X-Rays
Original Editor - Rachael Lowe and The Open Physio project.
Top Contributors - Rachael Lowe, Admin, Lucinda hampton, Kim Jackson, WikiSysop, Naomi O'Reilly, Claire Knott and Samuel Winter
Introduction[edit | edit source]
X-rays are a type of radiation called electromagnetic waves (with wavelengths ranging from 0.01 to 10 nanometers). X-ray imaging creates pictures of the inside of your body. The images show the parts of your body in different shades of black and white. This is because different tissues absorb different amounts of radiation. Calcium in bones absorbs x-rays the most, so bones look white. Fat and other soft tissues absorb less and look grey. Air absorbs the least, so lungs look black.
In the setting of diagnostic radiology, X-rays have long enjoyed use in the imaging of body tissues and aid in the diagnosis of disease.
- The use of radiography frequently plays a critical role in assessing the various osseous structures of the body. eg used to determine the type and extent of a fracture
- Evaluation of the lungs is also possible, and with the use of contrast can also be used to examine soft tissue organs of the body including the gastrointestinal tract and the uterus.
- Radiography is useful in performing various procedures including catheter angiography, stereotactic breast biopsies as well as intra-articular steroid injections.
- Radiography helps in the evaluation of multiple pathologies including fractures, types of pneumonia, malignancies, as well as congenital anatomic abnormalities.[1]
- Radiographic interpretation is based on the visualisation and analysis of opacities on a radiograph.
Other uses of X rays for Imaging[edit | edit source]
Fluoroscopy
Produces real-time images of internal structures of the body in a similar fashion to radiography, but employs a constant input of x-rays, at a lower dose rate to provide moving projection radiographs of lower quality. Contrast media, such as barium, iodine, and air are used to visualize internal organs as they work. Fluoroscopy is mainly performed to view movement (of tissue or a contrast agent), or to guide a medical intervention, such as angioplasty, pacemaker insertion, or joint repair/replacement. Fluoroscopy is also used in image-guided procedures when constant feedback during a procedure is required such as intra-operative and catheter guidance.
Fluoroscopy can be used to examine the digestive system using a substance which is opaque to X-rays, (usually barium sulfate or gastrografin), which is introduced into the digestive system either by swallowing or as an enema. This is normally as part of a double contrast technique, using positive and negative contrast. Barium sulfate coats the walls of the digestive tract (positive contrast), which allows the shape of the digestive tract to be outlined as white or clear on an X-ray. Air may then be introduced (negative contrast), which looks black on the film.
Angiography
The use of fluoroscopy to view the cardiovascular system. An iodine-based contrast is injected into the bloodstream and watched as it travels around. Since liquid blood and the vessels are not very dense, a contrast with high density (like the large iodine atoms) is used to view the vessels under X-ray.
Angiography is used to find aneurysms, leaks, blockages (thromboses), new vessel growth, and placement of catheters and stents. Balloon angioplasty is often done with angiography.
Dual Energy X-ray Absorptiometry (or DEXA, or bone densitometry)
Used primarily for osteoporosis tests. It is not projection radiography, as the X-rays are emitted in 2 narrow beams that are scanned across the patient, 90 degrees from each other.
Usually the hip (head of the femur), lower back (lumbar spine) or heel (calcaneum) are imaged, and the bone density (amount of calcium) is determined and given a number (a T-score). It is not used for bone imaging, as the image quality is not good enough to make an accurate diagnostic image for fractures, inflammation etc. It can also be used to measure total body fat, though this isn't common. The radiation dose received from DEXA scans is very low, much lower than projection radiography examinations[2].
Physiotherapy Use[edit | edit source]
In terms of physiotherapy, X-rays are especially useful in detecting and monitoring pathologies of the skeletal system as well as the respiratory system.
Skeletal System[edit | edit source]
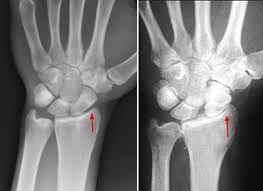
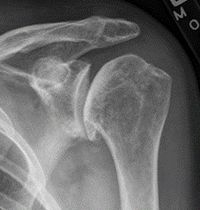
Since bone is a solid object it reflects the rays from the machine and project on the film as white in colour, one can easily identify a fracture or misalignment in the continuity of the bone. As mentioned above these images can be used for diagnostic purposes in terms of identifying the location and type of fracture and may give the clinician an idea of the prognosis of healing. The second use of X rays in the skeletal system is they may be used as a progress monitor as the clinician is able to identify which stage of healing the fracture is currently in i.e. gumming or union.
Chest X-rays[edit | edit source]
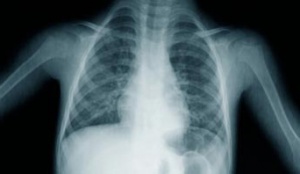
This form of radiography is commonly used to identify cardiopulmonary pathology such as Pneumothorax, Hemothorax or atelectasis in the lungs. Physiotherapist's use this form of radiography to locate areas of possible atelectasis and this allows them to focus their expansion techniques on the localized area of collapse i.e. right lingual lobe. This form of X-ray also allows the clinician to evaluate the general state of the lungs and to a lesser extent the heart.
As with skeletal X-rays, chest X-rays may be used to monitor progress during treatment as secretion accumulation, atelectasis or any other pathology in the lungs should theoretically decrease with effective treatment and this is often visible on a chest X-ray.
It is however important for the clinician to use other objective measures to monitor patient progress such as chest expansion measurements, auscultation and endurance testing as chest X rays may be contradicting or inconclusive with regards to prognosis evaluation.
Formation of Radiographs[edit | edit source]
X-ray photons have the potential to penetrate tissue and will be attenuated in part by the tissue, and in part will pass through the tissue to interact with and expose the radiographic film. Absorption of X-rays is a function of the atomic number and thickness of the tissues/objects. Tissues/objects with a higher atomic number will absorb more radiation than tissues with a lower atomic number. Thicker tissue/objects will absorb more X-rays than thinner tissue of similar composition. The greater the amount of tissue absorption, the fewer X-ray photons reach the film, and the whiter the image on the film. The radiograph will display a range of densities from white, through various shades of grey, to black. Radiopaque tissues/objects appear more white and radiolucent tissues/objects appear more black. The resultant pattern of opacities forms an image on the radiograph, which is recognisable in form, and which can be interpreted.
Radiopacity[edit | edit source]
The radiopacity of various objects and tissues results in radiographs showing different radiopacities, and hence they can be differentiated. Radiopaque tissues/objects result in a whiter image; less radiopaque objects result in a blacker image. The radiopacity depends on the atomic number (the higher the atomic number, the more radiopaque the tissue/object), physical opacity (air, fluid and soft tissue have approximately the same atomic number, but the specific gravity of air is only 0.001, whereas that of fluid and soft tissue is 1, therefore air will appear black on a radiograph, compared with fluid and soft tissue, which appear more grey), and thickness (the thicker the tissue/object, the greater the attenuation of X-Rays and the more white the image will be.
Basic Tissue Radiographic Opacities[edit | edit source]
Mineral. Bone is composed primarily of calcium and phosphorus. There is a normal variation in radiopacity within the same bone and between bones because of the difference in radiopacity of compact vs spongy bone, trabecular bone vs intertrabecular spaces and cortical bone vs medullary canal. Diseased bone may be more (sclerotic) or less (porotic) opaque than normal bone.
Soft tissue/fluid. Both soft tissues and fluids have the same radiopacity. This is the radiopacity of normal soft tissue and fluid-filled organs (heart, liver, spleen, urinary bladder). Variation in volume, thickness and degree of compactness of soft tissue creates a pattern of various densities on the radiograph
Fat. Fat is more lucent than bone or soft tissue but is more opaque than gas. Fat produces radiographic contrast for differentiation and visualisation of many organs and structures, in that fat surrounding an organ or structure will allow it to be delineated. In immature and thin animals, the lack of fat results in poorer contrast in the radiograph
Gas. Gas is the most radiolucent material visible on a film. This lucency provides contrast to allow visualisation of various structures, e.g. the heart and great vessels outlined against the air-filled lungs in the chest.
Metal. This is the most opaque shadow seen on radiographs, and may be seen as contrast media (barium, water-soluble iodine), orthopaedic implants, metallic foreign bodies.
Only these five radiographic opacities are visible on a radiograph, however, there is some variation in opacity within each group.
Potential areas for film and/or processing errors[edit | edit source]
- Heel effect – a source of visual error related to x-ray production, due to the fact that x-rays released by the machine are not uniform. There are two ends to an x-ray machine, a cathode end and anode end. The cathode end releases more photons than the anode end, which results in over-exposure of the film at the cathode end and under-exposure at the anode end. Due to this fact, technicians will position the patient on the table in a manner such that the thickest portion of the body region being studied is placed nearest the cathode end of the tube and the thinner end is placed near the anode end.
- Artefact – An error in the perception of the visual image of the radiograph, usually seen as an abnormal finding or foreign body. Artifacts occur when the cassettes that house the x-ray film plates get exposed to finger prints or small debris.
- Exposure – A measure of the amount of ionising radiation determined by 3 factors: time, x-ray energy, and the quantity of the x-ray photons. Exposure can be manipulated by the technician to highlight structures of interest. Over-penetration will tend to enhance bone visibility, while under-penetration will enhance soft tissue visibility.
- Movement – A blurring in the image as a result of movement by the patient the moment the x-ray exposure is made.
- Film processing – An error that occurs during the processing of the film can result in disturbances in the contrast, detail, or density of the image displayed.
- Radiodensity is a representation of the relative tissue density, based on the appearance of the tone of the tissue (white, gray, or black). The following structures may be found on a medical radiograph (in order of increasing radiodensity)
- Air – black appearance, often seen in structures such as the lungs, bowels, trachea
- Fat – dark grey appearance, often seen in structures such as thicker adipose tissue
- Muscle, tendon, organ tissue – appears “neutral” or mid-grey
- Bone – cancellous bone appears as light grey, while cortical bone appears as white
- Contrast media - white appearance
- Metal – white appearance, often seen in structures such as jewellery, dental fillings, or orthopaedic hardware
Caution to the radiograph viewer/interpreter – There is an inherent error that occurs when a 2-dimensional image is created to depict 3-dimensional structures that are often superimposed on one-another. Due to this fact, radiographic studies of specific body regions often include 3 or more views from different angles.[3]
Four principle sources of radiographic error
- Enlargement occurs because the x-ray beams exit the machine in an expanding conical pattern (similar to a flashlight beam). As a result, objects placed closer to the beam source appear larger than objects placed further away from the beam source.
- Elongation is produced by the increased beam angle at the periphery of the x-ray beam cone. As a result of the increased beam angle, objects in the periphery of the x-ray beam appear smeared or spread compared to objects in the centre of the beam.
- Foreshortening is the opposite effect of elongation. This occurs when the body region to be studied is placed at an angle to the primary x-ray beam, resulting in the appearance of decreased length.
- Superimposition occurs because anatomic structures are often stacked on one another, forcing the x-ray beam to penetrate multiple structures before arriving at the film plate. Superimposition can create the appearance of increased density of structures, or the appearance of novel structures altogether.[3]
Resources[edit | edit source]
The Norwich Image Interpretation Course. This is a great free online course on x-ray interpretation by Heidi Gable DCR(R) PgCert from the Norfolk & Norwich University Hospital NHS Trust.
References[edit | edit source]
- ↑ Tafti D, Maani CV. Radiation X-ray Production 24.9.2019.Available from:https://www.ncbi.nlm.nih.gov/books/NBK537046/
- ↑ Swain J, Bush K. Diagnostic Imaging for Physical Therapists. St. Louis: Saunders Elsevier; 2009
- ↑ 3.0 3.1 Biederman, R. E., Wilmarth, M. A., & Editor, C. M. D. T. (n.d.). Diagnostic Imaging in Physical Therapy Avoiding the Pitfalls. Diagnostic Imaging.