Urinary Tract Infection
Introduction[edit | edit source]
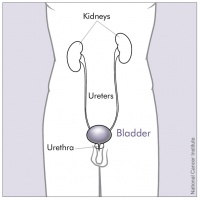
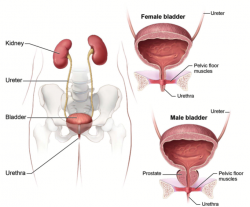
A urinary tract infection is an infection in any part of your urinary system, which includes the bladder, urethra, ureters (urine tubes) and kidneys. If untreated, UTIs can lead to kidney infection which can be very serious. UTIs are caused by microbes, mainly bacteria, but also fungi and viruses[1].
Normally, bacteria that enters the urinary tract is rapidly removed by the body before symptoms are present, but sometimes this bacteria overcomes the natural defences of the body, resulting in an infection. This infection may involve the lower urinary tract only, or both the lower and upper urinary tracts[2]. The upper urinary tract is made up of the kidneys and the ureters, while the lower urinary tract is made up of the bladder and urethra [2].
Types of urinary tract infections (UTIs)[edit | edit source]
The different types of UTI can include:
- Urethritis – infection of the urethra
- Cystitis – infection of the bladder
- Pyelonephritis – infection of the kidneys
- Vaginitis – infection of the vagina.[3]
Etiology[edit | edit source]
Pathogenic bacteria ascend from the perineum, causing the UTI.
- Women have shorter urethras than men and therefore are far more susceptible to UTI.
- A major risk factor for UTI is catheter use. Sexual intercourse and the use of spermicides and diaphragms are also risk factors for UTI. Frequent pelvic exams and the presence of anatomical abnormalities of the urinary tract can also predispose one to a UTI.
- UTIs are very common after a kidney transplant. The two triggers include the use of immunosuppressive drugs and vesicoureteral reflux. Other risk factors include the use of antibiotics and diabetes mellitus[4].
Epidemiology[edit | edit source]
An estimated 150 million UTIs occur every year world-wide, adding to $6 billion in health care costs [5].
- Urinary tract infections are very frequent bacterial infections in women.
- Usually occur between the ages of 16 and 35 years, with 10% of women getting an infection yearly and more than 40% to 60% having an infection at least once in their lives.
- Recurrences are common, with nearly half getting a second infection within a year.
- Urinary tract infections occur at least four times more frequently in females than males[4]
Characteristics/Clinical Presentation[edit | edit source]
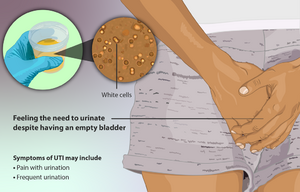
Some of the symptoms of UTIs include:
- Wanting to urinate more often and urgently, if only a few drops
- Burning pain or a ‘scalding’ sensation when urinating
- Feeling that the bladder is still full after urinating
- Pain above the pubic bone
- Cloudy, bloody or very smelly urine.
If infection reaches the kidneys, prompt medical attention is needed. In addition to the general symptoms of UTIs, a person with a kidney infection can also experience:
- Chills
- Fever
- Loin (lower abdominal) pain
- Pain in the back
- Vomiting.[3]
Urinary Tract infections that are left untreated may lead to many complications, including urosepsis, systemic inflammatory response syndrome (SIRS), and chronic kidney infections. Sepsis associated with UTIs often requires hospitalization[6].
Variation in Symptom Presentation
- Post-menopausal women present with constitutional symptoms, such as abdominal pain, back pain, chills, and constipation [2].
- Nursing home patients present with nonspecific symptoms, such as confusion and a decline in functional status.
- A urinary infection in a child needs to be investigated as it may indicate a more serious condition. The most common urinary system condition is urinary reflux. With this condition, the bladder valve isn’t working properly and allows urine to flow back to the kidneys, increasing the risk of a kidney infection[3].
Diagnosis[edit | edit source]
Tests and procedures used to diagnose urinary tract infections include:
- Analyzing a urine sample.
- Growing urinary tract bacteria in a lab. This test finds what bacteria is causing infection and which medications will be most effective.
Typically, symptoms of a UTI will conclude within 24-48 hours after treatment. A UTI is considered recurrent if the condition presents more than twice in 6 months [1]. Additional tests include the following: kidney and bladder ultrasound, voiding cystourethrogram, computerized tomography (CT) scan, MRI, radionuclide scan, urodynamics, and cystoscopy [7]
Prognosis[edit | edit source]
Even with proper antibiotic treatment, most UTI symptoms can last several days. In women with recurrent UTIs, the quality of life is poor, 25% of women experience such recurrences. Factors indicating a poor outlook include: Catheterization; Poor overall health; Advanced age; Presence of renal calculi; Diabetes (especially if poorly controlled); Presence of malignancy; Urinary Incontinence; Chronic diarrhea.[4]
Systemic Involvement[edit | edit source]
Urinary Tract infections that are left untreated may lead to many complications, including urosepsis, systemic inflammatory response syndrome (SIRS), and chronic kidney infections. Sepsis associated with UTIs often requires hospitalization[6]. Urosepsis spreads into the bloodstream from its origin in the urinary tract. Kidney infections also progress to the blood stream, referred to as septicemia[7]. This complication can be life threatening. Systemic inflammatory response syndrome can also become life threatening if treatment fails. SIRS is usually the first incidence of multi-organ failure[8].
Treatment[edit | edit source]
Antibiotics usually are the first line treatment for urinary tract infections. Which drugs are prescribed and for how long depend on persons health condition and the type of bacteria found in your urine.
The group of antibiotic medicines known as fluoroquinolones are not commonly recommended for simple UTIs, as the risks of these medicines generally outweigh the benefits for treating uncomplicated UTIs. In some cases, such as a complicated UTI or kidney infection, they may be prescribed, if there are no other treatment options.
Pain medications may be prescribed (numbs your bladder and urethra to relieve burning while urinating), but pain usually is relieved soon after starting an antibiotic[9].
Antibiotics are usually taken anywhere from 3 days to 10 days, depending on severity of symptoms, comorbidities, complications of infection, and dosage [2][1]. Overutilization of antibiotics is a common issue, particularly in hospitals and long term facilities, which may cause patients to develop resistance to the medication over time [2].
Alternative treatment includes the use of probiotics, ensuring proper hydration, drinking cranberry juice, and urinating frequently [10][6][7]. Using a heating pad on the patient’s lower back or abdomen may also help the symptoms of the UTI[11]. Surgery may be required in the presence of an anatomical abnormality [1].
Prevention[edit | edit source]
Measures include:
- Although, not evaluated in a controlled trails, women should urinate after sexual intercourse[12] because bacteria in the bladder can increase by ten-fold after intercourse.
- After urination, women should wipe from front to back, not from the anal area forward, which seems to drag pathogenic organisms nearer to the urethra.
- Vigorous urine flow is helpful to prevention.
- Baths should be avoided in favor of showers.
- A gentle, liquid soap should be used in bathing or a liquid baby soap, which is very acceptable for the vagina. The soap should be applied using a clean, soft cotton or microfiber washcloth and the vaginal area should be cleaned first to avoid unnecessary contamination of the area with germs[4]
Physical Therapy Management[edit | edit source]
Pelvic floor dysfunctions has been linked to the development of urinary incontinence as well as urinary tract infections[13]. A study concluded that improved pelvic floor muscle strength and coordination could contribute to decease in UTI re occurrence[13] Physical therapists that are trained in pelvic floor dysfunction can greatly improve a UTI patient’s quality of life. A typical approach includes training pelvic floor musculature, manipulative techniques, local heat, breathing and relaxation techniques, postural education, muscle coordination reeducation, and behavioral therapy[14].
Therapists are also encouraged to educate the patient on drinking and voiding schedules to ensure consistency[15]. Treatments and patient education have been found to improve efficiency of emptying the bladder, create better bowel habits, and promote full relaxation of the pelvic-floor when voiding[14]. All of these factors may lead to a decreased incidence and reoccurrence of UTIs.
For those patients in the hospital, recent studies have shown that mobilization of patients with a catheter is safe and is not associated with urinary-related adverse effects, including urinary tract infections[16].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Rosenblum, N. Recurrent Urinary Tract Infections. Urology. Available at: http://www.med.nyu.edu/urology/patient-care-information/conditions-we-treat/recurrent-urinary-tract-infections
- ↑ 2.0 2.1 2.2 2.3 2.4 Rowe, TA, Juthani-Mehta, M. Urinary tract infection in older adults. Aging Health. 2013;9(5).
- ↑ 3.0 3.1 3.2 Better Health UTIs Available:https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/urinary-tract-infections-uti (accessed 13.5.2022)
- ↑ 4.0 4.1 4.2 4.3 Bono MJ, Reygaert WC. Urinary tract infection. InStatPearls [Internet] 2021 Jun 23. StatPearls Publishing. Available:https://www.ncbi.nlm.nih.gov/books/NBK470195/ (accessed 13.5.2022)
- ↑ M, Pontari. Adult UTI. Advancing Urology. Available at: www.auanet.org/education/adult-uti.cfm
- ↑ 6.0 6.1 6.2 Mody, L, Juhani-Mehtta, M. Urinary Tract Infections in Older Women: A Clinical Review. JAMA. 2014;311:844–854.
- ↑ 7.0 7.1 7.2 Urinary Tract Infections in Adults. Urologic Diseases. 2013. Available at: http://www.niddk.nih.gov/health-information/health-topics/urologic-disease/urinary-tract-infections-in-adults/pages/ez.aspx.
- ↑ Grabe, M. Guidelines on Urological Infections. Urological Infections. Available at: http://uroweb.org/wp-content/uploads/19-urological-infections_lr2.pdf.
- ↑ Moyo clinic UTI Available;https://www.mayoclinic.org/diseases-conditions/urinary-tract-infection/diagnosis-treatment/drc-20353453 (accessed 13.5.2022)
- ↑ Becknell, B, Schober, M, Korbel, L, Spencer, JD. The Diagnosis, Evaluation and Treatment of Acute and Recurrent Pediatric Urinary Tract Infections. Expert Review of Anti-infective Therapy. 2015;13(1):81–90.
- ↑ Urinary Tract Infections in Adults. Urologic Diseases. 2013. Available at: http://www.niddk.nih.gov/health-information/health-topics/urologic-disease/urinary-tract-infections-in-adults/pages/ez.aspx.
- ↑ Pietrucha‐Dilanchian1 P, Hooton TM. Diagnosis, treatment, and prevention of urinary tract infection. Urinary Tract Infections: Molecular Pathogenesis and Clinical Management. 2017 Feb 15:41-68.
- ↑ 13.0 13.1 Divine K, McVey L. Physical Therapy Management in Recurrent Urinary Tract Infections: A Case Report. Journal of Women's Health Physical Therapy. 2021 Jan 1;45(1):27-33.
- ↑ 14.0 14.1 Souza, EL, Figueiredo, EM, Velloso, FB, Geo, MS. Physiotherapy For Women with Recurrent Urinary Tract Infection: A Promising Approach. International Continence Society. 2013:223.
- ↑ De Paepe, H, Hoebeke, P, Renson, C, et al. Pelvic-floor therapy in girls with recurrent urinary tract infections and dysfunctional voiding. British Journal of Urology. 1998;3:10–9113.
- ↑ Lima, NP, Cardim da Silva, GM, Park, M, Pires-Neto, RC. Mobility therapy and central or peripheral catheter-related adverse events on an ICU in Brazil. J bras pneumol. 2015;41(3):225–230.