Smoking Cessation and Brief Intervention
Original Editor - Lizzie White
Top Contributors - Lucinda hampton, Kim Jackson, Admin, Vidya Acharya, 127.0.0.1, Laura Ritchie and WikiSysop
Introduction[edit | edit source]
Tobacco use, primarily as cigarette smoking, is the leading cause of preventable disease and death. Assisting patients with smoking cessation is one of the most important tasks of clinicians, and the benefits of discontinuing smoking behavior are well established.
Brief intervention makes the most of any opportunity to raise awareness, share knowledge and get someone to think about making changes to improve their health and behaviours. Brief intervention uses counselling skills such as motivational interviewing and goal setting. An understanding of the stages of behaviour change is also important. Brief intervention takes as little as 3 minutes and is usually carried out in a one-to-one situation. The 5As for smoking cessation for health professionals is an international smoking cessation framework used in brief intervention that has been shown to be very effective in encouraging and supporting smoking cessation.[1]
Why Quit[edit | edit source]
It is well established that smoking increases the risk of different forms of cancer, including lung, liver, and colorectal. Eighty-five percent of lung cancers occur in smokers. Also, smoking increases the risk of respiratory diseases (such as chronic obstructive pulmonary disease) and cardiovascular disease. During pregnancy, smoking increases the rate of complications, some of which include miscarriage, stillbirth, preterm birth, fetal growth restriction, and congenital anomalies. Neonatal and pediatric complications of exposure to cigarette smoking include sudden infant death syndrome and abnormal lung function in children, such as asthma. Despite the magnitude of disease burden related to smoking, 42.1 million adults in the United States smoke cigarettes, according to the National Health Interview Survey data from 2013. This makes quitting smoking one of the most important, yet challenging steps a person can take to improve his or her health, and most smokers make several attempts to quit before achieving abstinence from smoking[2].
Assisting patients with smoking cessation is one of the most important tasks of the primary care physician, and the benefits of assessing patients’ smoking behavior are well established.
WHO global report on trends in tobacco smoking 2000-2025[edit | edit source]
Tobacco is the only legal drug that kills many of its users when used exactly as intended by manufacturers. WHO has estimated that tobacco use (smoking and smokeless) is currently responsible for the death of about six million people across the world each year with many of these deaths occurring prematurely. This total includes about 600,000 people are also estimated to die from the effects of second-hand smoke. Although often associated with ill-health, disability and death from noncommunicable chronic diseases, tobacco smoking is also associated with an increased risk of death from communicable diseases[3]
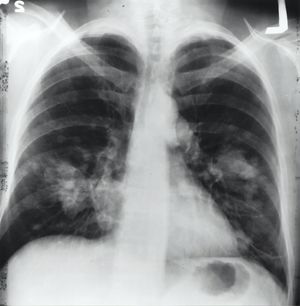
Image 3: X-ray image of a chest. Both sides of the lungs are visible with a growth on the left side of the lung, which could possibly be lung cancer.
Brief Interventions[edit | edit source]
The US Preventive Services Task Force (USPSTF) recommends using the 5 As model; ask, advise, assess, assist and arrange.
- Ask all patients whether they smoke,
- Advise the smokers to quit,
- Assess willingness to quit,
- Assist with quitting treatment/referrals and
- Arrange follow-up contact.
All staff should implement 5A’s[4].
NICE[5] also states that BI usually takes between 5 and 10 minutes.
- Evidence shows that BI of 3 minutes can be effective[6].
- BI often occurs through one or a small number of encounters, unlike other methods of smoking cessation such as intensive intervention, consisting of multiple counselling sessions[7].
- BI could be used by healthcare professionals (HCPs) who see a lot of patients in a short period of time[7].
This approach has been found to be most effective when combined with other interventions such as behavioural support, and nicotine replacement therapy (NRT). Although it is usually delivered in a one-to-one situation, increasing access to brief intervention training is an important and effective part of a population health promotion approach. This is because:
- simple advice delivered in the right way can have a significant effect on smoking cessation
- increasing the number of people in different organisations trained in brief interventions will increase the capacity to tackle smoking rates[1].
Clinical Significance[edit | edit source]
Physicians should make it a priority to help patients stop smoking.
- Smoking even a few cigarettes a day or only smoking occasionally increases a person's chance of developing lung cancer.
- There are immediate benefits to smoking cessation which occur only hours, weeks, and months after a person stops smoking.
- The primary benefits include lowering of blood pressure, decreased cough and phlegm production, increased lung capacity.
- In the long-term, quitting smoking reduces a patient's risk of developing cancer, heart disease, and chronic lung disease.
- The earlier a person stops smoking, the more their risk of developing lung cancer is reduced. However, stopping smoking at any age is beneficial, and the benefits of smoking cessation are cumulative over time.
- When a person stops smoking before the age of 40, they reduce their chances of dying from smoking-related disease by 90%. Even people already diagnosed with cancer benefit from smoking cessation.
- In some forms of cancer, quitting smoking at the time of diagnosis can reduce the chances of dying from cancer by as much as 40%[2]
Conclusion[edit | edit source]
In conclusion, it is clear that Brief Intervention (BI) by more than one type of health care provider increases smoking cessation and attempts to quit[8].
- Nicotine has been linked to many cancers and even second-hand exposure to nicotine can increase the risk of lung and heart disease. Despite four decades of urging the public to stop smoking, people continue to smoke in large numbers.
- There is no magic pill that can help people quit smoking. All the currently available medications to help people quit smoking are no better than a placebo. The big problem is that while many people can cease smoking for a few days, the urge to smoke is overwhelming and relapse rates are high. Clinicians, pharmacists, and nurses should assist in educating patients about the adverse effects of smoking.
- Today both family- and school-based smoking prevention programs are in operation, but scientific evidence reveals that their benefits are limited.
- The majority of patients simply quit smoking on their own but why they succeed in quitting smoking and others can't is not well understood.
- All healthcare workers should continue to insist that patients not smoke - even if only a few percentage stop smoking; with nicotine addiction, even 1% is considered a success[2].
References[edit | edit source]
- ↑ 1.0 1.1 Aust Gov. Tackling Smoking Available from:https://tacklingsmoking.org.au/introduction-to-activities/brief-intervention/ (last accssed 6.4.2021)
- ↑ 2.0 2.1 2.2 Sealock T, Sharma S. Smoking Cessation. StatPearls [Internet]. 2020 Jan 30. Available from:https://www.statpearls.com/articlelibrary/viewarticle/29164/ (accessed 6.4.2021)
- ↑ WHO Tobacco Smoking Available from:https://www.who.int/tobacco/publications/surveillance/reportontrendstobaccosmoking/en/ (accessed 6.4.2021)
- ↑ Simmons, V. N., Litvin, E. B., Unrod, M., Brandon, T. H. (2012). Oncology healthcare providers’ implementation of the 5A’s model of brief intervention for smoking cessation: Patients’ perceptions. Patient Education and Counselling. [Online]. 86. P 414-419. Available from- http://www.sciencedirect.com/science/article/pii/S0738399111003648 [Accessed: 12/11/13].
- ↑ National Institute for Health and Clinical Excellence. (2006). Brief interventions and referral for smoking cessation in primary care and other settings- Quick reference guide. London: National Institute for Health and Clinical Excellence. Available from- http://www.nice.org.uk/nicemedia/live/11375/31866/31866.pdf [Accessed: 12/11/13].
- ↑ The Tobacco Use and Dependence Clinical Practice Guideline Panel, Staff, and Consortium Representatives. (2000). A clinical practice guideline for treating tobacco use and dependence: A US Public Health Service report. Journal of the American Medical Association. [Online]. 283. (24). P 3244-3254. Available from- http://jama.jamanetwork.com/article.aspx?articleid=192834 [Accessed: 05/12/13].
- ↑ 7.0 7.1 Cofta-Woerpel, L., Wright, K. L., Wetter, D. W. (2007). Smoking Cessation 3: Multicomponent Interventions. Behavioral Medicine. [Online]. 32. P 135-149. Available from- http://web.ebscohost.com/ehost/pdfviewer/pdfviewer?sid=5c20b1d2-16ce-45bc-8a9f-8d929e95bfac%40sessionmgr113&vid=21&hid=112 [Accessed: 17/11/13].
- ↑ An, L. C., Foldes, S. S., Alesci, N. L., Bluhm, J. H., Bland, P. C., Davern, M. E., Schillo, B. A., Ahluwalia, J. S., Manley, M. W. (2008). The Impact of Smoking-Cessation Intervention by Multiple Health Professionals. American Journal of Preventive Medicine. [Online]. 34. (1). P 54-59. Available from- http://www.sciencedirect.com/science/article/pii/S0749379707006137 [Accessed: 17/11/13].