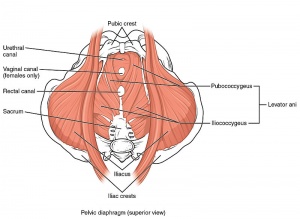
Pelvic Floor and Other Pelvic Disorders
Original Editor - Laura Ritchie
Top Contributors - Laura Ritchie, Kim Jackson, Evan Thomas, Vidya Acharya, Nicole Hills and Rishika Babburu
Vulvodynia
[edit | edit source]
Definition
[edit | edit source]
Vulvar discomfort occuring in the absence of relevant visible findings or a specific, clinically-identifiable, neurological disorder.
Symptoms
[edit | edit source]
- Burning
- Stabbing
- Stinging
- Itching
- Allodynia (light touch perceived as pain)
- Hyperalgesia (mildly noxious stimulus perceived as severely noxious)
- Functional limitation (e.g. pain during intercourse, using tampons, sitting)
Diagnosis
[edit | edit source]
Symptoms should be present for 3-6 months before this diagnosis is considered.
Other conditions that should be ruled out include;
- Vulvovaginal candidiasis
- Bacterial vaginosis
- Trichomoniasis
- Genital herpes
- Neuropathic viruses (e.g. Herpes zoster)
- HPV
- Lichens simples chronicus
- Lichens simples sclerosus
- Lichens planus
- Contact dermatitis
- Atrophic vaginitis
- Squamous cell carcinoma
- Pudendal nerve injury
- Referred pain from sacral nerve roots after disc injury
- Neurologic disease (e.g. MS)
Classifications
[edit | edit source]
Generalized vulvodynia;
- Almost constant, typically burning pain
- Affects the entire vulva
- Provoked (sexual, non-sexual or both)
- Unprovoked
- Mixed (provoked and unprovoked)
Localized vulvodynia / vestibulodynia;
- Localized to vulvar vestibule
- Burning / cutting pain at entrance of vagina
- Provoked (sexual, non-sexual or both)
- Unprovoked
- Mixed (provoked and unprovoked)
Co-Morbidities
[edit | edit source]
- Interstitial cystitis
- Fibromyalgia
- Irritable Bowel Syndrome
- Depression
- Dyspareunia
- TMJ or facial pain
- Overactive pelvic floor
Dyspareunia / Vaginismus[edit | edit source]
Definition[edit | edit source]
Dyspareunia: Painful vaginal penetration in the absence of disease
Vaginismus: Inability to penetrate due to spasm of the muscles
Causes[edit | edit source]
- Painful scar / episotomy
- Vulvodynia - Interstitital cystitis
- Protective response to infection, inflammation, injury or decreased estrogen or fear
Lichens Simplex[edit | edit source]
- Chronic irritation of the vulva
- Leads to itching, scratching and thickening of the skin
- Vulva can be weepy, causing moisture
Lichens Sclerosis[edit | edit source]
- Auto-immune disorder
- Itching or burning
- Skin with white patches
- Scars and adhesions of the vulva
- Easily bruised and torn
Lichens Planus[edit | edit source]
- Chronic mucocutaneous disease
- Itching or burning
- Scar adhesions
- On the vulva and in the vagina
- Affects other mucosal membranes e.g. oral, genital, esophageal - oral rash typically occurs first
- Significant pain
Desquamative Inflammatory Vaginitis[edit | edit source]
Definition[edit | edit source]
- Profuse discharge with irritation of the vulva and vagina
- Inflammation causes the vaginal wall to peel or shed (desquamation)
- No cancerous, contagious or bacterial origin known
Signs and Symptoms[edit | edit source]
- Pus-like yellow/green discharge
- May be vulvar burning and itching
- Usually no odour
- PAP smear may be abnormal
- No improvement with anti-biotics or anti-fungals
Atrophic Vaginitis[edit | edit source]
- Decreased estrogen causes thinning of the vaginal epithelium leading to inflammation
- Can cause vaginal soreness, itching and dyspareunia
- Sores and cracks can occur spontaneously
- Can have an odours discharge
Interstitial Cystitis / Painful Bladder Syndrome[edit | edit source]
Go to this page for more information
Dysmenorrhea[edit | edit source]
Definition[edit | edit source]
Painful menstrual periods
Classification[edit | edit source]
Primary: Menstrual pain without pelvic pathology, onset shortly after menarche
Secondary: Pain associated with secondary pathology, onset may be years after menarche
Risk Factors[edit | edit source]
- Low BMI and low consumption of fruit, eggs and fish (for primary dysmenorrhea)
- Poor mental health
- Primary co-morbidities: irritable bowel syndrome, interstitial cystitis, vulvodynia, dyspareunia, TMJ and migraines
- Secondary co-morbidities: endometrioses, presence of intra-uterine device, pelvic inflammatory disease, uterine myomas and adhesions
- Smoking
Endometriosis[edit | edit source]
Definition[edit | edit source]
The abnormal presence of endometrial tissue outside of the uterus. This tissue implants and can behave in a similar manner to the uterus, shedding tissue and inflammatory molecules into the abdominal/pelvic cavity.
Symptoms[edit | edit source]
- Subfertility
- Pelvic pain including dysmenorrhea
Co-morbidities[edit | edit source]
- Irritable bowel syndrome
- Interstitial cystitis
- TMJ disorders
- Migraines
- Fibromyalgia
- Autoimmune disordersAutoimmune_Disorders
Anal Fissures[edit | edit source]
Definition[edit | edit source]
Tears in the mucosal membrane of the anal canal, usually extending from anal opening. Can become chronic and deep.
Signs and Symptoms[edit | edit source]
- Pain after bowel movement
- May notice bright red bleeding on toilet paper
Causes[edit | edit source]
- Stretching of anal mucosa beyond its capacity
- Constipation or prolonged diarrhea
- Trauma during childbirth
- Crohn's disease
- Anal sex
- Poor toileting in young children
Prostatitis
[edit | edit source]
Category 1: Acute Bacterial Prostatitis
[edit | edit source]
- Diagnosed through expressed prostatic excretions
- Symptoms may include fever/chills, prostate pain, dysuria, perineal pain, difficulty urinating (hesitancy), urinary retention, low back pain
Category 2: Chronic Bacterial Prostatitis
[edit | edit source]
- Recurrent bacterial infection
- Diagnosed through expressed prostatic excretions
- Symptoms may include fever/chills, prostate pain, dysuria, perineal pain, difficulty urinating (hesitancy), urinary retention, low back pain
- Constant or intermittent symptoms that tend to be associated with the same bacteria
Category 3: Chronic Non-Bacterial Prostatitis
[edit | edit source]
Category 3A: With inflammation
[edit | edit source]
Category 3B: Without inflammation
[edit | edit source]
- Also called Chronic Pelvic Pain Syndrome or Prostatodynia
- Symptoms may include pain (perineal, rectal, suprapubic, penile, coccygeal, groin, low back), pain radiating into testicles/scrotum/central perineal tendon/anus, burning, itchiness, muscle tension, pain during and after ejaculation, feeling as if sitting on a golf ball
- Urinary symptoms may include hesitancy, dysuria, nocturia, frequency and urgency, decreased stream, feeling of poor emptying
Category 4: Asymptomatic Inflammatory Prostatitis
[edit | edit source]
- Inflammation found in the semen