Rebound Therapy
Introduction[edit | edit source]
The phrase Rebound Therapy, when correctly applied describes a specific methodology, assessment, and programme of use of trampolines to provide opportunities for enhanced movement patterns, therapeutic positioning, exercise and recreation for a wide range of users with additional needs. It is used to enhance movement patterns, develop and promote motor skills, body awareness, balance, coordination, and communication. It is a highly enjoyable activity and is used to great effect as a cross-curricular teaching tool.
Though the idea of using trampolines in special education has existed since the 1950s it was not until the 1970s that the concept of Rebound Therapy was developed by the physiotherapist, remedial gymnast and headteacher Eddy Anderson who worked with children with both physical and learning disabilities.[1]
In 1992, following interest from the Chartered Society of Physiotherapy and the British Trampoline Federation, Eddy Anderson provided training courses to both organisations in the use and implementation of Rebound Therapy following many years of working in education delivering Rebound Therapy on staff development courses. Since 2011, Rebound Therapy has been introduced into Australia, Malaysia, Canada, and the USA..
When working with individuals in Rebound Therapy, if appropriate, progress can be accurately measured and recorded using the Huddersfield Functional Index in conjunction with the Winstrada development programme.
Since its inception Rebound Therapy has expanded beyond its original user base and is being used with an increasingly expanding client base. Rebound Therapy should always be used as part of a therapeutic development programme. For students with profound and complex needs, it is recommended that this programme is developed in liaison with a physiotherapist. For more ambulant students, it is recommended that the first three grades of the Winstrada development programme are followed because this is based entirely on the Rebound Therapy training course.
Benefits of Rebound Therapy[edit | edit source]
Rebound Therapy is a fun and interactive activity that can not only influence a person's physical function but also participation, communication, and sensory system. These benefits can be enhanced by using games that incorporate activities such as counting, teamwork, silly sounds, finding specific colour flashcards, identification of images or colours.
The benefits of Rebound Therapy have been likened to those found in hippotherapy, it provides a weightless environment and as well as three-dimensional movement.[2] [3] This challenges the body in a multitude of ways for a variety of benefits
Rebound Therapy can provide multiple benefits including the development and improvement of:
|
|
Other benefits[edit | edit source]
Other benefits include:
- Stimulation of the digestive system
- Improved bowel function
- Internal organ massage
- Clearing of toxins from the body
- Respiratory Benefits
The added benefits of stimulation of the digestive system, improved bowel function, and internal organ massage are achieved by the rhythmic acceleration and deceleration, and increase and decrease in weight offered by movement on the trampoline.
The clearing of toxins from the body is a process brought about by bouncing on a trampoline causing stretching and contracting of cells in the body.
Contraindications[edit | edit source]
Listed below are the known contraindications for Rebound Therapy. If any of the following are present, the physiotherapist will use their clinical knowledge and judgement and seek appropriate advice and medical information in order to make an informed decision about modification of treatment or whether a potential service user is unsuitable to take part in Rebound Therapy:
- Cardiac or circulatory problems
- Downs Syndrome
- Respiratory problems
- Vertigo
- Blackouts or nausea
- Epilepsy
- Spinal cord or neck problems
- Spinal rodding
- Open wounds
- Any recent medical attention
- Brittle bones/osteoporosis
- Friction effects on the skin
- Unstable/hypermobile/painful joints
- Herniae
- Implant surgery (e.g. Baclofen pump)
- Prolapse
- Severe challenging behaviour
- Gastrostomy/colostomy
- Gastric reflux
- Stress Incontinence
- Joint replacement [4]
Absolute Contraindications[edit | edit source]
The following six are absolute contraindications for Rebound Therapy and under no circumstances should they be performed due to the risks posed to anyone with any of these six contraindications:
- Pregnancy -Trampolining during pregnancy can cause disruptions to the womb and has the potential to cause harm to an unborn baby. Also, the extra strain of such a high energy sport may cause damage to the mother whose vital organs are already functioning at a higher than normal level.
- Detaching retina -This disorder is caused when the retina (the thin layer, at the back of the eye, responsible for light detection) starts to separate from the eye socket. It can cause blindness if not treated early. Trampolining can cause the retina to completely detach, leading to total blindness.
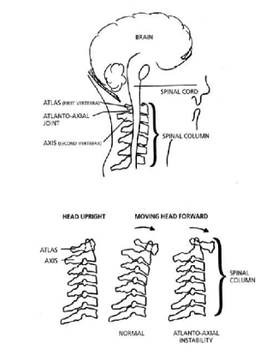
- Atlantoaxial instability (AAI)- A condition associated with 10-40% of people with Down’s Syndrome. Weakened ligaments are normal in people with Down’s Syndrome, causing slack joints. This may cause a weakness in the Atlanto- Axial joint of the first (Atlas) and second (Axis) vertebrae, right below the skull. This makes sufferers of AAI prone to slippage of these vertebrae which can cause brain damage and paralysis.
- People with Achondroplasia or another genetic skeletal dysplasia. People with Achondroplasia and some other forms of dwarfism have an exaggerated lumbar lordosis and spinal stenosis, these 2 factors increase the jarring forces through the spine on impact.
- People who have Spinal rods
- People with Osteo-Genesis Imperfecta (Brittle bone disease)
- The image directly below demonstrates Atlantoaxial Instability (AAI)[4][5]
Conditions That Can Be Treated With Rebound Therapy[edit | edit source]
Rebound Therapy, as stated above, can provide a large array of benefits for a large group of patient groups. As a physiotherapy intervention, one of Rebound Therapy's primary aims is to impact upon muscle tone disorders. However, it is important to provide information on the type of conditions that may benefit from Rebound Therapy. It is important to remember that the conditions that will be elaborated upon are not the only ones that can benefit from Rebound Therapy. The following conditions stand to benefit from Rebound Therapy:
Hypertonia[edit | edit source]
Hypertonia is increased tightness in the muscle tone, which reduces the capacity of the muscle tissue to stretch. This is caused by damage to the motor pathways, in the central nervous system, which carries information from the central nervous system to the muscles that control basic activities such as posture, muscle tone, and muscle reflexes. Left untreated hypertonia can cause severe pain, reduced quality of life, loss of function and deformity. In the most severe cases hypertonia can completely stop joint movement. There are two types of hypertonia; spastic hypertonia and dystonic hypertonia.
- Spastic hypertonia- Spastic hypertonia can be caused by a number of conditions such as; cerebral palsy, stroke, spinal cord injury. This variant of spastic hypertonia leads to uncontrolled muscle spasms, stiffening and straightening of the muscles and sudden contractions of all or part of the muscle leading to abnormal muscle tone.
- Dystonic hypertonia- This refers to the resistance of the passive stretching of muscles (passive stretching of muscles occurs when the physiotherapist stretches the muscle at a low velocity to a comfortable length). Dystonic hypertonia also refers to when the muscle returns to its previously fixed position following movement. This type of hypertonia is most common in Parkinsonism.
Hypotonia[edit | edit source]
Hypotonia is a state of low muscle tone which can often lead to reduced muscle strength. Hypotonia is not the same as muscle weakness but it can sometimes be difficult to utilise the muscle which exhibits low tone. Muscle weakness can develop in association with hypotonia dependent on the underlying cause of the hypotonia. Hypotonia itself is not a specific medical condition but is a manifestation of one or several conditions.
Profound and Multiple Learning Disabilities (PMLD)[edit | edit source]
People with PMLD represent a group of individuals with severe learning disabilities as well as other disabilities, such as difficulties with movement, communication, vision, hearing etc. They are often wheelchair bound and have complex health issues. It has been proposed that Rebound Therapy can offer physical and communication benefits to these individuals.[6][7]
Autistic Spectrum Disorders[edit | edit source]
Rebound Therapy can also useful in the treatment of individuals with Autistic Spectrum Disorders (ASDs). During Rebound Therapy the individual with an ASD will be paired with a qualified Rebound Therapy instructor, in most cases a physiotherapist, who will be tasked with leading a treatment session. This is a great example of how Rebound Therapy can improve focus and concentration and improve the ability to maintain eye contact as the child with an ASD will need to focus and pay attention to the instructions provided by the Rebounder. With Rebound Therapy being originally developed in the educational environment, an opportunity to improve attentiveness and concentration is an often welcomed opportunity for child development.
Developmental Coordination Disorder (DCD)[edit | edit source]
Research has shown that students 7-11 years old with developmental coordination disorder (DCD) that were involved in a trampolining exercise program showed improved neuromuscular coordination.[8]
Equipment Requirements/Training Requirements/Safety[edit | edit source]
Training Requirements[edit | edit source]
Rebound Therapy can only be carried out by therapists who have received training and have gained practical experience by attending a Rebound Therapy course which will typically include the Winstrada Trampoline Development Programme (grades 1 to 3) and the Huddersfield Functional Index for accurate measuring and recording or progress and providing evidence of outcomes. While the physiotherapist remains responsible for the overall assessment and re-evaluation of the Rebound Therapy service user, the modality itself can be delivered by other trained individuals. When delivered in the stereotypical special education environment with which Rebound Therapy is most closely associated, this means it may be delivered by teachers, teaching assistants, support workers, and speech and language therapists.
Equipment/Personnel Requirements[edit | edit source]
For safety reasons Rebound Therapy can be resource-intensive due to the number of spotters required around the trampoline to ensure the safety of the service user. In addition to this, the facilities required for the safe practice of Rebound Therapy may be hard to find. A ceiling height of 4.87 metres is indicated as the safe minimum ceiling height for the delivery of Rebound Therapy. Ceiling heights can be lower but the service user should not be bouncing more than a safe height and a risk assessment should be written up that accommodates the characteristics of the environment as well as the students.
In addition to the ceiling height, the environment must be able to contain a regular-sized trampoline. Due to the unique needs of the equipment, Rebound Therapy is both staff-intensive, and as a result, cost-intensive. This is in addition to the large setup cost of equipment. As a result of the staff requirements, equipment, and cost requirements it may be difficult to effectively and safely implement Rebound Therapy in some settings.[4]
Key Evidence[edit | edit source]
While there are many listed benefits of Rebound Therapy the evidence behind these benefits is often hard to find. There have been studies that have been conducted on Rebound Therapy in clinical populations but most have very small sample sizes.
A study of 7 high functioning children with cerebral palsy showed that after a 12-week programme of Rebound Therapy there was an improvement in occupational performance and participation. There was limited improvement in their physical function, however, these children were already relatively high functioning.[9] A case study from 2020 found that rebound therapy had a positive effect on the gross motor function of a child with spastic cerebral palsy, but the authors recommend that further randomised controlled trials are needed.[10]
Jones et al (2007) conducted a study looking at behavioural and psychosocial outcomes of a 16-week Rebound Therapy based exercise program for people with profound intellectual disabilities. This also had a small sample size of only 6 adults. The study found that there were positive changes such as a decrease in lethargy and and reduction in hyperactivity.[11] Rebound Therapy, however, was not the only activity these participants were exposed to and so it is difficult to say that Rebound Therapy alone would bring about these positive changes. Another small study of only 4 children with profound and multiple learning disabilities (PMLD) found that benefits such as improvements in physical co-ordination and increased communication.[6] It was too small of a study to conclude whether Rebound Therapy is beneficial in people with PMLD and, as in all the above-mentioned studies, the authors suggested that research with larger sample sizes be conducted.) A 2019 study looked at the effect of a 12-week rebound therapy programme on the static stability of patients with spinal cord injury (SCI). This study found that rebound therapy helped to reinforce static stability in patients with SCI during motionless standing. Again, however, the sample size was small with only 16 participants included.[12]
The benefits of rebound therapy have also been explored in:
- Patients with high BMIs (alongside dietary interventions)[13][14]
- Individuals with hearing impairment (particularly in relation to postural control)[15]
- Patients with type 2 diabetes[16]
ReboundTherapy.org holds many studies and papers which are available on request.[17][18]. Despite this apparent lack of easily available evidence, Rebound Therapy is commonly used by Special Needs Educational Schools as a means of providing movement and physical experiences for those with physical disabilities. These establishments are encouraged to measure and record progress and provide evidence of outcomes using the Huddersfield Functional Index. Plenty of evidence has been provided anecdotally by physiotherapists performing the modality and there has been evidence from a few studies but it is not a practice that has been extensively researched. Anecdotally, it has been collectively agreed that Rebound Therapy does help to improve muscle tone, but again, this is not supported by any concrete evidence [18] It is hypothesised that muscle tone is affected in Rebound Therapy in the following ways. Low amplitude bouncing causes the vibration of muscle spindles. This results in their relaxation and thus can cause a decrease in muscle tone [3]. High amplitude bouncing can help increase muscle tone by stimulating the stretch receptors. The feeling of the trampoline on the skin can also provide a stimulatory sensation that can help to normalise muscle tone [3].
Previously the CSP has identified Rebound Therapy as an area of physiotherapy which would benefit from further research[17]. Given the high costs associated with Rebound Therapy in comparison to other alternative treatments, there is a definite need to carry out further research into the area to compare it to more traditional interventions to see if there is a more significant benefit to Rebound Therapy which could, in turn, justify the higher costs.[9]
One thing to consider however is the "fun" aspect of Rebound Therapy due to the very nature of the equipment involved. Considering the main client group likely to be involved in Rebound Therapy (children), the fact that the use of a trampoline is more likely to hold the attention of a child and as a result increased engagement with the modality. Due to increased willingness to engage with Rebound Therapy, this means Rebound Therapy may hold an advantage over more traditional modalities which may be considered "boring" in comparison. This is especially important in children with learning disabilities who may be at a predisposition to become inattentive. To summarise, Rebound Therapy is especially effective in client groups who would usually be resistant to Rebound Therapy.[1] [5]
Resources[edit | edit source]
Revised Huddersfield Functional Index Manual
The below videos an examples of the uses of Rebound Therapy. While not exhaustive, this video provides a good example of the range of techniques that are used in Rebound Therapy.
References[edit | edit source]
- ↑ 1.0 1.1 Eddy Anderson. What is Rebound Therapy? (Accessed Online 16 August 2019).
- ↑ Mostafijur R. Effectiveness of rebound therapy for management of muscle tone in children with cerebral palsy(Doctoral dissertation, Bangladesh Health Professions Institute, Faculty of Medicine, the University of Dhaka, Bangladesh)).
- ↑ 3.0 3.1 3.2 Graham E. The effect of rebound therapy on muscle tone. Unpublished Master Thesis. Leeds Metrop Univ. 2006;4:1-57.
- ↑ 4.0 4.1 4.2 Chartered Society of Physiotherapy. Safe Practice in Rebound Therapy. London: Chartered Society of Physiotherapy, 2007, Revised September 2016.
- ↑ 5.0 5.1 Thomas Sanderson. A report on Rebound Therapy’s usefulness with Children with Disabilities. (Accessed 16 August 2019).
- ↑ 6.0 6.1 Smith E, Griggs G. Good Vibrations’: The effectiveness of teaching rebound therapy to children with profound and multiple learning difficulties. Journal of Qualitative Research in Sport Studies. 2010;3(1):91-104.
- ↑ Haghigh A, Mohammadtaghipoor F, Hamedinia M, Harati J. Effect of a combined exercise program (aerobic and rebound therapy) with two different ratios on some physical and motor fitness indices in intellectually disabled girl. Baltic Journal of Health and Physical Activity. 2019;11:24-33.
- ↑ Daneshvar, P., Ghasemi, G., Zolaktaf, V. and Karimi, M.T., 2019. Comparison of the effect of 8-week rebound therapy-based exercise program and weight-supported exercises on the range of motion, proprioception, and the quality of life in patients with Parkinson's disease. International journal of preventive medicine, 10.
- ↑ 9.0 9.1 Duff CJ, Sinani C, Marshall P, Maz J. Can rebound therapy improve gross motor skills and participation in children with cerebral palsy? Evidence from a small scale study. APCP J. 2016;7(1):4-13.
- ↑ Kora AN, Abdelaziem FH. The Effect of Rebound Therapy on Gross Motor Functions in a Child with Spastic Cerebral Palsy: A Case Study. BioScientific Review. 2020;2(3):1-7.
- ↑ Jones MC, Walley RM, Leech A, Paterson M, Common S, Metcalf C. Behavioral and Psychosocial Outcomes of a 16‐Week Rebound Therapy‐Based Exercise Program for People With Profound Intellectual Disabilities. Journal of Policy and Practice in Intellectual Disabilities. 2007 Jun;4(2):111-9.
- ↑ Sadeghi M, Ghasemi G, Karimi M. Effect of 12-Week Rebound Therapy Exercise on Static Stability of Patients With Spinal Cord Injury. J Sport Rehabil. 2019;28(5):464-7.
- ↑ Shah MR, Parab S. Effect of Rebound Exercises in Overweight Individuals on Bmi, Waist- Hip Ratio and Lung Functions : Randomized Control Trial. International Journal of Scientific Research in Science and Technology. 2018;4:1837-43.
- ↑ Justina OA, Petronilla OC, Ikenna UC, Nneka IC, Gloria MU. Effects of rebound exercises on overweight and obese adults: A scoping review. Archives of Physiotherapy & Global Researches. 2021 Jan 1;25(1).
- ↑ Ghavaminejad M, Ali A. Ghasemi. The Impact Of Rebound Therapy On Postural Control Of Hearing-Impaired People. Specialty Journal Of Sport Sciences. 2016;1(1):24-34.
- ↑ Nuhu JM, Maharaj SS. Influence of a mini-trampoline rebound exercise program on insulin resistance, lipid profile and central obesity in individuals with type 2 diabetes. The Journal of Sports Medicine and Physical Fitness. 2018;58(4):503-9.
- ↑ 17.0 17.1 Chartered Society of Physiotherapy. Priorities for Physiotherapy Research in the UK: Topics Prioritised by the Mental Health and Learning Disabilities Expert Panel. London: Chartered Society of Physiotherapy, 2002.
- ↑ 18.0 18.1 Watterston, R. and Delahunty, M. A Pilot Study Investigating the Use of Rebound Therapy for Clients with a Learning Disability. Page 20 in: Huddersfield Functional Index: Rebound Therapy Outcome Measures Toolkit. Huddersfield: Huddersfield NHS Trust, 2001.