Oxygen Therapy at Home
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Kapil Narale
Introduction[edit | edit source]
Supplemental oxygen is ordered to maintain adequate tissue oxygenation with the minimum amount of energy expenditure by the heart and lungs.
- People with low levels of oxygen in the bloodstream will benefit from home oxygen therapy.
- Home oxygen therapy increases the amount of oxygen in the blood and therefore the amount of oxygen getting to the vital organs
Objective: to prevent or correct the abnormal condition in which available oxygen to the body’s cells is inadequate to meet the body’s needs.
- For patients with chronic pulmonary and/or cardiac diseases, there is often a need for oxygen therapy to continue after discharge from hospitalization.
- Providing oxygen for patients at home has many benefits when given appropriately[1].
- The use of supplemental oxygen in the home remains the most common and popular respiratory home care modality.[2]
- More than 1.5 million adults in the United States use supplemental oxygen for a variety of respiratory disorders to improve their quality of life and prolong survival.[3][2].
Methods of Supplemental Oxygen Therapy Delivery[edit | edit source]
- Long-term oxygen therapy (LTOT) in which oxygen is delivered for patients with chronic hypoxemia, for at least 15 hours daily.
- Ambulatory oxygen therapy (AOT): Oxygen supplementation during exercise and daily activities for patients who are not hypoxemic at rest but who develop hypoxemia on exercise.
- Nocturnal oxygen therapy (NOT) in which oxygen administered overnight alone with no oxygen therapy during daytime hours
- Short burst oxygen in which a brief and intermittent oxygen supplementation used as needed in the absence of hypoxemia.
- Palliative oxygen therapy (POT): The use of oxygen for relieving of breathlessness in advanced or life-limiting disease in the absence of known hypoxemia[1]
Indications[edit | edit source]
Indications for Long-term oxygen therapy (LTOT)
- Chronic Obstructive Pulmonary Disease (COPD)
- LTOT is indicated for patients with chronic obstructive pulmonary disease (COPD) when:
- A resting PaO2 = 7.3 kPa (55 mm Hg) or SaO2 88% or less while being at rest in a stable clinical condition
- A resting PaO2 = 8.0 kPa (59 mm Hg) or SaO2 89% or less if there is evidence of cor pulmonale, right heart failure or polycythemia (hematocrit greater than 55%) while being in a stable clinical condition.
Studies showed a survival benefit of LTOT in COPD patients with chronic hypoxemia. - LTOT may improve patient outcome measures other than survival benefits, including quality of life, depression, cognitive function, exercise capacity, and hospital admission rate.
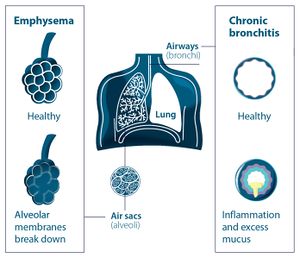
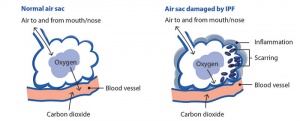
- Interstitial Lung Disease (ILD)
- Patients with severe ILD may develop chronic hypoxemia, possible leading to reduced tissue oxygenation with many subsequent complications and worsen prognosis.
- The use of LTOT in patients with ILD may improve survival and prevent complications.
- Pulmonary Hypertension
- LTOT in pulmonary hypertension may improve tissue oxygenation and prevent complications due to chronic hypoxemia.
- Cystic Fibrosis (CF)
- Severe CF patients may develop chronic hypoxemia.
- LTOT in patients with CF may lead to survival improvement and prevent complications caused by chronic hypoxemia.
- Advanced Cardiac Failure
- Using LTOT in patients with advanced cardiac failure and resting hypoxemia may lead to an improvement in tissue oxygenation and preventing complications due to hypoxemia[1]
Respiratory Therapist[edit | edit source]
A respiratory therapist can evaluate and assist patients with their home oxygen needs.
- The respiratory therapist can provide expertise in the various types of home oxygen delivery devices and provide ongoing assessment of the patient. Patient compliance can be maximized by selecting the appropriate device.
- Before, referring patients to home oxygen evaluation services, patients should receive both written and verbal information[1]
Oxygen Equipment[edit | edit source]
Typical routes for home oxygen therapy include:
- The low-flow nasal cannula: supplies a low flow of oxygen (1 to 6 liter per minute). For each liter per minute of oxygen flow, about 3% to 4% is added to the oxygen concentration. Oxygen delivered by nasal cannula to the nasopharynx mixes with room air. Consequently, the concentration of oxygen by nasal cannula varies depending upon the patient's respiratory rate, tidal volume, oxygen flow rate, and extent of mouth breathing.[1]
- Simple oxygen mask: used to supply a flow of oxygen rates between 6 and 10 L per minute with oxygen concentrations between 35% and 50%, and this depends on the patient's respiratory rate and the mask fit. In a simple mask, oxygen delivery is through a small-bore tube connected at the base of the mask. Exhaled gas escapes through holes on each side of the mask. Room air enters through these holes and mixes with oxygen, an oxygen flow rate greater than 5 L per minute is needed to prevent CO2 rebreathing.[1]
- Venturi mask (also known as an air-entrainment mask, utilizes a flow meter to deliver a precise amount of oxygen): allow for a fixed O2%, are available for delivery of controlled oxygen concentrations of 24% to 40%. May benefit patients with hypercapnic respiratory failure requiring LTOT[1]
Oxygen comes from either oxygen concentrators or medical oxygen cylinders.
- A home oxygen concentrator has long tubing that allows client to move freely around the house. It concentrates oxygen by filtering the nitrogen out of the air in the room. It requires electricity to operate.
- A portable oxygen concentrator is a smaller, lightweight machine that is designed to be carried around outside the home. They contain their own power supply.
Oxygen cylinders also come in different sizes.
- A portable cylinder is designed to be used when leaving the home. It can be wheeled and attached to a walker, wheelchair or carried in a backpack.
- A larger freestanding cylinder can be used in the home as a back-up source in the event of a power failure[4].
Screening Clients for Use of LTOT[edit | edit source]
A pulse oximeter is widely available and can be useful for screening patients who might be indicated for LTOT.
- Studies showed that using the SpO2 level equal to 92% has 100% sensitivity and specificity of only 69% for identifying patients with a PaO2 less than 7.3 kPa.
- Stable patients with oxygen saturation (SpO2) equal to 92% at rest should be referred for a blood gas evaluation, and assessment for LTOT need.
- Stable patients with clinical evidence of peripheral edema, hematocrit equal to 55% or pulmonary hypertension with oxygen saturation (SpO2) equal to 94% at rest should be referred for a blood gas evaluation, and assessment for LTOT need.
Follow-up of LTOT Patients
- Follow-up should occur at three months after initiating LTOT, to ensure LTOT is still necessary.
- Patients receiving LTOT should have follow-up at 6 to 12 months after the first 3-month follow-up[1]
Complications[edit | edit source]
There are potential toxicities in patients administered oxygen in high concentrations (above 50%) for long periods
- Atelectasis
- Oxidative stress
- Peripheral vasoconstriction
- Uncontrolled oxygen delivery may lead to a worsening of hypercapnia in patients with chronic obstructive pulmonary disease.
However the benefits outweigh the risks.
It is advised to target the SpO2 to 90% to 92% to prevent tissue hypoxia while minimizing any side effects, which might be associated with excessive oxygen supplementation.
- Patients should be made aware of the dangers of using home oxygen in the presence of any naked flame, such as cookers and candles.
- Oxygen cylinders should be at least 5 feet away from naked flames, a heat source, or electrical devices.
- There is a significant risk of fire associated with smoking while using home oxygen therapy. Smoking cessation should be advocated.
- And a written education should be given to patients before ordering home oxygen[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Shebl E, Cates TD. Home Oxygen Therapy. 2020 Available from:https://www.ncbi.nlm.nih.gov/books/NBK532994/ (last accessed 7.10.2020)
- ↑ 2.0 2.1 CME Home O2 what you should know Available from:https://cmetoolkit.com/wp-content/uploads/What-You-Should-Know-About-Home-Oxygen-Therapy.pdf (last accessed 7.10.2020)
- ↑ Jacobs SS, Lederer DJ, Garvey CM, Hernandez C, Lindell KO, McLaughlin S, Schneidman AM, Casaburi R, Chang V, Cosgrove GP, Devitt L. Optimizing home oxygen therapy. An official American Thoracic Society workshop report. Annals of the American Thoracic Society. 2018 Dec;15(12):1369-81.Available from:https://www.atsjournals.org/doi/full/10.1513/AnnalsATS.201809-627WS (last accessed 7.10.2020)
- ↑ Lung Foundation Oxygen Therapy Available from:https://lungfoundation.com.au/wp-content/uploads/2018/09/Factsheet-Home-Oxygen-Therapy-Jun2016.pdf (last accessed 7.10.2020)