Therapeutic Alliance
Original Editor - Laura Ritchie, posting on behalf of Wei Seah, MPT Class of 2017 at Western University, a project for PT9584.
Top Contributors - Laura Ritchie, Ewa Jaraczewska, Kim Jackson, Mandy Roscher, Wanda van Niekerk, Naomi O'Reilly, Jess Bell, Robin Tacchetti, Evan Thomas and Vidya Acharya
Introduction[edit | edit source]
The therapeutic alliance, also referred to as the working alliance, is a description of the interaction between the health care professional and their patients. The therapeutic alliance is considered an important aspect of the therapeutic process and can have an impact on treatment outcomes.[1] By establishing a therapeutic alliance, the therapist seeks to provide patient-centred care, in which the therapist is seen as a facilitator for the patient to achieve their goals, rather than an authority figure.[2] Previous research has highlighted the importance of providing patient-centred care not only in physiotherapy but in other medical and rehabilitation professions as well.[3] This is accomplished by encouraging the patient to become more active in their treatment to engage them in a collaborative, active approach to recovery.[4] With a strong therapeutic alliance and encouraging patient participation, therapists can also address psychosocial aspects of pain,[5] which are often overlooked in traditional unidirectional patient-therapist interactions. This is especially important as recent research supports that physical treatment alone cannot fully account for the improvement of patient outcomes.[6]
Background[edit | edit source]
The therapeutic alliance was first described by Freud in 1912.[7] He outlined the concepts of transference and countertransference, which are the unconscious feelings or emotions that a patient feels towards their therapist, and vice-versa.[7] Further research by Rogers (1951)[8] was the first to highlight empathy as a core characteristic of this therapeutic alliance. Anderson et al.(1962)[9] conceptualised both empathy and rapport as qualities within the “therapeutic bond”.[8] [9] Hougaard (1994)[10] consolidated previous data into a conceptual structure composed of two branches, the personal relationship area and the collaborative area.[10] The personal relationship area focuses on the socio-emotional aspect of the therapist-patient relationship. The collaborative relationship area consists of more task-related aspects, such as goal-setting and treatment planning. It was Martin, Garske and Davis (2000)[11] who concretely described the therapeutic alliance as “…the collaborative and affective bond between therapist and patient – is an essential element of the therapeutic process.”[11]
Components of a Therapeutic Alliance[edit | edit source]
Bordin[12] describes the 3 components that contribute to a strong therapeutic alliance:
- Agreement on goals (Collaborative Goal Setting)
- Agreement on interventions (Shared Decision Making)
- Effective bond between patient and therapist (The Therapeutic Relationship)
Collaborative Goal Setting[edit | edit source]
Goal setting serves a fundamental role in guiding rehabilitation so that a specific outcome is reached. Setting SMART (Specific, Measurable, Attainable, Relevant and Time Limited) goals is a useful way to ensure goals are successful.
The agreement of goals between the patient and the therapist increases adherence to those goals. Adherence in turn leads to improved outcomes,[13] improved patient satisfaction and motivation. All of these factors positively influence the therapeutic alliance.[13] When patients are excluded from this process and goals are simply set for them, it creates a situation of dissatisfaction which will negatively influence the therapeutic alliance.[13]
[edit | edit source]
Shared decisions help to strengthen the therapeutic alliance.[13] It is a process of providing the patient with information and supporting them through the decision-making process.[14]
A process for shared decision making is outlined by Elwyn et al.[14] whereby you move through a 3 step approach:
- Choice Talk
- Step back
- Offer choice
- Justify choice - consider preferences
- Check reaction
- Defer closure
- Option Talk
- Check knowledge
- List options
- Describe options - explore preferences
- Harms and benefits
- Provide patient decision support
- Summarise
- Decision Talk
- Focus on preferences
- Elicit preferences
- Move to a decision
- Offer review
The Therapeutic Relationship[edit | edit source]
The therapeutic relationship refers to the professional bond between the therapist and patient.[15] It is the key component of a strong therapeutic alliance.
The following components contribute to the development of a strong therapeutic relationship:[13]
- Communication Skill
- Active listening
- Empathy
- Friendliness
- Encouragement
- Confidence
- Non-verbal communication
- Practical Skills
- Patient education that is simple and clear
- Therapist expertise and training
- Patient-Centred Care
- Individualised treatments
- Taking patients' opinions and preferences into consideration
- Organisational and Environmental Factors
- Giving patients enough time for thorough assessment and management
- Flexibility with patient appointments and care
Patient-Centred Care[edit | edit source]
Patient-centredness has been defined as “Health care that establishes a partnership among practitioners, patients, and their families…to ensure that decisions respect patients’ wants, needs, and preferences and that patients have the education and support they need to make decisions and participate in their own care."[16] Essentially, patient-centred care is care that ensures the patients' needs, values and preferences guide all clinical decisions. [17]
Good communication skills are an integral tool for achieving a strong therapeutic alliance and research has shown that effective communication also leads to increased patient adherence and satisfaction.[18] Mead and Bower[3] identified five key dimensions of patient-centred care which have been associated with a positive therapeutic alliance:[19]
- Utilising a biopsychosocial perspective
- The ‘patient-as-person'
- Sharing power and responsibility
- The therapeutic alliance
- The ‘doctor-as-person’
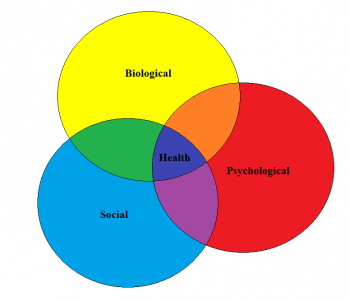
Utilising a biopsychosocial perspective[edit | edit source]
The traditional premise of the biopsychosocial model is that a patient's disease cannot be separated from their physosocial causes, personality or surroundings.[20] In recent years, scholars and clinicians have added in additional factors such as spiritual, economical, cultural and political. [21]. In health care, the biopyschosocial model provides the clinician with a better understanding of the components responsible the disease while educating the patient on how to adjust their lifestyles to have a better quality of life.[22]
Several conditions treated by physiotherapists appear to have little relation to structural or physiological changes, which can themselves be interpreted with high variability.[23] [24] [25] Thus, an approach that considers not only biological but also psychological and sociological factors is needed to appreciate the full scope of the problems presented and provide patient-centred care. [26]
The 'patient-as-person'[edit | edit source]
Although the biopsychosocial model seeks to address all of the factors surrounding the patient, it may not be sufficient to fully appreciate the patient experience.[27] We need to understand that each patient may perceive the same pain experience differently. Eliciting the individual patient’s fears, expectations and feelings of illness should be one of our primary concerns.[28]
Sharing power and responsibility[edit | edit source]
The patient-practitioner relationship has always been fundamentally seen as a ‘paternalistic’ relationship, which some see as inevitable due to the competence gap between the two parties.[29] By shifting patients from ‘consumers’ to active ‘participants’, we can help place patients in control of their own illness, which has been correlated with better health outcomes.[30]
The therapeutic alliance[edit | edit source]
Just as patient-centred care can strengthen the therapeutic alliance, a reciprocal relationship can also occur. As mentioned above, Bordin[12] described the three main components of the therapeutic alliance as 1) agreement on goals, 2) agreement on interventions, and 3) an effective bond between patient and therapist.[12]
The ‘doctor-as-person’[edit | edit source]
Since both the therapeutic alliance and patient-centred care acknowledge the relationship between therapist and patient, it is logical to place importance on the qualities of the therapist. The interaction between therapist and patient is constant, and the subjectivity of the therapist is something that cannot be separated from this interaction.[31]
Effect on Patient Outcomes[edit | edit source]
The therapeutic alliance has previously been shown to improve patient outcomes in both medicine and psychology.[32] [33] [34] [35] It is only recently that its effects on other rehabilitative sciences have been investigated. In 2007, Burns and Evon[36] studied its effect on cardiac rehabilitation. They found that increased self-efficacy is not enough on its own to predict increased cardiorespiratory fitness, weight reduction and return to work.[36] Instead, it must be combined with a strong therapeutic alliance to achieve these outcomes. A poor therapeutic alliance can undermine the potential for improvement. In 2012, Ferreira and colleagues[37] examined the relationship between the therapeutic alliance and patient outcomes in the rehabilitation of patients with chronic low back pain.[37] They found that a strong therapeutic alliance leads to increased perceived changes following a variety of conservative treatments. Interestingly, a strong therapeutic alliance was associated with improved disability and function outcome measures, but no pain. Fuentes et al.[38] also conducted a study on patients with low back pain, this time measuring the therapeutic alliance’s effect on pain intensity and muscle pain sensitivity.[38] They found that a strong therapeutic alliance can significantly modify perceived pain intensity after interferential current therapy (IFC). Another point of interest from this study is that active IFC with a limited therapeutic alliance was not statistically different from sham IFC with a strong therapeutic alliance.[38]
A systematic review of the impact of the therapeutic alliance for chronic musculoskeletal pain found that the therapeutic alliance has a significant impact on patient outcomes.[39] The authors of this review recommend communication training in health care professionals as a way of improving the therapeutic alliance and encouraging patient-therapist collaboration in treatment decisions.[39]
Measuring the Therapeutic Alliance[edit | edit source]
Popular outcome measures for the therapeutic alliance include the Working Alliance Theory of Change Inventory (WATOCI), which itself is derived from the Working Alliance Inventory.[40] Hall et al.[41] found that there was some room for improvement in the WATOCI, specifically relating to the wording in certain sections.[41] The nine remaining items were found to be a uni-dimensional tool for measuring the therapeutic alliance, despite demonstrating a ceiling effect. Due to the complexity of the therapeutic alliance, it may be difficult to find a perfect measurement. However, patient-administered outcomes are a step in the right direction as the patient perception of the therapeutic alliance has been found to be a better predictor of outcome than therapist perception.[42]
References[edit | edit source]
- ↑ Babatunde F, MacDermid J, MacIntyre N. Characteristics of therapeutic alliance in musculoskeletal physiotherapy and occupational therapy practice: a scoping review of the literature. BMC Health Serv Res. 2017;17(1):375.
- ↑ Walton D, Dhir J, Millard J. Introduction and Application of the CARE Model in Physiotherapy Practice. Presentation presented at; 2016; London, Ontario, Canada
- ↑ 3.0 3.1 Mead N, Bower P. Patient-centredness: a conceptual framework and review of the empirical literature. Social Science and Medicine. 2000;51(7):1087-1110.
- ↑ Epstein R, Street R. The Values and Value of Patient-Centered Care. The Annals of Family Medicine. 2011;9(2):100-103
- ↑ Gatchel R, Peng Y, Peters M, Fuchs P, Turk D. The biopsychosocial approach to chronic pain: Scientific advances and future directions. Psychological Bulletin. 2007;133(4):581-624.
- ↑ Ambady N, Koo J, Rosenthal R, Winograd C. Physical therapists' nonverbal communication predicts geriatric patients' health outcomes. Psychology and Aging. 2002;17(3):443-452.
- ↑ 7.0 7.1 Freud S. The Dynamics of Transference. The Standard Edition of the Complete Psychological Works of Sigmund Freud. 1912; XII (1911-1913):97-108.
- ↑ 8.0 8.1 Rogers C. Client-centered therapy. 1st ed. Boston: Houghton Mifflin; 1951
- ↑ 9.0 9.1 Anderson R, Anderson G. Development of an instrument for measuring rapport. The Personnel and Guidance Journal. 1962;41(1):18-24
- ↑ 10.0 10.1 Hougaard E. The therapeutic alliance–A conceptual analysis. Scandinavian Journal of Psychology. 1994;35(1):67-85.
- ↑ 11.0 11.1 Martin D, Garske J, Davis M. Relation of the therapeutic alliance with outcome and other variables: A meta-analytic review. Journal of Consulting and Clinical Psychology. 2000;68(3):438-450
- ↑ 12.0 12.1 12.2 Bordin E. The generalizability of the psychoanalytic concept of the working alliance. Psychotherapy: Theory, Research and Practice. 1979;16(3):252-260
- ↑ 13.0 13.1 13.2 13.3 13.4 O'keeffe M, Cullinane P, Hurley J, Leahy I, Bunzli S, O'Sullivan PB, O'Sullivan K. What influences patient-therapist interactions in musculoskeletal physical therapy? Qualitative systematic review and meta-synthesis. Physical therapy. 2016 May 1;96(5):609-22.
- ↑ 14.0 14.1 Elwyn G, Frosch D, Thomson R, Joseph-Williams N, Lloyd A, Kinnersley P, Cording E, Tomson D, Dodd C, Rollnick S, Edwards A. Shared decision making: a model for clinical practice. Journal of general internal medicine. 2012 Oct 1;27(10):1361-7
- ↑ Miciak M, Mayan M, Brown C, Joyce AS, Gross DP. The necessary conditions of engagement for the therapeutic relationship in physiotherapy: an interpretive description study. Arch Physiother. 2018;8:3.
- ↑ Edgman-Levitan S, Schoenbaum SC. Patient-centered care: achieving higher quality by designing care through the patient’s eyes. Israel Journal of Health Policy Research. 2021 Dec;10(1):1-5.
- ↑ Hower KI, Vennedey V, Hillen HA, Kuntz L, Stock S, Pfaff H, Ansmann L. Implementation of patient-centred care: which organisational determinants matter from decision maker’s perspective? Results from a qualitative interview study across various health and social care organisations. BMJ open. 2019 Jun 1;9(4):e027591.
- ↑ Gyllensten A, Gard G, Salford E, Ekdahl C. Interaction between patient and physiotherapist: a qualitative study reflecting the physiotherapist's perspective. Physiotherapy Research International. 1999;4(2):89-109.
- ↑ Pinto R, Ferreira M, Oliveira V, Franco M, Adams R, Maher C et al. Patient-centred communication is associated with positive therapeutic alliance: a systematic review. Journal of Physiotherapy. 2012;58(2):77-87.
- ↑ Xiao X, Song H, Sang T, Wu Z, Xie Y, Yang Q. Analysis of Real-World Implementation of the Biopsychosocial Approach to Healthcare: Evidence From a Combination of Qualitative and Quantitative Methods. Frontiers in Psychiatry. 2021;12.
- ↑ Ventres WB, Frankel RM. Personalizing the BioPsychoSocial Approach:“Add-Ons” and “Add-Ins” in Generalist Practice. Frontiers in Psychiatry. 2021;12.
- ↑ Syed S, Bhardwaj SS. The role of the bio-psychosocial model in public health. The Journal of Medical Research. 2020;6(5):252-4.
- ↑ Rogers A, Nicolaas G, Hassell K. Demanding patients?. 1st ed. Buckingham [etc.]: Open University Press; 1999
- ↑ Deyo R, Weinstein J. Low Back Pain. New England Journal of Medicine. 2001;344(5):363-370
- ↑ Herzog R, Elgort D, Flanders A, Moley P. Variability in diagnostic error rates of 10 MRI centres performing lumbar spine MRI examinations on the same patient within a 3-week period. The Spine Journal. 2017;17(4):554-561
- ↑ Silverman D. Communication and medical practice. 1st ed. Inglaterra: Sage Publications; 1987.
- ↑ Armstrong D. The emancipation of biographical medicine. Social Science and Medicine Part A: Medical Psychology and Medical Sociology. 1979;13:1-8
- ↑ Levenstein J, McCracken E, McWhinney I, Stewart M, Brown J. The Patient-Centred Clinical Method. 1. A Model for the Doctor-Patient Interaction in Family Medicine. Family Practice. 1986;3(1):24-30
- ↑ Parsons T, Smelser N. The social system. 1st ed. New Orleans, La.: Quid Pro Books; 2012
- ↑ Kaplan S, Greenfield S, Ware J. Assessing the Effects of Physician-Patient Interactions on the Outcomes of Chronic Disease. Medical Care. 1989;27(Supplement):S110-S127
- ↑ Balint E., Courtenay M., Elder A., Hull S., Julian P. The doctor, the patient and the group: Balint re-visited. 1st ed. London: Routledge; 1993
- ↑ Kao A, Green D, Davis N, Koplan J, Cleary P. Patients’ trust in their physicians. Journal of General Internal Medicine. 1998;13(10):681-686
- ↑ Bachelor A. Comparison and relationship to outcome of diverse dimensions of the helping alliance as seen by client and therapist. Psychotherapy: Theory, Research, Practice, Training. 1991;28(4):534-549
- ↑ Barber J, Connolly M, Crits-Christoph P, Gladis L, Siqueland L. Alliance predicts patients' outcome beyond in-treatment change in symptoms. Journal of Consulting and Clinical Psychology. 2000;68(6):1027-1032
- ↑ Gaston L, Piper W, Debbane E, Bienvenu J, Garant J. Alliance and Technique for Predicting Outcome in Short-and Long-Term Analytic Psychotherapy. Psychotherapy Research. 1994;4(2):121-135
- ↑ 36.0 36.1 Burns J, Evon D. Common and specific process factors in cardiac rehabilitation: Independent and interactive effects of the working alliance and self-efficacy. Health Psychology. 2007;26(6):684-692
- ↑ 37.0 37.1 Ferreira P, Ferreira M, Maher C, Refshauge K, Latimer J, Adams R. The Therapeutic Alliance Between Clinicians and Patients Predicts Outcome in Chronic Low Back Pain. Physical Therapy. 2012;93(4):470-478
- ↑ 38.0 38.1 38.2 Fuentes J, Armijo-Olivo S, Funabashi M, et al. Enhanced therapeutic alliance modulates pain intensity and muscle pain sensitivity in patients with chronic low back pain: an experimental controlled study. Phys Ther. 2013;94:477-489
- ↑ 39.0 39.1 Kinney M, Seider J, Beaty AF, Coughlin K, Dyal M, Clewley D. The impact of therapeutic alliance in physical therapy for chronic musculoskeletal pain: A systematic review of the literature. Physiotherapy theory and practice. 2018 Sep 24:1-3
- ↑ Horvath A, Greenberg L. Development and validation of the Working Alliance Inventory. Journal of Counseling Psychology. 1989;36(2):223-233
- ↑ 41.0 41.1 Hall A, Ferreira M, Clemson L, Ferreira P, Latimer J, Maher C. Assessment of the therapeutic alliance in physical rehabilitation: a RASCH analysis. Disability and Rehabilitation. 2011;34(3):257-266
- ↑ Castonguay L, Constantino M, Holtforth M. The working alliance: Where are we and where should we go?. Psychotherapy: Theory, Research, Practice, Training. 2006;43(3):271-279