Goal Setting in Rehabilitation
Original Editor - Lauren Lopez
Top Contributors - Luisa Holt, Lauren Lopez, Kim Jackson, Naomi O'Reilly, Tony Lowe, Stacy Schiurring, Tarina van der Stockt, Uchechukwu Chukwuemeka, Claire Knott, Amanda Ager, Simisola Ajeyalemi, Rucha Gadgil, Nicole Hills, Rishika Babburu and Admin
Introduction[edit | edit source]
Goal setting between physiotherapists/physical therapists and their patients or clients is a complex and fundamental part of rehabilitation. It is “the formal process whereby a rehabilitation professional or a multidisciplinary team, together with the patient and/or their family, negotiate goals”[1]. For further consideration regarding the complexities of rehabilitation, Wade [2] has provided an evidence-based description of effective rehabilitation.
Goal setting is used to direct rehabilitation interventions towards a specific outcome(s), and can result in greater client satisfaction and improved recovery. Shared goal setting can also co-ordinate members of the multidisciplinary team and ensure they are working together towards a common goal and that nothing important is missed[1]. Goals can also be used to evaluate the success of rehabilitation interventions[1].
There is no consensus on a gold standard for goal setting methods, but it is widely held that it is a priority for guiding rehabilitation interventions toward achievable and meaningful outcomes[1]. There is a growing body of literature dedicated to the theories underpinning, methods of, and evidence for,[1][3][4] [5]goal setting in rehabilitation.
The Basics of Goal Setting[edit | edit source]
Goal setting is grounded in psychology and based on the belief that humans can change their behaviour and work towards a goal[6]. Goal setting is important for rehabilitation because it can provide the patient with motivation[1], particularly when they are functional and directly relate to real life activities. A meaningful goal can maximise patient engagement and motivate a patient to participate in rehabilitation in order to achieve their goals. For example, an elderly patient in rehabilitation following a hip replacement who wants to return to living independently in their own home with their spouse. In order to do this, the patient needs to be independently mobile and therefore can see the importance of participating in physiotherapy.
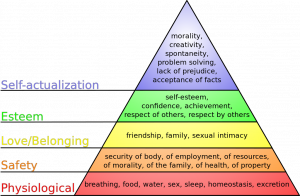
Goals can be thought of as hierarchical[7]. Maslow suggested that a person will make their physiological needs their primary goals. Once a person has met their physiological needs, he or she will make goals at the next level, safety and security, and so on.
Goal setting is also important as it keeps the focus of rehabilitation patient-centred. Goal setting helps health professionals plan their interventions for what is best or most meaningful for the patient instead of what suits the health professionals (where there are differences). Considering goals within the context of the biopsychosocial model will help to maintain this patient-centred focus [8]. Critical reflection and further training in advanced interaction and communication skills assist with undertaking this holistic approach[9][10][11][12].
Goals can be defined by time e.g. short, medium or long-term. In physiotherapy, goals are often activity-based. For example, a patient being able to do a functional task independently or being able to walk a certain distance with the aid of a walking frame.
Goal Setting Methods[edit | edit source]
Goal setting is the process of discussing, planning and documenting outcomes for a patient or client. It can be as simple as a conversation between a physiotherapist / physical therapist and a patient during a treatment session, or it can be more complex and structured in a meeting between a multidisciplinary team and a patient. The literature advocates a more formal, structured approach with the use of decision aids/tools e.g. prompt sheets, workbooks to gain greater engagement from the patient [13][14]. The patient’s social supports, e.g family members or friends, may also be invited to join in with goal setting if they have a role to play in helping the patient achieve a particular goal.
SMART Goals[edit | edit source]
One common method of goal setting has been derived from SMART goals. SMART goals originated in the field of project management[15]. There are some variations, but it is generally accepted that the acronym stands for:
S Specific
M Measurable
A Attainable or Assignable
R Realistic
T Time-related
MEANING[edit | edit source]
A term and acronym to underpin, remind and support rethinking of goal setting actions and activities, with potentially more relevance for rehabilitation[16].
M Meaning
E Engage
A Anchor
N Negotiate
I Intention-implementation gap
N New goals
G Goals as behaviour change
The International Classification of Functioning, Disability and Health (ICF)[edit | edit source]
The World Health Organization (WHO) ICF can be used to identify goals which envelope all aspects of a person’s life and to help in the clinical goal-setting processes. A study published in 2021 looked at using the ICF framework in paediatric rehabilitation goal-setting. The study found the ICF framework is enhance goal-setting practices by providing a common focus to facilitate collaborative goal-setting with families and healthcare providers[17].
Implications of the ICF Framework on Rehabilitation goal setting:[17]
- The International Classification of Functioning, Disability and Health (ICF) provides a common framework and language to support collaborative goal-setting between families and healthcare providers
- Despite the opportunity for the ICF to be used as a framework with goal-setting approaches, to date the ICF has mainly been used to match the content of goals to ICF domains for documentation purposes
- The ICF should be incorporated into the established clinical routines in order to promote its use among healthcare providers
- The ICF can be used with existing goal-setting tools in clinical practice and to inform the ongoing development of new tools to support the goal-setting process in family-centred services
The International Classification of Functioning, Disability and Health - WHO
Goal Attainment Scaling[edit | edit source]
Another system which is grounded in rehabilitation research is the Goal Attainment Scaling (GAS) by Turner-Stokes[18]. GAS is “a mathematical technique for quantifying the achievement of goals”[18]. GAS describes a process for setting goals and uses a five-point scale to measure if the goal is achieved or not. GAS scores can then be aggregated. Individual scores can be weighted to reflect either the relative importance of a goal to the patient or health professional or the difficulty in achieving the goal.
Rehabilitation Goal Setting Guidelines and Toolkit[edit | edit source]
Below is a link to some useful resources for clinicians released in 2019.
https://clinicalexcellence.qld.gov.au/resources/goal-setting-rehabilitation/guidelines-and-resources
Ask Questions[edit | edit source]
Questions are a good way of starting the goal setting process. The following questions from The Learning Corp[19] may help.
- What can’t you do since your injury that you want to get back to?
- What are you finding more difficult since your injury that you’d like to be easier?
- How will you know when you’re ready to stop coming to see me?
Using the person's responses to these questions, the clinician can help form them into SMART, concrete goals. Also of importance, is defining the goals in an active, first-person manner e.g. "I will do..."[19]. Taking on a 'coaching' role as opposed to an 'expert' role can help with more meaningful patient engagement in the process[20]. Some NHS Trusts have adopted a health coaching approach to improve their patient-centred care.
Supported self-management guide - NHS
Examples of Goal Setting[edit | edit source]
The table below is from The Learning Corp[19] and is an excellent demonstration of taking initial statements from the patient or client and turning them into practical, measurable goals.
| Initial Goal Statement | More Functional & Meaningful Real-World Goal Statement | Turning The Functional Goal Statement Into A SMART Goal | Example Of Evidence-Based Therapy Tasks Which Can Help |
|---|---|---|---|
| Talk Better | “I want to participate in the dinner table conversation with my family.” | On 4 out of 7 nights this week, I will use my word-finding strategies at the dinner table to share 3 things that happened to me that day. | All Speaking tasks, for example: |
| Be Able to Follow Directions | “I want to bake with my grandkids.” | On Saturday I will use strategies (e.g. note-taking, verbal mediation, planning) to follow a 6-step brownie recipe with 95% accuracy. | Instruction Sequencing |
| Improve Memory | “I want to remember to take my morning pills without a reminder from my spouse.” | On 5 out of 7 days this week, I will use my memory strategies to independently take my medicine every morning at 8 a.m. | All Visual Memory Tasks and Auditory Memory Tasks are relevant. For example: Repeat Number Sequences and Picture N-Back Memory |
| Be Able to Read | “I want to read to my son at bedtime.” | On 3 out of 7 nights this week, I will read a short storybook to my son. | Read Active Sentences AloudRead Passive Sentences AloudRead Number Sequences Aloud |
| Not Get So Distracted | “I want to watch my daughter’s soccer game without getting distracted.” | On Sunday I will use my strategies to attend to my daughter’s soccer game for 20 min without getting distracted. | Playing Card SlapjackSpoken Word N-Back Memory |
| Not Get Lost In New Places | “I want to walk around the town without getting lost.” | This week I will map out the route to town & walk there 3 times without getting lost. | Map Reading |
| Be Able To Write | “I want to write in my journal again.” | “On 3 out of 7 nights this week, I will write 2 complete sentences in my journal. | Picture Spelling |
| Get My Math Skills Back | “I want to return to paying for things when I go out with my family.” | When I go out to lunch with my family tomorrow, I will use strategies (e.g. note-taking, slowing down, double-checking work) to accurately calculate the tip on the bill. | CurrencySpeak CurrencyFunctional Math |
Measuring Goals[edit | edit source]
Measuring person-centred goals is a helpful way to measure outcomes in rehabilitation, particularly patient satisfaction with their performance of a specific goal[19]. Sometimes a person's goals may not seem realistic to the clinician, or, the person not achieve their goals. Instead of regarding this as failure, the unachieved goals can be used for a discussion about what might be a realistic outcome for the person's rehabilitation and to guide challenging discussions on expectations versus reality. Additionally, the unachieved goal could be broken down into smaller, more achievable parts[19]. Differentiating between goals and hope, aspirations and dreams within the goal setting process is also an important consideration[21][11].
As above, GAS is another way to measure goals.
Influences on Goal Setting[edit | edit source]
There are some factors which can facilitate or create barriers to successful goal setting, see Table 1 below.
Table 1: Factors Influencing Goal Setting
| Factor | Influence | Evidence |
|---|---|---|
| Time | Facilitator or barrier | [22] |
| Social supports | Family and friends may help or hinder | [23] |
| Pain | Barrier | [23] |
| Health professionals’ expertise or lack of | Facilitator or barrier | [22][24] |
| Cognition | Barrier | [4] |
| The patient’s self awareness | Facilitator or barrier | [25] |
| Patient involvement | Facilitator or barrier | [24][26][27] |
| Patient’s desire to pursue goals and modify as needed | Facilitator | [28] |
Evidence For Goal Setting[edit | edit source]
| Author | Date | Population | N= | Intervention | Outcome Measure | Main Results |
|---|---|---|---|---|---|---|
| Rasquin et al.[29] | 2009 | Acquired brain injury | 48 | Cognitive rehabilitation programme | Goal Attainment Scaling, number of goals made, time to set goals, domains in which goals were set | It is possible to set three realistic goals per patient within 30 minutes. Goals were set in cognitive and behavioural domains |
| Rosewilliam et al.[3] | 2011 | Stroke | N/A | Systematic review of 18 qualitative studies, eight quantitative studies and one mixed methods study | N/A | Nominal adoption of goals setting, discrepancies between perceptions and practice of goal setting, related ethical conflicts, strategies to improve goal setting, weak methodologies, some improvement in psychological outcomes, further research needed. |
| Coffey et al.[28] | 2014 | Lower limb amputation | 64 | Not applicable | WHODAS 2.0, WHO-QOL-BREF,
Tenacious Goal Pursuit Scale, Flexible Goal Adjustment Scale |
High levels of disability in this population. QoL stable over first six months. Stronger goal pursuit and goal adjustment tendencies predicted lower disability and higher QoL six months post discharge |
| Alanko et al.[23] | 2018 | Stroke and back pain | 20 | Not applicable | Qualitative interviews and analysis of rehabilitees perspectives on goal setting in rehabilitation | Five meanings:
1) “trust in the rehabilitation situation, professionals, oneself and relatives” 2) “respectful presence” 3) “confusing awareness” 4) “disturbing pain” 5) “fear of unpredictability” |
Clinical Rehabilitation Collections[edit | edit source]
Below is a link to find a collection of papers that relate to goal setting in rehabilitation.
https://journals.sagepub.com/topic/collections-cre/cre-1-goal_setting/cre?pbEditor=true#/
Practical Points to Remember[edit | edit source]
- Use goals to guide and evaluate your physiotherapy treatments.
- Discuss, plan and review goals for rehabilitation with your patient.
- Discuss, plan and review goals for rehabilitation with other members of your multidisciplinary team (if applicable).
- Use a method such as SMART, MEANING or GAS, and document the goals made with a date to review them and check for progress.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Wade DT. Goal setting in rehabilitation: an overview of what, why and how. Clin Rehabil. 2009;23(4):291-5
- ↑ Wade DT. What is rehabilitation? An empirical investigation leading to an evidence-based description. Clin Rehabil. 2020; 0269215520905112.
- ↑ 3.0 3.1 Rosewilliam S, Roskell CA, Pandyan AD. A systematic review and synthesis of the quantitative and qualitative evidence behind patient-centred goal setting in stroke rehabilitation. Clin Rehabil. 2011; 25(6): 501-514.
- ↑ 4.0 4.1 Bouwens SFM, van Heugten CM, Verhey FRJ. The practical use of goal attainment scaling for people with acquired brain injury who receive cognitive rehabilitation. Clin Rehabil. 2009; 23 (4):310 - 320.
- ↑ Levack WM, Weatherall M, Hay‐Smith EJ, Dean SG, McPherson K, Siegert RJ. Goal setting and strategies to enhance goal pursuit for adults with acquired disability participating in rehabilitation. Cochrane Database of Systematic Reviews. 2015(7).
- ↑ Scobbie L, Wyke S, Dixon D. Identifying and applying psychological theory to setting and achieving rehabilitation goals: development of a practice framework. Clin Rehabil. 2009; 23 (4): 321-333. ISSN 0269-2155.
- ↑ Maslow AH. A Theory of Human Motivation. Originally published in Psychological Review 1943; 50: 370-396. Accessed from Green, CD.https://psychclassics.yorku.ca/Maslow/motivation.htm (accessed 25 July 2018).
- ↑ Wade DT, Halligan PW. The biopsychosocial model of illness: a model whose time has come. Clin Rehabil. 2017; 995-1004
- ↑ Melin J, Nordin Å, Feldthusen C, Danielsson L. Goal-setting in physiotherapy: exploring a person-centered perspective. Physiotherapy theory and practice. 2019 Aug 25:1-8.
- ↑ Alexanders J, Douglas C. The role of psychological skills within physiotherapy: A narrative review of the profession and training. Physical Therapy Reviews. 2016 Nov 1;21(3-6):222-7.
- ↑ 11.0 11.1 Mudge S, Stretton C, Kayes N. Are physiotherapists comfortable with person-centred practice? An autoethnographic insight. Disability and rehabilitation. 2014 Mar 1;36(6):457-63.
- ↑ Joseph-Williams N, Lloyd A, Edwards A, Stobbart L, Tomson D, Macphail S, Dodd C, Brain K, Elwyn G, Thomson R. Implementing shared decision making in the NHS: lessons from the MAGIC programme. BMJ. 2017 Apr 18;357:j1744.
- ↑ Holliday RC, Cano S, Freeman JA, Playford ED. Should patients participate in clinical decision making? An optimised balance block design controlled study of goal setting in a rehabilitation unit. Journal of Neurology, Neurosurgery & Psychiatry. 2007 Jun 1;78(6):576-80.
- ↑ Stevens A, Köke A, van der Weijden T, Beurskens A. Ready for goal setting? Process evaluation of a patient-specific goal-setting method in physiotherapy. BMC health services research. 2017 Dec;17(1):618.
- ↑ Doran GT. There’s a S.M.A.R.T. Way to Write Management’s Goals and Objectives. Management Review. 1981; 70: 35-36.
- ↑ McPherson KM, Kayes NM, Kersten P. MEANING as a smarter approach to goals in rehabilitation. Chapter 6 in Rehabilitation goal setting: Theory, practice and evidence. 2014 Jul 10:105-119.
- ↑ 17.0 17.1 Nguyen L, Cross A, Rosenbaum P, Gorter JW. Use of the International Classification of Functioning, Disability and Health to support goal-setting practices in pediatric rehabilitation: a rapid review of the literature. Disability and Rehabilitation. 2021 Mar 12;43(6):884-94.
- ↑ 18.0 18.1 Turner-Stokes L. Goal attainment scaling (GAS) in rehabilitation: a practical guide. Clin Rehabil. 2009; 23 (4): 362-370.
- ↑ 19.0 19.1 19.2 19.3 19.4 The Learning Corp. More successful brain rehabilitation: turning therapy goals into real-life activities. 2018. Available from: https://thelearningcorp.com/brainwire/targeting-more-successful-recovery-turning-therapy-goals-into-real-life-activities/#ppm21717 (accessed 28 October 2019).
- ↑ Stretton C, Mudge S, Kayes NM, Taylor D, McPherson KM. Activity coaching to improve walking is liked by rehabilitation patients but physiotherapists have concerns: a qualitative study. Journal of physiotherapy. 2013 Sep 1;59(3):199-206.
- ↑ Soundy A, Smith B, Butler M, Lowe CM, Helen D, Winward CH. A qualitative study in neurological physiotherapy and hope: beyond physical improvement. Physiotherapy Theory and Practice. 2010 Jan 1;26(2):79-88.
- ↑ 22.0 22.1 Playford ED, Siegert R, Levack W, Freeman J. Areas of consensus and controversy about goal setting in rehabilitation: a conference report. Clin Rehabil. 2009. 23(4): 334-344.
- ↑ 23.0 23.1 23.2 Alanko T, Karhula M, Kröger T, Piirainen A, Nikander R. Rehabilitees perspective on goal setting in rehabilitation – a phenomenological approach. Disabil Rehabil. 2018. DOI: 10.1080/09638288.2018.1463398.
- ↑ 24.0 24.1 Plant SE, Tyson SF, Kirk S, Parsons J. What are the barriers and facilitators to goal-setting during rehabilitation for stroke and other acquired brain injuries? A systematic review and meta-synthesis. Clin Rehabil. 2016; 30(9): 921-930.
- ↑ Fischer S, Gauggel S, Trexler LE. Awareness of activity limitations, goal setting and rehabilitation outcome in patients with brain injuries. Brain Inj. 2004;18(6): 547-562.
- ↑ Evans JJ. Goal setting during rehabilitation early and late after acquired brain injury. Curr Opin Neurol. 2012;25(6):651-5.
- ↑ Barnard RA, Cruice, MN, Playford ED. Strategies Used in the Pursuit of Achievability During Goal Setting in Rehabilitation. Qual Health Res. 2010. 20(2): 239-250.
- ↑ 28.0 28.1 Coffey L, Gallagher P, Desmond D. Goal Pursuit and Goal Adjustment as Predictors of Disability and Quality of Life Among Individuals With a Lower Limb Amputation: A Prospective Study. Arch Phys Med Rehabil. 2014; 95 (2): 244-252.
- ↑ Rasquin SM, Bouwens SF, Dijcks B, Winkens I, Bakx WG, Van Heugten CM. Effectiveness of a low intensity outpatient cognitive rehabilitation programme for patients in the chronic phase after acquired brain injury. Neuropsychological rehabilitation. 2010 Oct 1;20(5):760-77.