Secondary Progressive Multiple Sclerosis - A Case Study
Top Contributors - Eliana Stein, Kim Jackson, Vince DePaul, Sandeep Saroya, Laura Ritchie, Purvang Patel and Anker Gonsalves
Abstract[edit | edit source]
- Purpose: To present a fictional case study of a multiple sclerosis (MS) patient including her clinical presentation of symptoms and then to offer evidence-based recommendations for disease management and symptom modulation.
- Case Presentation: Mrs. X is a 40-year-old woman with Secondary Progressive Multiple Sclerosis (SPMS). Her primary complaints include fatigue, dizziness, spasticity, coordination problems, and muscles weakness which affect her balance and overall quality of life (QoL).
- Intervention: Interventions included gait aid recommendations, a home exercise program (HEP), and therapist-administered approaches to improve ambulation, muscular endurance, and managing pain symptoms.
- Outcomes: Follow-up assessment showed moderate improvements in patient’s QoL scores. Improvements in patient’s gait scores were noted with decreased walking time as well as upper extremity movement measures. Patient also noted fewer falls with gait aid and marked improvements in fatigability.
Introduction[edit | edit source]
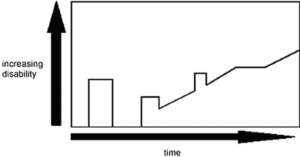
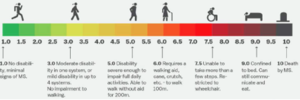
Mrs. X is a 40-year-old female with Secondary Progressive Multiple Sclerosis (SPMS). She came into the MS Clinic at Kingston General Hospital (KGH) as an outpatient to seek progression management and manage her current diagnosis of MS. Mrs. X lives with her husband and two adolescent children in a bungalow. Currently, she is equipped with home assistance devices provided by the Occupational Therapist (i.e., raised toilet seat, shower chair, grab bars). Since her diagnosis of MS 10 years ago, Mrs. X has complained of episodes of dizziness and fatigue and has noticed some changes in her balance and coordination, along with muscle weakness and spasticity. Due to this, she has experienced recent falls and has increased difficulty in her ambulation. Mrs. X’s disease progression is characteristic of the disease trajectory and prognosis for someone with SPMS (Figure 1). She has also noticed increased pain and reduced sensory deficits. She scored 5.5 on the estimated disability disease steps scale (EDDS) (Figure 2). Mrs. X has also reported a sensitivity to heat and has often complained that she doesn’t enjoy exercising as it makes her tired and is worried it will exacerbate her symptoms.
Many studies have shown to support Mrs. X’s symptoms. Approximately, throughout the course of MS, it is estimated that between 52% and 70% of patients will experience some form of sensory disturbance[2]. In a study conducted by Galey et al.[2] people with MS have sensory disturbances and that pain, temperature, and vibration deficits were found in the upper and lower extremities as well as the torso. The study also noted that some of the subjects experienced no sensory deficits; however, for most body parts, the number was quite small (<30%). The literature also showed that people with MS experience visual disturbance, muscle weakness, spasticity, and balance issues[3].
The purpose of this fictional report is to provide research-derived physiotherapy management for a patient with MS. The objectives of this report are to discuss the patient's characteristics, assessment findings, treatment interventions, and outcomes.
Client Characteristics[edit | edit source]
Mrs. X is a 40-year-old female with SPMS and lives in Kingston, Ontario. She doesn’t have any genetic dispositions to the disease as MS is not in her family history. Currently, she is working part-time as an accountant due to her limitations in mobility. Mrs. X could benefit from physiotherapy services to help with gait, balance, muscle strength, pain, and a HEP. In addition, physiotherapy services would be able to target functional endurance with day-to-day activities, support independent living, and QoL in order to reduce her fatigue symptoms.
Examination Findings[edit | edit source]
Subjective[edit | edit source]
Patient's primary concern was muscle weakness, as it impacts her balance and puts her at a high risk of falls. She reported that one of her first symptoms was pain with different eye movements but this decreased after approximately 10 days. She also reported frequent pain in her joints preventing her from engaging in an exercise program. She was worried that she might have to quit her job and won’t be able to support her family if her symptoms progress. She initially rated her pain an 8/10 upon exertion and a 4/10 at rest and described her pain as stabbing upon exertion and a dull achy pain at rest in her hips, legs, and arms. She complained of constant and severe pain in her lower extremities more than her upper extremities.
Objective[edit | edit source]
The following outcome measures were selected based on the recommendations From the American Physical Therapy Association Neurology Section Task Force[4]:
- Multiple Sclerosis Quality of Life-54 (MSQOL-54)
- Split into Mental and Physical Health sub-scores:
- Physical Score = 43
- Physical function = 8
- Health perceptions = 7
- Energy/fatigue = 6
- Role limitations - physical =6
- Pain = 5
- Sexual function = 3
- Social function = 5
- Health distress = 5
- Mental health score = 40
- Health distress =6
- Overall quality of life = 6
- Emotional well-being = 10
- Role limitations - emotional = 10
- Cognitive function = 8
- Two summary scores: Physical Health and Mental Health
- Both are scored of 100
- Split into Mental and Physical Health sub-scores:
- Berg Balance Scale
- Results: 32
- <36/56 = fall risk
- Timed 25-Foot Walk (T25-FW)
- Results: 10 seconds
- 9-Hole Peg Test (9-HPT)
- Results: 18 seconds
- Normative mean for MS is 17.81
- 12-Item MS Walking Scale
- Results: 50
- Higher score is indicative of a greater perceived impact of MS on walking
- Neurological Testing
- Reflexes
- UMN: Positive Clonus and Hoffman Reflexes
- LMN: Hyper-reflexivity (+3) for patellar and achilles reflexes
- Cranial Nerve Testing: positive nystagmus
- Spasticity: Refer to table 1 for spasticity scores
- Reflexes
Table 1. Spasticity scores according to Modified Ashworth Scale[5]
| Muscle Group | Right | Left |
|---|---|---|
| Elbow Flexors | 1 | 0 |
| Elbow Extensors | 1 | 0 |
| Wrist Flexors | 0 | 0 |
| Wrist Extensors | 0 | 0 |
| Hip Adductors | 1+ | 1+ |
| Hip Abductors | 1+ | 1+ |
| Knee Extensors | 1+ | 2 |
| Knee Flexors | 1+ | 2 |
| Plantar Flexors | 1 | 1 |
| Dorsiflexors | 1 | 2 |
Clinical Impression[edit | edit source]
Physiotherapy Diagnosis[edit | edit source]
Secondary Progressive Multiple Sclerosis (SPMS) presenting with decreased balance/coordination, strength, muscle weakness mainly in the LE and fatigue-like symptoms with declining functional mobility.
Problem List[edit | edit source]
| Fatigue |
| Muscle cramps/spasms/weakness/stiffness |
| Decreased sensation |
| Decreased endurance |
| Decreased balance/coordination |
| Spasticity |
| Fear/avoidance behaviour |
| Catastrophizing thinking |
Intervention[edit | edit source]
Gait Aid[edit | edit source]
- Recommending 4WW for ambulating outside for longer distances and to help with balance and coordination
Home Self-Management[edit | edit source]
- Pain education to reduce fear-avoidance of exercise
- Walking program to improve aerobic capacity/ endurance
- Starting at 5 min/session (3-5 times per week as tolerated)
- Adding 1 minute to the walk per week
- Using “Talk Test” to monitor intensity and ensure not to exacerbate fatigue or pain symptoms
- Resistance training to improve muscular endurance
- 3 times per week, 3 sets of 12-15 repetitions for each major muscle group, emphasizing functional movements. (e.g. sit-to-stand, reaching with resistance, compound full-body exercises)
- Stretching Program
- Daily; hold each stretch for 4 X 15 sec
- Stretching all major muscle groups
- Cold application at home to improve spasticity[6]
- As needed; apply every 2 hours for 15-20 minutes
- Refer to to Psychologist for Cognitive Behavioural Therapy (CBT) to address catastrophizing and fear-avoidance behaviours
Therapist-administered Interventions[edit | edit source]
- Acupuncture: Once a week for 10 weeks (or longer if patient finds beneficial) aimed at improving: fatigue, spasticity and overall quality of life[7].
- Manual Therapy: 1-2 times per week for 30 minutes (or as patient’s budget allows for)
- Aimed at improving pain, walking speed and dynamic balance[8].
Outcome[edit | edit source]
Mrs. X's follow-up assessment was conducted 2 months after her initial assessment. Beginning with the MSQOL-54 score, Mrs. X's score improved from 43 to 54 for physical health and from 40 to 46 for mental health. The Berg Balance Scale re-assessment showed an improvement from 32 to 42. The Timed 25-foot walk was re-assessed with the mobility aid this time, where in her score decreased from 10 seconds to 7 seconds. Her 9-Hole Peg test decreased from 19 seconds to 17 seconds. Lastly, her 12-Item MS walking scale decreased from 50 to 38.
Mrs. X has had fewer falls due to her gait aid and she experienced more stability with the 4WW. She also experienced positive impacts of the HEP (specifically, the walking program) in reducing her fatigue symptoms. In addition, she also had positive impact on her cardiorespiratory fitness and general health.
Mrs. X’s discharge plan should include home-based physiotherapy. The program will include a HEP, including walking, stretching, and resistance training. Her discharge plan also includes a follow-up assessment in 2 months to re-evaluate her symptoms and to track her changes in function and mobility. Re-evaluation will also include follow-up regarding catastrophizing and fear-avoidance beliefs.
Our intervention demonstrated that a short-term outpatient rehabilitation program can improve levels of fatigue, strength, and fitness and can confirm the effectiveness of individualized rehabilitation program for an MS patient.
Discussion[edit | edit source]
Mrs. X presented to the MS clinic at KGH with symptoms from her previous diagnosis with MS. As an outpatient, her goals were to seek progression management and manage her current diagnosis of MS. She presented with gait and balance issues and was prescribed a 4WW. In addition, she presented with symptoms of fatigue which was limiting her functional day-to-day activities. She was prescribed a HEP that had an aerobic component which targeted her cardiovascular fitness and fatigue symptoms. She also presented with fear-avoidance behaviour and catastrophizing thoughts, which were previously debilitating to her motivation to exercise and therefore was referred to CBT.
From our case, patients presenting with similar symptoms of MS may benefit from physiotherapy intervention involving gait and balance interventions, exercise programs that emphasize aerobic capacity/endurance, resistance training, and stretching, as well as manual therapy. Therapists carrying out program should be mindful of allowing patient to exercise within their own limits and not to point of maximal exertion, as patients with MS often present with issues with heat sensitivity - as in our case study. From a multidisciplinary perspective, patients with MS may also present with cognitive and behavioural deficits or issues around motivation and catastrophic thinking. Patients may benefit from other health care professionals such as psychologists or occupational therapists.
References[edit | edit source]
- ↑ MS Society [Internet]. Types. 2019. [cited 10 May 2019]. Available from: https://mssociety.ca/about-ms/types?gclid=EAIaIQobChMIqu3u1aqK4gIVWPfjBx20BQmKEAAYASAAEgLQgPD_BwE.
- ↑ 2.0 2.1 Galey T, Miller C, Nazareth M, Bakshi R, Brownscheidle CM, Weinstock-Guttman B, Moise C, Jacobs L. Sensory Abnormalities in MS: Patient Descriptions of “Macrosomatic Illusions”. International Journal of MS Care. 2004 Dec;6(4):144-7. Retrieved from: https://ijmsc.org/doi/abs/10.7224/1537-2073-6.4.144.
- ↑ Cosh A, Carslaw H. Multiple sclerosis: symptoms and diagnosis. InnovAiT. 2014 Nov;7(11):651-7. Retrieved from: https://journals.sagepub.com/doi/full/10.1177/1755738014551618.
- ↑ Potter K, Cohen ET, Allen DD, Bennett SE, Brandfass KG, Widener GL, Yorke AM. Outcome measures for individuals with multiple sclerosis: recommendations from the American Physical Therapy Association Neurology Section Task Force. Physical therapy. 2014 May 1;94(5):593-608. Retrieved form: https://academic.oup.com/ptj/article/94/5/593/2735536.
- ↑ Erwin A, Gudesblatt M, Bethoux F, Bennett SE, Koelbel S, Plunkett R, Sadiq S, Stevenson VL, Thomas AM, Tornatore C, Zaffaroni M. Intrathecal baclofen in multiple sclerosis: too little, too late?. Multiple Sclerosis Journal. 2011 May;17(5):623-9.
- ↑ Wolf BA. Effects of temperature reduction on multiple sclerosis. Physical Therapy. 1970 Jun 1;50(6):808-12. Retrieved from: https://www.researchgate.net/publication/18254241_Effects_of_Temperature_Reduction_on_Multiple_Sclerosis
- ↑ Karpatkin, HI, Napolione, D and Siminovich-Blok, B. Acupuncture and Multiple Sclerosis: A Review of the Evidence.Evidence-Based Complementary and Alternative Medicine. 2014; 2014: 1-9. Retrieved from: http://dx.doi.org/10.1155/2014/972935.
- ↑ Negahban H, Rezaie S, Goharpey S. Massage therapy and exercise therapy in patients with multiple sclerosis: a randomized controlled pilot study. Clinical rehabilitation. 2013 Dec;27(12):1126-36. Retrieved from:https://journals.sagepub.com/doi/full/10.1177/0269215513491586.