Total Hip Replacement Dislocation: Difference between revisions
No edit summary |
No edit summary |
||
| Line 33: | Line 33: | ||
Treatment is closed reduction of the hip. Surgical management with possible revision THA is advisable for irreducible dislocations, recurrent instability, and implant malposition.<ref name=":0" /> | Treatment is closed reduction of the hip. Surgical management with possible revision THA is advisable for irreducible dislocations, recurrent instability, and implant malposition.<ref name=":0" /> | ||
Roughly 66% of cases are successfully treated; one third of cases will require surgical treatment (including revision arthroplasty with use of constrained liners, elevated rim liners or dual mobility implants or trochanteric advancement)<ref name=":2">Lu Y, Xiao H, Xue F. [https://pubmed.ncbi.nlm.nih.gov/31410129/ Causes of and treatment options for dislocation following total hip arthroplasty.] Experimental and Therapeutic Medicine. 2019 Sep 1;18(3):1715-22.Available:https://pubmed.ncbi.nlm.nih.gov/31410129/ (accessed 7.1.2023)</ref>. | Treatment of recurrent hip dislocation starts looking for the cause. | ||
* Component position needs careful evaluated, as does hip offset and leg length. | |||
* When planning a reconstruction, it is generally not a good idea to compensate for malposition of one component by overcorrecting the other. | |||
* Patients needs to be informed that stability may require lengthening of the leg.<ref>Brooks PJ. [https://online.boneandjoint.org.uk/doi/full/10.1302/0301-620X.95B11.32645 Dislocation following total hip replacement: causes and cures]. The bone & joint journal. 2013 Nov;95(11_Supple_A):67-9. Available:https://online.boneandjoint.org.uk/doi/full/10.1302/0301-620X.95B11.32645 (accessed 7.1.2023)</ref> | |||
Roughly 66% of cases are successfully treated; one third of cases will require surgical treatment (including revision arthroplasty with use of constrained liners, elevated rim liners or dual mobility implants or trochanteric advancement)<ref name=":2">Lu Y, Xiao H, Xue F. [https://pubmed.ncbi.nlm.nih.gov/31410129/ Causes of and treatment options for dislocation following total hip arthroplasty.] Experimental and Therapeutic Medicine. 2019 Sep 1;18(3):1715-22.Available:https://pubmed.ncbi.nlm.nih.gov/31410129/ (accessed 7.1.2023)</ref> | |||
Surgical options include exchange of modular components to increase soft-tissue tension, or a switch to a larger head diameter, including bipolar or tripolar arthroplasty, and use of an acetabular lip. Malposition and impingement must be corrected. Soft-tissue or trochanteric advancement, and the use of constrained liners should be a last resort.<ref name=":2" /> | |||
== Physiotherapy == | == Physiotherapy == | ||
Revision as of 08:07, 7 January 2023
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
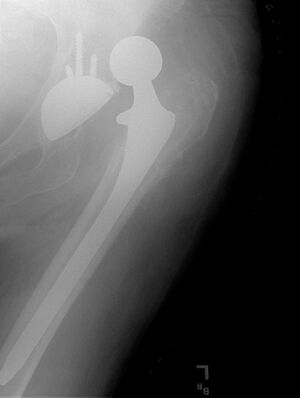
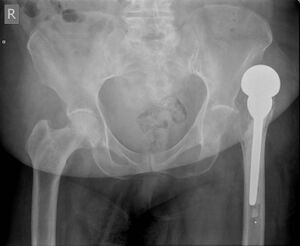
Total hip replacement (THR) dislocation is a complication of THR usually occurring due to patient noncomplicance with post-operative precautions, implant malposition, or soft-tissue deficiency. This type of dislocation normally caused by minimal trauma, usually falls or turning, moving into the contra-indicated positions, and putting stress on the capsule that was incised for the replacement surgery.[1][2]
Epidemiology[edit | edit source]
Incidence: 1-3% with 70% occur within first month and 75-90% being posterior dislocations.[2]
Risk Factors[edit | edit source]
Following a THR the normal hip anatomy and support structures is altered. This violation may cause a decrease in the amount of inherent/anatomic force that assists in maintaining the femoral head within the acetabulum. Consequently the amount of energy necessary for a dislocation to occur is reduced. Significant risk factors mechanically predisposing individuals with THRs to dislocation include:
- Surgical approach used, for example, anterior or posterior
- King of prosthesis (hemi or total arthroplasty)
- Previous hip surgery
- Female
- Malposition of the prosthesis during surgery
- Drug/alcohol abuse
- Neuromuscular disease for example Parkinson, Demetia. [3]
- Polyethylene wear, a common cause of late instability occurring >5 years after surgery.[2]
Presentation[edit | edit source]
Typically the dislocation include falls, bending down to tie one's shoes, sitting on a low/short chair then trying to stand, or sitting, standing, or lying down with crossed legs.[3] eg After a fall patient presents with a painful affected hip and shortened and internally rotated affected leg.[4]
Diagnosis[edit | edit source]
Diagnosis is with plain x-rays of the hip. CT of the pelvis assists with assessing for implant malpositioning.[2]
Treatment[edit | edit source]
Treatment is closed reduction of the hip. Surgical management with possible revision THA is advisable for irreducible dislocations, recurrent instability, and implant malposition.[2]
Treatment of recurrent hip dislocation starts looking for the cause.
- Component position needs careful evaluated, as does hip offset and leg length.
- When planning a reconstruction, it is generally not a good idea to compensate for malposition of one component by overcorrecting the other.
- Patients needs to be informed that stability may require lengthening of the leg.[5]
Roughly 66% of cases are successfully treated; one third of cases will require surgical treatment (including revision arthroplasty with use of constrained liners, elevated rim liners or dual mobility implants or trochanteric advancement)[6]
Surgical options include exchange of modular components to increase soft-tissue tension, or a switch to a larger head diameter, including bipolar or tripolar arthroplasty, and use of an acetabular lip. Malposition and impingement must be corrected. Soft-tissue or trochanteric advancement, and the use of constrained liners should be a last resort.[6]
Physiotherapy[edit | edit source]
This follows the same protocol as Total Hip Surgery (see link). Be aware however that the surgeon may have specific advice to follow, especially as this is a more complex procedure. The total rehabilitation phase in hospital and home may also be longer due to more extensive damage and repair.
References[edit | edit source]
- ↑ Radiopedia Hip dislocation Availablehttps://radiopaedia.org/articles/hip-dislocation (accessed 7.1.2023)
- ↑ 2.0 2.1 2.2 2.3 2.4 Orthobullets THA Dislocation Available:https:https://www.orthobullets.com/recon/5012/tha-dislocation (accessed 7.1.2023)
- ↑ 3.0 3.1 Masiewicz S, Mabrouk A, Johnson DE. Posterior hip dislocation.Available:https://www.ncbi.nlm.nih.gov/books/NBK459319/ (accessed 7.1.2023)
- ↑ Radiopedia Dislocated hip prosthesis Available: https://radiopaedia.org/cases/dislocated-hip-prosthesis?lang=gb (accessed 7.1.2023)
- ↑ Brooks PJ. Dislocation following total hip replacement: causes and cures. The bone & joint journal. 2013 Nov;95(11_Supple_A):67-9. Available:https://online.boneandjoint.org.uk/doi/full/10.1302/0301-620X.95B11.32645 (accessed 7.1.2023)
- ↑ 6.0 6.1 Lu Y, Xiao H, Xue F. Causes of and treatment options for dislocation following total hip arthroplasty. Experimental and Therapeutic Medicine. 2019 Sep 1;18(3):1715-22.Available:https://pubmed.ncbi.nlm.nih.gov/31410129/ (accessed 7.1.2023)