Glasgow Coma Scale
Original Editor - Megan Craig as part of the Queen's University Neuromotor Function Project
Top Contributors - Jillian Burton Megan Craig Emily Lingerfelt Kendyl Wilson
Objective[edit | edit source]
The Glasgow Coma Scale (GCS) was first created by Graham Teasdale and Bryan Jennett in 1974. It is a clinical scale to assess a patient’s “depth and duration of impaired consciousness and coma” following an acute brain injury[1].
Healthcare practitioners can monitor the motor responsiveness, verbal performance, and eye-opening of the patient in the form of a simple chart. The GCS is the most commonly used tool internationally for this assessment and has been translated into 30 languages. It should not, however, be confused with the Glasgow Outcome Scale (GOS), which evaluates persistent disability after brain damage. [2]
Intended Population[edit | edit source]
The Glasgow Coma Scale was originally developed to help determine the severity of a coma or dysfunction following a traumatic brain injury, but can be useful for any condition leading to impaired consciousness. [3]
Today, it is consistently used for many conditions including:
- stroke (subarachnoid haemorrhage, intracerebral haemorrhage, or ischemic stroke),
- infection
- seizures
- brain abscess
- general traumas and ITU patients
- non-traumatic coma
- overdose
- poisoning[3]
It can also be administered in a variety of settings such as pre-hospital, arrival at the emergency department and in the hours following admission, giving it the ability to monitor changes and trends in patient consciousness over time.[3]
Modified scales have been developed for use in other populations. The Glasgow Coma Scale - Extended (GCS - E) includes the use of an amnesia scale in order to avoid the premature discharge of patients with mild traumatic brain injury. [4] There have also been modified scales developed for use in the paediatric population.
The motor scale has proved the most useful for assessment in both older children and preverbal children when studying blunt trauma. [5] Research has indicated that using the motor scale alone can simplify the assessment process while maintaining the accuracy of the score. [6]
Method of Use[edit | edit source]
The GCS Assessment Aid has four steps to the assessment process: Check, observe, stimulate, rate. [7]
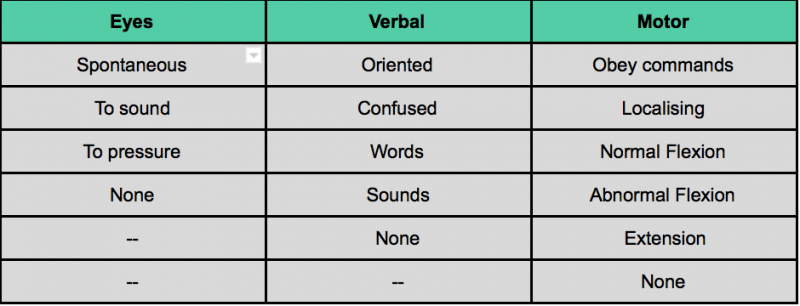
The assessor should evaluate each of the subscales as listed in the Assessment Aid. Each subscale has several components. Based on the level of consciousness, a score is assigned. A higher score indicates a greater level of consciousness.
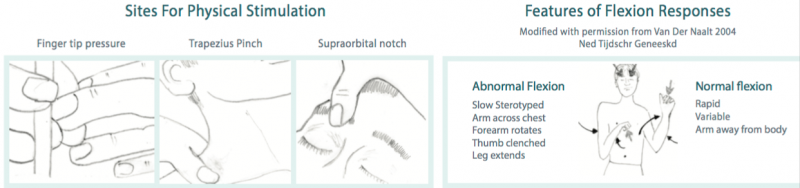
The GCS uses three sites for stimulation. This includes fingertip pressure, trapezius pinch and supraorbital notch. When stimulating these areas, health care practitioners should look for one of two responses: an abnormal flexion response or a normal flexion response. [7]
The National Institute for Health Care and Excellence (NICE) published Clinical Guidelines on Head Injuries for Assessment and Early Management. NICE recommends the following Clinical Guidelines:
- Until a patient has achieved a GCS score of 15 on the GCS, patients should be observed every half hour.
- Once the GCS Score has reached 15, the patient should be re-assessed using the GCS every half hour for two consecutive hours.
- If the patient's GCS score remains above 15, the patient should then be observed once every hour for four hours and then every 2 hours after that.
- Note: If at any time a patient's GCS score drops below 15, the healthcare practitioners should revert to observing the patient every half hour.[8]
The Institute of Neurological Sciences NHS Greater Glasgow and Clyde created a YouTube video to demonstrate how to properly use the outcome measure.
Scoring[edit | edit source]
- Mild TBI: GCS 13-15. These patients are awake, can present with confusion but are able to follow directions and communicate.
- Moderate TBI: GCS 9-12. These patients are typically drowsy or obtunded, they can open eyes and localise painful stimuli upon assessment.
- Severe TBI: GCS 3-8. These patients present as obtunded to comatose, they are unable to follow directions. They may exhibit decorate or decerebrate posturing. [10]
Evidence[edit | edit source]
Reliability[edit | edit source]
The inter-rater reliability of the total Glasgow Coma Scale is p = 0.86. Some research has subdivided the inter-rater reliability for each subscale. For the eye score the inter-rater reliability is p = 0.76, the verbal score is p = 0.67, and the motor score is p=0.81. [11] The research for test-retest reliability is not recent and should be updated, however, the best available evidence is k = 0.66 - 0.77. [12]
Based on a recent systematic review, the total score is typically less reliable than the individual components with a total Kappa value of 77% as compared to the eye, motor, and verbal scores which had Kappa values of 89%, 94%, and 88% respectively. [13]
Validity[edit | edit source]
The validity of the Glasgow Coma Scale comes under fire because a lot of hospitals administer the test while patients have been sedated, often underestimating patient scores. It’s also difficult to elicit accurate scores when patients are intubated. [14] Recent research has refuted that intubation elicits significantly different survival rates with the verbal score of r = 0.90 and the total score of r = 0.97. [15] The motor score is consistently the most predictive component of the GCS. [16]
Responsiveness[edit | edit source]
Given the current best available evidence, the GCS has a low sensitivity (56.1%) and a high specificity (82.2%). Therefore, there are very few false positives predicting a low rate of survival in healthy individuals. [17]
It is argued that the GCS does not accurately score patients who are intubated and does not assess brainstem reflexes, which may account for its low predictive capacity. A GCS administered at 24 hours post-injury has an odds ratio of 0.4 for predicting in-hospital mortality. When administered at 72 hours post-injury, the odds ratio improves to 0.59 for predicting in-hospital mortality. [18]
Evidence suggests that the Glasgow Coma Scale has a 71% accuracy in predicting functional independence post-injury. The GCS also modestly correlates with the Disability Rating Scale (-0.28) and the Cognitive component of the Functional Independence Measure (0.37). [19]
Resources[edit | edit source]
- The Glasgow Structured Approach to Assessment of the Glasgow Coma Scale
- NICE Guideline to Head Injury Assessment and Early Management
- Glasgow Outcome Scale [20]
- Glasgow Outcome Scale - Extended
- Traumatic Brain Injury: Physiopedia
- Stroke: Physiopedia
- Disability Rating Scale
- Functional Independence Measure (FIM): Physiopedia
References[edit | edit source]
- ↑ Teasdale G, Jennett B. Assessment of coma and impaired consciousness: a practical scale. The Lancet. 1974 Jul 13;304(7872):81-4.
- ↑ Frej M, Frej J. The Glasgow Structured Approach to Assessment of the Glasgow Coma Scale: what is GCS - glasgow coma scale. http://www.glasgowcomascale.org/what-is-gcs/ (accessed 7 May 2017).
- ↑ 3.0 3.1 3.2 Middleton PM. Practical use of the Glasgow Coma Scale; a comprehensive narrative review of GCS methodology. Australasian Emergency Nursing Journal. 2012 Aug 1;15(3):170-83.
- ↑ Nell V, Yates DW, Kruger J. An extended Glasgow Coma Scale (GCS-E) with enhanced sensitivity to mild brain injury. Archives of physical medicine and rehabilitation. 2000 May 1;81(5):614-7.
- ↑ Holmes JF, Palchak MJ, MacFarlane T, Kuppermann N. Performance of the pediatric Glasgow Coma Scale in children with blunt head trauma. Academic emergency medicine 2005 Sep 1;12(9):814-9. PMID:16141014 (accessed 5 May 2017).
- ↑ Acker SN, Ross JT, Partrick DA, Nadlonek NA, Bronsert M, Bensard DD. Glasgow motor scale alone is equivalent to Glasgow Coma Scale at identifying children at risk for serious traumatic brain injury. Journal of trauma and acute care surgery. 2014 Aug 1;77(2):304-9.
- ↑ 7.0 7.1 Institute of Neurological Sciences NHS Greater Glasgow and Clyde. Glasgow Coma Scale: do it this way [Internet]. Sir Graham Teasdale; 2015 [cited 2017 May 7]. Available from: http://www.glasgowcomascale.org/downloads/GCS-Assessment-Aid-English.pdf?v=3
- ↑ National Institute for Health and Care Excellence. Head Injury: assessment and early management [Internet]. https://www.nice.org.uk/guidance/cg176/resources/head-injury-assessment-and-early-management-pdf-35109755592901 (accessed 7 May 2017).
- ↑ GCS at 40. Glasgow Coma Scale at 40 | The new approach to Glasgow Coma Scale assessment. Available from: https://www.youtube.com/watch?v=v6qpEQxJQO4 [last accessed 05/07/17]
- ↑ Zollman FS, editor. Manual of traumatic brain injury: Assessment and management. Springer Publishing Company; 2021 Jul 22.
- ↑ Gill M, Reiley D, Green S. Interrater reliability of Glasgow Coma Scale scores in the emergency department. Annals of Emergency Medicine 2004;43(2):215-223. https://doi.org/10.1016/S0196-0644(03)00814-X (accessed 6 May 2017).
- ↑ Brott T, Adams H, Olinger C, Marler J, Barsan W, Biller J et al. Measurements of acute cerebral infarction: a clinical examination scale. Stroke 1989;20(7):864-870. PMID: 2749846 (accessed 6 May 2017).
- ↑ Reith F, Synnot A, van den Brande R, Gruen R, Maas A. Factors influencing the reliability of the Glasgow Coma Scale: a systematic review. Neurosurgery 2017;42:3-15. PMID: 28327922 (accessed 7 May 2017).
- ↑ Marion D, Carlier P. Problems with initial Glasgow Coma Scale assessment caused by prehospital treatment of patients with head injuries. The Journal of Trauma: Injury, Infection, and Critical Care 1994;36(1):89-95. PMID: 8295256 (accessed 6 May 2017).
- ↑ Meredith W, Rutledge R, Fakhry S, Emery S, Kromhout-Schiro S. The conundrum of the Glasgow Coma Scale in intubated patients. The Journal of Trauma: Injury, Infection, and Critical Care 1998;44(5):839-845. PMID: 9603086 (accessed 7 May 2017).
- ↑ Lesko M, Jenks T, Perel P, O'Brien S, Childs C, Bouamra O et al. Models of mortality probability in severe traumatic brain injury: results of the modeling by the UK Trauma Registry. Journal of Neurotrauma 2013;30(24):2021-2030. PMID:23865489 (accessed 6 May 2017).
- ↑ Grote S, Böcker W, Mutschler W, Bouillon B, Lefering R. Diagnostic value of the Glasgow Coma Scale for traumatic brain injury in 18,002 patients with severe multiple injuries. Journal of Neurotrauma 2011;28(4):527-534. PMID: 21265592 (accessed 6 May 2017).
- ↑ McNett M, Amato S, Gianakis A, Grimm D, Philippbar S, Belle J et al. The FOUR Score and GCS as predictors of outcome after traumatic brain injury. Neurocritical Care 2014;21(1):52-57. doi:10.1007/s12028-013-9947-6 (accessed 5 May 2017).
- ↑ McNett M. A review of the predictive ability of Glasgow Coma Scale scores in head-injured patients. Journal of Neuroscience Nursing 2007;39(2):68-75. PMID: 17477220 (accessed 6 May 2017).
- ↑ Jennett B. Assessment of outcome after severe brain damage: a practical scale. The Lancet 1975 ;305(7905):480-484. http://www.sciencedirect.com/science/article/pii/S0140673675928305?via%3Dihub (accessed 7 May 2017).
- Queen's University Neuromotor Function Project
- Assessment
- Outcome Measures
- Neurology
- Neurological - Assessment and Examination
- Neurological - Outcome Measures
- Primary Contact
- Screening Tools
- Acute Care
- Acquired Brain Injuries
- Cardiopulmonary
- Stroke
- Stroke - Assessment and Examination
- Stroke - Outcome Measures
- Cardiovascular System - Assessment and Examination
- Cardiovascular Disease - Outcome Measures
- Head
- Head - Assessment and Examination
- Head - Outcome Measures
- Course Pages