruption over clothed areas |
| Heat syncope | Normal | Dizziness, generalised weakness | Loss of postural control, rapid mental status recovery once supine |
| Heat cramps | Normal or elevated but <104°F (40°C) | Painful muscle contractions (calf, quadriceps, abdominal) | Affected muscles may feel firm to palpation. |
| Heat exhaustion | 98.6°F-104°F (37°C-40°C) | Dizziness, malaise, fatigue, nausea, vomiting, headache | Flushed, profuse sweating, cold clammy skin, |
| Heat stroke | >104°F (40°C) | Possible history of heat exhaustion symptoms before mental status change | Hot skin with or without sweating, CNS disturbance (confusion, ataxia, irritability, coma) |
Risk Factors[edit | edit source]
Risk factors for the development of heat illness can generally be categories into 2 areas:
- Internal (related to the athlete)
- External (environmental) factors
Populations at high risk of heat illness include the elderly, children, and those with comorbid medical conditions which will inhibit their thermoregulatory ability. Alcoholism, living on the higher floors of multi-story buildings, and the use of psychiatric medications, like tricyclic antidepressants and typical antipsychotics, contribute to an increased risk of developing heat stroke.[10]
Internal Factors
- Age (<15 years or >65 years)
- Alcohol Consumption
- Comorbid medical conditions- respiratory, cardiovascular, hematologic
- Dehydration
- History of heat-related illness
- Lack of air conditioning
- Lack of appropriate sleep
- Medications or supplements
- Obesity
- Over-motivation
- Poor acclimatization
- Poor cardiovascular fitness
- Recent febrile illness
- Sickle cell trait
- Skin condition—eczema, psoriasis, burns, etc.
- Sunburn
- Use of psychiatric medications[11][12]
External (Environmental) Factors
- Activity level
- Excessive clothing wear
- Lack of water or sufficient shade
- Humidity
- Temperature (ambient)
- Wet bulb globe temperature[11][12]
Treatment[edit | edit source]
The goal is to get core body temperature down to a normal acceptable level (below 38°C or 100.4° F) as quickly as possible. It’s important to note that although fevers generally present at similar temperatures as hyperthermia (temperatures above 100.9° F) the underlying mechanism is different.[13]
The main focus of heat-related illnesses is to cool the athlete down as quickly as possible to protect the athlete’s brain and vital organs. To do that, the critical first step is to identify that a player is in trouble. This step is often missed, which allows heat illness to progress to serious levels. Evaluation of the ABC's is important in addition to removing equipment and clothing. Move the player away from direct sunlight and into a shaded, cooler environment. Finally, use cold applications - this can include dousing with cold water from a hose or shower, wrapping in cold towels, applying ice packs or immersion in an ice bath, and having them ingest cold fluids.[3]
Specific Strategies are as follows:
- Heat Oedema: Elevation of the affected limbs with relative rest and the use of compression garments may help with dependent swelling. Ensuring the athlete is well hydrated and has adequate salt intake is important as these conditions can delay resolution. Usually, this condition improves within 7 to 14 days as acclimatisation occurs or sooner if the athlete returns to his or her home climate.[13][3]
- Heat Rash/Miliaria: A staple of treatment consists of the avoidance of tight-fitting clothing. Symptoms are treatable with topical lotions like calamine or steroids of mid-potency like triamcinolone 0.1% cream, which can also help to reduce inflammation.[3]
- Heat Cramps: An athlete should cease physical activity and start oral rehydration. Rest and passive stretching of the muscle groups have also demonstrated to be helpful.[3]
- Heat Exhaustion: Move athletes into the shaded or air-conditioned area. Remove extra clothing and equipment. Cool the player with cold water, fans, and/or cold towels. Have athletes lie with legs raised above the heart level. Encourage athletes to drink chilled water or sports drink if not nauseated or vomiting. If the condition persists, seek medical attention More aggressive measures at cooling should take place, including lukewarm water sprayed over the skin with forced air conduction to promote evaporation and consideration towards parenteral rehydration if the athlete can not tolerate oral rehydration due to symptoms or degree of injury. Further, the correction of electrolyte and divalent disturbances can also require treatment.[3][13]
- Heat Stroke. The treatment strategies for athletes experiencing heat stroke is different and needs immediate medical care with the goal of lowering body temperature to below 104° F within 30 minutes.[3]
On-Field Treatment[edit | edit source]
- Recognize an athlete with signs or symptoms of heat illness.
- Initiate cooling methods: move to a cool area, ice bags to groin/axilla/neck, ice water tub immersion, fan-sprayed mist.
- Assess mental status changes.
- Assess the need for rectal temperature (and repeat during cooling every 3-5 min).
- Encourage liberal oral fluid intake with cool sports drinks or water if able to tolerate it.
- Check blood glucose and sodium levels if available.
- Access emergency medical system( EMS) immediately if the athlete has any of the following:
- Altered mental status
- Temperature elevated >104°F
- Persistent vomiting (unable to rehydrate orally)[13]
Treatment involves the replacement of fluid losses with a preference towards oral rehydration over parenteral rehydration. Supine positioning with leg elevation above the level of the heart can be helpful. Orthostatic sign measurements are often considered as an adjunct to monitor for adequate replacement additionally to the resolution of symptoms during positional changes.[14]
Prevention[edit | edit source]
The best ways to prevent heat-related illness are to heat acclimatise prior to training heavy or racing in hot weather, monitor and manage hydration requirements, and incorporate cooling techniques to assist manage core body temperature. These things will help to reduce the physiological strain of training and racing in the heat and optimize performance.[16][13]
Heat Acclimation[edit | edit source]
Acclimatization to heat and humidity for at least 10-14 days prior to competition.[13]
See the Heat Acclimation page for an explanation of the physiological process of being accustomed to the heat.
see the Physical Activity and Perspiration page for a different explanation of heat acclimation as it relates to sweating, and the discussion of physical exercise and perspiration as it may relate to heat illnesses.
Hydration[edit | edit source]
Dehydration is one of the key precursors to developing a heat-related illness. Although dehydration occurs due to an inadequate intake of fluids, it may be made worse by an additional amount of fluid loss through sweating, putting an athlete in a state of hypohydration. During strenuous exercise in the heat, sweat rates can reach 1.5 litres/hour or higher sometimes. The ideal recommendations are to consume 16 – 24 ounces of the fluid hourly, but endurance athletes in hot environments often need to consume 2-3 times that much. An athlete can figure out the approximate sweat rate by weighing themselves pre- and post-workout.[13]
Cooling Practices[edit | edit source]
Wear light-coloured, loose-fitting clothing, and protective against the sun.[2][13]
Modifying controllable factors[edit | edit source]
These preventive measures have been mentioned below:
- Make sure athletes are adequately hydrated before practice or competition.
- Make fluids readily available for all athletes. There's no benefit to restricting access to water; athletes don't adapt to dehydration.
- Remove equipment/clothing. As temperature increases, practices should be modified to remove the necessity for equipment that increases heat retention, including helmets, shoulder pads, and restrictive clothing.
- Schedule practice matches and competitions during cooler portions of the day.
- Supply water and provide shade for dousing/wetting clothing during breaks.
- Encourage proactive monitoring of fluid intake and athlete behaviour. Talk to them during breaks, assign hydration buddies so that athletes can monitor and remind one another to stay hydrated.
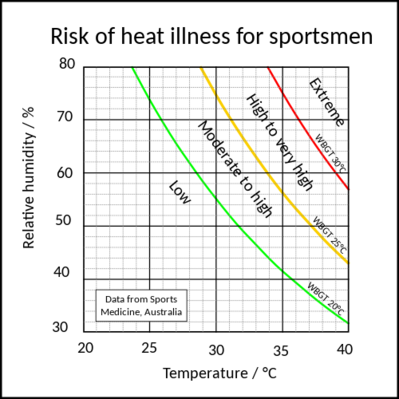
- Increase frequency of breaks: Guidelines based on wet bulb globe temperature, a measure that takes under consideration temperature, humidity, sun angle, and other factors in measuring what it calls ‘heat stress’.
- Activity planning or moderation of activity based on heat, humidity, athlete’s injury history, and training levels, etc.
- Reviewing all medications with a physician including supplements and herbs.[2][3]
Acclimatization Guidelines for Football[edit | edit source]
NCAA Guidelines[edit | edit source]
5-day acclimatization period at the beginning of the season— restricted to no more than 1 practice session a day lasting <3 hours
- Helmet wear only for days 1, 2
- Helmet plus shoulder pads only days 3, 4
- Full equipment on day 5
- After day 5, multi-practice days are allowed with specific guidelines:
- The total practice time per day must be <5 hours
- A single practice may not last longer than 3 hours
- At least 3 hours of rest between practices must occur
- The multi-practice days must not occur on consecutive days[2][17]
ACSM Guidelines[edit | edit source]
6-day acclimatization period at the beginning of the season - no more than 1 practice lasting <3 hours during this time
- Days 1, 2: helmet only
- Days 3-5: helmet and shoulder pads only
- Day 6: full equipment
- No contact drills during the acclimatization period
- Limit consecutive practice days to 6
- Day 8: multi-practice sessions with the same restrictions as above.[2][18]
Fluid Management during Exertion: Specific Guidelines[edit | edit source]
| NCAA Sports Medicine | 8 to 16 oz of water 1 hour before exertion.
Continue drinking during activity every 15-20 min. At the end of the exercise, replace fluids lost (1 qt [32 oz] for every 2 pounds lost) [17] |
| National Athletic trainers association (NATA) | 16-20 oz of fluid 2-3 hours before exertion.
Just before exercise, take in another 6-10 oz. Take 6-10 oz every 15-20 min during exercise. After the event, consume fluid in excess of what was lost.[19][20] |
Return to Play[edit | edit source]
For milder forms of heat illness, it is probably safe for athletes to return within 24 hours with proper hydration. athletes should be evaluated by a physician prior to return to play.
In order to successfully return to full participation after an exertional heat stroke (EHS), a specific return-to-play (RTP) strategy should be implemented. These guidelines are as follows:
- Physician clearance prior to return to physical activity - an athlete must be asymptomatic and lab tests should be normal.
- Recovery time is primarily dictated by the severity of the illness.
- The athlete should begin a gradual RTP protocol under the direct supervision of an appropriate healthcare professional such as an athletic trainer or physician.
- In general, they should wait at least 1 week before resuming exercise, first in a cool environment with light activity, and then gradually progress intensity, heat exposure, and amount of equipment.[2]
References[edit | edit source]
- ↑ Poore S, Grundstein A, Cooper E, Shannon J. Regional differences in exertional heat illness rates among Georgia USA high school football players. International journal of biometeorology. 2020 Apr;64(4):643-50.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Howe AS, Boden BP. Heat-related illness in athletes. The American Journal of Sports Medicine. 2007 Aug;35(8):1384-95.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 Leiva DF, Church B. Heat Illness. InStatPearls [Internet] 2020 Jan 16. StatPearls Publishing.
- ↑ 4.0 4.1 Giersch GE, Belval LN, Lopez RM. Minor Heat Illnesses. InExertional Heat Illness 2020 (pp. 137-147). Springer, Cham.
- ↑ Miller KC. Exercise-associated muscle cramps. InExertional Heat Illness 2020 (pp. 117-136). Springer, Cham.
- ↑ 6.0 6.1 Altman, Joshua MDa; Stern, Evan MDb; Stern, Mori MDc; Prine, Bryan MD, CAQ-SMd; Breuhl Smith, Kristy MDe; Smith, Michael Seth MD, CAQ-SM, PharmDd Current paradigms in the prehospital care of exertional heat illness: A review, Current Orthopaedic Practice: January-February 2020 - Volume 31 - Issue 1 - p 1-7 doi: 10.1097/BCO.0000000000000824
- ↑ Armstrong LE. Heat Exhaustion. InExertional Heat Illness 2020 (pp. 81-115). Springer, Cham.
- ↑ Eichner ER. Updates on Heat Stroke, Carbon Monoxide, and Muscle Cramping. Current Sports Medicine Reports. 2020 Nov 1;19(11):446-7.
- ↑ Agustini NN, Arsani NL. Exertional Heat Stroke. InProceeding ICOPESH (International Conference on Physical Education, Sport, and Health) 2020 May 1 (pp. 63-66).
- ↑ Hew-Butler T, Almond C, Ayus JC, Dugas J, Meeuwisse W, Noakes T, Reid S, Siegel A, Speedy D, Stuempfle K, Verbalis J. Consensus statement of the 1st international exercise-associated hyponatremia consensus development conference, Cape Town, South Africa 2005. Clinical Journal of Sport Medicine. 2005 Jul 1;15(4):208-13.
- ↑ 11.0 11.1 Westwood CS, Fallowfield JL, Delves SK, Nunns M, Ogden HB, Layden JD. Individual risk factors associated with exertional heat illness: A systematic review. Experimental Physiology. 2020 Apr 6.
- ↑ 12.0 12.1 Pryor JL, Périard JD, Pryor RR. Predisposing Factors for Exertional Heat Illness. InExertional Heat Illness 2020 (pp. 29-57). Springer, Cham.
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 13.7 Lipman GS, Gaudio FG, Eifling KP, Ellis MA, Otten EM, Grissom CK. Wilderness Medical Society Clinical Practice Guidelines for the Prevention and Treatment of Heat Illness: 2019 Update. Wilderness & Environmental Medicine. 2019 Dec 1;30(4):S33-46.
- ↑ Bhatia PK, Biyani G, Mohammed S. Hyperthermia and Heatstroke. chronic illness.;10:11.
- ↑ Heat stroke prevention available from https://www.youtube.com/watch?v=Zg7P7EHgHb8
- ↑ Larsen T, Kumar S, Grimmer K, Potter A, Farquharson T, Sharpe P. A systematic review of guidelines for the prevention of heat illness in community-based sports participants and officials. Journal of science and medicine in sport. 2007 Feb 1;10(1):11-26.
- ↑ 17.0 17.1 17.2 https://www.ncaa.org/sport-science-institute/heat-and-hydration
- ↑ https://www.acsm.org/acsm-positions-policy/official-positions/ACSM-position-stands
- ↑ Casa DJ, Csillan D, Inter-Association Task Force Participants, Armstrong LE, Baker LB, Bergeron MF, Buchanan VM, Carroll MJ, Cleary MA, Eichner ER, Ferrara MS. Preseason heat-acclimatization guidelines for secondary school athletics. Journal of Athletic Training. 2009 May;44(3):332-3.
- ↑ 20.0 20.1 https://www.nata.org/practice-patient-care/health-issues/heat-illness