Obstructed Defecation Syndrome
Top Contributors - Khloud Shreif, Temitope Olowoyeye, Kim Jackson and Aminat Abolade
Introduction[edit | edit source]
Obstructed defecation syndrome (ODS) is a pelvic floor disorder[1] characterized by constipation with straining during defecation, incomplete evacuation, and the need for digital support.
It consists of :
- Structural disorders such as rectocele, rectal mucosal intussusception, solitary rectal ulcer syndrome, enterocele, or descending perineum syndrome
- Functional disorders such as dysynergy defecation.[1][2]
ODS occur significantly more frequently in women than in men. Increases with advancing age in both sexes.[3]
Clinical Anatomy and Physiology[edit | edit source]
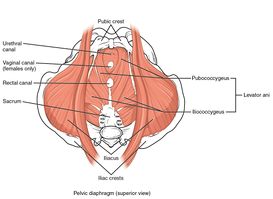
The levator ani muscles as a component of pelvic floor muscles ( the iliococcygeus, the pubococcygeal, and the puborectalis muscles) in addition to its role as a supportive structure and keeping visceral and internal organs in place, levator ani muscles specifically puborectalis have a role to maintain the urinary and fecal continence, contraction, and relaxation of puborectalis, lower abdominal muscles, and anal sphincter work synchronically for normal and smooth defecation.
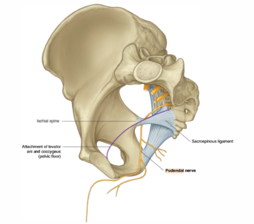
The pudendal nerve innervates the external anal sphincter and part of the puborectalis muscle, with frequent and prolonged straining that may stretch the pudendal nerve causing pudendal neuropathy.
While we have voluntary control over the external anal sphincter the internal anal sphincter muscles are involuntary muscles affected by the rectum, it is relaxed if the rectum is filled with stool and vice versa, so the sensitivity of the rectum is important for normal physiology.[4]
During normal defecation, the relaxation of the anal sphincters and the puborectalis muscle allows the anorectal angle to widen and the perineum to descend. Concurrently, the voluntary effort of bearing down increases the intra-abdominal pressure. These movements (mixed voluntary and involuntary movements) enable the development of a stripping wave which moves the stool from the rectum and causes the relaxation pelvic floor muscles and the anus, resulting in stool evacuation.[4]
Mechanism of Injury / Pathological Process[edit | edit source]
In general the pathogeneses of ODS varying from:
- Neurological origin (multiple sclerosis, spinal cord lesions, and pudendal neuropathy that impairs rectal sensitivity cause excess distension and stretch of the rectal wall, paradoxical rectal contractions and overflow incontinence can happen[5].
- Muscular origin such as (pelvic floor dyssynergia, anismus)
- Psychological origin (anxiety and spastic colon).
- Organ/ mechanical origin, cases of rectocele, outlet rectal obstruction, or intussusception obstruction is defined as overlapping of a part of intestine to the adjacent part blocking the passage of food and fluid.
Cases of rectal prolapse, rectocele most common in female. and internal rectal mucosal prolapse are most common associated and found in patient with ODS[6].
Clinical Presentation[edit | edit source]
The patient will have symptoms of the need to strain with bowel movement, episodes of incomplete evacuation, fragmented stool, pelvic heaviness, and sometimes accidental bowel leakage.
Frequent, prolonged straining becomes the prime mover this may cause stretch on the pudendal nerve and pudendal neuropathy causing rectal hypo sensation, internal organ descends (prolapse), muscle weakness, and spending too much time than usual in toilet.
Lower abdominal/rectal pain, feeling of incomplete evacuation of the rectum. The patient will tend to use perineal manipulation to help with the evacuation.
Patients with ODS will have a small, more hard stool and difficulty to evacuate, responses to laxatives and enema, and less effective to trigger the peristaltic reflex[5].
Fecal incontinence one of the symptoms of ODS.
Diagnosis[edit | edit source]
Diagnosis of ODS is essentially based on detailed evaluation of patient's clinical history and the use of some imaging techniques.
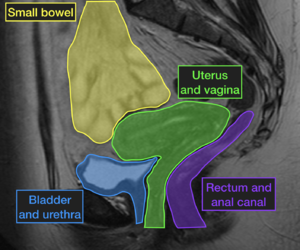
Defecography: This imaging technique is particularly used prior to surgery to confirm rectal prolapse, excessive perineal descent, a significant rectocele, an enterocele, or internal rectal intussusception. It measures and records the anatomy of the rectum and pelvic floor functions at rest, during coughing, squeezing, and straining to expel barium from the rectum.[7]
The colonoscopy: rule out rare causes of obstructive defecation tumors for example.
Anorectal manometry: a primary diagnostic test to assess rectum hyposensitivity, use inserted balloon into rectum fill with water or air to trigger the need for evacuation.[7]
Electromyography (EMG): Used to assess the strength and coordination of pelvic floor muscles around the anus, vagina, and the movement of rectum during defecation.
Perineal ultrasound: A painless procedure done in lithotomy position using a perineal or abdominal probe.[8]
Outcome Measures[edit | edit source]
Obstructed Defecation Syndrome score: consists of 5 items each item graded from 0-5, as 0 no symptoms and 20 sever symptoms[9].
| Symptoms | 0 | 1 | 2 | 3 | 4 |
|---|---|---|---|---|---|
| Excessive straining Rarely Sometimes Usually Always | Never | rarely | sometimes | usually | always |
| Incomplete rectal evacuation | Never | rarely | sometimes | usually | always |
| Vaginal/Perineal digital pressure | Never | rarely | sometimes | usually | always |
| Abdominal discomfort/pain | Never | rarely | sometimes | usually | always |
| Use of enemas/laxative | Never | rarely | sometimes | usually | always |
Management / Interventions[edit | edit source]
Conservative treatment[edit | edit source]
Conservative management usually is the first line management of anorectal dysfunction because there is minimal risk and a high rate of success with completion of therapy. It involves change in dietary regimen and pelvic floor rehabilitation.
Dietary regimen
Patients are encouraged to consume food rich in fibers as it affects stool consistency and helps in digestion of other types of food[5], to drink plenty of water
Is the first step in the treatment of patient with ODS mainly for patients with pelvic floor dyssynergy, some RCT show it is effect is superior to patient education and laxatives[10].
Before start explain to the patient the defecation problems result from un voluntary and unconscious contraction of anus, a rectal manometry (balloon inflated with air or water) and a screen in front of patient to give feedback of performance and how to correct.
In patient with pelvic floor dyssynergia, train the patient to try to relax the pelvic floor muscles during stimulated defecation and instead tighten the abdominal muscles and lower the diaphragm to increase the intra-abdominal pressure and push the stool[10]
Surgical intervention[edit | edit source]
surgical interventions should be carried if the conservative treatment failed and there is structural or organ origin for the problem such as in some cases of rectocele, rectal obstruction, or intussusception.
Rectocele can be managed via pelvic floor rehabilitation as long it isn’t significant and don’t become larger.
Physiotherapy Management[edit | edit source]
Physiotherapy is regarded as the cornerstone management[8] of ODS. It involves pelvic floor muscle retraining, biofeedback, and electrical stimulation of the pelvic floor and functionally associated musculature. A pelvic health physiotherapist carries out an assessment of the pelvic floor to identify abnormalities from which a therapeutic program is individualized and prescribed.[11]
Standardizes biofeedback-guided pelvic floor exercise[12] verbal training techniques with or without instruments has been shown to be helpful.[13]
References[edit | edit source]
- ↑ 1.0 1.1 Rao SS, Go JT. Treating pelvic floor disorders of defecation: management or cure?. Current gastroenterology reports. 2009 Aug;11(4):278-87.
- ↑ Ascanelli S, Portinari M, Canella M, Solari S, Dall’Omo F, Danese S, De Troia A, Carcoforo P. Obstructed defecation syndrome associated with paradoxical puborectalis contraction: osteopathic treatment versus anal biofeedback. Results of a pilot study. Techniques in Coloproctology. 2021 May;25:589-95.
- ↑ Siproudhis L, Lehur PA. Defecation disorders. Coloproctology. 2017:121-33.
- ↑ 4.0 4.1 Poylin V, Cataldo TE. Anal physiology: the physiology of continence and defecation. The ASCRS Textbook of Colon and Rectal Surgery. 2016:37-44.
- ↑ 5.0 5.1 5.2 Podzemny V, Pescatori LC, Pescatori M. Management of obstructed defecation. World journal of gastroenterology: WJG. 2015 Jan 28;21(4):1053.
- ↑ Linardoutsos D. Assessment and treatment of obstructed defecation syndrome. InCurrent Topics in Faecal Incontinence 2019 May 22. IntechOpen.
- ↑ 7.0 7.1 Podzemny V, Pescatori LC, Pescatori M. Management of obstructed defecation. World journal of gastroenterology: WJG. 2015 Jan 1;21(4):1053.
- ↑ 8.0 8.1 Robert-Yap J. Diagnosis and management of pelvic floor dyssynergia. Hamdan Medical Journal. 2021 Jan 1;14(1):1-8.
- ↑ Renzi A, Brillantino A, Di Sarno G, d’Aniello F. Five-item score for obstructed defecation syndrome: study of validation. Surgical innovation. 2013 Apr;20(2):119-25.
- ↑ 10.0 10.1 Wald A, Bharucha AE, Cosman BC, Whitehead WE. ACG clinical guideline: management of benign anorectal disorders. Official journal of the American College of Gastroenterology| ACG. 2014 Aug 1;109(8):1141-57.[1]
- ↑ Pedraza R, Nieto J, Ibarra S, Haas EM. Pelvic muscle rehabilitation: a standardized protocol for pelvic floor dysfunction. Advances in Urology. 2014 Oct;2014.
- ↑ Wen NR, Hu YL, Zhao L, Tuxun T, Husaiyin A, Sailai Y, Abulimiti A, Wang YH, Yang P. Biofeedback-guided pelvic floor exercise therapy for obstructive defecation: an effective alternative. World Journal of Gastroenterology: WJG. 2014 Jul 7;20(27):9162.
- ↑ George SE, Borello-France DF. Perspective on physical therapist management of functional constipation. Physical therapy. 2017 Apr 1;97(4):478-93.