Feeding the Child with Cerebral Palsy
Original Editor - Verbena Bottini as part of ICRC Cerebral Palsy Content Development Project
Top Contributors - Naomi O'Reilly, Kim Jackson, Admin, Simisola Ajeyalemi, Olajumoke Ogunleye, Ewa Jaraczewska, 127.0.0.1, WikiSysop, Jess Bell and Chelsea Mclene
Introduction[edit | edit source]
Dysphagia is a condition in which disruption of the swallowing process interferes with a patient's ability to eat and drink. But it should be seen in a more wide prospective including the huge impact that this problem has on the social/family interaction and on the personal/emotional status of the child. Therefore the treatment approach should not focus only to biomechanically make feeding safely possible but also should consider the emotional aspect of eating (pleasure, social moment etc.).
Assessment of Feeding Difficuties - Key Elements[edit | edit source]
Feeding History[edit | edit source]
Ask questions to the parents like: does the child cough when eating and drinking? How often? With certain texture more than others? Do you have any weight/growth concern? Did you notice something that make you think your child has feeding problems? Did the child get chest infection? If yes when? How often? Is the bowel movement regular? He has been ever investigated for feeding problems? Does he vomit after lunch? How much does he drink? What food does he like more? And what he doesn’t? Did you ever find food in her mouth? Is breath difficult, noisy when eating/drinking? etc.
Clinical Observation[edit | edit source]
MOST IMPORTANT PART OF THE ASSESSMENT
Children with CP have normally poor alignment due to altered postural and motor control, this, in most of the cases, leads to poor oral motor control and therefore eating/drinking problems.
As well poor breath capacity makes more difficult to take food in. These 2 aspects need to be addressed before starting any assessment of eating/drinking difficulties. Keep in mind that signs of food aspiration are more difficult to detect than liquids/saliva aspiration.
- Videofluoroscopy - Gold Standard
- Dietetic Assessment to see how the child absorbs nutrients
Main Clinical Signs/Features of Feeding Difficulties[edit | edit source]
| Poor Head / Trunk Alignment in Midline |
|
| Mouth Kept Open |
|
| Mouth Kept Firmly Closed |
|
| Bite Reflex | |
| Irregular Swallow | |
| Quick Breath | |
| Sometimes Interruption of Breath | |
| Chest Flat and Poor / No Mobility of Rib Cage | |
| Uncoordinated, Non Graded, Limited Movements of the Jaw |
|
| Passive Lips, Lack of Lip Closure and Spoon Clearance |
|
|
Tongue Forward Thrust and Lack of Grading
|
|
| Excessive Production of Saliva and Poor Saliva Control |
|
| Ineffective or Delay in Swallow |
|
| Vocalisation and Sounds, Wet Voice | |
|
Coughing, Choking, Gaggin, Crying, Blinking, Abnormal Facial Expressions and Aversive Reaction towards Food |
|
| Increased Tone & Involuntary Movements |
General Basic Treatment Principles[edit | edit source]
Postural Management[edit | edit source]
- Use of preparation techniques to normalize abnormal tone and to develop more normal pattern of movements (TIPs)
- Use of adequate seating equipment and/or handling techniques to maintain head/trunk aligned and upright - Chin tuck and elongation of the back of the neck in midline neutral position and chin tuck and provide adequate symmetric postural stability - stable base of support for bottom and trunk, hip symmetrically flexed at around 90°, tray to support harms and headrest. [1]
- Take care of child posture at ALL times also outside mealtime
Hand and Mouth Responses[edit | edit source]
- It is very important to look at feeding considering the strong connection with sensation and hands as well. Hand’s sensory cortex is very close in the homunculus to the mouth sensory cortex, therefore when stimulating one the other is also activated. Stimulation of hand sensation, manipulation, grasp release, hands to face before/during feeding can help mouth movements.
Provide Adequate Sensory Oral Experience[edit | edit source]
- A child with Cerebral Palsy normally misses the mouthing experience, missing important sensory feedback that helps development of chewing patterns. It is therefore good to provide touch on the face and around the mouth through kissing and stroking, letting the child chomp on the carer’s finger, supporting the child to bring his own finger to the mouth and holding teething toys for the child to chew on, tooth cleaning etc. [1]
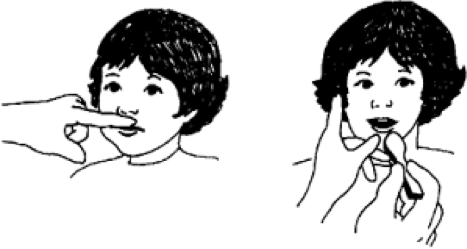
Provide Jaw and Cheek Support Through Oral Control and Stimulate Upper Lip Closure[edit | edit source]
- It is a facilitation technique to time and grade mouth opening that helps as well maintaining good alignment and a base of stability for more selective jaw movements.
- It can be performed from the side and front (oral control can be practice also outside of meal time to increase tolerance)
- Applying gentle, firm pressure downward on the tongue can help some children achieve better lip closure to clear the spoon and avoid further tongue movement [1]
Position of the Feeder, Communication, Environment[edit | edit source]
- If the feeder is in front of the child, in midline, this will facilitate the communication with the child (Feeder should inform child what is going to happen and can read child’s signs more easily). Communication is particularly important for those children with sensory impairments (vision)
- The orientation of the spoon should be slightly below level of the mouth, never from above or from the side
- Create a quiet environment and slowly introduce an element of distraction when the child’s ability progresses - start with backround sounds like radio.
Timing, Speed of Feeding, Food Quality[edit | edit source]
- The child should be able to clear the food before taking a new spoon and should recover breath - give the child time
- The quantity of the food on the spoon should be enough but safe for the child to handle
Use Different Food Texture, Temperature and Taste[edit | edit source]
- Use different food texture, temperature and taste to improve sensory responses but before make sure to assess carefull which texture maybe potential cause of aspiration
Choice of Right Feeding Equipment[edit | edit source]
- Some children that have difficulties in sucking may benefit from the introduction of a cup. Initially drinks may need thickening so they move more slowly, giving the child time to organize a safe swallow [1]
- A small, shallow-bowled spoon will be most appropriate to help the child remove the food from the spoon though lip closure.
- Some adapted equipment may help children in achieving independence during meal time, for example angled spoon, scoop plates etc.
Dietetic Supplements[edit | edit source]
- If the child doesn’t grow and is underweight dietetic advices to the family should be given or the child should be referred to the hospital paediatric nutrition ward. Inadequate nutrients intake will have negative impact of motor development of motor skills, the ability to fight infections and general well-being [1]
Promote Child Self Feeding[edit | edit source]
- For children who have difficulties grasping and manipulating the spoon, specific hand-over-hand assistance can be provided and then gradually withdrawn as motor control improves.
- Assisted eating for part of the meal or snack may help to develop functional skills, without compromising nutrition.
|
[2]
Preparatory Work for Better Feeding Experience |
[3]
Feeding Practise for High Calorie Intake |
Long Term Implications of Feeding Difficulties[edit | edit source]
Children with feeding difficulties very often develop one or more of the following long-term problems:
Poor General Health[edit | edit source]
- Low Calorie Intake
- Poor Gas Exchange
- Continuous Infections
- Poor Immune System etc.
Compromised Chest Status[edit | edit source]
- Damage at the deepest level of the lungs can impact breath capacity when adult
Poor Bone Density[edit | edit source]
- Reduced Mineral Build Up
Limited Participation in Society
- Sickness limiting access to school and other social events
Recurrent Chest Infections[edit | edit source]
- X ray - Repeated
- Bronchoscopy if there is evident inflammation or recurrent feeding history (chest infections)
Dietary Problems and Management[edit | edit source]
Inadequate Weight Gain:[edit | edit source]
- Improve Oral Control - Make Eating / Drinking Easier
- Use Supplements - Especially for children with Cerebral Palsy because they normally are smaller than typical and they don’t always get adequate Feeding Therapy
- Increase Calories Value of Food / Drinks and Variety / Quality of food intake providing all necessary Minerals, Vitamins etc.,
- Use Enteral Feeding - Naso Gastric Tube (NGT), can be used temporarily to provide nourishment support if safe but should not be a long term solution - Max 6 weeks as it reduces the sensitivity of Oral Motor Responses and GAG Reflex)
Dehydration: [edit | edit source]
- Use of Naturally Thicker Fluids e.g. yogurt, milkshakes, to improve control over fluids
- Use of Artificial Thickener to allow a better fluid intake
Constipation:[edit | edit source]
Very common in children with Cerebral Palsy due to neurological damage of the Gastric System and Reduced bowel peristaltic movements with increased bowel pressure and pain
- Increase Fluid Intake
- Increase Fiber Intake
- Limit as much as possible the pain with bowel massage and medicines if needed
Oral Hygiene:[edit | edit source]
Children with Cerebral Palsy and oral motor problems are at high risk of dental decay due to:
- Inability of the tongue to clean the teeth by moving around the mouth
- Loss of saliva (drooling), losing the enzymes needed to break down food
- High sugar/caloric diet
- Reduce intake of liquids
- Problem tolerating tooth cleaning
- Medication
- Difficult dental check-up by Doctors
It is very important to introduce tooth cleaning as soon as possible, using fingers before the toothbrush, using water at first and tooth paste later on (see notes for more details regarding the techniques).
Gastro-Oesphageal Reflux (GOR)[edit | edit source]
GOR is defined as the frequent return of stomach contents into the oesophagus caused by a dysfunction of the lower oesophagus (normally the lower oesphagael sphincter prevents free reflux of gastric content into the oesphagus.
Premature Children are more at risk of GOR because if relates to multiple contributing factors:
- Problems in coordination of the breath
- Problems with abdominals activations
- Problems of tone etc.
GOR is present in adults as well and can be triggered by:
- Gravity (Lying down after Meal)
- Alcohol
- Food Rich / High in Fat
- Pressure on the Abdomen (Eat too Much, Pregnant Women).
Symptoms of GOR (Presenting in Clusters):[edit | edit source]
- Posseting and Vomiting - Significant quantity sometimes hours after the feeding) but sometimes they don’t vomit at all!
- Delayed Gastric Emptying
- Regurgitating - Sucking / Swallowing for some time after meals / drinks
- Blood in Vomit / Stool - Indication of active ulcers in the gastric tract to due acidity (very painful)
- Aenemia - Bleeding
- Oesophagitis - Inflammation
- Halitosis - Smelly Breath
- Frequent Hiccoughs - Irritation of Diaphragm
- Aspiration - Recurrent Chest Infection which can be due to aspiration of vomit
- Coughing and Choking
- Intractible Asthma - Bronchi are inflamed because constantly exposed to the acid fumes from the stomach
- Apnoea
- Nasopharyngeal Congestion - Runny Nose
- Irritability - Very difficult to settle, alternating up-down pattern with good days and bad days
- Screaming / Crying during or after feeding - very common
- Loss of Appetite
- Interrupted Feeding
- Expression of Pain - Can be altered in children with severe learning difficulties
- Refusal to eat/drink - Hold food in the mouth because swallow is painful
- Discrepancy between Oral Skills and Actual Intake
- Pushing into extension or discomfort associated with position - Hip flexion increases abdominal pressure which increases flexors spasms
- Chronic Pharyngitis - Throat Inflammation
- Hoarse Voice - Thickened vocal folds produce a raspy voice
- Loos of Dental Enamel
Causes of GOR:[edit | edit source]
- Transient and inappropriate relaxation of the Lower Oesphygael Sphincter (LOS)
- Poor Oesophageal and Gastric Mobility
- Pressure Changes within the Abdomen / Thorax - Increase tone - spasms - constipation - scar tissue after surgery etc.
- Hiatus Hernia
- Effects of Medication - Baclofen, Antiepilepsy drugs because produce muscle relaxation
Effects of GOR:[edit | edit source]
- Ulceration of Oesophagus
- Aenemia
- Stricture Formation - Scars inside the Oesophagus walls narrowing the Lumen
- Associated Dysphagia
- Weight Loss
- Chronic Brassy Cough - Chesty type of Cough
- Reflex Bronch / Laryngospasms - Spasms that occlude the airways
- Central Apnea and Bradycardia - Temporary
Investigation:[edit | edit source]
- Clinical Evaluation and Feeding History - Ask the right questions
- Handling and Observation of the Child
- pH studies - Measure PH changes but not sensitive if the child if milk fed
- Motility Studies
Children with Gastrostomy normally have increased reflux symptoms therefore before applying the gastrostomy investigation should be done.
Treatment of GOR:[edit | edit source]
Positioning and Handling
- Raise the head end of bed for example reduce the risk of reflux
- Using antigravity position immediately after feeding
- Use extension
- Reduce flexors spasms and tone around the pelvis
- Normalise tone and facilitate more normal pattern of movement
- Change the nappy in side lie and not supine
Changes in Feeding Regime
- Feed more frequently in small portion but not more often than every 2 hours
- Decrease volume of each feed
- Thickening the liquids
- High carbohydrates feeds may promote gastric emptying
- Reduce intake of acid food/drink
- Avoid food before bed time
- Control constipation via diet
Drugs can help but can not resolve alone the problem
Surgery is advised by Paediatric Gastroenteroligist the in extreme cases when the child is not safe even after a correct management trial. It is performed wrapping the stomach to allow the food to go down but not up (safer procedure is Endoluminal Gastroplication-reduced risk of scar tissue and less invasive)
Additional Resources[edit | edit source]
Hambisela_Module_6_Feeding_Your_Child In: Getting to Know Cerebral Palsy: A learning resource for facilitators, parents, caregivers, and persons with cerebral palsy
References [edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Finnie NR. Handling the Young Child with Cerebral Palsy at Home. Elsevier Health Sciences; 1997.
- ↑ Yvonne Frizzell. Amber Kari Institute - Preparatory work for better feeding experience. Available from: https://youtu.be/ebUz2gVPdIk [last accessed 13/08/16]
- ↑ Yvonne Frizzell. Amber Kari Institute - Feeding practise for high calorie intake. Available from: https://www.youtube.com/watch?v=5rX3eg1qTIY&feature=youtu.be [last accessed 13/08/16]