Antibiotics
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Nupur Smit Shah and Vidya Acharya
Introduction[edit | edit source]
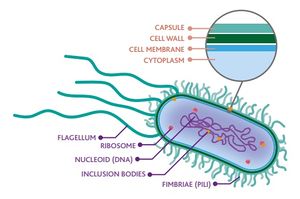
What are Antibiotics? Image R: Bacteria
- Any substance that inhibits the growth and replication of a bacterium or kills it outright.
- Designed to target bacterial infections within (or on) the body.[1]
- Some are highly specialised and are only effective against certain bacteria. Others, known as broad-spectrum antibiotics, attack a wide range of bacteria, including ones that are beneficial to us.
Pharmacology of antibiotics: Includes destroying the bacterial cell by either preventing cell reproduction or changing a necessary cellular function (eg blocking an enzymes function) or process within the cell. Classically grouped into 2 main categories based on their in vitro effect on bacteria:
- Bactericidal antibiotics "kill" bacteria - stop the mechanism responsible for building their cell walls[1].
- Bacteriostatic antibiotics "prevent growth" of bacteria - prevent the reproduction of bacteria.
- In the United States, it has been reported that nearly half of the antibiotics prescribed were incorrect in some way and almost one-third of antibiotics were deemed as unnecessary in hospitalized patients. Appropriate antibiotic use has become a public health issue[2].
Historic Perspective[edit | edit source]
The first antibiotic, salvarsan, was deployed in 1910. In just over 100 years antibiotics have drastically changed modern medicine and extended the average human lifespan by 23 years. The discovery of penicillin in 1928 started the golden age of natural product antibiotic discovery that peaked in the mid-1950s. Since then, a gradual decline in antibiotic discovery and development and the evolution of drug resistance in many human pathogens has led to the current antimicrobial resistance crisis.[3]
- Salvarsan provided the first real cure for the extremely unpleasant disease syphilis (caused by the parasitic spirochete Treponema pallidum)[4].
Approach to Antimicrobial Therapy[edit | edit source]
Empiric Therapy[edit | edit source]
- The causative organisms and infection source are not always known when a patient first presents. Antibiotic therapy is often initiated before an exact infectious disease diagnosis is made and microbiological results are available. Antibiotics used in this manner are referred to as Empiric Therapy.
- Empiric antibiotics are broad-spectrum which refers to medications that target many different types of bacterial classes (i.e., gram-positive, gram-negative, and anaerobic bacteria).
- This approach attempts to cover all potential pathogens before culture results.
- When microbiology tests result and antibiotic susceptibilities are known, definitive antibiotic therapy can then be tailored to the specific infection etiology.
Prophylactic therapy[edit | edit source]
- Used to prevent infections in patients who do not have an active infection.
- Immunocompromised patients may receive prophylaxis against certain opportunistic pathogens.
- Prophylactic antibiotics are also used before surgical procedures and in traumatic injuries such as open fractures and animal bites.
Level of aggressiveness in antibiotic therapy[edit | edit source]
- The severity of potential bacterial infection will determine this. eg in a life-threatening infectious disease such as sepsis, empiric broad-spectrum parenteral antibiotics should be administered quickly after sepsis identification and continued until more information is gathered regarding the etiology and causative bacteria.
Patient factors (to be taken into consideration)[edit | edit source]
- Patient age, medication allergies, renal and hepatic function, past medical history, the presence of an immunocompromised state, and recent antibiotic usage need to be evaluated before an antibiotic selection. These patient factors contribute to the pharmacodynamics and pharmacokinetic actions of antibiotics and influence dosing to optimize efficacy.
Adverse Reactions[edit | edit source]
i.e. A harmful or abnormal result. May be caused by administration of a medication and be indicated by an untoward result such as by illness or death
- One of 5 hospitalized patients has been shown to develop an adverse reaction to an antibiotic.
- Nearly the 1 out of 5 drug-related Emergency Department visits are due to adverse antibiotic reactions.
- Usually an immune-mediated reaction or hypersensitivity reaction (classified as an allergy). This includes IgE-mediated anaphylaxis and angioedema.
- The anticipation of adverse events is warranted when initiating antimicrobial therapy. Certain patients are at higher risk, for example, the elderly, patients with multiple co-morbidities, and hospitalized patients. [2]
Side Effects[edit | edit source]
i.e. An undesirable secondary effect which occurs in addition to the desired therapeutic effect of a drug or medication. Side effects may vary for each individual depending on the person's disease state, age, weight, gender, ethnicity and general health.
- Antibiotics commonly cause the following side effects:
- diarrhea
- nausea
- vomiting
- rash
- upset stomach
- fungal infections of the mouth, digestive tract, and vagina
2. Less common side effects of antibiotics include:
- formation of kidney stones, when taking sulphonamides
- abnormal blood clotting, when taking some cephalosporins
- sensitivity to sunlight, when taking tetracyclines
- blood disorders, when taking trimethoprim
- deafness, when taking erythromycin and the aminoglycosides
- Some people, especially older adults, may experience bowel inflammation, which can lead to severe, bloody diarrhea.
- In less common instances, penicillins, cephalosporins, and erythromycin can also cause inflamed bowels[5].
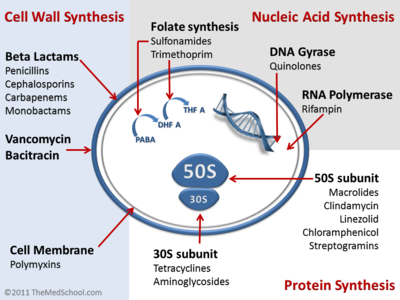
Classification of Antibiotics[edit | edit source]
A broad range of antibiotics exist, each with its own sets of usage and action mechanisms.
- The most effective classification is derived from the chemical composition (antibiotics with similar structural classes typically have comparable patterns of toxicity, effectiveness and allergic potential).
- Even though each class consists of a variety of drugs, each one is still unique in its own way.
The main classifications are:
1. Beta-Lactam Antibiotics (Penicillin & Cephalosporin)[edit | edit source]
- Penicillin: The eldest type of antibiotics is penicillin. Generally bactericidal, penicillin hinders bacteria's ability to form their cell walls. This antibiotic is often used in cases of dental, skin, respiratory tract, ear, and urinary tract infections as well as gonorrhea.
- Cephalosporin: In the same classification of antibiotics as penicillin even though its chemical structure differs in several respects. They both have a structure that hinders the growth of bacterial cell walls. The main difference is cephalosporin is cephalosporium acremonium based.
2. Fluoroquinolones[edit | edit source]
- The newest classification of antibiotics. A synthetic antibiotic, fluoroquinolones belong to the family of quinolones and are not derived from bacteria. These newer versions are broad-spectrum bacteriocidal antibiotics that are easily absorbed into the body. Because of this, fluoroquinolones can be administered in both pill form or intravenously. Fluoroquinolones work by inhibiting bacteria ability to produce DNA, making it difficult to reproduce.
- This antibiotic is mostly used to treat skin infections, urinary tract infection and respiratory infections like bronchitis and sinusitis.
3. Tetracycline[edit | edit source]
- Having a chemical structure with four rings, tetracyclines are derived from a type of Streptomyces bacteria. They are broad-spectrum bacteriostatic antibiotics, effective against a multitude of microorganisms.
4. Macrolides[edit | edit source]
- Obtained from the Streptomyces bacterium, macrolides are types of antibiotics that are bacteriostatic, thus inhibiting protein synthesis. The prototype of this class is erythromycin and is used similarly as penicillin.
5. Aminoglycosides[edit | edit source]
- Aminoglycosides are made from different Streptomyces species, which are derived from a fungus called Streptomyces griseus. They are bactericidal and stop bacteria from producing proteins[6].
Gram Staining[edit | edit source]
Bacteria can be divided into two groups on the basis of a process known as crystal violet staining, or Gram staining- these groups are known as gram-positive and gram-negative. Image: Gram stains with comparisons of gram positive and gram negative bacteria
- Gram-positive bacteria have a thicker layer of peptidoglycan that makes up the cell wall and thus stain purple in a Gram stain test. Gram-negative bacteria have a cell wall composed of a thin layer of peptidoglycan surrounded by an outer membrane. This outer membrane of gram-negative bacteria contains a unique component, lipopolysaccharide, in addition to proteins and phospholipids.
- The outer membrane of gram-negative bacteria is often hidden by a slime layer, which in turn hides the antigens of the cell. The unique structure of the outer membrane of gram-negative bacteria prevents certain drugs and antibiotics from entering into the cell, which means these bacteria have increased resistance to drugs and are more dangerous as disease-causing organisms[7].
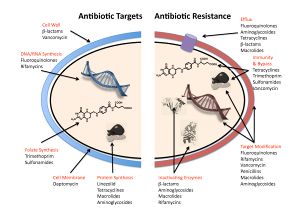
Antibiotic Resistance[edit | edit source]
The increased use of antimicrobial agents in clinical practice and other industries such as livestock farming has lead to bacteria resistant to antibiotic agents. Bacteria have developed mechanisms to promote this resistance in order to survive.
Bacteria also have the capability to gain resistance through attaining resistance genes from other bacteria or developing a mutation resulting in reduced or elimination of antibiotic efficacy. This type of resistance is known as acquired resistance
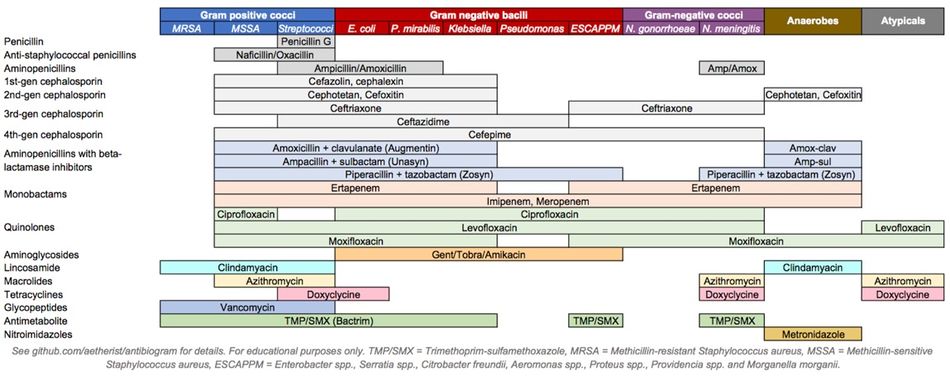
Antibiotics Coverage Diagram[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 Microbiology society Antibiotics Available from:https://microbiologysociety.org/members-outreach-resources/outreach-resources/antibiotics-unearthed/antibiotics-and-antibiotic-resistance/what-are-antibiotics-and-how-do-they-work.html (last accessed 25.11.2020)
- ↑ 2.0 2.1 Calhoun C, Wermuth HR, Hall GA. Antibiotics. [Updated 2020 Jun 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK535443/ (accessed 25.11.2020)
- ↑ Hutchings MI, Truman AW, Wilkinson B. Antibiotics: Past, present and future. Current Opinion in Microbiology. 2019 Oct 1;51:72-80.Available from:https://www.sciencedirect.com/science/article/pii/S1369527419300190 (last accessed 25.11.2020)
- ↑ Lloyd NC, Morgan HW, Nicholson BK, Ronimus RS, Riethmiller S. Salvarsan-the first chemotherapeutic compound.Available from:https://researchcommons.waikato.ac.nz/bitstream/handle/10289/188/content.pdf?sequence=1 (last accessed 25.11.2020)
- ↑ Medical News Today Antibiotics Available from:https://www.medicalnewstoday.com/articles/10278#side-effects (last accessed 26.11.2020)
- ↑ NHA How Many Classifications Do Antibiotics Have?Available from:https://www.newhealthadvisor.org/Classification-of-Antibiotics.html (last accessed 26.11.2020)
- ↑ The biochemist Gram staining Available from:https://medium.com/the-biochemists/why-are-gram-negative-bacteria-resistant-to-antibiotics-c732fe9afd06 (last accessed 26.11.2020)