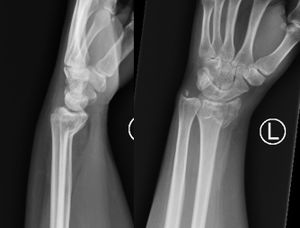
Smith's Fracture
Definition/Description[edit | edit source]
Smith's Fracture is a fracture of the distal end of the radius caused by a fall on the back of the hand (flexed), resulting in a volar displacement of the fractured fragment. It is also known as a reverse Colles fracture. The Smith's fracture was named by Irish surgeon Robert William Smith in 1847, however, this injury was first named for French Physician Jean-Gaspard-Blaise Goyrand (1746-1814) and is commonly known as a Goyrand fracture in French literature[1].
Aetiology[edit | edit source]
The causes of the fracture:
- a fall on a flexed wrist or
- a direct blow to the dorsal aspect of the wrist.
Mechanism of Injury:
Injury resulting from a fall on the palm of the hand, the dorsum or ulno‐dorsum of the hand, or a fisted hand[2] or a direct blow to the back of the wrist[3] causing a volar displacement of the distal radius. The mechanism of injury includes:
- tripping forward while walking or
- falling while cycling or
- slipping backwards
Epidemiology[edit | edit source]
The injury site, i.e., the distal radius, is the most common fracture site in the upper limb, accounting for the second most common fracture in the elderly. Smith fracture makes up approximately 5% of all combined radial and ulnar fractures[1].
The highest incidence of Smith's fractures is in young males after sustaining high-energy falls and in elderly females who suffering a low energy fall due to osteoporosis[1]
Classification[edit | edit source]
Smith fractures divide into three types[1]:
- Type I - most common type, accounting for about 85% of cases, is an extra-articular fracture through the distal radius
- Type II - less common, accounting for approximately 13%, is an intra-articular oblique fracture, also referred to as a reverse Barton fracture
- Type III - uncommon, less than 2%, is a juxta-articular oblique fracture
Clinical Presentation[edit | edit source]
The physical exam may reveal pain, swelling, and reduced ROM, and a deformity of the distal forearm, but the direction of volar angulation is difficult to spot visually. The diagnostic criteria for Smith's Fracture is a deformed wrist with swelling visible on the volar side and the prominence of the ulna along the dorsum of the wrist. Besides the volar displacement of the distal fragment, disruption of the distal radioulnar joint and the triangular fibrocartilage complex often occurs. There may also be an association of ulnar styloid base fractures[1].
Evaluation of the extremity's neurovascular status is critical. Research suggests that up to 15% of Smith's fractures may show symptoms of acute carpal tunnel syndrome from compression to the median nerve. Both radial and ulnar nerve compression are less commonly involved. Acute compartment syndrome of the forearm is also seen in Smith's Fracture.[1]
Diagnosis[edit | edit source]
X-rays[edit | edit source]
AP and the lateral radiograph of the wrist can diagnose the fracture. It can show the presence of a distal radial fracture with volar angulation, the fracture location (extra-, juxta-, or intra-articular), the degree of angulation, and displacement. It can also comment on carpal malalignment, carpal fractures, and the articulation of the radio-lunate and radio-scaphoid joints. Additional radiographs of the wrist such as traction, oblique, and fossa lateral views may provide critical information about the associated soft tissue injuries[1].
CT Scan[edit | edit source]
In cases of comminuted or intra-articular fracture, a CT scan assists not only the pattern of injury but also helps the surgeon plan for a strategy for operative reduction[1].
Differential Diagnosis[edit | edit source]
- Colles Fracture - extra-articular distal radius fracture with dorsal displacement/angulation[1]
- Barton Fracture - intra-articular distal radius fracture with dorsal displacement/angulation[1]
- Reverse Barton Fracture - intra-articular distal radius fracture with volar displacement/angulation[1]
- Die-Punch Fracture - fracture of the articular surface with depression of the lunate facet[1]
- Chauffer’s Fracture - avulsion fracture of the radial styloid[1]
- Distal Radioulnar Joint (DRUJ) disruption- injury to the sigmoid notch of the radius and the lunate facet[1]
- Triangular Fibrocartilage Complex (TFCC) tear - damage to the cartilaginous structure on the ulnar aspect of the wrist[1]
- Galeazzi Fracture - fracture to the distal third of the radius with disruption of the DRUJ[1]
Outcome Measures[edit | edit source]
The patient outcome can be assessed using several variables: X-rays, ROM, grip strength, pinch strength, and patient-rated functional outcome measures[4].
- Disabilities of the Arm, Shoulder (DASH) is a validated outcome measure that comprises a 30-question survey, with a lower score showing the better function.
- Michigan Hand Questionnaire (MHQ) measures outcomes using 6 scales including overall hand function, activities of daily living, pain, work performance, aesthetics, and satisfaction with hand function.
Complications[edit | edit source]
- Malunion: Malunion may occur with a residual volar displacement or shortening of the distal radius, causing a cosmetic abnormality known as a garden spade deformity. It may also narrow the entryway into the carpal tunnel, with resultant delayed carpal tunnel syndrome. Research shows a correlation between decreased bone density and trouble maintaining a closed reduction in the aged population, further increasing the risk of displacement, in spite of an appropriate immobilization procedure. In cases of resulting malunion, an osteotomy is suggested[1].
- Compression of the Median Nerve: The compression of the Median Nerve could result due to excessive flexion or extension exercises[1].
- Entrapment of the extensor pollicis longus (EPL) tendon: This is a less common complication in traumatic settings. The entrapment of the extensor pollicis longus (EPL) tendon with malunion in both conservative and ORIF surgeries. Late rupture of the EPL is also commonly cited in the literature[1].
- Complex regional pain syndrome (CRPS): reported in up to nearly 40% of fractures[1].
Treatment[edit | edit source]
Conservative[edit | edit source]
Treatment of a non-displaced and a stable Smith's fracture is by closed reduction and splint or cast. The reduction is carried out by reversing fracture deformity with longitudinal traction and applying a long arm cast with the forearm in supination and wrist in neutral or a degree of extension[5].
The closed reduction can be done under procedural sedation, hematoma block, regional nerve block, intravenous regional/Bier block, or general anesthesia. AAOS clinical guidelines suggest weekly radiographs for the first three weeks after reduction and immobilization and before the removal of splints[1]. Patients can also be treated with closed reduction and percutaneous pinning for distal radius fractures using Kirschner wires. Pinning is an efficacious, low-cost treatment option for 2- and 3-part distal radius fractures with excellent long-term outcomes, however, it is not recommended in presence of poor bone quality and multiple fragments[6]. Pinning may cause injury to the tendons, nerves, or vasculature, pin migration, fracture settling, and a pin site track infection[1].
Surgical[edit | edit source]
Indications for surgical management include[1]:
- Dorsal or volar comminution
- Intra-articular involvement
- Instability post-reduction
- Surface angulation greater than 20 degrees
- Articular surface step-off over 2 mm
- Radial shortening greater than 5 mm
Open reduction internal fixation (ORIF) is the best option for treating an unstable or not reducible fracture. According to the American Academy of Orthopaedic Surgeons (AAOS) guidelines, volar plate internal fixation is recommended as it reduces the risk of extensor tendon rupture and also preserves the blood supply of the metaphysis[1].
Pain management in the postoperative period can be managed by discussing with the operative team and primary care. Research suggests transdermal buprenorphine and codeine-acetaminophen provided superior pain control than celecoxib in the six weeks following ORIF with a volar locking plate, thus citing better compliance and faster functional recovery, however, the use of opioid analgesics should be limited outside the acute management environment[1].
Physiotherapy[edit | edit source]
Stable fractures are immobilized for 4 to 8 weeks followed by rehabilitation exercises and bracing another 4 to 6 weeks until pain-free ROM and have achieved normal strength.[1] Unstable fractures are often immobilized for 6 to 12 weeks, followed by rehabilitation for regaining motion and strength.[1]
During immobilisation[edit | edit source]
- Pain can be managed with cryotherapy and elevation.[1]
- Movement of fingers to be encouraged to maintain mobility as well as assists lymphatic drainage.
- Shoulder and elbow range of motion exercises are encouraged.
After the removal of the cast[edit | edit source]
- Heat whether in the form of a heat pack or paraffin wax can be effective to increase ROM and decrease pain. It is alternated with cold therapy to improve the venous return.
- Massage can help in reducing swelling and scar tissue mobilization.
- Hand, wrist, elbow, and shoulder exercises to increase the range of movement and strength. Mobility exercises: tearing a paper, writing, and drawing, picking small objects, typing, combing, simple tasks like buttoning a shirt. Strengthening exercises: isometrics for the wrists flexors and extensors, shoulder and elbow training, squeezing a rubber ball in the affected wrist.
Physiotherapy management is explained in the video below:
Fall prevention[edit | edit source]
Preventive measures of distal radius fractures mainly revolve around fall prevention, which is especially relevant in the elderly population[1].
AAOS 2009 Clinical Practice Guidelines recommend adjuvant treatment with vitamin D for the prevention of complex regional pain syndrome (CRPS) development following distal radius fractures (moderate level of recommendation).[1]
Prognosis[edit | edit source]
Research shows a closed reduction yields a good outcome in patients, with functional healing around six weeks. Low-level medical evidence is available for long-term outcomes of early postoperative mobilization. For athletes, stable fixation, edema management, early mobilization with rehabilitation, and functional bracing is essential for an early return to sports activity[1].
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 Schroeder JD, Varacallo M. Smith's Fracture Review. InStatPearls [Internet] 2019 Oct 1. StatPearls Publishing.
- ↑ Matsuura Y, Rokkaku T, Kuniyoshi K, Takahashi K, Suzuki T, Kanazuka A, Akasaka T, Hirosawa N, Iwase M, Yamazaki A, Orita S. Smith's fracture generally occurs after falling on the palm of the hand. Journal of Orthopaedic Research. 2017 Nov;35(11):2435-41.
- ↑ Andrew Murphy. Assoc Prof Frank Gaillard et al.Smith fracture. Radiopedia.accessed on 4/10/20https://radiopaedia.org/articles/smith-fracture
- ↑ Ikpeze TC, Smith HC, Lee DJ, Elfar JC. Distal radius fracture outcomes and rehabilitation. Geriatric orthopaedic surgery & rehabilitation. 2016 Dec;7(4):202-5.
- ↑ Emergency Care South Wales Smiths.Accessed fromhttps://www.aci.health.nsw.gov.au/networks/eci/clinical/clinical-resources/clinical-tools/orthopaedic-and-musculoskeletal/musculoskeletal-orthopaedic-guide/smiths#:~:text=Most%20commonly%20an%20extra%2Darticular,falling%20on%20a%20flexed%20wrist.on 28/10/20
- ↑ Glickel SZ, Catalano LW, Raia FJ, Barron OA, Grabow R, Chia B. Long-term outcomes of closed reduction and percutaneous pinning for the treatment of distal radius fractures. The Journal of hand surgery. 2008 Dec 1;33(10):1700-5.
- ↑ Physio VibesSMITH'S FRACTURE & PHYSIOTHERAPY MANAGEMENT. Avaialable fromhttps://www.youtube.com/watch?v=QaMoQx06yjMAccessed 26.10.20