Tibial Spine Fracture and Physical Therapy Protocol: Difference between revisions
Ruchi Desai (talk | contribs) No edit summary |
Mohit Chand (talk | contribs) No edit summary |
||
| (13 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
'''Original Editor '''- [[User:Ruchi Desai|Ruchi Desai]] | |||
'''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | |||
Tibial spine | == Introduction == | ||
Tibial spine fractures are uncommon injuries that occur when the bony projection on the tibia, known as the tibial spine, is subjected to significant trauma. These fractures often result from high-energy events such as motor vehicle accidents, falls, or sports-related injuries. The severity can range from non-displaced to displaced fractures, which poses a greater risk of complications if not managed properly. Understanding the relevant anatomy, pathogenesis, diagnosis, management, and rehabilitation strategies is crucial for achieving favorable patient outcomes. | |||
1) | === '''Clinically Relevant Anatomy''' === | ||
The lower leg is made up of two bones: the [[Tibia|tibia and fibula.]] The tibia is the larger of the two [[Bone|bones]]. It supports most of your weight and is an essential part of both the [[knee]] joint and ankle joint. The tibial spine is a specialized ridge of bone in the tibia where the anterior cruciate ligament ([[Anterior Cruciate Ligament (ACL) Reconstruction|ACL]]) attaches. This ligament is integral maintaining flexibility and stability in the knee. | |||
Tibial spine fracture (also called Tibial Eminence Fracture) is a break at the top of the tibia bone in the lower leg near the knee as a result of high amounts of tension placed upon the Anterior cruciate ligament ([[Anterior Cruciate Ligament (ACL) Reconstruction|ACL]]). This type of injury is most common in | |||
1) Children ages 8 to 14 years of age<ref>GronkvistHFracture of the anterior tibial spine in children. J Pediatr Orthop, 19844465468</ref>.<ref>eyersM. HMckeeverF. MFracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am 19705216771683</ref> | |||
2) The incidence of these fractures is higher among adolescent girls due to their inherent skeletal immaturity. | 2) The incidence of these fractures is higher among adolescent girls due to their inherent skeletal immaturity. | ||
| Line 13: | Line 18: | ||
4) It can occur during a sporting event or direct trauma with a hyperextension injury causes an avulsion fracture occurring at the tibial eminence while the ACL is spared. | 4) It can occur during a sporting event or direct trauma with a hyperextension injury causes an avulsion fracture occurring at the tibial eminence while the ACL is spared. | ||
Here is a video for better understanding: | |||
{{#ev:youtube| Kt_iAsqns8A|300}}<ref>Dr. David Geier. Tibial spine fracture: What is this knee injury, and how can you get better?: https://www.youtube.com/watch?v=Kt_iAsqns8A [last accessed 19/6/2024]</ref> | |||
=== Mechanism of Injury / Pathological Process === | === Mechanism of Injury / Pathological Process === | ||
Tibial spine fractures are typically caused by the stress from a high-intensity activity, a hard impact to the bone, or from an already compromised or weakened bone. Usually younger people will get a tibial spine fracture from a hard impact injury, such as a fall from a height or a sports-related injury. Older people tend to get a tibial spine fracture from weaker bones or a small injury. | Tibial spine fractures are typically caused by the stress from a high-intensity activity, a hard impact to the bone, or from an already compromised or weakened bone. Usually, younger people will get a tibial spine fracture from a hard impact injury, such as a fall from a height or a sports-related injury. Older people tend to get a tibial spine fracture from weaker bones or a small injury. | ||
This type of force causes the ACL to pull on the tibial spine. Because the bones of children this age still have open growth plates, the ACL is stronger than the tibial spine and can pull away from the bone (avulse), causing a fracture. | This type of force causes the [[ACL Rehabilitation: Acute Management after Surgery|ACL]] to pull on the tibial spine. Because the bones of children this age still have open growth plates, the ACL is stronger than the tibial spine and can pull away from the bone (avulse), causing a [[Fracture]]. | ||
</ | === Classification and Management for Tibial spine fracture === | ||
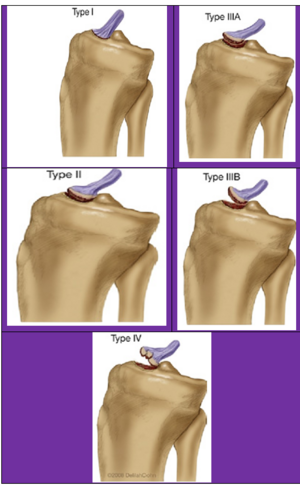
Under the Meyers and McKeever system (with modifications by Zaricznyj) injuries are classified into four main types<ref name=":0">Salehoun, Roya, and Nima Pardisnia. “Rehabilitation of tibial eminence fracture.” The Journal of the Canadian Chiropractic Association vol. 51,2 (2007): 99-105.</ref><ref>Indranil Kushare, Rushyuan Jay Lee, Henry B. Ellis, Jr.,Peter D. Fabricant, Theodore J. Ganley,Daniel W. Green, Scott McKay, Neeraj M. Patel, Gregory A. Schmale, Morgan Weber, Tibial Spine Research Interest Group (PRiSM); R. Justin Mistovich, | |||
Tibial Spine Fracture Management - Technical Tips and Tricks from the Tibial Spine Fracture Research Interest Group | |||
Available from:https://jposna.org/index.php/jposna/article/download/68/68</ref>: | |||
* '''Type I is the minimal displacement of an avulsed fragment:''' This injury is treated conservatively by closed reduction, where the tibia is set into place without a surgical incision. and then the knee is immobilized in a long-leg cast or a fracture brace set at 10 to 20 degrees of knee flexion. Fixed flexion is recommended due to the fact that full extension may place excessive tension on the ACL and popliteal artery. Immobilization is then recommended for approximately 6 weeks depending on the patient's age, healing rate, and radiological findings. | * '''Type I is the minimal displacement of an avulsed fragment:''' This injury is treated conservatively by closed reduction, where the tibia is set into place without a surgical incision. and then the knee is immobilized in a long-leg cast or a fracture brace set at 10 to 20 degrees of knee flexion. Fixed flexion is recommended due to the fact that full extension may place excessive tension on the ACL and popliteal artery. Immobilization is then recommended for approximately 6 weeks depending on the patient's age, healing rate, and radiological findings. | ||
* '''Type II classification is the displacement of half of the anterior third of the ACL insertion causing a posterior hinge:''' In most cases, closed reduction and immobilization may be attempted after aspirating knee haemarthrosis. Knee extension allows femoral condyles to reduce the displaced fragment. If acceptable reduction is achieved conservative management should be continued. If there is persistent superior displacement of the fragment seen in the x-ray then it is preferable to do arthroscopic reduction and internal fixation because chances for soft tissue entrapment at the fracture site are high. | * '''Type II classification is the displacement of half of the anterior third of the ACL insertion causing a posterior hinge:''' In most cases, closed reduction and immobilization may be attempted after aspirating knee haemarthrosis. Knee extension allows femoral condyles to reduce the displaced fragment. If acceptable reduction is achieved conservative management should be continued. If there is persistent superior displacement of the fragment seen in the x-ray then it is preferable to do arthroscopic reduction and internal fixation because chances for soft tissue entrapment at the fracture site are high. | ||
* ''' Type III is the complete separation of the avulsion site:''' | * ''' Type III is the complete separation of the avulsion site:''' | ||
* '''Type IV was later added by Zariczynj to include comminuted fractures of the tibial spine:''' Type III & Type IV | * '''Type IV was later added by Zariczynj to include comminuted fractures of the tibial spine:''' Type III & Type IV Treatment of displaced tibial spine avulsion fractures has evolved over a period of time from conservative management to open reduction and internal fixation to arthroscopic reduction and internal fixation. Various methods of fixation are used in the operative treatment of these fractures varying from retrograde wires /screws, antegrade screws, sutures, suture anchors, and a recently described suture bridge and K wire and tension band wiring technique. | ||
* [[File:Tibial spine avulsion fracture.png|center|thumb|Figure shows Meyers and McKeever system (with modifications by Zaricznyj) Classification ]] | * [[File:Tibial spine avulsion fracture.png|center|thumb|Figure shows Meyers and McKeever system (with modifications by Zaricznyj) Classification ]] | ||
| Line 37: | Line 45: | ||
* Reduced knee range of movement (ROM) | * Reduced knee range of movement (ROM) | ||
* History of trauma | * History of trauma | ||
* Pain | * [[Pain Assessment|Pain]] | ||
=== Differential Diagnosis === | |||
* ACL tear, | |||
* [[Meniscal Lesions|Meniscal tear]], | |||
* [[Lateral Collateral Ligament of the Knee|LCL]] or [[Medial Collateral Ligament Injury of the Knee|MCL]] sprain, | |||
* [[Patellar Fractures|Patella fracture]], | |||
* Osteochondral fragment, | |||
* [[Femoral Fractures|Femoral condyle fracture]], | |||
* [[Tibial Plateau Fractures|Tibial plateau fracture.]] | |||
Differential diagnosis can be ruled in or out by obtaining radiographs of the knee and using further diagnostic imaging such as [[CT Scans|CT]] or [[MRI Scans|MRI]] to assist in the diagnosis. | |||
=== Diagnostic Procedures & Imaging === | === Diagnostic Procedures & Imaging === | ||
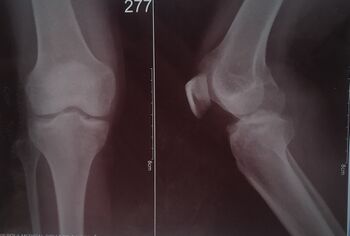
Standard imaging for tibial spine fractures | Standard imaging for tibial spine fractures includes anteroposterior (AP) and lateral radiographs. Lateral radiographs should be true lateral radiographs which are particularly useful to assess degree of displacement and type of fracture. CT scan is useful in better assessment of fracture anatomy and degree of communitions. MRI is useful in outlining the non-osseous concomitant injuries like meniscal injury, cartilage injury and other ligamentous injury<ref>Vikram Sapre and Vaibhav Bagaria | ||
Tibial Spine Avulsion Fractures: Current Concepts and Technical Note on Arthroscopic Techniques Used in Management of These Injuries | |||
Last accessed on 19/6/2024 | |||
Available from: | |||
https://www.intechopen.com/chapters/43257</ref>. along with this on physical examination with special test for knee joint doctor will rule out other knee conditions. | |||
[[File:Xray of right knee.jpg|center|thumb|350x350px|Right knee x-ray AP & Lateral view showing tibial spine avulsion fracture]] | |||
=== Management / Post-Operative Rehabilitation === | === Management / Post-Operative Rehabilitation === | ||
Tibial eminence fractures have excellent prognosis. Previously, prolonged immobilization may lead to arthrofibrosis and a permanent loss of full extension. Therefore, earlier rehabilitation is crucial as it encourages a faster recovery and prevents the development of secondary complications. Rehabilitation is similar to ACL tear protocols and which has been described in below table. | Tibial eminence fractures have excellent prognosis. Previously, prolonged immobilization may lead to arthrofibrosis and a permanent loss of full extension. Therefore, earlier rehabilitation is crucial as it encourages a faster recovery and prevents the development of secondary complications. [[Rehabilitation During a Pandemic in People with Specific Rehabilitation Needs|Rehabilitation]] is similar to ACL tear protocols and which has been described in below table<ref>https://www.slu.edu/medicine/orthopaedic-surgery/sports-medicine/_pdfs/tibial-spine-repair.pdf</ref><ref name=":0" />. | ||
{| class="wiki table" | {| class="wiki table" | ||
|+ | |+ | ||
| Line 70: | Line 96: | ||
* Weeks 0-2: TTWB | * Weeks 0-2: TTWB | ||
* Weeks 3-4: PWB | * Weeks 3-4: PWB | ||
* Weeks 5-6: Wean from crutches as the patient demonstrates normal gait mechanics and improved quad control. | * Weeks 5-6: Wean from crutches as the patient demonstrates normal [[gait]] mechanics and improved quad control. | ||
| | | | ||
* AAROM → as tolerated starting in week 2 | * AAROM → as tolerated starting in week 2 | ||
| Line 86: | Line 112: | ||
* Maintain full extension, obtain full flexion | * Maintain full extension, obtain full flexion | ||
* Increase hip, quadriceps, hamstring, and calf strength | * Increase hip, quadriceps, hamstring, and calf strength | ||
* Increase proprioception | * Increase [[proprioception]] | ||
| | | | ||
* Begin unlocking in 30⁰ increments (every 3-4 days) after Week 6. | * Begin unlocking in 30⁰ increments (every 3-4 days) after Week 6. | ||
| Line 116: | Line 142: | ||
| | | | ||
| | | | ||
* Progress flexibility/strength program based on individual needs/deficits | * Progress [[flexibility]]/[[Strength Training|strength]] program based on individual needs/deficits | ||
* Initiate plyometric program as appropriate for patient’s athletic goals | * Initiate plyometric program as appropriate for patient’s athletic goals | ||
* Agility progression including Side steps + Crossovers, Figure 8 and Shuttle Running,One & Two Leg Jumping Cutting/Accelerative/Deceleration/Springs, Agility Ladder Drills | * [[Agility]] progression including Side steps + Crossovers, Figure 8 and Shuttle Running, One & Two Leg Jumping Cutting/Accelerative/Deceleration/Springs, Agility Ladder Drills | ||
* Continue progression of running distance based on patient needs | * Continue progression of running distance based on patient needs | ||
* Sport-specific drills as appropriate for patient | * Sport-specific drills as appropriate for patient | ||
| Line 125: | Line 151: | ||
=== References === | === References === | ||
[[Category:Ligaments]] | [[Category:Ligaments]] | ||
[[Category:Knee - Conditions]] | [[Category:Knee - Conditions]] | ||
[[Category:Injury]] | [[Category:Injury]] | ||
[[Category:Knee - Bones]] | [[Category:Knee - Bones]] | ||
<references /> | |||
[[Category:Fractures]] | |||
[[Category:Sports Injuries]] | |||
[[Category:Musculoskeletal/Orthopaedics]] | |||
Latest revision as of 15:43, 19 June 2024
Original Editor - Ruchi Desai
Top Contributors - Ruchi Desai, Mohit Chand, Kim Jackson and Lucinda hampton
Introduction[edit | edit source]
Tibial spine fractures are uncommon injuries that occur when the bony projection on the tibia, known as the tibial spine, is subjected to significant trauma. These fractures often result from high-energy events such as motor vehicle accidents, falls, or sports-related injuries. The severity can range from non-displaced to displaced fractures, which poses a greater risk of complications if not managed properly. Understanding the relevant anatomy, pathogenesis, diagnosis, management, and rehabilitation strategies is crucial for achieving favorable patient outcomes.
Clinically Relevant Anatomy[edit | edit source]
The lower leg is made up of two bones: the tibia and fibula. The tibia is the larger of the two bones. It supports most of your weight and is an essential part of both the knee joint and ankle joint. The tibial spine is a specialized ridge of bone in the tibia where the anterior cruciate ligament (ACL) attaches. This ligament is integral maintaining flexibility and stability in the knee.
Tibial spine fracture (also called Tibial Eminence Fracture) is a break at the top of the tibia bone in the lower leg near the knee as a result of high amounts of tension placed upon the Anterior cruciate ligament (ACL). This type of injury is most common in
1) Children ages 8 to 14 years of age[1].[2]
2) The incidence of these fractures is higher among adolescent girls due to their inherent skeletal immaturity.
3) It has also been proposed that injury occurs secondary to greater elasticity of ligaments in young people.
4) It can occur during a sporting event or direct trauma with a hyperextension injury causes an avulsion fracture occurring at the tibial eminence while the ACL is spared.
Here is a video for better understanding:
Mechanism of Injury / Pathological Process[edit | edit source]
Tibial spine fractures are typically caused by the stress from a high-intensity activity, a hard impact to the bone, or from an already compromised or weakened bone. Usually, younger people will get a tibial spine fracture from a hard impact injury, such as a fall from a height or a sports-related injury. Older people tend to get a tibial spine fracture from weaker bones or a small injury.
This type of force causes the ACL to pull on the tibial spine. Because the bones of children this age still have open growth plates, the ACL is stronger than the tibial spine and can pull away from the bone (avulse), causing a Fracture.
Classification and Management for Tibial spine fracture[edit | edit source]
Under the Meyers and McKeever system (with modifications by Zaricznyj) injuries are classified into four main types[4][5]:
- Type I is the minimal displacement of an avulsed fragment: This injury is treated conservatively by closed reduction, where the tibia is set into place without a surgical incision. and then the knee is immobilized in a long-leg cast or a fracture brace set at 10 to 20 degrees of knee flexion. Fixed flexion is recommended due to the fact that full extension may place excessive tension on the ACL and popliteal artery. Immobilization is then recommended for approximately 6 weeks depending on the patient's age, healing rate, and radiological findings.
- Type II classification is the displacement of half of the anterior third of the ACL insertion causing a posterior hinge: In most cases, closed reduction and immobilization may be attempted after aspirating knee haemarthrosis. Knee extension allows femoral condyles to reduce the displaced fragment. If acceptable reduction is achieved conservative management should be continued. If there is persistent superior displacement of the fragment seen in the x-ray then it is preferable to do arthroscopic reduction and internal fixation because chances for soft tissue entrapment at the fracture site are high.
- Type III is the complete separation of the avulsion site:
- Type IV was later added by Zariczynj to include comminuted fractures of the tibial spine: Type III & Type IV Treatment of displaced tibial spine avulsion fractures has evolved over a period of time from conservative management to open reduction and internal fixation to arthroscopic reduction and internal fixation. Various methods of fixation are used in the operative treatment of these fractures varying from retrograde wires /screws, antegrade screws, sutures, suture anchors, and a recently described suture bridge and K wire and tension band wiring technique.
Clinical Presentation[edit | edit source]
- Swelling
- Inability to weight bear
- Bruising
- Reduced knee range of movement (ROM)
- History of trauma
- Pain
Differential Diagnosis[edit | edit source]
- ACL tear,
- Meniscal tear,
- LCL or MCL sprain,
- Patella fracture,
- Osteochondral fragment,
- Femoral condyle fracture,
- Tibial plateau fracture.
Differential diagnosis can be ruled in or out by obtaining radiographs of the knee and using further diagnostic imaging such as CT or MRI to assist in the diagnosis.
Diagnostic Procedures & Imaging[edit | edit source]
Standard imaging for tibial spine fractures includes anteroposterior (AP) and lateral radiographs. Lateral radiographs should be true lateral radiographs which are particularly useful to assess degree of displacement and type of fracture. CT scan is useful in better assessment of fracture anatomy and degree of communitions. MRI is useful in outlining the non-osseous concomitant injuries like meniscal injury, cartilage injury and other ligamentous injury[6]. along with this on physical examination with special test for knee joint doctor will rule out other knee conditions.
Management / Post-Operative Rehabilitation[edit | edit source]
Tibial eminence fractures have excellent prognosis. Previously, prolonged immobilization may lead to arthrofibrosis and a permanent loss of full extension. Therefore, earlier rehabilitation is crucial as it encourages a faster recovery and prevents the development of secondary complications. Rehabilitation is similar to ACL tear protocols and which has been described in below table[7][4].
| Goals | Brace | Weight Bearing | ROM | Exercises | |
|---|---|---|---|---|---|
| Phase -I
(0-6 Weeks) |
|
|
|
|
|
| Phase II: (Weeks 7-12) |
|
|
|
| |
| Phase III: (Weeks 13-18) |
| ||||
| Phase IV: (Months 5-6 )- Return to Sport |
|
References[edit | edit source]
- ↑ GronkvistHFracture of the anterior tibial spine in children. J Pediatr Orthop, 19844465468
- ↑ eyersM. HMckeeverF. MFracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am 19705216771683
- ↑ Dr. David Geier. Tibial spine fracture: What is this knee injury, and how can you get better?: https://www.youtube.com/watch?v=Kt_iAsqns8A [last accessed 19/6/2024]
- ↑ 4.0 4.1 Salehoun, Roya, and Nima Pardisnia. “Rehabilitation of tibial eminence fracture.” The Journal of the Canadian Chiropractic Association vol. 51,2 (2007): 99-105.
- ↑ Indranil Kushare, Rushyuan Jay Lee, Henry B. Ellis, Jr.,Peter D. Fabricant, Theodore J. Ganley,Daniel W. Green, Scott McKay, Neeraj M. Patel, Gregory A. Schmale, Morgan Weber, Tibial Spine Research Interest Group (PRiSM); R. Justin Mistovich, Tibial Spine Fracture Management - Technical Tips and Tricks from the Tibial Spine Fracture Research Interest Group Available from:https://jposna.org/index.php/jposna/article/download/68/68
- ↑ Vikram Sapre and Vaibhav Bagaria Tibial Spine Avulsion Fractures: Current Concepts and Technical Note on Arthroscopic Techniques Used in Management of These Injuries Last accessed on 19/6/2024 Available from: https://www.intechopen.com/chapters/43257
- ↑ https://www.slu.edu/medicine/orthopaedic-surgery/sports-medicine/_pdfs/tibial-spine-repair.pdf