Patellofemoral Instability
Original Editors - Assia Dad as part of the Vrije Universiteit Brussel's Evidence-based Practice project
Top Contributors - Claudia Karina, Julie Plas, Admin, Michelle Lee, Assia Dad, Rachael Lowe, Kim Jackson, Kai A. Sigel, WikiSysop, Niels Cornand and 127.0.0.1
Definition/Description[edit | edit source]
A frequent cause of knee pain and knee disability is patellofemoral instability. Patellofemoral instability can be defined in different ways. One way is when the patient has undergone a traumatic dislocation of the patella. It can also describe a sign on physical examination, signifying the ability of the patella to be translated out of the trochlear groove of the femur in a passive manner. Moreover, patellofemoral instability can be a symptom, when the patient gives a feeling that the knee “gives way’’. This feeling occurs when the patella slips out of the trochlear groove. The relationships between the symptoms, injuries, and diseases of the patellofemoral joint are often confusing for the therapist.[1]
Clinically Relevant Anatomy[edit | edit source]
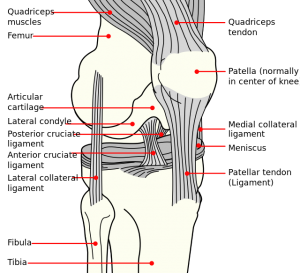
The patella is the largest sesamoid bone. It is located within the complex of the quadriceps and patellar tendon. Through its articulation with the femoral trochlea, the patellofemoral joint forms a highly complex unit with potential for joint instability. Patellofemoral joint stability is multifactorial and can be categorized into static and dynamic stabilizers.[2]
Static stabilizers:[edit | edit source]
- The medial side exists of three ligaments: The medial patellofemoral ligament (MPFL), the patellomeniscal ligament (MPML) and patellotibial ligament (MPTL): These are the primary ligamentous structures constraining lateral movement of the patella, the MPFL is the most important one. The MPFL is a continuation of the deep retinacular surface of the vastus medialis obliquus (VMO). It runs transversely between the proximal half of the medial border of the patella to the femur between the medial epicondyle and the adductor tubercle, forming the second layer between the superficial medial retinaculum and the capsule.[2]
- The anatomy of the lateral side is more complex:
- The vastus lateralis (anterior) and the superficial oblique retinaculum (further posteriorly) are part of the superficial.
- The deep layer mirrors the medial structures and consists of the lateral patellofermoral ligament (LPFL), the deep transverse retinaculum and the patellotibial ligament (LPTL).
- The LPTL attaches directly to the distal pole of the patella and sends fibers both into the lateral meniscus and into the underlying tibia. The LPFL is not attached directly to the femur, but indirectly via the proximal and distal attachments of the iliotibial band (ITB). Thus the tightness of the ITB (dynamic stabilizer) will influence the lateral stability force inferred by the lateral retinacular structures.
- The medial and lateral retinacular structure's' are most effective within the range of 20 ° flexion and full extension, during which the patellofemoral joint is most vulnerable due to the lack of resistance offered by other stabilizing structures.
- Trochlear geometry: The shape of the trochlea is concave. When the patella enters the trochlea, it allows for the inherent stability of the patellofemoral joint.
- Patellar geometry: The patella is convex and this congruity between the patella and the trochlea provides some constraint to the patellofemoral joint. When the knee begins to bend, the initial contact area is the distal and lateral patella facet. With further flexion, the contact area on the patella articular surface moves more proximally until in deep flexion where the medial facet has then made contact.
- Patellar height: the height of the patella also contributes to patellofemoral joint stability. Engagement of the patella depends entirely on patella height.
- Limb alignment: The angle between the pull of the quadriceps and the axis of the patella tendon (Q-angle) is very important. In males, the angle is 8 to 10° and in females, it is 15 ± 5°.[2]
Dynamic stabilizers:[edit | edit source]
- The quadriceps is a dynamic stabilizer of the patella. The patella is used as biomechanical lever, magnifying the force exerted by the quadriceps on knee extension.
- The patella also centralises the divergent forces of the quadriceps and transmits the tension around the femur to the patellar tendon.
Epidemiology /Etiology[edit | edit source]
There are two ways to develop patellofemoral instability by dislocation of the patella. It can develop after a traumatic dislocation of the kneecap in which the medial kneecap-stabilisers are stretched or ruptured, which eventually can result in recurrent dislocations of the patella. The other way is caused by anatomical anomaly of the knee joint.
Chronic instability of the patellofemoral joint and recurrent dislocation may lead to progressive cartilage damage and severe arthritis if not treated adequately
Patella dislocation after trauma[edit | edit source]
Acute traumatic patellar dislocation accounts for approximately 3% of all knee injuries. The leading mechanism of an acute dislocation of the patella is knee flexion with internal rotation on a planted foot with a valgus component.[3] This scenario accounts for 93% of all cases.[4] One of the common findings related to acute, primary, traumatic patellar dislocations is hemarthrosis of the knee, caused by rupture of the medial ligamentous stabilizers of the patella. This causes bleeding into joint spaces resulting in swelling and the formation of bruises around the kneecap. Knee joint effusion is also a typical finding after patellar dislocation. This can cause severe pain and it may limit the clinical examination.
Traumatic kneecap dislocation is typically the result of a sports injury and about 2/3 of the cases occur in young, active patients under the age of 20.[4] In case of traumatic dislocation conservative management may be preferred although nearly half of all patients with a first-time dislocation will suffer additional dislocations.[3] Subjects may even develop patellar instability, (aspecific) pain, patellofemoral arthritis or even chronic patellofemoral instability, depending on the presence and severity of the anatomic damage.[5]
Patella dislocation with a specific functional or anatomical cause[edit | edit source]
Dislocations without an acute knee hemarthrosis, which are mainly recurrent dislocations, may be associated with anomalies of the patellofemoral joint. These anomalies include trochlear dysplasia, patella alta, and lateralization of the tibial tuberosity (excessive lateral distance between the tibial tubercle and the trochlear groove). These are the primary causes of dislocations with an anatomical cause.
Important secondary factors contributing to patellofemoral instability are femorotibial malrotation, genu recurvatum (hyperextended knee), and ligamentous laxity caused by Ehlers-Danlos syndrome, and Marfan syndrome.[3]
Characteristics/Clinical Presentation[edit | edit source]
Patients experience Anterior Knee Pain and episodes of mechanical instability. [2] The pain can be aggravated by activities such as up and down the stairs, sports such as running, hopping and jumping, and changing direction. Upon functional assessment the patient may struggle with control of the patella, resulting in the patella being pull from midline, therefore to assess this you need to observe what is happening to the patella during static and dynamic movements such as squatting / lunging.
Risk factors
- Insufficient deep articular surface (trochlea dysplasia) [6]
- Insufficient distance between tibial tuberosity and the trochlear quarry [6]
- Insufficiency of the MPFL [6]
- Patella alta (engagement into the trochlea does not occur in the early phase of knee flexion, thus potentiating instability at the patellofemoral joint) [2][6]
- Knee valgus: an increased Q-angle can affect the patella tracking. [2]
- Inadequate VMO[2]
- A lesion of the medial retinaculum [7]
Differential Diagnosis[edit | edit source]
- Patellar dislocation: It may take place as a direct traumatic event (acute dislocation of the patella) in a patient with normal patellar alignment. It can also occur in a patient with pre-existing malalignment, especially if there is significant baseline subluxation.
- Patellar subluxation: When the patella is transiently or permanently medial or lateral to its normal tracking course, then the patella may articulate abnormally. Subluxation or lateral translation will involve a transient lateral movement of the patella. In general, it is early in knee flexion such that the patient will experience a feeling of pain or instability. This form of patellar subluxation is rather a recurrent dislocation of the patella. It is essential to distinguish between this form of abnormal patellar alignment and tilt.
Types of subluxations:
• Minor Recurrent Subluxation
• Major Recurrent Subluxation
• Permanent Lateral Subluxation
Diagnostic Procedures[edit | edit source]
Patellar instability is normally diagnosed through a comprehensive history of the patient's symptoms and functional objective assessment of the knee. Further scans such as MRI's and Ultrasound imaging can be performed to rule out any structural deficits. Patellofemoral instability can also be examined through a lateral radiography or CT scan. In the case of trochlea dysplasia, medical images show different flexion angles and varus movements are limited in the knee. CT scans provide better images than MRI scans. A lateral radiography can provide information about the height of the patella and whether there is trochlea dysplasia. [6]
Outcome Measures[edit | edit source]
There are many outcome measures that can be used with this condition. Currently, there are no specific recommendations from COMET, therefore it is up to the clinician to clinically reason which outcome measure would be most appropriate for their patient, for example:
- Anterior Knee Pain Scale
- Lower Extremity Functional Scale
- Pain Assessment Scales
- Numeric Pain Rating Scale
Examination[edit | edit source]
The first diagnostic step is a detailed history. It is the most important clue for a correct diagnosis. The second diagnostic step is a careful, complete and essential physical examination. The purpose of this examination is to reproduce the symptoms (pain/instability) and to locate the painful zone. The location can indicate which structure is injured, it is truly helpful to compose the diagnosis and to plan the treatment.
Key points for examination are;
- Assessment of acute dislocation: Deformity and swelling that may mask a persistent lateral subluxation of the patella [2]
- Lower limb alignment in coronal, sagittal and axial planes. [2]
- Evidence of joint hyperlaxity: Measured by the Beighton hypermobility score. [2]
- Measurement of the Q-angle: An increase in Q-angle results in an increased valgus vector. This is associated with an increased risk of instability, due to more laterally orientated forces. [2]
- Palpation of the patella: It may reveal a palpable defect at the medial patellar margin and tenderness along the course or at the insertion of the MPFL. [2]
- Patellar-glide test: This test is used to evaluate the instability. A medial/lateral displacement of the patella greater than or equal to 3 quadrants, with this test, is consistent with incompetent lateral/medial restraints. Lateral patellar instability is more frequent than medial instability.
- Fairbanks patellar apprehension test: It is positive when there is pain and muscle defensive contraction of lateral patellar dislocation with 20°–30° of knee flexion. The positive test indicates that lateral patellar instability is an important part of the patient’s problem. This may be so positive that the patient pulls the leg back when the therapist approaches the knee with his hand, preventing so any contact, or the patient grabs the therapist’s arm.[8] → 100% sensitivity, 88.4% specificity, and overall accuracy of 94.1%
- Patellar-gravel test and J-sign test: It will test dynamic patellar tracking, but they are non-specific and have been noted to be absent in most cases of instability. [2]
Medical management[edit | edit source]
Non-operative treatment is usually attempted for 3 to 6 months. If that fails, surgical options are considered [9][10][11]
A review to assess the clinical and radiological outcomes of surgical compared to non-surgical interventions for treating primary or recurrent patellar dislocation did not show sufficient high-quality evidence to confirm a difference between both intervention types.[12] (level of evidence 1a)
Surgical Procedures[edit | edit source]
- Lateral-release: the aim of this procedure is to release the tight lateral ligaments that pull the kneecap from its groove causing increased pressure on the cartilage and dislocation. Therefore, the ligaments that tightly hold the kneecap are cut using an arthroscope[9][13][14][15] (level of evidence 4)
- MPFL reconstruction: in this procedure, the torn MPFL is removed and reconstructed using a grafting technique. Grafts are usually harvested from the Hamstring tendons, located at the back of the knee and are fixed to the patella tendon using screws. The grafts are either taken from the same individuals (autograft) or from a donor (allograft). This procedure is also performed using an arthroscope.[9][13][14][16] (level of evidence 4) [17]
- Tibia tubercle realignment or transfer: tibia tubercle is a bony attachment below the patella tendon which sits on the tibia. If the tibial tubercle is rotated too much then there is a surgery needed to set it in an improved position. In this procedure, the tibia tubercle is moved towards the center which is then reattached by two screws. The screws hold the bone in place and allow faster healing and prevent the patella to slide out of the groove. This procedure is also performed using an arthroscope. [9][13][14]
- In the rare case where the groove for the patella (trochlear groove) is too shallow: this may have to be addressed with surgery to make the groove deeper. In the similarly rare situation of a patella that sits too high on the knee, surgery may be required to bring the patella down to a more normal position so that it rides better in its groove[9][13][14]
- Lateral side ligament injuries (often in combination with injury to the ACL and/or PCL.) which occur as a result of a knee dislocation are quite rare when compared to other knee ligament injuries.[18][19] In addition, there is controversy surrounding the acute treatment of these injuries. However, most authors agree these injuries should be surgically treated within three weeks.
The repair technique for the lateral side ligament injury is described as an “en masse” surgical repair.[20] (level of evidence 4) This procedure is performed via a longitudinal incision from the tibial tubercle to the fibular head with the lateral side surgically exposed in a distal to proximal fashion.
The “en masse” approach is utilized due to the strong connection between the structures in the healing mass. Thus the “en masse” technique allows the surgeon to take advantage of the body's healing response in this area rather than individually repairing each component of the lateral side ligaments.
Post-operative care:[edit | edit source]
If an arthroscopy is performed to remove loose bodies in the knee following a dislocation, then the recovery is relatively quick and not much different from non-operative treatment. Physical therapy will be necessary for a few months in order for the patients to regain their range of motion and strength.[11]
Patellar stabilizing surgery will take much longer for a patient to recover from because these procedures typically require a larger open incision. Following the surgery, the ligament repair or reconstruction will have to heal. If a bone cut is performed for the tibial tubercle, then there also will be a period of time necessary for the bones to heal together. Although there will be variability depending on the specific surgery performed, recovery from these procedures will commonly take many months.[11]
Physical Therapy Management[edit | edit source]
There is no consensus yet whether surgical or conservative treatment after patellar dislocation is preferable[12](level of evidence 1a) To assess this more research is needed. In any case, for both conservative and surgical treatment, physical therapy will be needed.
Nonsurgical treatment after acute patellar dislocation[edit | edit source]
After a first dislocation of the knee, a period of immobilization is appropriate. This is necessary to heal the soft tissues, especially the supporting structures on the medial side of the knee. There are several possibilities for immobilization: a cylinder cast, a posterior splint, a brace or a tape. There is no consensus yet on which type of immobilization is more appropriate.[21](Level of Evidence 2b) [22](level of evidence 1b)[23] (level of evidence 3a)
The duration of immobilization may vary from no immobilization to six weeks. The optimal duration has not been defined yet.[24](level of evidence 2a) Mostly two to three weeks of immobilization are applied.[12](level of evidence 1a) [21][25] (level of evidence 2b) It is important to keep the immobilization period as short as possible since immobilization may have some deleterious effects on ligament strength, joint cartilage and may cause prolonged weakness of the bony origin of ligaments.[21][22](level of evidence 1b) [26] (level of evidence 2b)[27] (level of evidence 2b) [28] This might result in muscular atrophy, flexion deficit and potential poor (short-term) functional outcome.[23] (level of evidence 3a)[22](level of evidence 1b) Therefore rehabilitation must start as soon as possible.
The aim of rehabilitation is to restore knee range of motion and improve patellar stability by reinforcing the quadriceps.[12] (level of evidence 1a)[21][29](level of evidence 1b)[30][31]
Early mobilization starts with closed-chain exercises and passive mobilization.[22] (level of evidence 1b) In the acute period quadriceps setting exercises and three sets of 15 to 20 straight leg raises are done four to five times a day. Ice is applied for 20 minutes every two to three hours to reduce swelling. [32](level of evidence 2b) Some examples of closed chain exercises are wall sets (the patient squats until approximately 40° while keeping his back flat to the wall for 15 to 20 seconds, for a total of 10 to 15 repetitions), side and forward step-up exercises, short arc leg presses, stationary bike and stepping machine exercises.[32] There has been a lot of research on whether the focus should be on the VMO, but there is no evidence that this would significantly improve patellar stability.[21][33]
Besides training the quadriceps muscle, stretching of the Hamstring muscle and articular retinaculum should be included in the rehabilitation program one month after trauma.[24] (level of evidence 2b) Patient-education should be part of the therapy as well. The patient should receive home exercises which he/she should regularly do.
Athletes must be guided in the process to return to the level prior to injury or even higher. To succeed specific exercises have to be integrated into the rehabilitation program. Not only the quadriceps muscle but also the pelvic stabilizers and the lateral trunk muscles have to regain force and dynamic stability.[10](level of evidence 4)
To be able to return to sports, the following criteria should be fulfilled mostly at six weeks after injury:
- Absence of pain
- No effusion
- Complete range of motion: the range of motion is mostly restored after six weeks when exercises are done.[10] (level of evidence 4) If not, the full range of motion might not be regained.[25](level of evidence 2a)
- Symmetrical strength: strength can be recovered with quadriceps exercises as mentioned above. For high-demanding sports, the limb symmetry index (LSI) should be at least 90%.[34] [35][36][37](level of evidence 5)
- Dynamic stability: to acquire excellent dynamic lower limb stability, exercises with cutting maneuvers, side hops and sudden change of direction should be incorporated in the training program and performed on different surfaces.[10](level of evidence 4)
- In the final phase sport-specific activities such as plyometric and landing strategies for jumping sports, one leg stability for material arts, cutting maneuvers and pivoting for team sports, proprioception, side stability and landing capacities for skiers dominate the therapy.[10] (level of evidence 4)
To evaluate if the criteria mentioned above are fulfilled, the following tests can help:
- Single-leg squat: to evaluate dynamic stability. This test can also serve as an exercise, part of the program.[38]
Execution: Squat on a single leg (compare both legs). Attention should be paid that the knee does not go into a valgus movement and stays above the foot. The pelvis must remain stable (no dropping or turning).[10](level of evidence 4) - Star Excursion Balance Test (SEBT): to evaluate dynamic stability
- Drop jump test: evaluates control of landing. This is important for sports which demand to land from jumps (e.g. basketball, volleyball etc)
Execution: the patient drops from a box and lands on both feet, after which he/she directly jumps as high as possible for a second time. Pay attention to the symmetry of the reception, the alignment of both knees, deceleration and the capacity for absorbing the shock.[10](level of evidence 4)[39](level of evidence 2b) - Side-hop test: evaluates speed, agility, muscle coordination, limb alignment, trunk stability and control in changing directions.[10](level of evidence 4)
Execution: The patient jumps on one leg as often as possible during 30s between two lines at a distance of 40 cm.[10](level of evidence 4)
Ideally, the patient has done them in the beginning of the therapy as well so that advancement can be registered during and after therapy. It might be helpful to film the test. This way it is easier to analyze the test, to give feedback and to select new exercises for the weak spots.
Nonsurgical treatment after recurrent dislocation of the patella[edit | edit source]
Surgery is not necessarily needed for patients with patellofemoral malalignment or relaxation of the patella. Adequate results can be achieved with a conservative exercise treatment program. It is very important in the rehabilitation program to strengthen the quadriceps muscle and VMO. It’s advised to follow the program which is similar to that followed after acute dislocation, but with more resistive exercises. This program can also be started early. In addition, a stabilization brace of the patella may help to prevent chronic recurrent subluxation.[19]
Specific postoperative care[edit | edit source]
An important aspect of knee dislocation surgery is postoperative rehabilitation.[40]
- Care after a posterolateral corner repair:
The knee is placed in a Jones dressing and the knee brace is locked at 30° for 2 weeks to promote wound healing and to minimize stress on the peroneal nerve and popliteal artery. Active quadriceps exercises are begun immediately. The early protected range of motion is important to prevent arthrofibrosis. When both cruciates are torn, knee flexion is performed in the prone position to minimize the posterior tibial sag.[13](Level of Evidence : 5)[14][41]
- Care after Proximal realignment and MPFL reconstruction:
Generally, patients are encouraged to weight-bear in a knee immobilizer or hinged knee brace locked in extension from up to 2 weeks postoperatively. From 2 to 6 weeks postoperatively, patients may perform active and passive range of motion of the knee from 0° to 90°. At 3 weeks postoperatively, closed chain quadriceps strengthening exercises are suggested, and this can progress to open chain exercises at 3 months postoperatively. Patients may then gradually return to non-contact sports, with a potential return to contact sports 4 to 6 months postoperatively.[13][14][41][42](level of evidence 2b)
- Care after Anterior-medialization of the tibial tubercle (Fulkerson osteotomy):
Rehabilitation generally involves protected weight-bearing with crutches and a knee immobilizer for 4 weeks to reduce the risk of postoperative fracture. At 4 to 6 weeks, closed chain quadriceps strengthening exercises can be initiated, with the expectation of a full recovery by 3 to 4 months. The patient should delay running and more forceful activities until 8 to 12 months postoperatively to allow maximum bony healing [9][13][14][15](level of evidence 4)[41]
- Care after surgery following lateral side ligament injuries due to knee dislocation and rehabilitation with the Knee Symmetry Model (KSM):
When using the KSM for ACL postoperative rehabilitation the ultimate goal of treatment is to regain symmetry of the knees. The range of motion and strength become the primary objective measures.[9][42]
Already after the first week of bed rest, patients are allowed to resume normal daily activities. Full weight bearing with the immobilizer is encouraged and crutches are only used for support or balance until the patient is comfortable walking without them. When the patient can demonstrate good leg control via good quadriceps activation and straight leg raises, the leg immobilizer is discontinued. In some cases, damage to the common peroneal nerve can lead to foot drop.[9][42]
A continuous passive motion (CPM) machine is initiated immediately following surgery. (e.g.: passive stretch, heel slide, and flexion exercise to evaluate own range of motion )
Strength testing is performed at 2 months after surgery. This includes open kinetic chain (OKC) isokinetic testing at 180 and 60 ° per second speeds, an isometric leg press test and when appropriate, a single-leg hop test.[9][42]
Return to sports can only occur once the patient has achieved goals, like good stability, bilaterally symmetrical range of motion and strength, and he/she is comfortable with the rigors of their activity. Usually, patients return to sports from a lateral side knee ligament repair in 4-6 months after surgery.[42][43]
Patients are progressed in accordance t their own unique healing abilities and progression. Initial postoperative goals are to prevent effusion and swelling. Restoration of a symmetrical range of motion and strength are achieved according to patient tolerance[9][42][43] (level of evidence 4)
Clinical relevant bottomline[edit | edit source]
Patellofemoral instability is a result of malalignment of the patella in the trochlear grove caused by stretched or ruptured medial kneecap-stabilizers (traumatic) or anatomical anomalies of the knee joint. Primarily a conservative, non-operative exercise treatment is initiated, where quadriceps muscle strengthening is the main objective. Nearly half of all patients with a first-time dislocation will suffer additional dislocations. Chronic instability of the patellofemoral joint and recurrent dislocation may lead to progressive cartilage damage and severe arthritis if not treated adequately. In those cases, one can opt for operative intervention. The post-operative physical therapy treatment depends on the type of surgery that has been performed.
References[edit | edit source]
- ↑ Distefano, M. John P. Fulkerson. Disorders Of The Patellofemoral Joint. Ed. 3. Baltimore: Williams and Wilkins, 1998. 365 pp.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 Rhee, S. J., Pavlou, G., Oakley, J., Barlow, D., & Haddad, F. Modern management of patellar instability. International Orthopaedics. 2012; 36(12): 2447-2456.
- ↑ 3.0 3.1 3.2 Diederichs, G., Issever, A. S., & Scheffler, S. MR imaging of patellar instability: injury patterns and assessment of risk factors. Radiographics. 2010; 30(4):961-981.
- ↑ 4.0 4.1 Tsai, C. H., Hsu, C. J., Hung, C. H., & Hsu, H. C. Primary traumatic patellar dislocation. Journal of orthopaedic surgery and research. 2012: 7(1), 21
- ↑ Diederichs, G., & Scheffler, S.MRI after patellar dislocation: assessment of risk factors and injury to the joint. RoFo: Fortschritte auf dem Gebiete der Rontgenstrahlen und der Nuklearmedizin. 2013; 185(7), 611-620
- ↑ 6.0 6.1 6.2 6.3 6.4 Dietrich, T. J., Fucentese, S. F., & Pfirrmann, C. W. Imaging of individual anatomical risk factors for patellar instability. In Seminars in musculoskeletal radiology. 2016; 20(01):065-073
- ↑ Frosch, S., Balcarek, P., Walde, T. A., Schuttrumpf, J. P., Wachowski, M. M., Ferleman, K. G. & Frosch, K. H. Die therapie der patellaluxation: eine systematische literaturanalyse. Z Orthop Unfall, 2011;149(06): 630-45
- ↑ Sanchis-Alfonso, V. Anterior Knee Pain and Patellar Instability. London: Springer-Verlag London Ltd.; 2011
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 9.8 9.9 Kissin Y, Shein D, Treatment Options for Patellar Instability. Available from: https://icjr.net/articles/treatment-options-for-patellar-instability (accessed 06/11/2016)
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 10.8 Colvin A, West R. Patellar Instability. The Journal of Bone and Joint Surgery-American Volume. 2008;90(12):2751-2762
- ↑ 11.0 11.1 11.2 Andrish J. The Management of Recurrent Patellar Dislocation. Orthopedic Clinics of North America. 2008;39(3):313-327.
- ↑ 12.0 12.1 12.2 12.3 Smith T, Donell S, Song F, Hing C. Surgical versus non-surgical interventions for treating patellar dislocation. Cochrane Database of Systematic Reviews. 2015;. (level of evidence 1a)
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 Kaar S. Patellar Dislocation – SportsMD. Available from: https://www.sportsmd.com/sports-injuries/knee-injuries/patellar-dislocation-instability/(accessed 06/11/2016) (Level of Evidence 5)
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 Eldridge J. Kneecap Dislocation (Patella Dislocation). Available from: http://www.kneesurgeonbristol.co.uk/conditions-treatments/kneecap-dislocation/ (accessed 06/11/2016)
- ↑ 15.0 15.1 Dantas P, Nunes C, Moreira J, Amaral L. Antero-medialisation of the tibial tubercle for patellar instability. International Orthopaedics. 2005;29(6):390-391. (level of evidence 4)
- ↑ Dopirak R, Adamany D, Bickel B, Steensen R. Reconstruction of the Medial Patellofemoral Ligament Using Quadriceps Tendon Graft: A Case Series. Orthopedics. 2008;31(3):1-8. (level of evidence 4)
- ↑ Tom A, Fulkerson J. Restoration of Native Medial Patellofemoral Ligament Support After Patella Dislocation. Sports Medicine and Arthroscopy Review. 2007;15(2):68-71.
- ↑ Rubinstein R, Shelbourne K. Management of combined instabilities: Anterior cruciate ligament/medial collateral ligament and anterior cruciate ligament/lateral side. Operative Techniques in Sports Medicine. 1993;1(1):66-71
- ↑ 19.0 19.1 Shelbourne, K. D., & Carr, D. R. Combined anterior and posterior cruciate and medial collateral ligament injury: nonsurgical and delayed surgical treatment. Instructional course lectures. 2003; 52: 413-418.
- ↑ Shelbourne K, Haro M, Gray T. Knee Dislocation With Lateral Side Injury: Results of an En Masse Surgical Repair Technique of the Lateral Side. The American Journal of Sports Medicine. 2007;35(7):1105-1116. (level of evidence 4)
- ↑ 21.0 21.1 21.2 21.3 21.4 Duthon, V. B. Acute traumatic patellar dislocation. Orthopaedics & Traumatology: Surgery & Research.2015;101(1):S59-S67.
- ↑ 22.0 22.1 22.2 22.3 Rood A, Boons H, Ploegmakers J, van der Stappen W, Koëter S. Tape versus cast for non-operative treatment of primary patellar dislocation: a randomized controlled trial. Archives of Orthopaedic and Trauma Surgery. 2012;132(8):1199-1203. (level of evidence 1b)
- ↑ 23.0 23.1 ] van Gemert J, de Vree L, Hessels R, Gaakeer M. Patellar dislocation: cylinder cast, splint or brace? An evidence-based review of the literature. International Journal of Emergency Medicine. 2012;5(1):45. (level of evidence 3a)
- ↑ 24.0 24.1 Smith T, Davies L, Chester R, Clark A, Donell S. Clinical outcomes of rehabilitation for patients following lateral patellar dislocation: a systematic review. Physiotherapy. 2010;96(4):269-281. (evidence level 2a)
- ↑ 25.0 25.1 Camanho G, Viegas A, Bitar A, Demange M, Hernandez A. Conservative Versus Surgical Treatment for Repair of the Medial Patellofemoral Ligament in Acute Dislocations of the Patella. Arthroscopy: The Journal of Arthroscopic Related Surgery. 2009;25(6):620-625. (level of evidence 2b)
- ↑ Maenpaa H, Lehto M. Patellar Dislocation: The Long-term Results of Nonoperative Management in 100 Patients. The American Journal of Sports Medicine. 1997;25(2):213-217. (level of evidence 2b)
- ↑ Mäenpää H, Latvala K, Lehto M. Isokinetic thigh muscle performance after long-term recovery from patellar dislocation. Knee Surgery, Sports Traumatology, Arthroscopy. 2000;8(2):109-112. (level of evidence 2b)
- ↑ Kannus R, Jòzsa L, Renström R, Järvtoen M, Kvist M, Lento M et al. The effects of training, immobilization and remobilization on musculoskeletal tissue. Scandinavian Journal of Medicine Science in Sports. 2007;2(3):100-118.
- ↑ Beasley L, Vidal A. Traumatic patellar dislocation in children and adolescents: treatment update and literature review. Current Opinion in Pediatrics. 2004;16(1):29-36. (Level of Evidence 1b)
- ↑ Cosgarea A, Browne J, Kim T, McFarland E. Evaluation and Management of the Unstable Patella. The Physician and Sportsmedicine. 2002;30(10):33-40.
- ↑ Woo R, Busch M. Management of patellar instability in children. Operative Techniques in Sports Medicine. 1998;6(4):247-258.
- ↑ 32.0 32.1 Minkowitz R., Inzerillo C, Sherman O. Patella Instability. Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-293. (level of evidence 2b)
- ↑ Smith T, Bowyer D, Dixon J, Stephenson R, Chester R, Donell S. Can vastus medialis oblique be preferentially activated? A systematic review of electromyographic studies. Physiotherapy Theory and Practice. 2009;25(2):69-98.
- ↑ Bizzini M, Hancock D, Impellizzeri F. Suggestions From the Field for Return to Sports Participation Following Anterior Cruciate Ligament Reconstruction: Soccer. Journal of Orthopaedic & Sports Physical Therapy. 2012;42(4):304-312. (level of evidence 5)
- ↑ Kokmeyer D, Wahoff M, Mymern M. Suggestions From the Field for Return-to-Sport Rehabilitation Following Anterior Cruciate Ligament Reconstruction: Alpine Skiing. Journal of Orthopaedic & Sports Physical Therapy. 2012;42(4):313-325. (level of evidence 5)
- ↑ Verstegen M, Falsone S, Orr R, Smith S. Suggestions From the Field for Return to Sports Participation Following Anterior Cruciate Ligament Reconstruction: American Football. Journal of Orthopaedic & Sports Physical Therapy. 2012;42(4):337-344. (level of evidence 5)
- ↑ Waters E. Suggestions From the Field for Return to Sports Participation Following Anterior Cruciate Ligament Reconstruction: Basketball. Journal of Orthopaedic & Sports Physical Therapy. 2012;42(4):326-336. (level of evidence 5)
- ↑ McConnell J. Rehabilitation and Nonoperative Treatment of Patellar Instability. Sports Medicine and Arthroscopy Review. 2007;15(2):95-104
- ↑ Noyes F. The Drop-Jump Screening Test: Difference in Lower Limb Control By Gender and Effect of Neuromuscular Training in Female Athletes. American Journal of Sports Medicine. 2005;33(2):197-207. (level of evidence 2b)
- ↑ Noyes F, Barber-Westin S. Reconstruction of the Anterior and Posterior Cruciate Ligaments After Knee Dislocation: Use of Early Protected Postoperative Motion to Decrease Arthrofibrosis. The American Journal of Sports Medicine. 1997;25(6):769-778.
- ↑ 41.0 41.1 41.2 Daley R. Patellar Dislocation Treatment Chicago. Available from: http://www.daleymd.com/patient-info/conditions-procedure/knee/knee-problems/patellar-dislocation/(accessed 06/11/2016)
- ↑ 42.0 42.1 42.2 42.3 42.4 42.5 Kinzer A, Jenkins W, Urch S, Shelbourne K. Rehabilitation following knee dislocation with lateral side injury: Implementation of the knee symmetry model. North American Journal of Sports Physical Therapy. 2010;5(3): 155-165. (level of evidence 2b)
- ↑ 43.0 43.1 Anderson A. The International Knee Documentation Committee Subjective Knee Evaluation Form: Normative Data. American Journal of Sports Medicine. 2005;34(1):128-135. (level of evidence 4)