Vestibular Anatomy and Neurophysiology
Introduction[edit | edit source]
The vestibular system is a part of the sophisticated human postural control system[1], normal static stance relies on three sensory inputs: vision, proprioception and vestibular[2]. It is sensitive to two types of information: the position of the head in space and sudden changes in the direction of movement of the head[3]. Together this information helps to orient a person's sense of balance and equilibrium[4].
The vestibular system is divided into a central and peripheral system.
The vestibular system has both a sensory and motor component to help us sense and perceive motion and provides information about the movement of the head and its position with respect to gravity and other inertial forces (like those generated when driving in a car). This information is used to stabilise the eyes to maintain our gaze on targets of interest, with or without head movement.[4]
The vestibular system also employs complicated strategies to maintain blood pressure when one quickly goes from supine to an erect posture. It helps us to maintain good head and body orientation in relation to our environment, most often in an upright posture[4] allowing us to maximise sensory integration of our senses (see, hear, and smell).
The Peripheral Vestibular System (PVS)[edit | edit source]
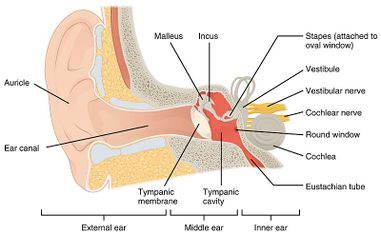
The PVS is situated in the inner ear, behind the tympanic membrane. Inputs from the PVS are integrated by the central vestibular processor called the ‘vestibular nuclear complex’ which generates motor commands to drive the eyes and the body. The system is normally very accurate. To maintain accuracy, the vestibular system is monitored and calibrated by the cerebellum[5].
Figure 1: Anatomy of the Peripheral Vestibular system
Semi-Circular Canals[edit | edit source]
The Semi-circular canals (SCC’s) are specialised mechanoreceptors to help us access information regarding angular velocity[6]. The sensory input received from the SCC’s enables the Vestibular Ocular Reflex (VOR) to generate an eye movement that matches the velocity of the head movement.
The 3 SCC’s are positioned at right angles to each other to give us feedback in 3 different planes of movement. Remember there are 2 ears, so effectively six SCC’s.
The six individual semi-circular canals become three coplanar pairs:
- right and left lateral
- left anterior and right posterior
- left posterior and right anterior
The planes of the canals are close to the planes of the extraocular muscles, so sensory neurons and motor output neurons can give quick information to individual ocular muscles.
Inside the canals there are hair cells in endolymph, and with head movement, the swishing of endolymph displaces these hair cells of the coplanar pair in opposite directions with respect to their ampullae, and neural firing increases in one vestibular nerve and decreases on the opposite side. Endolymph displacement is proportional to angular head velocity, so the semi-circular canals transmit a velocity signal to the brain.
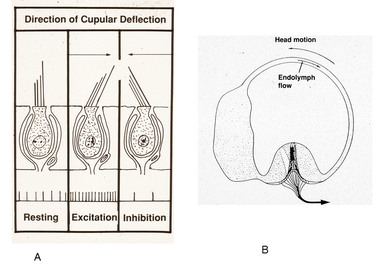
Figure 2: Endolymph displacement of coplanar pairs sends a velocity signal the brain.
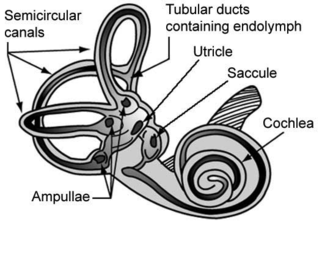
Otoliths[edit | edit source]
The Otoliths are made up of the Utricle (horizontal) and Saccule (vertical). Their job is to give us information about linear acceleration[8] by triggering an action potential to the brain to detect head position. Because earth’s gravitational field is a linear acceleration field, the otoliths register tilt[8]. For example, as the head is tilted laterally (which is also called roll), shear force is exerted upon the utricle, causing excitation, while shear force is lessened upon the saccule. Similar changes occur when the head is tilted forwards or backwards (called pitch).
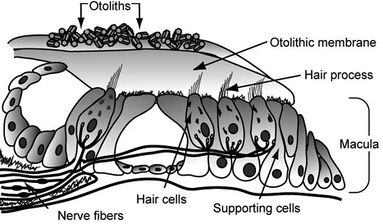
Otoconia are little calcium carbonate crystals embedded in the otolithic membrane. Head tilt and linear head motion cause displacement of the otoconial complex, producing a shearing force that deflects the hair bundles and subsequently depolarizes the sensory hair cells. These electrical signals are then relayed to the central nervous system (CNS) by the afferent vestibular nerve, which jointly with other proprioceptive information, stimulate the CNS to initiate neuronal responses for maintaining body balance.
The correct formation and anchoring of otoconia is essential for optimal vestibular function and maintaining body balance[9][10]. Otoconia abnormalities are common and can cause vertigo and imbalance in humans[10].
Side Note: Benign Paroxysmal Positional Vertigo (BPPV) is thought to be caused by dislodging of calcium carbonate crystals (otoconia) from the otolithic membrane in the utricle which migrates into one of the semi-circular canals of the inner ear. This dislodgment physically displaces hair cells on movement and creates persistent action potentials until the response is fatigued, generally within 30 to 60 seconds.
Dizziness is a common symptom post [[assessment and management of concussion] and the health professional needs to be able to differentiate dizziness from vertigo. Vertigo is most often characterised with nystagmus and dizziness particularly with positional changes of the head.
Figure 3: Otoconia embedded in the otolithic membrane
In summary, the hair cells of the canals and otoliths convert the mechanical energy generated by head motion into neural discharges directed to specific areas of the brainstem and the cerebellum. With their special orientation, the SCC’s and otolithic organs can respond selectively to head motion in particular directions. It is important to remember that the otoliths and semi-circular canals have different fluid mechanics: SCC’s measure angular velocity whereas the otoliths measure linear acceleration.
Vestibular Reflexes[edit | edit source]
Vestibular Ocular Reflex (VOR)[edit | edit source]
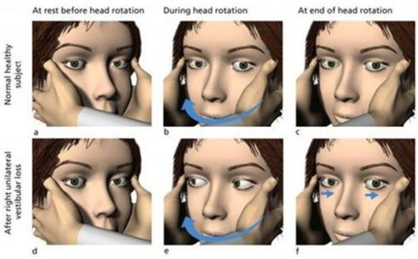
The VOR enables us to have gaze stability by maintaining stable vision during head motion[11][12]. The VOR has two components. The angular VOR, mediated by the SCC’s, compensates for rotation. The linear VOR, mediated by the otoliths, compensates for translation. The angular VOR is primarily responsible for gaze stabilization. The linear VOR is most important in situations where near targets are being viewed and the head is being moved at relatively high frequencies.
To have clear vision, the eyes must move in an equal and opposite direction during head motion. If the VOR is not firing, you will see a corrective saccade. In other words the eyes will move in the same direction as head movement before correcting and moving in the opposite direction.
Interestingly the output neurons of the VOR send information to the extraocular muscles. The extraocular muscles are arranged in pairs, which are oriented in planes very close to those of the semi-circular canals. This geometrical arrangement enables a single pair of canals to be connected predominantly to a single pair of extraocular muscles. The result is conjugate movements of the eyes in same plane as head motion.
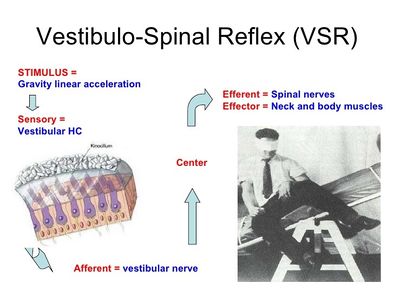
Vestibular Spinal Reflex (VSR)[edit | edit source]
The VSR stabilises the body. As an example of a vestibulospinal reflex, let us examine the sequence of events involved in generating a labyrinthine reflex.
- When the head is tilted to one side, both the canals and otoliths are stimulated. Endolymphatic flow deflects the cupula and shear force deflects hair cells within the otoliths.
- The vestibular nerve and vestibular nucleus are activated.
- Impulses are transmitted via the lateral and medial vestibulospinal tracts to the spinal cord.
- Extensor activity is induced on the side to which the head is inclined, and flexor activity is induced on the opposite side. The head movement opposes the movement registered by the vestibular system.
Figure 5: The Vestibulospinal Reflex (10)
The output neurons of the VSR are the anterior horn cells of the spinal cord gray matter, which drive skeletal muscle. However, the connection between the vestibular nuclear complex and the motor neurons is more complicated than for the VOR.
The VSR has a much more difficult task than the VOR, because there are multiple strategies that can be used to prevent falls, which involve entirely different motor synergies. For example, when shoved from behind, one’s centre of gravity might become displaced anteriorly. In order to restore “balance,” one might (1) plantarflex at the ankles; (2) take a step; (3) grab for support; or (4) use some combination of all three activities.
The VSR also has to adjust limb motion appropriately for the position of the head on the body. The VSR must also use otolith input, reflecting linear motion, to a greater extent than the VOR. The eyes can only rotate and thus can do little to compensate for linear motion, whilst the body can both rotate AND translate.
Vestibulocollic Reflex (VCR)[edit | edit source]
The VCR is a dynamic stabilizing system. This reflex maintains neck musculature in relation to head position[14].
Cervical Reflexes[edit | edit source]
The cervical spine has an important, and often under-recognized role as part of the vestibular system[14].
Cervico-collic Reflex (CCR)[edit | edit source]
The function of the cervico-collic reflex is to stabilize the head on the body and, thereby, provide information about motion of the head with respect to the trunk. Afferent sensory changes caused by changes in neck position, create opposition to that stretch by reflexive contractions of neck muscles. The CCR is a compensatory response of the neck muscles that is driven by cervical proprioceptor inputs during motion of the body.
Cervico-ocular Reflex (COR)[edit | edit source]
Cervico-ocular reflex is a feedback type reflex controlling eye movements modulated by neck proprioceptors, which can supplement the VOR.
Cervicospinal Reflex (CSR)[edit | edit source]
Cervicospinal reflex refers to the changes in limb position driven by neck afferent activity. The reticulospinal system plays a role along with the vestibulospinal system in maintaining this.
Cranial Nerve VIII and the Vestibular Nerve[edit | edit source]
The 8th cranial nerve is the Vestibulocochlear nerve, which divides to form the cochlear and vestibular nerve respectively. It contains sensory fibres for sound and equilibrium (balance), and transmits this information from the inner ear to the brain.
The vestibular nerve transmits afferent signals from the labyrinths through the internal auditory canal and enters the brainstem at the pontomedullary junction. The cochlear nerve is responsible for hearing by transmitting auditory signals from the inner ear to the cochlear nuclei within the brainstem, and ultimately to the primary auditory cortex (in the temporal lobe)[15].
The Central Vestibular Processor[edit | edit source]
There are two main targets for vestibular input from primary afferents: the vestibular nuclear complex and the cerebellum. At both locations, vestibular sensory input is processed in association with somatosensory and visual sensory input.
The vestibular system projects to many areas of the cerebral cortex but unlike other sensory systems there is no primary vestibular cortex that only receives vestibular signals. All cortical neurons that receive vestibular signals also receive other sensory signals, particularly visual and somatosensory.
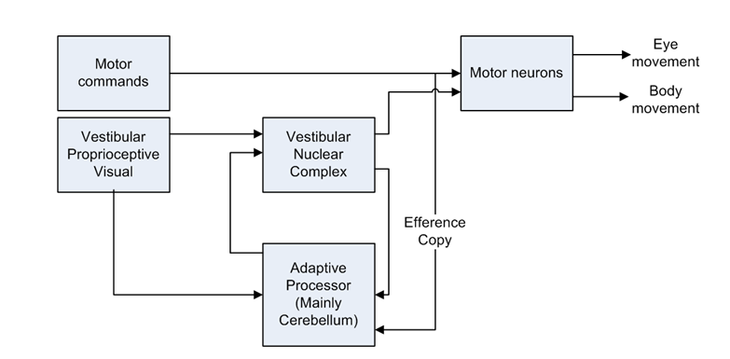
Figure 7: The Central Vestibular Processor https://www.researchgate.net/figure/Diagram-of-the-central-vestibular-system-with-multiple-interactions_fig5_47934549 (accessed 28 June 2019)
The Vestibular Nuclear Complex[edit | edit source]
The vestibular nuclear complex is the primary processor of vestibular input, and implements direct, fast connections between incoming afferent information and motor output neurons.
The vestibular nuclear complex consists of four major nuclei (superior, medial, lateral, and descending). This large structure, located primarily within the pons, also extends caudally into the medulla. The superior and medial vestibular nuclei are relays for the VOR. The medial vestibular nucleus is also involved in VSR, and coordinates head and eye movements that occur together. The lateral vestibular nucleus is the principal nucleus for VSR.
In the vestibular nuclear complex, processing of the vestibular sensory input occurs concurrently with the processing of extra-vestibular sensory information (proprioceptive, visual, tactile, and auditory). This is often referred to as sensorimotor integration.
The Cerebellum[edit | edit source]
The cerebellum is considered one of three important brain areas contributing to coordination of movement in addition to the motor cortex and basal ganglia. The cerebellum monitors vestibular performance and readjusts central vestibular processing if necessary [16]. The cerebellum receives afferent input from almost every sensory system, including the vestibular nuclear complex, consistent with its role as regulator of motor output[17].
Although not required for vestibular reflexes, vestibular reflexes become uncalibrated and ineffective when the cerebellum is removed. The cerebellar cortex, through the cerebellar and brainstem nuclei, can direct corrective action both at the cortical source through ascending pathways, as well as at the spinal cord level through descending pathways.
So in simple terms we can say that the function of the cerebellum is related to neuronal circuitry. Through this circuitry and its input and output connections, it appears to act as a comparator, a system that compensates for errors by comparing intention with performance[3]. Signs and symptoms of cerebellar dysfunction include muscle weakness, hypotonia, nystagmus (dancing eyes), intention tremors and ataxia.
Summary[edit | edit source]
The human vestibular system is made up of 3 components: a peripheral sensory apparatus, a central processor and a mechanism for motor output. The peripheral apparatus (SCC’s and Otoliths) consist of a set of motion sensors that send information to the CNS (specifically the Vestibular nuclear complex and cerebellum) about head angular velocity and linear acceleration. The CNS processes these signals and combines them with other sensory information to estimate head and body orientation.
The output of the central vestibular system goes to the ocular muscles, skeletal muscles and spinal cord to serve various important reflexes, the vestibulo-ocular reflex (VOR), vestibulocollic reflex (VCR), and the vestibulospinal reflex (VSR), cervico-ocular reflex (COR), cervicospinal reflex (CSR) and cervicocollic reflex (CCR). We can conclude that the vestibular system is a very sophisticated human control system; being able to see whilst your head is moving and being able to avoid falls is so important, even critical to survival.
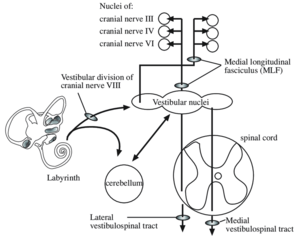
Figure 8: The organisation of the vestibular system
Additional Resources[edit | edit source]
If you are interested in learning more about the Vestibular System, the lecture below provides a comprehensive look into the Anatomy and Physiology of the Vestibular System
References[edit | edit source]
- ↑ Hain TC. Neurophysiology of vestibular rehabilitation. NeuroRehabilitation. 2011 Jan 1;29(2):127-41.
- ↑ Halmágyi GM, Curthoys IS. Vestibular contributions to the Romberg test: Testing semicircular canal and otolith function. European Journal of Neurology. 2021 Sep;28(9):3211-9.
- ↑ 3.0 3.1 Shumway-Cook A, Woollacott MH, 2007. In: Chapter 3. Physiology of Motor Control. In: Motor Control. Translating research into clinical practice. 3rd Ed. Lippincott Williams & Wilkins. Philadelphia, 2007: 46-82
- ↑ 4.0 4.1 4.2 HANRAHAN J, BLEIL C. NEURO-ANATOMY AND NEUROPHYSIOLOGY NATALIE SIMON HAZEL SANGHVI PRIYA SEKHON. The Basics of Intra-Operative Neurophysiological Monitoring for the Clinician: A Practical Guide. 2021 Jun 2:26.
- ↑ Hain TC & Helminski J, 2014. Anatomy and Physiology of the Normal Vestibular System. Chapter 1. Vestibular Rehabilitation. Herdman SJ and Clendaniel RA. 4th Ed p2-19
- ↑ Rabbitt RD. Semicircular canal biomechanics in health and disease. Journal of neurophysiology. 2018 Dec 19;121(3):732-55
- ↑ Bach-Y-Rita et al, 1971. Image direction of cupula flow
- ↑ 8.0 8.1 Kniep R, Zahn D, Wulfes J, Walther LE. The sense of balance in humans: Structural features of otoconia and their response to linear acceleration. PloS one. 2017 Apr 13;12(4):e0175769.
- ↑ Lundberg YW, Xu Y, Thiessen KD, Kramer KL. Mechanisms of otoconia and otolith development. Developmental Dynamics. 2015 Mar;244(3):239-53.
- ↑ 10.0 10.1 Hegemann SC, Bockisch CJ. Otoconial loss or lack of otoconia–An overlooked or ignored diagnosis of balance deficits. Medical hypotheses. 2019 Jul 1;128:17-20.
- ↑ Dunlap PM, Mucha A, Smithnosky D, Whitney SL, Furman JM, Collins MW, Kontos AP, Sparto PJ. The Gaze Stabilization Test Following Concussion. Journal of the American Academy of Audiology. 2019 May 1.
- ↑ Robinson DA. Neurophysiology of the optokinetic system. Progress in Brain Research. 2022 Jan 7;267(1):251-69.
- ↑ MBBS IMS MSU. CNS 15 https://www.slideshare.net/ananthatiger/cns-15?qid=cc1f4d14-630b-46e9-b8e1-8427df893928&v=&b=&from_search=1. LinkedIn Slideshare: 1-48 (accessed 27 June 2019).
- ↑ 14.0 14.1 Renga V. Clinical Evaluation of Patients with Vestibular Dysfunction. Neurol Res Int. 2019;2019:3931548.
- ↑ Bordoni B, Mankowski NL, Daly DT. Neuroanatomy, cranial nerve 8 (vestibulocochlear). InStatPearls [Internet] 2021 Jul 21. StatPearls Publishing.
- ↑ Todd NP, Govender S, Lemieux L, Colebatch JG. Source analyses of axial and vestibular evoked potentials associated with brainstem-spinal reflexes show cerebellar and cortical contributions. Neuroscience Letters. 2021 Jul 13;757:135960.
- ↑ Ghez C, Thatch WT. The cerebellum. In: Kandel E, Schwartz J, Jessel T, eds. Principles of neuroscience, 4th ed. New York: McGraw-Hill, 2000:832-852.