Degenerative Disc Disease
Original Editor - Amanda E Davidson and Colby Boers, Lisa Pernet
Top Contributors - Lisa Pernet, Gaëlle Vertriest, Admin, Vanbeylen Antoine, Amanda E Davidson, Garima Gedamkar, Candace Goh, Scott Cornish, Uchechukwu Chukwuemeka, Laura Ritchie, Kim Jackson, WikiSysop, 127.0.0.1, De Maeght Kim, Lucinda hampton, Aya Alhindi and Eric Robertson
Definition/Description[edit | edit source]
Degenerative disc disease (DDD) is a process in which the intervertebral discs, which provide cushioning between the vertebra of the spine, lose height and hydration. When this occurs, the intervertebral discs are unable to fulfill their primary functions: cushioning and providing mobility between the vertebrae.
Although the exact cause of DDD is unknown, it is thought to be associated with the aging process during which the intervertebral discs become dry, lose elasticity, and collapse. Furthermore a degenerative disc disease may develop at any level of the spine, but is most common in the cervical and lower lumbar sections of the spine.[1][2][3]
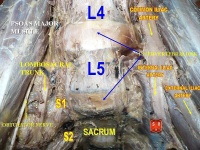
Clinically Relevant Anatomy[edit | edit source]
Lumbar DDD is a condition that can imply lower back pain, this results from the co-existence of two different time scales: on one hand the slow dynamics of disc degeneration and on the other hand the fast dynamics of pain recurrence. [4]
Lumbar DDD can also imply radiating pain from damaged discs in the spine. A lumbar spinal disc acts as a shock absorber between two vertebrae and allows the joints and the spine to move easily. The outer portion, the annulus fibrosis, contains the soft inner core of the disc, the nucleus pulposus. Each person’s spinal discs undergo degenerative changes as they age. But not all people will notice symptoms as a result of these changes. One of the ways DDD causes pain is through inflammation of the nerves. When the outer portion of the disc breaks, the inner part can leak out, releasing proteins that can irritate the nerves surrounding from the disc. Another cause is when degenerated discs can’t properly absorb stress. Leading to abnormal movement around the vertebral segment. Back muscles will hereby spasm painfully in order to stabilize the spine. In some cases the segment may collaps so a nerve root gets compressed, leading to radiculopathy. the pain from DDD often goes away with time because the inflammatory proteins will disappear and the disc collaps in a stable position. [5]
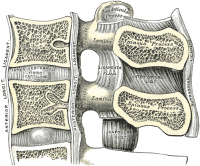
Intervertebral Discs
Dengenerative Disc Disease (DDD) is thought to begin with changes to the annulus fibrosis, intervertebral disc, and subchondral bone. The process of degeneration is divided into three classifications including: early dysfunction, intermediate instability, and final stabilization.
Early dysfunction is the classifed as the beginning of degenerative changes which can occur as early as 20 years. Intermediate instability is classified by a loosening of the annulus fibrosis, which can cause back pain. Fibrosis to the posterior structure and formation of osteophytes denotes the final stabilization classification. Pain decreases, and motion descreases. Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Epidemiology /Etiology[edit | edit source]
Degenerative disc disease refers to a condition in which the involved disc causes LBP. Lumbar degenerative disc disease is usually the result of a twisting injury to the lower back, such as when a person swings a golf club or rotates to put an object on a surface to the side of or behind them.Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
The pain is also frequently caused by simple wear and tear on the spine and comes with the general aging process.
Degenerative disc disease is fairly common, and it is estimated that at least 30% of people aged 30-50 years old will have some degree of disc space degeneration, although not all will have pain or ever receive a formal diagnosis.Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
The process that leads to DDD begins with structural changes. The annulus fibrosis (outer portion of the disc) loses water content over time which will make it increasingly unyielding toward everyday stress and strain on the spine. The loss of compliance in the discs contributes to forces being redirected from the anterior and middle portions of the facets to the posterior aspect, thus causing facet arthritis. Another result is hypertrophy of the vertebral bodies adjacent to the degenerating disc. The overgrowths are known as bony spurs (or osteophytes.)
Characteristics/Clinical Presentation[edit | edit source]
Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
|
DDD commonly occurs with other diagnoses such as:
- idiopathic low-back pain
- lumbar radiculopathy
- myelopathy
- lumbar stenosis
- spondylosis[3]
- osteoarthritis
- zygapophydeal joint degeneration Cite error: Invalid
<ref>tag; name cannot be a simple integer. Use a descriptive title
Activities that typically increase pain include:
- Sitting for extended periods of time
- Rotating, bending, or lifting
- Activities that typically decrease pain include:
- Changing positions often
- Lying down
- Staying active Cite error: Invalid
<ref>tag; name cannot be a simple integer. Use a descriptive title
Differential Diagnosis[edit | edit source]
People with DDD will have low back painCite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title; however there are varying levels of severity. Pain is often chronic, but one with DDD can experience varying episodes of exacerbation where pain levels are elevatedCite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
There are different degrees of annular disruption[1]. We can classify them into 4 grades, at which grade 0 is added. We differentiate these grades by means of a contrast medium injection.
- Grade 0: no disruption
- Grade 1: the contrast medium passes into the cartilage endplate through tear
- Grade 2: the contrast medium flows into the bony endplate
- Grade 3: the contrast medium is going into the cancellous bone of vertebra under endplate
- Grade 4: the contrast medium leaks completely in the cancellous bone.
Diagnostic Procedures[edit | edit source]
Provocation discography is a diagnostic test to identify a painful disc. To evaluate the degree of disruption, a combination of discogram and CTscan afther discography is used.[1]
Xray findings are used to diagnose DDD. Anterior-Posterior and lateral views are taken; presence of osteophytes, narrowing of the disc joint space, or a “vacuum sign” is noted. Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Outcome Measures[edit | edit source]
None of the analyzed literature has reported a uniform system of outcome measuring. The most common form of outcome measure for DDD is Oswestry Disabilty Index (ODI) in combination with other forms of outcome measure: Short Form 36(or SF-12) questionnaire, self-paced walk, timed up-and-go test (TUG),Visual Analogue Scale (VAS), Roland-Morris disability index (RMDI)[6][7] (level of evidence 3A,1B).
A radomized controle trial (Lars G Johnsen et al., 2013, level of evidence:1B ) analysed the difference between the ODI, the SF6D and the EQ5D.
In their research the several outcome measures reached different scores in the Receiver Operator Curve (ROC). The ODI showed a sensitivity of 88% and specificity of 85%, the EQ5D a sensitivity of 73% and specificity of 79% and the SF6D a sensitivity 93% and specificity 78%. But the EQ5D and the SF6D don’t measure the same constructs and therefore cannot be used interchangeably.[8]
A systematic review tried to evaluate wich outcome measure were suitable for DDD. They found out that the Oswestry Disability Index a good primary outcome measure is for lumbar fusion and nonsurgical interventions for various symptomatic degenerative spine disorders (level of evidence: 3A).[9] Although further research is needed.
Examination[edit | edit source]
It is very important to look at the patient’s history, this is a very valuable tool for identifying the intervertebral disc as the nociceptive source. Patients may present with a history of Chronic LBP, and can experience symptoms into the buttock. They may also state a history of spine stiffness that gets worse with activity and tenderness with palpation over involved area. Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Mood and anxiety disorders were diagnosed using the Structured Clinical Interview of the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition/Clinical Version Mood and anxiety disorders were more commonly seen in patients with lumbar or cervical disc herniation than in those without herniation. No relationship was detected between pain severity and mood or anxiety disorders. However, mood and anxiety disorders were associated with neurological deficits. [10]
Magnetic resonance imaging (MRI) is the most common used method of specifically assessing intervertebral disc degeneration. Based on proton density, water content an chemical environment MR depicts disc hydratation and morphology which can be visualized on MR images with T2 weighting as hypointense signal. Pfirrmann et al devised a grading system for disc degeneration based on MR signal intensity, disc structure, distinction between nucleus and anulus, and disc height.[11] This useful grading system has been accepted and applied clinically
The modified system comprises 8 grades for lumbar disc degeneration (Table 1). Sagittal T2-weighted images were used for classification as they provide a comprehensive perception of disc structure and good tissue differentiation.The 8 grades represented a progression from normal disc to severe disc degeneration. Grade 1 corresponds to no disc degeneration while Grade 8 corresponds to end-stage degeneration. Beside the 8-grade table there is also an image reference panel (Figure 1).[12]
Medical management
[edit | edit source]
The preferential treatment for patients with chronic low back pain, caused by disc degeneration, is a conservative method consisting of physical therapy and medications (O'Halloran, 2007 (D)). Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Conservative treatment (home or hospital) includes rest, adequate program for motoractivity, regime of physical activity, strengthening of musculature, analgetic medication, physiotherapy, rehabilitation programs and lifestyle adjustments such as weight loss. [13]
Medications such as non-steroidal anti-inflammatories (e.g., ibuprofen, naproxen, COX-2 inhibitors) and pain relievers like acetaminophen (such as Tylenol) help many patients feel good enough to engage in regular activities. Stronger prescription medications such as oral steroids, muscle relaxants or narcotic pain medications may also be used to manage intense pain episodes on a short-term basis, and some patients may benefit from an epidural steroid injection. Not all medications are right for all patients, and patients will need to discuss side effects and possible factors that would preclude taking them with their physician. Epidural steroid injections can provide low back pain relief by delivering medication directly to the painful area to decrease inflammation.
Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Lately, successful outcomes were demonstrated by animal experiments with mesenchymal stem cells.[13][1]
Surgical intervention includes disc arthroplasty and lumbar spinei[1][13] fusion to reduce chronic low back pain due to degenerative disc disease.[14]
In some cases another form of chirurgical management is used for treatment of DDD, it is named: Device for Intervertebral Assisted Motion (DIAM). The DIAM is a polyester-encased silicone interspinous dynamic stabilization device that can unload the anterior column and reestablish the functional integrity of the posterior column. This device is designed for preservation of the functional spinal unit. [15] (Level of evidence 2B)
In some other cases, patients are not responsive to nonsurgical treatment for symptomatic degenerative disc disease (DDD). In that case patients can undergo a lumbar total disc replacement (TDR). Patients presenting with symptomatic single-level lumbar DDD who failed at least 6 months of nonsurgical management were randomly allocated to treatment with an investigational TDR device (also called: TDR activL device) or FDA-approved control devices TDR. After 2 years of research, we can conclude that the single-level activL TDR is safe and effective for the treatment of symptomatic lumbar DDD. Lumbar total disc replacement (TDR) improved mean back back pain. (level of evidence: 2B) [16]
Physical management[edit | edit source]
A part of the physical therapy treatment is aimed at reducing pain. For this purpose, different physical modalities are used, including heat and cold application, traction, spinal manipulations (Beattie P, 2008 (D); Zhang Y (C), 2008; Mirza SK, 2007 (A1))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive titleCite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive titleCite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title, exercise programs and electrical stimulation such as ‘TENS’ and ‘pulsed radiofrequency (PRF)’ treatment.[17] With this PRF treatment, 56% of 76 patients with discogenic pain had more than 50% pain reduction one year after the first treatment.
Other objectives are to enhance the core stability by strengthening and improving the coordination between the abdominal and back muscles through a spinal stabilization program (Brox JI, 2003 (A2)).Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title These stabilization exercises can increase the patient’s capacity to resist higher loads in the degenerative discs(Beattie P, 2008 (D))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title. A posterior dynamic stabilization program proved a significant improvement in pain and disability.[18][19]
In patients with degenerative disc disease it is also advised to add behavioral therapy to the usual treatment since it has been shown that the addition of behavioral therapy gives better results (Brox JI, 2003 (A2))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title. This is related to the fact that the diagnosis of degenerative disc disease also entails many psychological effects. Many patients assume that degeneration means that their spine is becoming weaker, associated with constant pain. These erroneous thoughts often cause fear of movement (kinesiophobia) and lead to the avoidance of movements of the spine (Beattie P, 2008 (D))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title.
The task of the physical therapists includes giving information and advice to improve the compliance rate.(Mirza SK, 2007 (A1))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title. Good communication with patients is of great importance, they have to realize that degeneration of the intervertebral disc is a normal aging process. The physiotherapist must help the patients to identify and overcome their fears and to adapt their coping strategies (Mirza SK, 2007 (A1))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title. It is important that patients understand that they must stay active and that activities of daily life and other moderate physical activity will not cause additional damage or have adverse effects (Brox JI, 2003 (A2))Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title. Patients must be encouraged to perform low impact aerobic exercises, such as walking and water aerobics. Low impact aerobic conditioning ensures adequate flow of nutrients and blood to spine structures, and decreases pressure on the discs. They should avoid prolonged static postures as much as possible (Beattie P, 2008 (D); Brox JI, 2003 (A2)).Cite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive titleCite error: Invalid <ref> tag; name cannot be a simple integer. Use a descriptive title
Extension exercises are given to displace the pressure on the discus intevertebralis anteriorly. Some exercises are:
- Hollow the back
- Make a sphinx posture
- Lie with the upper body prone on a table, the legs hang off. Lift the legs against the force of gravity. This is a back strengthening exercise.
- The last exercise can also be carried out on a ball.[20][21][19]
Resources
[edit | edit source]
add appropriate resources here
Clinical Bottom Line[edit | edit source]
add text here
Recent Related Research (from Pubmed)[edit | edit source]
Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1pMPQVclnMMdhoCVXc_6QwikGZ1oJDfw8DH__4CDKu4nrbvM0x|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1jcCSTNs5ufLgbvB_E4LH4yZzt4a0ktD5ViUIMh5VyqUJQjkEn|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=16ooSLsIx9qeAalLyyodh3w-tSqfHVVKzfdnn87DcC_P-Li1ho|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1-KHXJhm35hbwR0UYXkVZjhNASb5b-RjWyFkmfxYo6-ZaVdEW9|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1ZEzhvEsCLGbIuvYmXIo6xEHcunDWsjfD7C6_2bOnLhZURUEZG|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1hMQ8bQB8dXT7O4UMxfVfcMjjYIGeLpWzOjsX-ExF6bYCr1kfx|charset=UTF-8|short|max=10: Error parsing XML for RSS Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1PsNRxjiL269MVconGgUNMELZlAiuh-M_iP9ofPKouYgWJQMZ3|charset=UTF-8|short|max=10: Error parsing XML for RSS
</div>
References[edit | edit source]
References will automatically be added here, see adding references tutorial.
- ↑ 1.0 1.1 1.2 1.3 1.4 Peng B., Pathophysiology, diagnosis, and treatment of discogenic low back pain, World J Orthop 2013 April 18; 4(2): 42-52 LEVEL OF EVIDENCE 1
- ↑ Dr Vanaclocha V., et al, Degeneratieve ziekte van het disc, Clinica Neuros Neurochirurgie, 2010fckLR(http://neuros.net/nl/algemene_degenerative_ziekte_van_disc.php) LEVEL OF EVIDENCE 5
- ↑ 3.0 3.1 McCormack BM, Weinstein PR. Cervical spondylosis. An update. West J Med 1996; 165(1-2): 43-51 (Level of evidence: 1A)
- ↑ Chang-jiang Zheng et al.; Disc degeneration implies low back pain; Theoretical Biology and Medical Modelling (2015) (Level of evidence: 2C)
- ↑ Spine-health, Degenerative Disc Disease Health Center, http://www.spine-health.com/conditions/degenerative-disc-disease (asseced 18-05-2016) (level of evidence 5)
- ↑ Bono, C. M., & Lee, C. K.; Critical Analysis of Trends in Fusion for Degenerative Disc Disease Over the Past 20 Years: Influence of Technique on Fusion Rate and Clinical Outcome; Spine Volume; 2004; vol. 29; p455-463. (level of evidence: 3A)
- ↑ Malhar N. Kumar, F. J. (2001); Long-term follow-up of functional outcomes and radiographic changes at adjacent levels following lumbar spine fusion for degenerative disc disease; European Spine Journal volume 10; p309-313. (level of evidence: 1B)
- ↑ Lars G Johnsen, Christian Hellum, Øystein P Nygaard, Kjersti Storheim, Jens I Brox , Ivar Rossvoll, Gunnar Leivseth and Margreth Grotle; Comparison of the SF6D, the EQ5D, and the oswestry disability index in patients with chronic low back pain and degenerative disc disease; BMC Musculoskeletal Disorders; 2013; vol. 14; p148-157. (level of evidence: 1B)
- ↑ LY Carreon, S. G.; Fusion and nonsurgical treatment for symptomatic lumbar degenerative disease: a systematic review of Oswestry Disability Index and MOS Short Form-36 outcomes; The spine journal; 2007 (Level of evidence: 3A)
- ↑ Kayhan F, Albayrak Gezer İ, Kayhan A, Kitiş S, Gölen M. Mood and anxiety disorders in patients with chronic low back and neck pain caused by disc herniation. Int J Psychiatry Clin Pract. 2015 Nov 2:1-5. (level of evidence 1B)
- ↑ Pfirrmann CW, Metzdorf A, Zanetti M, et al. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 2001;26:1873–8 (Level of evidence 2A)
- ↑ Griffith JF et al; Modified Pfirrmann grading system for lumbar intervertebral disc degeneration; Spine (Phila Pa 1976). 2007 Nov 15;32(24):E708-12. ( Level of evidence: 2C)
- ↑ 13.0 13.1 13.2 Drazin D., Rosner J., Avalos P., Acosta F., Stem cell therapy for degenerative disc disease, Advances in orthopedics, volume 2012, 8pg LEVEL OF EVIDENCE = 1
- ↑ Phillips F.M., Slosar P.J., Youssef J.A., Andersson G., Papatheofanis F., Lumbar spine fusion for chronic low back pain due to degenerative disc disease, SPINE Volume 38, Nr 7, Pp. E409-E422, 2013 LEVEL OF EVIDENCE = 1
- ↑ Jean Taylor, M., Patrick Pupin, M., Stephane Delajoux, M., & Sylvain Palmer, M.; Device for Intervertebral Assisted Motion: Technique and Initial Results; Neurosurg Focus; 2007; p1-22. (Level of evidence 2B)
- ↑ Garcia R, Yue JJ, Blumenthal S, Coric D, Patel VV, Leary SP, Dinh DH, Buttermann GR, Deutsch H, Girardi F, Billys J, Miller LE. Lumbar Total Disc Replacement for Discogenic Low Back Pain: Two-year Outcomes of the activL Multicenter Randomized Controlled IDE Clinical Trial. Spine (Phila Pa 1976). 2015 Nov 27 (2B)
- ↑ Rohof O., Intradiscal pulsed radiofrequency application following provocative discography for the management of degenerative disc disease and concordant pain: a pilot study, Pain practice, 2012, Volume 12, Issue 5, Pg 342-349 LEVEL OF EVIDENCE 2
- ↑ Zagra A., et al; Prospective study of a new dynamic stabilisation system in the treatment of degenerative discopathy and instability of the lumbar spine, Eur Spine J, 2012, 21, suppl 1: S83-S89 LEVEL OF EVIDENCE 2
- ↑ 19.0 19.1 Canbay S., et al, Posterior dynamic stabilization for the treatment of patients with lumbar degenerative disc disease: long-term clinical and radiological results, Turkish Neurosurgery 2013, vol. 23, No. 2, 188-197 LEVEL OF EVIDENCE 2
- ↑ Extremiteiten, www.fysio.net, Extensieoefening voor de lumbale wervelkolom in buikligging, 29-10-2009fckLR(http://www.youtube.com/watch?v=SNamjanZttM&amp;amp;amp;feature=youtube_gdata) LEVEL OF EVIDENCE 5
- ↑ Kielbaso J., Hardcore abs training, Fit4Less4Info, 19oktober2012fckLR(http://fit4lessamsterdam.wordpress.com/2012/10/) (http://fit4lessamsterdam.files.wordpress.com/2012/10/crunchleg-raise.jpg) LEVEL OF EVIDENCE 5