Splinting for Burns
Original Editor - Kirenga Bamurange Liliane
Top Contributors - Kirenga Bamurange Liliane, Naomi O'Reilly, Simisola Ajeyalemi, Kim Jackson, Vidya Acharya and Wanda van NiekerkDescription[edit | edit source]
A burn is an injury to the skin or other organic tissue primarily caused by heat or due to radiation, radioactivity, electricity, friction, or contact with chemicals [1]. Most burns are due to heat from hot liquids (called scalding), solids, or fire. A splint is a rigid support made from metal, plaster, or plastic. It's used to protect, support, or immobilize an injured or inflamed part of the body.
Positioning and Splinting[edit | edit source]
It is imperative that a burn patient be positioned and splinted as soon as the injury occurs for the best functional outcomes of his rehabilitation. Therefore, positioning and splinting should:
- Minimize edema formation
- Prevent tissue destruction
- Maintain soft tissue in an elongated state to facilitate recovery
- Adopt the anticontracture position
Physical therapy and splinting should immediately after the injury as they play an important role in different body parts function, especially in hand function [2].
Areas at High Risk for Contracture[edit | edit source]
- Neck
- Axilla
- Hand
Indication for Splint Use[edit | edit source]
Splints are generally used for:
- Prevention of contractures
- Protection of a joint or tendon
- Immobilization following a skin graft
- Decreased Range of Motion (ROM)
- Maintenance of ROM obtained while exercising or during a surgical release
- Poor patient compliance
For patients with burns injury, splints are used to hold parts of the body so that:
- The skin graft can be immobilized and protected while healing
- The skin can be prevented from shrinkage and contractures while healing
- The new grafts and flaps are protected
- The deformity is prevented and/or corrected
- The ROM is maintained and/or increased
- The weak muscles can counteract the effect of gravity [3]
Different Types of Splints[edit | edit source]
There are 3 types of splints usually used with burn patients namely static, static progressive, and dynamic splints [4].
- Static or Primary splints are used in the acute phase for skin graft protection after surgery or anticontracture positioning. These splints are applied to adjacent intact skin.
- Static progressive or postural splints are used after the graft phase when there is no sufficient ROM obtained with static positioning and exercise. These splints may be implemented for correction and contractures.
- Dynamic or follow-up splints are used to increase function by providing a slow force to stretch a contracture or provide resistive force for exercise
Clinical Presentation[edit | edit source]
Splints may be used to immobilize injuries such as sprains or fractures, or soft tissue injuries. They may also be used as definitive management to treat these injuries. In some cases, Educating patients regarding splint care and return precautions aids in a successful outcome [5].
Different splints used for different body parts[edit | edit source]
| Body Part and purpose | Type of Splint |
|---|---|
| Anterior Neck Burns | Halo neck splint that positions the neck in extension using the head and upper torso for stabilization |
| Neck Contractures | Neck Willis applied directly over the burn wound or over a single layer of gauze |
| Neck Contractures | Watusi Collar ( a series of cylindrical plastic foam tubes fastened circumferentially around the neck) |
| Chest | Back brace or Spinal support |
| Shoulder or Axilla | Airplane or axillary splint |
| Finger | Finger extension splint or a thumb spacer |
| Mouth | Mouth splint to keep the skin from shrinking around during the healing process and restore motion of the shoulder |
| Hand | Hand splint |
| Wrist | Wrist splint or wrist orthosis |
| Elbow | Elbow splint |
| Hip | Anterior hip spica splint |
| Knee | Common knee splints are: Gutter or/trough splint; knee comforter |
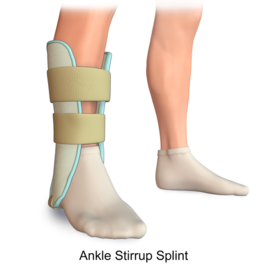
| Ankle and foot | Posterior foot splint; anterior ankle comforter and toe comforter |
Table adapted from [2]
Splinting and Positioning Goals for Rehabilitation[edit | edit source]
| Phase of rehabilitation | Goal |
|---|---|
| Acute | Edema control and pressure relief |
| Intermediate | Tisue elongation and graft protection |
| Long term | Tissue elongation |
Table 1 from here [4]
Combining splinting and positioning is among the most effective methods by which a physical therapist can help an acute burn patient to achieve mobility and independence.
Contra-indications for Splinting[edit | edit source]
- Compartment Syndrome
- Need for an open reduction
- The skin at high risk for infection
References[edit | edit source]
- ↑ Burns. Available from: https://www.who.int/violence_injury_prevention/other_injury/burns/en/ (Accessed 29 November 2020)
- ↑ 2.0 2.1 Rrecaj S, Hysenaj H, Martinaj M, Murtezani A, Ibrahimi-Kacuri D, Haxhiu B, Buja Z. Outcome of Physical Therapy and Splinting in hand burns injury. Our last four years experience. Materio socio-media. 2015 Dec; 27(6): 380-382.
- ↑ Splints for burns. Available from: https://www.healthpartners.com/hospitals/regions/specialties/burn-center/splints/#:~:text=Splints%20for%20burns,-Overview&text=Splints%20or%20orthoses%20are%20used,with%20a%20low%20temperature%20thermoplastic (Accessed 27 November 2020)
- ↑ 4.0 4.1 Dewey WS, Richard RL, Parry IS. Positioning, Splinting, and Contracture Management. Physical Medicine and Rehabilitation Clinics of North America. 2011 May 1;22(2):229-47.
- ↑ Althoff AD, Reeves RA. Splinting. StatPearls [Internet]. 2020 May 24.
- ↑ University of Iowa Health Care. Burn Unit Series- " Stretching, Scar Management, and Compression" (UI Health Care). Available from: https://www.youtube.com/watch?v=da389tmq62g [last accessed 5/1/2021]
- ↑ UW Surgery. Burns 401: Axillary Splints. Available from: https://www.youtube.com/watch?v=QpQHpW9JK4w [last accessed 5/1/2021]