Module 3: Positioning Your Child
Page Outcomes[edit | edit source]
When you have finished this page, you should be:
- More confident to position a child with cerebral palsy,
- Be able to show others better ways to position a child with cerebral palsy
Positioning and Handling[edit | edit source]
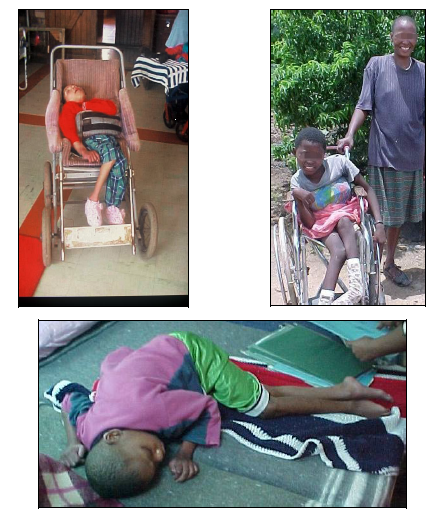
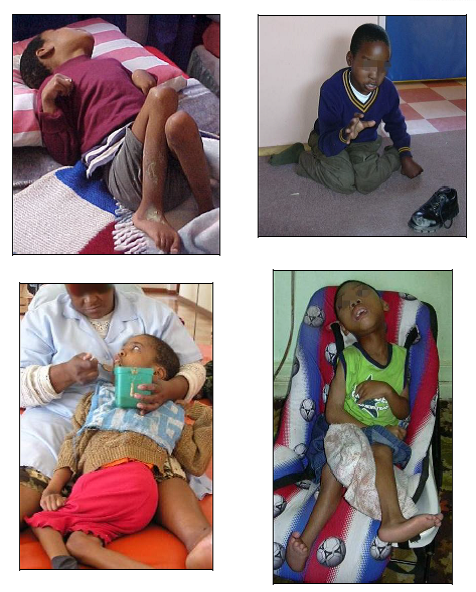
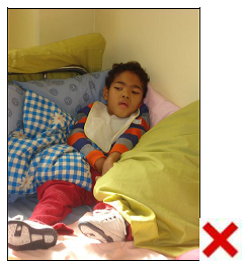
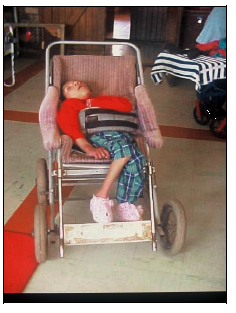
Here are some photos of poor positioning and handling of children with cerebral palsy
Good Handling and Positioning[edit | edit source]
Here are some of the benefits of good handling and positioning skills
Now let's look at the problems with poor handling and positioning techniques
And as children with disabilities gain access to wheelchairs, they very often spend long hours poorly positioned in the wheelchair, and are still unable to move themselves. And they still develop a crooked back and other disabling deformities, including eventually breathing difficulties due to the chest space being so crooked and confined. You can see this in some of the pictures above
Now let's look at positioning a child, and what you can do to improve her position.
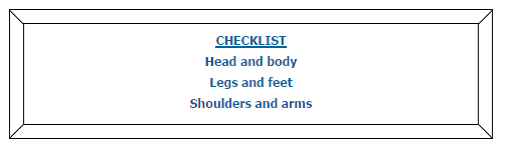
In the next section we will be looking at specific positions, both those that are 'poor' positions, and suggestions for „helpful‟ positions. For each position, we will use this checklist (see diagram below) to help us decide in an ordered way whether the child is in a poor or helpful position.
Lying
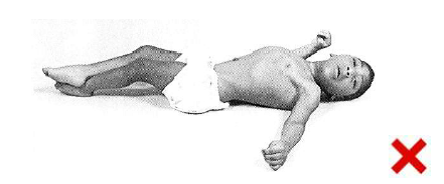
Supine (on their back)
Poor position
|
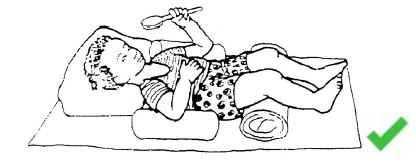
Correct position
|
Supine Checklist
Head and body
- If she can move her head on her own, make sure it is comfortable
- If she cannot move her head on her own, make sure it is in the middle and comfortable
- Her body (spine) must be straight – support on her sides if needed with a rolled up towel to keep her straight
Legs and feet
- Bend her hips – this helps to release tension in her lower back which is often arched, and it
- helps to relax stiffness in her legs. Place support under her knees to keep hips bent (not under her feet)
- Keep her legs open and uncrossed – use a pillow between if needed
- Feet should be as close to a standing position as possible – if her feet push down, talk to a therapist about the need for an ankle/foot orthosis
Shoulders and arms
- They should be forward and supported, especially if her arms pull back. This position also helps to relax her upper back, and allows her hands to open more easily.
- Lying in a hammock can help to relax tight muscles.
- Babies/small children can „hang‟ in a large towel (held by two adults) to relax tight muscles.
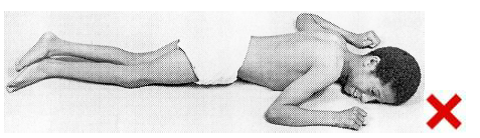
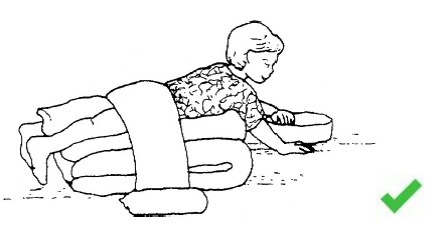
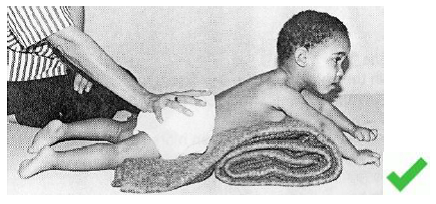
Prone ( on their tummy )[edit | edit source]
| | |
|
|
Prone Checklist
Head and body
- In a straight line
- Encourage her to lift her head and look at something in front of her on the floor. This is a good time to get a sibling, also lying on the floor, to play with her
Shoulders and arms
- Her arms should be in line with or slightly in front of her shoulders.
Make sure the pillow or towel she is lying on comes all the way up to her armpits to help keep her arms forward
- If possible, encourage her to open her hands and push down on them
Parents may need to gently open them out for her; if too stiff to stay open, keep helping her each time you use this position
Legs and feet
- Straight – push down on her bottom from side to side in a rocking motion to help her straighten her hips
- You can put weighted bags over her hips
MOST IMPORTANT about this position is that it is not for all children! Be careful when using this position for children who are always pushing back strongly with their heads. It is possible that it will reinforce the pushing back of the head, while the child is not actually learning to use her arms or control her head.
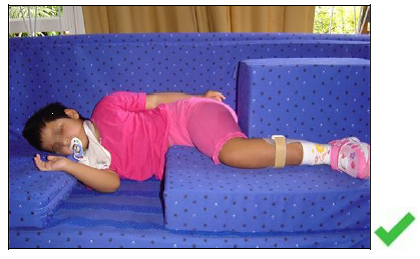
Side Lying[edit | edit source]
Side-lying checklist
Head and body
- Head supported on a pillow so her chin is level (in the middle, with her head and spine in a straight line)
- Give good support at her back, from the top of her head to her feet
Shoulders and arms
- Her lower shoulder and arm must be brought forward so they are not trapped underneath her
- Keep both arms forward to bring her hands together – encourage her to use her hands by playing a game with her, or putting a toy nearby for her to touch and reach for
Legs and feet
- Keep her bottom leg straight
- Support her top leg bent at her knee with pillows or blankets so her knee is level with her hip – this is important to help prevent injury to her hip (dislocation)
- Bending one leg and keeping the other straight helps to relax the stiffness in her legs
| During the day this position should be changed from one side to the other, or to another position, every half an hour. | This is also a good position for a child to sleep in. |
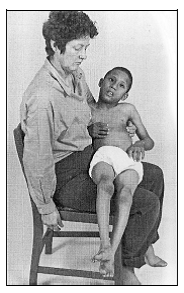
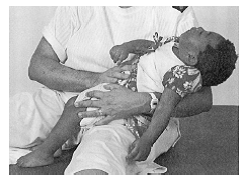
Sitting with Carer[edit | edit source]
These are poor positions because:
- Her head is hanging backwards, or to one side, or just leaning against the caregiver
- She is just lying, and not sitting on her bottom
- Her hips are not bent, and wrong muscles are working
- Her hands are not free to do anything
- Her arms aren't helping her to sit
- She is not able to do anything with her hands
Sitting with a carer checklist
Head and body
- If she cannot hold her head upright, make sure she is sitting up straight with the head and her back supported.
- If she can hold her head upright, use your hands to support her chest and/or hips just enough to help her stay up straight and control her head.
- She should be working her muscles to move her body and keep it upright
Legs and feet
- Bend her hips to at least a right angle – this will help keep her back in a good position and help stop her from pushing backwards and sliding off your lap.
- If possible, have her feet supported.
Shoulders and arms
- Her shoulders should be slightly forward so that her arms and hands are in front of her body, and she can explore objects and her own body.
It is also important for your child‟s development to be given an opportunity to practice using the muscles she needs to balance in sitting. Play a game with her, or help her explore her own body, toys, or other objects. This shows a more active way of playing with your child in a good position.
Sitting on a chair, in a buggy, or on a couch [edit | edit source]
These are poor positions because:
- Her head is pushing back, and she tends to slide herself out of the chair
- Hips are too straight and stiff
- Shoulders are not supported, and are either pulling back, or pushed too far forward
- She leans sideways and is not stable
- Leg problems can develop from twisting of leg bones
Sitting checklist:
Head and body
- She sits upright with her back straight and her head upright
- Her buttocks are all the way to the back
- If she has a lap strap, make sure it is tightened firmly enough to stop her from sliding down in the chair
Legs and feet
- These must be supported
Shoulders and arms
- These should be supported slightly forward and in front of her body.
Sitting on the floor[edit | edit source]
Therapists generally don‟t like your child to sit in this position. However, if it is the only way that allows your child to be independent in sitting, then it should probably be allowed. But do not let her sit in this position all the time.
- This position can hurt the knees and hips and hips of the child.
- She does not need much control to sit like this, so she does not need to learn to or practice balancing her upper body over her pelvis.
- She does not learn to develop a good sitting balance if she is always in this position. She may therefore never learn to sit with good balance in any other sitting position.
Floor sitting suggestions:
- She can sit independently with legs crossed
- She should sometimes sit with legs straight, not always bent (beware of contractures)
- Sitting with her back in a corner helps to keep shoulders forward and head level
- Her hands are more free to do something
- What about sitting on her side? First one side, and then the other.
Standing[edit | edit source]
Poor position:
|
These positions in standing are much more functional:
- Her balance is not difficult in this position
- Her hips and knees are in a good position, helping to keep her feet flat
- Her shoulders and arms are forwards
- She no longer needs to hold on for support
- Her hands are now free to do something
- Look at her smile!
Standing frame checklist:
Head and body
- Her back is straight – if her body leans to the left or right, put a rolled up towel on either side of her in the frame to keep her body straight
- Her hips are facing the front – adjust gently if necessary
- Her shirt is covering her tummy so that her skin is not touching the Velcro in front
Legs and feet
- Her feet are firmly on the ground (including her heels), her toes are facing forward, and her feet are not falling in or out
- If you can easily move her feet, she is not putting enough weight on them. Loosen the frame, and let her fall more onto her feet before easing her into standing again and closing the frame.Recheck her hips and feet
- If the child‟s feet are in a very poor position, she should only stand once she has been assessed for, and is using, orthotics
Shoulders and arms
- Her arms should come forward onto the tray, which should be at about nipple height.
- It is good if she pushes on her arms, or uses them to touch a toy or object she likes on her tray.
Standing is very important for all children above the age of 1 year (this is when children without disabilities will usually start to stand).This includes those children who do not even try to or cannot stand by themselves at all.
Remember rather use a more helpful position than a poor position, even if you're not doing anything with her
PDF Handout[edit | edit source]
Hambisela Module 3: Positioning your child
Sources and Resources[edit | edit source]
Ideas from many sources have helped us to develop the Hambisela programme. The following material and references have been particularly helpful, either as sources or as inspiration on how to present training, and we gratefully acknowledge their use. In many cases we have been given permission to use photographs. Where permission could not be obtained, the faces have been re-touched in order to protect identity
- Disabled Village Children – A guide for community health workers, rehabilitation workers, and families, David Werner, The Hesperian Foundation, Berkeley (1999).
- Promoting the Development of Young Children with Cerebral Palsy – A guide for mid-level rehabilitation workers, World Health Organisation, Geneva (1993).
- Let's Communicate – A handbook for people working with children with communication difficulties, World Health Organisation, Geneva (1997).
- Community Based Rehabilitation -- Training and Guide, World Health Organisation, Geneva (1989).
- Cerebral Palsy, ga se boloi (it‟s not witchcraft), Physiotherapist Department of Gelukspan Center, Reakgona.
- Polokwane Hospital CP Group Manual, Polokwane Hospital.
- Community-Based Rehabilitation Workers – a South African training manual, Marian Loveday, SACLA Health Project, Cape Town (1990).
- Foden Manuals 1-4, Foden Centre, East London (1999).
- Practicing the new ways of feeding your child at home, Diane Novotny, Speech, Language and Feeding Therapist, Western Cape CP Association & Red Cross Children‟s Hospital, Cape Town (circa 2006)
- Learning for Life, Masifunde 2002, Staff Development Special Care Centres, Cape Mental Health.
- The Education of Mid-Level Rehabilitation Workers, World Health Organisation, Geneva (1992).
- Disability Prevention and Rehabilitation in Primary Health Care – A guide for district health and rehabilitation managers, World Health Organisation, Geneva (1995).
- Disability Prevention and Rehabilitation – A guide for strengthening the basic nursing curriculum, World Health Organisation, Geneva (1996).