Wheelchair Users
Original Editor - Naomi O'Reilly as part of the Wheelchair Service Provision Content Development Project
Top Contributors - Naomi O'Reilly, Kim Jackson, Jess Bell, Simisola Ajeyalemi, Olajumoke Ogunleye, Uchechukwu Chukwuemeka, Rucha Gadgil, Amrita Patro and Lucinda hampton
Introduction[edit | edit source]
According to the WHO World Report on Disability,[1] disability is a complex multidimensional experience which poses several challenges for measurement. Broad groupings of different “types of disability or "different types of impairments" have been used to determine epidemiological data with approaches to measuring disability varying across countries, which influence the results. As such, gaining adequate epidemiological data in relation to wheelchair use is difficult but, it is estimated that approximately 15% of the global population people have a disability.[2] It is also currently estimated that 131.8 million people (or 1.85% of the global population) require a wheelchair.[3]
In the United States of America there is an estimated 3.3 million wheelchair users, with estimated 1.825 million of those users aged 65 and older, and the number increasing every year with an expected 2 Million new wheelchair users every year.[4] In Canada there are approximately 288,800 community-dwelling wheelchair and scooter users aged 15 years and over, representing 1.0% of the Canadian population. This includes 197,560 manual wheelchair users but does not include any individuals in residential or long-term care, so the true prevalence of wheelchair users in the total population in Canada is likely to be higher.[5] Finally figures from the EU's Statistics Office Eurostatin suggest an estimated 5 million wheelchair users in Europe. In 2003, it was estimated that 20 million of those requiring a wheelchair for mobility did not have one, and of those who did have a wheelchair, very few had an appropriate wheelchair to meet their needs. [6]
Wheelchair users are people who already have a wheelchair or who can benefit from using a wheelchair because their ability to walk is limited or inefficient. The needs of each wheelchair user will vary. However, they all need an appropriate wheelchair. Every well-fitting wheelchair provides the user some postural support. The backrest, cushion, footrests and armrests all provide postural support when adjusted to suit the wheelchair user’s size. However many children and adults need additional postural support in their wheelchair. Wheelchair users include Children, Adults and the Elderly; both men and women who have a wide range of mobility impairments, lifestyles, life roles and backgrounds; living and working in different environments including rural, semi-urban and urban.[6] Here we will take a look at just some of the range of wheelchair users and some of their requirements in relation to wheelchair mobility.
Non-Progressive Neurological Conditions[edit | edit source]
Cerebral Palsy[edit | edit source]
Cerebral Palsy has been defined as a group of permanent, but not unchanging, disorders of movement and/or posture, causing activity limitations which are due to a non-progressive interference, lesion, or abnormality of the developing or immature brain, resulting in a wide range of impairments which affect people very differently.[7][8]
Personal mobility can range from independent, unaided walking through to totally dependent wheelchair mobility with up to one third of children and adults with Cerebral Palsy being non-ambulant and reliant on some form of wheelchair mobility, either manual or powered, indoor or outdoor.[9] Many individuals with cerebral palsy who use a wheelchair also frequently require additional postural support for them to be functional in the wheelchair.
A recent study by Rodby-Bousquet and Hägglund describe the use of manual and powered wheelchair indoors and outdoors in relation to the degree of independent wheelchair mobility or need for assistance in children with Cerebral Palsy, suggesting that environmental factors, influence of parents, personal factors (e.g. choice, motivation, acceptance of disability) and body functions (e.g. spasticity, fatigue) are important when it comes to use of a manual or powered wheelchair, both indoors and outdoors.[9]Children at GMFCS Level III predominantly used manual wheelchairs for self-mobility, while powered wheelchairs were more frequent at GMFCS Level IV. (Fig 1). More children used a wheelchair for outdoor mobility than indoor mobility, with the number using both manual and powered wheelchair outdoors increasing with GMFCS Levels. At GMFCS Level I 2% used a wheelchair, 39% at Level II and 85-90% at Levels III-V. Similarly the number of children requiring adult assistance increased with increasing GMFCS Levels, with only 14% overall being able to independently self-propel for outdoor mobility. (Fig.1).[9]
Rodby-Bousquet and Hägglund also found a difference in wheelchair use between different subtypes of cerebral palsy, with a higher incidence of wheelchair use for indoor mobility among the dyskinetic subtype. In this group of children only 11% could self propel (Fig.2), [9] while those who were utilising Powered Wheelchairs indoors had predominantly dyskinetic cerebral palsy or spastic diplegia.More children with spastic bilateral cerebral palsy had independent wheeled mobility compared to the other subtypes, in total 24% (Fig.2). [9]
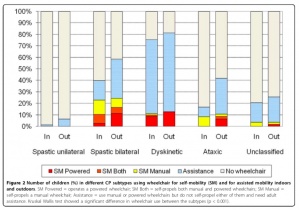

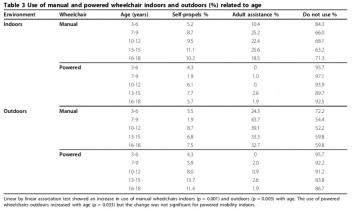
Finally Rodby-Bousquet and Hägglund [9] found that the use of manual wheelchairs for indoor mobility was similar for boys (30%) and girls (29%) with overall indoor wheelchair mobility increasing with age, although the same was not evident for powered wheelchair use.
Postural instability was seen as one of the key areas that can restrict functional performance and upper extremity function in children with cerebral palsy, in some cases leading to difficulties in self propulsion in wheelchair mobility both in manual and powered wheelchair use, with up to 89% showing instability during manual wheelchair self-propulsion and 61% during powered wheelchair self-propulsion.[13][9]
There is sometimes a resistance to prescribe a wheelchair to children, in particular younger children who may have some ability to walk. Current evidence suggests that there are many benefits for children with impaired walking ability to access a wheelchair to increase their independence in their environment, with early self-produced mobility crucial for the child's cognitive and psychosocial development. [14] Use of wheelchairs in children with impaired walking ability has been shown to have a less negative impact on visuomotor accuracy than walking with assistive devices due to a lower energy cost, while social interaction and participation in the improved. Self-initiated behaviours including interaction with objects, communication and changes in location were also more evident in children, as young as 23-38 months when provided with access to wheelchair mobility.[9][15]
To achieve as high a level of independent mobility as possible, both manual and powered wheelchairs should be considered at an early age for children with cerebral palsy who show impaired walking ability, ensuring provision of a stable sitting posture to improve function and wheeled mobility.[9]
Common characteristics that may affect Wheelchair Provision; [16][17][18][19]
- difficulty with lying, sitting or standing up;
- poor balance;
- difficulty controlling one part of the body whilst moving another – for example, sitting still while writing or taking a drink from a cup and swallowing
- high or low muscle tone;
- spasms/uncontrolled movements; poor coordination;
- a tendency to sit in the same posture all the time (habitual posture);
- other physical concerns such as visual, hearing, epilepsy, speech or communication difficulties;
- may have difficulty controlling their bowel and bladder, which may increase the risk for development of pressure sores;
- can be difficult to be able to get to a toilet and sit on or squat over the toilet independently;
- hip dislocation (the head of the femur comes out of the hip socket), which can limit movement and be painful.
Considerations for Wheelchair Use; [16]
- For most wheelchair users with cerebral palsy, good postural support is important to help improve posture, balance and how easily they can control their body to do things.
- Be aware that changes in posture may at first feel strange for a wheelchair user with cerebral palsy. The wheelchair user may need time to adjust. Consider changing postural support gradually to allow them to reach a more neutral posture over time.
- Other physical issues can have an impact upon the wheelchair and postural support solutions. Find out during the assessment what other difficulties a wheelchair user with cerebral palsy may have.
Spina Bifida[edit | edit source]
Spina Bifida is defined as a neural tube defect (NTD) that results when the inferior neuropore does not close. Developing vertebrae do not close around an incomplete neural tube, resulting in a bony defect at the distal end of the tube. [20] Symptoms of spina bifida vary widely dependant on both on the severity of the neural tube defect and the location on the spinal cord, which are also the key factor in determining the type of wheelchair mobility.
Average worldwide incidence of spina bifida is 1 per 1000 births, but marked geographic variations occur. The highest rates are found in Ireland and Wales, where 3-4 cases of myelomeningocele per 1000 population have been reported with frequencies ranging from 0.9 in Canada, 0.7 in France, 7.7 in United Arab Emirates and 11.7 in South America. [21]
Spina bifida, in particular the more severe myelomeningocele form, can cause a number of clinical and developmental concerns, typically including difficulty with mobility, altered sensation and in some cases hydrocephalus, which is often treated with a ventriculoperitoneal shunt that drains excess fluid into the abdominal cavity, where it is absorbed by the body. If this fluid imbalance creates too much pressure on the brain, it can cause damage to the brain, resulting in additional neurologic insult potentially affecting mobility i.e., tonal changes, balance issues, etc.[21]
Personal mobility can range from independent, unaided walking through to totally reliant on some form of wheelchair mobility, either manual or powered. In some children with lower-level lesions they will have some degree of ambulation, but acquisition of this mobility is often delayed, while those with higher-level lesions often have no functional ambulation, requiring manual or powered wheelchairs.
Children with sensory levels below L3 are more likely to ambulate as adults and are less likely to have pressure sores or need daily care.[22] Evidence shows that approximately 50-60% of young adults with spina bifida ambulate household or community distances, with about 20% of these using some orthotic or assistive device, while the other 50% use a wheelchair as their primary form of mobility. Approximately 20% of these individuals ambulate with orthotics and assistive devices as a form of therapeutic exercise. [22][23]
Some challenges when prescribing mobility equipment for children with spina bifida are reducing the risk for spinal deformity, risk of shoulder-overuse injury associated with lifetime wheelchair use and addressing the need for multiple types of mobility equipment, including orthotic management, ambulation aids such as crutches or walkers, and a wheelchair.
| Level of Neural
Tube Defect |
Muscle Function | Anticiapted Mobility |
|---|---|---|
| Group 1
Thoracic High Lumbar |
|
Household ambulator till approx. 13 years, with use of Hip-Knee-Ankle-Foot-Orthosis (HKAFO) or Reciprocating Gait Orthosis
95%-99% are wheelchair users as adults, although exceptions are seen Manual Wheelchair main form of mobility Power Wheelchair may be used due to impairments such as poor cardiovascular fitness, shoulder pain, severe scoliosis / kyphosis |
| Group 2
Low Lumbar |
|
Ambulation requires ankle-foot orthoses (AFO) and crutches
79% retain community ambulation as adults Most use wheelchairs for long-distance mobility Significant difference in ability to walk between L4 and L3 level Lesions Medial hamstring function is needed for community ambulation |
| Group 3
High Sacral |
|
Walks with and without support but uses AFO Braces;
Has characteristic gluteus lurch with excessive pelvic obliquity and rotation during gait |
| Group 3
Low Sacral |
|
Walks without the need for AFO’s;
Gait is close to normal |
For more information on how Spina Bifida impacts on daily function you can read the following handout from the Spina Bifida Association;
Common characteristics that may affect Wheelchair Provision; [16][25]
- movement difficulties will depend on where the spina bifida is located over the spine and how much nerve and spine cord damage is present;
- difficulty controlling the bladder and bowel;
- able to walk short distances with the use of mobility devices;
- may have a bulge at the level of spinal cord, which is damage due to the spine not developing properly (particularly if there has been no surgical intervention);
- reduced muscle control and sensation makes sitting upright more difficult;
- may have hydrocephalus caused by build up of cerebrospinal fluid. The main treatment for hydrocephalus is to surgically insert a ‘shunt’, which allows the trapped fluid to drain away - usually into the child’s stomach. If the build-up is not treated it can lead to damage of the brain;
- at risk of developing a pressure sore due to lack of sensation below the level of the injury and the presence of moisture if bowel and bladder is not effectively managed.
Considerations for Wheelchair Provision; [16]
- Ensure the wheelchair is set up to enable efficient propelling.
- The amount of postural support will depend on the level of injury. The higher the level, the more support is likely to be needed.
- If orthotics are to be worn in the day, ask the wheelchair user to wear their orthotics during the wheelchair assessment.
- If any altered spinal anatomy is present, avoid any pressure on that area. This may require shaping the backrest or adjusting the backrest upholstery to accommodate it.
- Good postural support provided early can help to prevent postural problems. This is particularly important at times of growth.
- If a child has a ‘shunt’, be aware of its position if providing a headrest. If the child has hydrocephalus, which is not being treated, refer them to a doctor.
Spinal Cord Injury[edit | edit source]
Spinal cord injury is defined as traumatic damage to the spinal cord or nerves at the end of the spinal canal, which can affect conduction of sensory and motor signals across the site of the lesion. There are two types of spinal cord injury: Incomplete and Complete injury. [26]
- Incomplete Lesion: not all the nerves are severed or the nerves are only slightly damaged. Some recovery is possible, but never to pre-injury level. The individual with an incomplete injury often has some sensation or voluntary movement below the damaged part of the spinal cord
- Complete Lesion: the nerves are severed and there is no motor or sensory function preserved of this point. [26] the individual has no sensation or voluntary movement below the damaged part of the spinal cord.
The level of spinal cord injury can be described as tetraplegia/quadriplegia, high level paraplegia or low level paraplegia. Quadriplegia/tetraplegia occurs with an injury to the Cervical Spine in the neck, and the arms, trunk, pelvis and legs are affected. High level paraplegia occurs in the Thoracic Spine T6 and above, and the trunk, pelvis and legs are affected. The arms are not affected. Low level paraplegia occurs in the lower Thoracic Spine below T6 and the Lumbar Spine and the legs are affected, the pelvis may also be affected.
Symptoms of a spinal cord injury vary widely dependant on both on the severity of injury and the location or level on the spinal cord, which are also the key factor in determining the type of wheelchair mobility. Personal mobility can range from independent, unaided walking through to totally reliant on some form of wheelchair mobility, either manual or powered.
People with a spinal cord injury are very likely to be at risk of developing a pressure sore. This is because most people with a spinal cord injury cannot feel below the level of their injury. Always prescribe a pressure relief cushion.
| Level of Injury | Type of Wheelchair Mobility |
|---|---|
| C1 - C4 Tetraplegia |
|
| C5 Tetraplegia |
|
| C6 - C8 Tetraplegia |
|
| T1 - T12 Paraplegia |
|
Common characteristics that may affect Wheelchair Provision; [16]
- complete loss of movement and sensation if the injury is complete or partial loss of movement and sensation if the injury is incomplete;
- children and adults with quadriplegia/ tetraplegia and high level paraplegia will have poor balance due to the loss of muscle movement control and sensation around the trunk. This makes sitting upright more difficult and long-term postural problems can develop quickly without the correct support from the wheelchair;
- possible difficulty with controlling bowel or bladder;
- potential spasms/uncontrolled movements of lower legs;
- children and adults with a SCI are at risk of developing a pressure sore due to:
- lack of sensation below the level of the injury;
- presence of moisture if their bowel and bladder is not effectively managed.
Considerations for Wheelchair Provision in Spinal Cord Injury; [16]
- Always prescribe a pressure relief cushion to help prevent pressure sores.
- The amount of postural support required for a wheelchair user with an SCI will depend on the level of injury. The higher the level, the more postural support is likely to be needed.
- In the early stages after injury, additional support for the trunk and arms may be necessary - particularly for high level injuries.
- Most paraplegics and some quadriplegics/tetraplegics can self- propel very effectively. Ensure the wheelchair is set up to enable an efficient propelling position.
Stroke[edit | edit source]
According to the World Health Organisation a Stroke is defined as an accident to the brain with "rapidly developing clinical signs of focal or global disturbance to cerebral function, with symptoms lasting 24 hours or longer, or leading to death, with no apparent cause other than of vascular origin and includes cerebral infarction, intracerebral hemorrhage, and subarachnoid hemorrhage". [27]
According to the World Health Organization (WHO), 15 million people suffer stroke worldwide each year. Of these, 5 million die and another 5 million are left permanently disabled.[27] The Global Burden of Disease Study suggest Stroke is the second leading cause of death globally and the third leading cause of premature death and disability as measured in Disability Adjusted Life Years (DALY). Cerebrovascular disease is the largest neurologic contributor and accounts for 4.1% of total global DALY. [28]
Symptoms of a Stroke vary widely dependant on both on the severity and the location of the infarct, which are also the key factor in determining the type of mobility. Personal mobility can range from independent, unaided walking through to reliance on some form of wheelchair mobility, either manual or powered.
Common characteristics that may affect Wheelchair Provision; [16] [29]
- Weakness, less muscle control and sometimes pain on the affected side of the body (affecting the arm, trunk and leg);
- Reduced or altered sensation on side of the body, which has been affected;
- may have a lack of awareness of side of the body, which has been affected and this may lead to increased risk of falls during transfers;
- may have difficulty sitting upright with a tendency to lean or fall towards the affected side of the body;
- may be able to stand up, and take a few steps (maybe using different gait);
- may have difficulty speaking, as well as swallowing, which makes eating and drinking difficult;
- may have difficulty controlling bowel and bladder, and it can also be difficult to be able to get to a toilet quickly enough.
Considerations for Wheelchair Use; [16]
- Provide postural support to encourage a balanced and symmetrical (both sides the same) posture.
- Flip up or swing away footrests are often very helpful for wheelchair users with a stroke who can manage a standing transfer.
- As one arm is likely to be affected, many people who have had a stroke cannot push the wheelchair using their arms. Find out if a wheelchair user can propel with their unaffected arm and steer with their unaffected leg.
- If the wheelchair user has other problems, which are not yet being addressed, refer them for further help if available.
Acquired Brain Injury[edit | edit source]
Acquired brain injury, also known as head injury or traumatic brain injury (TBI), is defined as injury to the brain which occurred as a result of trauma, and is non-progressive. Damage can be caused by an accident or trauma, brain infection, meningitis, cerebral malaria, alcohol or drug abuse.
A 2010 study looked at data from several nations, and reported that:"each year 235 000 Americans are hospitalized for non-fatal TBI, 1.1 million are treated in emergency departments, and 50 000 die. The northern Finland birth cohort found that 3.8% of the population had experienced at least 1 hospitalization due to TBI by 35 years of age. The Christchurch New Zealand birth cohort found that by 25 years of age 31.6% of the population had experienced at least 1 TBI, requiring medical attention (hospitalization, emergency department, or physician office). An estimated 43.3% of Americans have residual disability 1 year after injury. The most recent estimate of the prevalence of US civilian residents living with disability following hospitalization with TBI is 3.2 million."[30]
The problems caused by a brain injury vary depending on the part of the brain that has been damaged and the severity of the injury. Brain injuries can affect a person’s whole body, or a part of the body. Even though brain injury is a permanent injury to the brain, the effects of the injury on the person’s abilities may change over time, especially during the initial few years following injury.
Common characteristics that may affect Wheelchair Provision; [16][31]
- difficulty with moving, poor coordination and strength;
- poor sitting and/or standing balance;
- high muscle tone (stiffness of muscles), which can cause either extension or flexion patterns;
- difficulty with eating, drinking and swallowing;
- difficulty with talking, reasoning and understanding;
- changes in personality or behaviour;
- seizure;
- difficulty controlling bowel and bladder, which increases the risks of development of pressure sores
Considerations for Wheelchair Use; [16][31]
- If the wheelchair user does not have the ability to propel their wheelchair with their arms, identify whether foot propulsion would be possible.
- Frequent follow up is important as the wheelchair user’s physical abilities may change over time. This means that the amount of support needed in the wheelchair may change.
- Be aware and sensitive to possible changes in personality or behaviour related to individual’s health condition.
Polio[edit | edit source]
Polio is an infectious disease caused by a virus. [32] The virus only attacks the nerves that control movement. [33][34] One in 200 people who have polio develop some form of permanent muscle paralysis as a result (18). Polio usually affects children under the age of five. [32] The number of countries that are affected by polio has dramatically decreased in recent decades.
Common characteristics that may affect Wheelchair Provision; [16][33]
- loss of movement in affected muscles (paralysis) – usually of both legs;
- thin legs and often buttocks due to muscle wasting;
- fixed non-neutral posture around the ankles, knees and hips;
- weakness in the trunk muscles. In this case, fixed curves of the spine may develop – including scoliosis, increased thoracic curve (kyphosis), anterior pelvis tilt and increased lumbar curve (lordosis);
- strong arms developed to compensate for the weakness in their legs.
Considerations for Wheelchair Use; [16]
- People with polio have often found ways to move and carry out different activities despite the paralysis and any postural problems that they may have developed.
- As for any wheelchair user - talk with the person about what postural support they want. Carefully consider the effect of any postural correction. For example - some people with polio sit with their legs further apart or cross-legged and this helps them to balance. Trying to correct this could make their balance worse – and therefore make them less independent.
- If a wheelchair user with polio has a shortened trunk - consider increasing the height of the cushion to place them in a more efficient position for pushing.
- As many people with polio have strong arms:
- make sure the wheelchair is set up to enable an efficient propelling position;
- consider suggesting a tricycle (where available) as this is a good mobility option for longer distances.
Progressive Neurological Conditions[edit | edit source]
Progressive diseases by nature CHANGE, some slowly over a number of years but some quickly in a period of months. By ignoring that during assessment for a wheelchair and only taking a “snapshot” of how the person currently is during the seating clinic we are doing a disservice to individuals with a progressive neurological condition and potentially providing them with an inappropriate wheelchair. There are diagnosis specific considerations that should be taken into account to ensure that the seating system can react to functional declines. Providing the right support at the right time can help prevent problems with posture. This can ensure the wheelchair user is able to continue living as full a life as possible for as long as possible. Certain factors need to be taken into consideration: [16]
- delays in assessment can cause posture to become worse;
- delays between assessment and provision may mean that a wheelchair and/or seating may no longer be suitable by the time it is provided;
- frequent follow up is important as mobility and posture support needs can change quickly.
Muscular Dystrophy[edit | edit source]
Muscular Dystrophy (MD) is a group of inherited conditions that have a steady degenerative progression[35]. It causes muscles to become weak over time[36]. The muscle weakness begins in the legs most often[37]. Some forms of this disease can affect the heart and lungs, which can create life-threatening complications[36]. It can affect babies, children and adults, both males and females, and all ethnic groups. Conditions can be inherited or occur out of the blue where there is no family history. It is caused by a mutation in the genes responsible for muscle structure, which interferes with the child’s ability to function[36]. As the disease progresses, the level of disability becomes worse. Both boys and girls can be affected by muscular dystrophy, however some affect boys predominantly, such as duchenne’s muscular dystrophy, which is also the most common type of muscular dystrophy.
There are many types of muscular dystrophy. Each is classified based on their presentation
| Type | Prevalence | Common Symptoms |
|---|---|---|
| Duchenne Muscular Dystrophy | 1 in 3,500 | • Difficulty walking, running or jumping • Difficulty standing up • Learn to speak later than usual • Unable to climb stairs without support • Can have behavioural or learning disabilities |
| Facio-Scapulo-Humeral Muscular Dystrophy | 1 in 7,500 | • Sleeping with eyes slightly open • Cannot squeeze eyes shut tightly • Cannot purse their lips |
| Myotonic Dystrophy | 1 in 8000 | • Muscle stiffness • Clouding of the lens in the eye • Excessive sleeping or tiredness • Swallowing difficulties • Behavioural and learning disabilities • Slow and irregular heartbeat |
| Becker Muscular Dystrophy | Varies; 1 in 18,000 – 1 in 31, 000 |
• Learn to walk later • Experience muscle cramps when exercising |
| Limb-Girdle Muscular Dystrophy | Estimated to be in a range of 1 in 14,500 – 1 in 123,000 | • Muscle weakness in hips, thighs and arms • Loss of muscle mass in these same areas • Back pain • Heart palpitations / irregular heartbeats |
| Oculopharyngeal Muscular Dystrophy | 1-9 in 100,000 | • Does not usually appear until age 50-60 • Dropped eyelids • Trouble swallowing • Gradual restriction of eye movement • Limb weakness, especially around shoulders and hips |
| Emery-Dreifuss Muscular Dystrophy | 1 in 100,000 | • Develop symptoms in childhood and adolescence • Muscle weakness • Trouble on stairs • Tendency to trip • Slow, irregular heartbeat |
The severity of conditions and how they affect individuals varies greatly from person to person. Most conditions are progressive, causing the muscles to gradually weaken over time often affecting an individuals mobility. It is progressive, which means that many individuals who have muscular dystrophy gradually lose the ability to walk, and will require a wheelchair. At first, a person can independently propel the wheelchair with a good posture. However, the ability to maintain good posture and propel themselves decreases as the condition progresses.
Common characteristics that may affect Wheelchair Provision; [16][43][44][45]
- pain and discomfort;
- fatigue;
- progressive muscle weakness by the time the person needs a wheelchair, weakness around the pelvis, trunk and shoulders affects posture;
- changes in posture:
- due to weak muscles around the trunk and the hip joint a person with muscular dystrophy may sit with their pelvis in anterior pelvis tilt and an increased lordosis (lumbar curve);
- as muscle weakness progresses there is a high risk of scoliosis (spine curving sideways);
- difficulties in breathing due to changes in posture and muscle weakness.
- a risk of developing a pressure sore due to:
- difficulty changing position;
- being under-weight or over-weight.
Considerations for Wheelchair Use; [16][45]
- As soon as someone with muscular dystrophy (or other progressive neurological conditions) begins to need their wheelchair on a daily basis, a thorough assessment of their postural support is needed;
- Good postural support provided early can help to prevent future postural problems;
- Additional postural support should focus on supporting a neutral posture and providing increased support as needed;
- Supportive footwear and angle adjustable footrests can help maintain a neutral (or close to neutral) feet position. Where available, an ankle- foot orthosis (AFO) may also be helpful;
- Arm support is important when weakness affects the shoulders.
Multiple Sclerosis[edit | edit source]
Multiple Sclerosis (MS) is an immune-mediated disease characterized by inflammation, selective demyelination of central nervous system axons and gliosis, destroying the myelin and the axon in variable degrees causing both acute and chronic symptoms resulting into significant physical disability and impaired quality of life.[46] The course that Multiple Sclerosis can be unpredictable with the hallmark being symptomatic episodes that occur months or years apart and affect different anatomic locations. In most cases, the disease follows a relapsing-remitting pattern, with short-term episodes of neurologic deficits that resolve completely or almost completely. A minority of patients experience steadily progressive neurologic deterioration.
There are approximately 2.1 million people worldwide affected by multiple sclerosis, affecting all races and all parts of the world with rates varying widely but generally the prevalence tends to increase with latitude (eg, lower rates in the tropics, higher rates in northern Europe), but with many exceptions to this gradient (eg, low rates among Chinese, Japanese, and African blacks; high rates among Sardinians, Parsis, and Palestinians). More than 30% of people with multiple sclerosis will develop significant physical disability, with a large portion relying on wheelchair for personal mobility in particular those with primary progressive which has a high incidence of spinal cord involvement. [46]
Symptoms of a multiple sclerosis vary widely dependant on both on the subtype and the location of the lesions including sensory loss, spinal cord symptoms (motor and autonomic), cerebellar symptoms nystagmus, and intention tremor, fatigue, dizziness, pain etc, which are also the key factor in determining the type of mobility. Personal mobility can range from independent, unaided walking through to totally reliant on some form of wheelchair mobility, either manual or powered. [46]
In contrast to cases involving sudden disability, mobility aids take on a new meaning in the context of diseases like multiple sclerosis that tend toward chronic progression making it particularly challenging to decide when to recommend the use of a wheelchair and which model to use. Many individuals with multiple sclerosis can be reluctant to make use of mobility aids feeling that they will become more dependant on them and often signifying an advanced element of disease progression. The selection of an appropriate wheelchair can be more complex due to the unpredictable and potentially progressive nature of multiple sclerosis e.g. the wheelchair needs of person with multiple sclerosis can change, as does ambulatory status, because the appropriate chair for occasional community access is different from one required for full-time mobility use. Most people with multiple sclerosis start using a wheelchair, either manual or powered, just for specific activities such as outdoor mobility to help conserve strength and reduce fatigue, or as an aid to help reduce the risk of falling. The goal with individuals with multiple sclerosis is to maintain mobility, maximize stability and safety, while reducing the effort required. [47]
Motor Neuron Disease[edit | edit source]
Motor Neuron Disease are a clinically and pathologically heterogeneous group of neurologic diseases characterized by progressive degeneration of motor neurons; which include both sporadic and hereditary diseases, that progressively damages parts of the nervous system. Attacking both the upper and lower motor neurones affecting either or both of the following 2 sets of motor neurons; [48][49]
- Upper Motor Neurons (UMNs), which originate from the primary motor cortex of the cerebrum (precentral gyrus) and possess long axons forming corticospinal and corticobulbar tracts
- Lower Motor Neurons (LMNs), which originate in the brainstem (cranial nerve, motor nuclei) and spinal cord (anterior horn cells) and directly innervate skeletal muscles
Characterised by muscles stiffness, muscle twitching and spasticity, and gradually worsening weakness due to muscles atrophy which results in difficulty with activities of daily living, mobility, speech, swallow, and eventually breathing. Individuals affected by the disorder may ultimately lose the ability to initiate and control all voluntary movement, although bladder and bowel function and the muscles responsible for eye movement are usually spared until the final stages of the disorder. As motor neuron disease is rapidly progressive, services face challenges to respond to the changing needs of clients with evidence highlighting lengthy delays in supplying wheelchairs which, when provided, are no longer appropriate due to functional deterioration. [48] It is important that a person with motor neurone disease has access to a holistic wheelchair and seating assessment as early as possible. This should take into account the progressive nature of motor neurone disease and determine the type of wheelchair that will best suit the changing needs of someone with the condition.
Recent research by Rolfe aimed to identify a timeline for mapping the different types of wheelchair used by people with motor neurone disease from diagnosis to death with review of the Amyotrophic Lateral Sclerosis Functional Rating Scale (ALSFRS) and the site of disease onset as predictors of wheelchair need.[49][50]
Rolfe's Timeline (Fig.4) identifies the average time, in months, that a person with motor neuron disease is likely to need a wheelchair and the type of wheelchair, which in this study included three main types of wheelchair, with some individuals issued with more than one chair at any one time. The three types of wheelchair included;
- Lightweight Manual Chair which can be folded easily e.g. Invacare Action 2000
- Electrically Powered Indoor /Outdoor Chair e.g. Invacare Spectra Plus
- Manual Tilt-In-Space Wheelchair [50]
Average time to provision of a Lightweight Chair was 14 months (range 0-114 months), to an Electrically Powered Indoor /Outdoor Chair was 22 months (range 0-117 months) and to a Manual Tilt-In-Space Chair was 26 months (range 0 - 64). The average time between the provision of a lightweight chair and an EPIOC was 8 months (range 2-17 months); from an EPIOC to a Manual Tilt-In-Space Chair was 7 months (range 3-16); and from a Lightweight to a Manual Tilt-In-Space Chair was 18 months (range 4-30). [50]
The type of onset of disease was also mapped against the timeline of wheelchair provision and the results showed that people with bulbar-onset disease required all types of wheelchair more quickly than those with limb-onset disease, which is consistent with the faster rate of progression of bulbar-onset disease therefore wheelchair services should know the type of onset of motor neuron disease when the client is referred, in order to prioritise their resources further to ensure appropriate and timely provision. [50]
Similarly the ALSFRS Scores, when mapped to the timeline and type of chair provided, assist in predicting when a specific type of chair would be most appropriate. [51]
- The lower the ALSFRS score, the more complex the wheelchair and seating that were required (EPIOC and manual tilt in space).
- The higher ALSFRS score indicated the need for a less supportive chair, such as a lightweight self-propelling standard seat manual chair.
Therefore, knowing the ALSFRS score allows better identification of the type of equipment required.[50]
For wheelchair services to be client-centred, provide appropriate and timely access to services and equipment, be preventative and forward planning they should use the timeline and the ALSFRS score to identify the anticipated wheelchair needs of people with motor neurone disease, which would minimise equipment abandonment and prevent lengthy delays that impact upon individuals’ quality of life.[50]
Orthopaedic Conditions[edit | edit source]
Amputations[edit | edit source]
Amputation is the removal of a limb or part therof, as a result of trauma, prolonged constriction or surgery (see Pathology leading to amputation). As a surgical measure, it is used to control pain or a disease process in the affected limb such as a malignancy, infection or gangrene, while in some cases it is carried out on individuals as a preventative surgery for such problems (see Principles of Amputation). Amputations can be both congenital or acquired. When we look at describing congenital amputation the term limb difference or limb deficiency is used and simply means the partial or total absence of a limb at birth (see Paediatric Limb Deficiency). [52]
Lower extremity amputation continues to be a major source of morbidity and mortality worldwide, although the extent of this burden cannot be accurately quantified because of international variation and a lack of standardized reporting measures. All forms of lower extremity amputation incidence ranges from 46.1 to 9600 per 105 in the population with diabetes, compared to 5.8-31 per 105 in the total population, while major amputation ranges from 5.6 to 600 per 105 in the population with diabetes and from 3.6 to 68.4 per 105 in the total population. This highlight the profound impact of diabetes on amputation rates, mainly resulting from peripheral arterial disease, neuropathy and soft tissue sepsis, which are responsible for the majority of lower extremity amputations, but have show the potential for significant reductions in incidence of lower extremity amputation following introduction of specialist diabetic foot clinics. [53]
The improvement of an individual post amputation is impacted by age, physical and mental health, nutritional status, tissue perfusion, complications post amputation (e.g. poor wound healing or infection), the individual’s motivation, level of amputation, co-morbitities, smoking habits, suitability for prosthesis and the availability of rehabilitation programs, [53][54] with the overall goals of rehabilitation being to optimise the patient’s health status, quality of life and functional independence including personal mobility either through use of a prosthetic and/or wheelchair. [54]
Personal mobility can range from independent, unaided walking through to totally reliant on some form of wheelchair mobility, either manual or powered. Many individuals with amputations will require the use of a wheelchair post-operatively and during the early stages of rehabilitation so functional training to maximise independence in everyday activities needs to be addressed in both a wheelchair and with a prosthesis. It should also be noted that use of a wheelchair as “back up” mobility when a prosthesis is common and in some instances may be preferable to using a prosthesis in some situations due to comfort, function and energy factors e.g. poor fitting prosthesis, or injury/pressure area to residual limb. A wheelchair may increase and enhance function e.g. when a participant may have been using the prosthesis during the day but returns home in the evening and “can’t wait” to get the prosthesis off, they may find accessing the home in the wheelchair is convenient and requires less physical demands compared to using crutches, therefore competent wheelchair skills are essential even for those patients who are prescribed and use a prosthesis daily. [54][55]
Wheelchair use post amputation has a higher incidence in those with bilateral lower limb amputations, with more proximal amputations including hip disarticulation, transfemoral amputation and in those with non-traumatic amputations resulting from peripheral arterial disease, neuropathy and soft tissue sepsis, which tend to occur in aging populations with numerous other comorbidities such as cardiovascular disease, hypertension, renal disease, and arthritis. [53][54] The impact of lower limb amputation on older people with amputations can be complex. Taking into account all possible complications and post-operative goals is paramount for effective management of these patients and depending on their past medical and functional history, the goals and expectations of rehabilitation can be variable. [56] According to Fleury et al, there is a low prosthetic success rate in older people with amputations, with only 36% being successfully fitted with a prosthesis. This may be due to the fact that this population tend to demonstrate more inefficient ambulation, which could be associated with their age, presence of greater comorbidities, and/or higher level of amputation), which contribute to wheelchairs being their mobility device of choice as it requires less energy than walking. While in some cases a prosthesis can aid the ability of the patient to transfer more effectively, the tendency for more fragile skin leading to increased risk for wound break down combined with often decreased range of movement around the hip and knee joint often make the applicability of a prosthesis less suitable. [57]
The Amputee Mobility Predictor (AmpPro / AmpNoPro): is an instrument to assess determinants of the Lower-Limb Amputee's Ability to Ambulate and measure function post-rehabilitation. The test can be performed with or without the prosthesis. The AmpPro form & instructions can be viewed here AmpNoPro (In Appendix 2 for instructions).
Common characteristics that may affect Wheelchair Provision; [16]
- can be very active in a wheelchair if they are provided with the help to learn good wheelchair mobility skills;
- the wheelchair balance changes as there is less weight at the front of the chair;
- amputees who have diabetes may be at a greater risk of developing pressure sores as their skin may not heal well from cuts or knocks.
Considerations for Wheelchair Use; [16]
- When setting up a wheelchair for the first time for a person with an amputation, set the rear wheels in the furthest back position (if adjustable) to reduce the chance of the wheelchair tipping backwards. Active users may quickly learn to balance the wheelchair, and then move the rear wheels forward.
- It is important to consider if the wheelchair user would prefer to wear their prosthetic limb when using the wheelchair, as this may change the fit of the wheelchair.
- When teaching mobility skills:
- always be careful when an individual with an amputation first uses a wheelchair
- teach mobility skills carefully as there is a greater chance that the wheelchair user will tip backwards.
Additional Considerations for Children with a Disability[edit | edit source]
When providing a child with a wheelchair, it is important to think about how children’s lives are different from adults’. These differences affect the way the wheelchair service personnel work with children and the choices about wheelchairs and additional postural support. Some important differences are; [58]
- the activities children carry out are different to activities of adults (play, school);
- children are often very active and do not stay in one position for very long;
- children are in the care of adults;
- children cannot always speak for themselves;
- children are still developing;
- young children have a different sitting posture to adults;
- children are still growing.
Wheelchairs that meet children’s needs should support them be a part of the activities that they carry out every day. Features in a wheelchair that are important for children include:[58]
If children push themselves, the wheelchair should:
- fit well to allow them to reach the push rims with comfort;
- be light enough for children to control, particularly going up or down hill.
- Try always to make sure the child is more visible than their wheelchair.
- Extended push handles can help family members or caregivers push the wheelchair without having to bend over.
- A wheelchair that can ride over uneven and soft surfaces such as grass and sand will make it easier for children to play with their friends.
A child’s wheelchair should make it easier for them to access education and enable them to both get to school and be mobile within school environment:[58]
- If most children in the child’s community walk to school, consider whether a wheelchair can travel on these paths?
- Does the child need a wheelchair that is good for rough terrain?
- If the child will go to school in transport (for example car, bus, rickshaw, taxi), think about how the wheelchair will be transported.
- The wheelchair should make it easy for them to be at school. The child should be able to pull up to a desk, or the wheelchair needs a tray as a work surface.
Ideally, children’s wheelchairs should: [58]
- enable children to push themselves, if they are able;
- have push handles to allow peers or adults to assist;
- be able to ride over uneven and soft surfaces such as grass and sand;
- make it easier for children to get to school;
- make it easier for children to be at school.
- attractive enough in terms of design, size and colour;
Importance of an early referral for children
Early referral for children is important, however often parents or referral sources do not refer a child for a wheelchair until the child becomes too heavy to carry. Some of the reasons for this include:
- it is sometimes thought that if a child is given a wheelchair, the child will no longer try to walk;
- while children are young and light, it is easier to carry them than manage a wheelchair over what may be difficult terrain and inaccessible environments;
- parents may not have funds to pay for a wheelchair and will delay until it becomes too difficult to carry the child. It is important to reassure parents and referral sources that a wheelchair will not usually prevent a child from walking. It is more likely that early provision of a wheelchair with good postural support will help the child.
Here are some reasons why early referral is better than delaying:
- Children who have difficulty sitting upright can develop postural problems if not well supported. If a child is referred late some postural problems may have become fixed. This can make it difficult for the child to sit comfortably even with support.
- Without the experience of sitting and being mobile, a child’s development can be delayed.
- For children who have some ability to walk, using a wheelchair may make their daily life easier and allow them to do more things in a day. For these reasons it is better if children come to a wheelchair service earlier.
Additional Considerations for Individuals who are Frail[edit | edit source]
Frailty is likely to cause individuals to become tired more easily, have reduced levels of physically active and decreased strength than previously, often causing a reduction in mobility. Older adults are at a higher risk of being frail. Often elderly people who are frail are given basic wheelchairs without good postural support that do not meet their needs. However, providing an appropriate wheelchair with good postural support for frail people and elderly people who are frail can have a very positive impact on the person’s quality of life. [16][59][60][61]
Common characteristics that may affect Wheelchair Provision; [16]
- get tired quickly;
- have limited strength to self-propel;
- may find it difficult to maintain an upright posture due to fatigue and general weakness;
- may be at risk of developing a pressure sore due to:
- thin / papery skin, which can bruise easily;
- slow healing time for bruises and pressure areas;
- if very weak, may be unable to reposition independently.
Considerations for Wheelchair Use; [16]
- Assess the amount of postural support needed carefully, considering that the longer the wheelchair user sits in the wheelchair the more tired he/she is likely to become, and the more the support that may be required.
- Wheelchair features that may be useful include:
- armrests provide additional postural support and assist with pushing up for transfers;
- footrests that swing out of the way to facilitate standing transfers for those that are able to stand;
- push handles to enable other people to assist with pushing;
- a lightweight wheelchair, which will require less energy for the wheelchair user to push themself.
References[edit | edit source]
- ↑ World Health Organisation. World Report on Disability 2011. World Health Organisation. Geneva. 2011. Available at; http://www.who.int/disabilities/world_report/2011/en/ (accessed 2 June 2018)
- ↑ The World Bank. Disability Inclusion. Available from: https://www.worldbank.org/en/topic/disability (accessed 15 June 2022).
- ↑ Wheelchair Foundation. Wheelchair needs in the world. Available from:https://www.wheelchairfoundation.org/fth/analysis-of-wheelchair-need/ (accessed 13 Junes 2022).
- ↑ Karmarkar AM, Dicianno BE, Cooper R, Collins DM, Matthews JT, Koontz A, Teodorski EE, Cooper RA.Demographic Profile of Older Adults using Wheeled Mobility Devices. Journal of Aging Research. 2011;2011.
- ↑ Smith EM, Giesbrecht EM, Mortenson WB, Miller WC. Prevalence of wheelchair and scooter use among community-dwelling Canadians. Physical therapy. 2016 Aug 1;96(8):1135-42.
- ↑ 6.0 6.1 William Armstrong, Johan Borg, Marc Krizack, Alida Lindsley, Kylie Mines, Jon Pearlman, Kim Reisinger, Sarah Sheldon. Guidelines on the Provision of Manual Wheelchairs in Less Resourced Settings. World Health Organization; Geneva: 2008.
- ↑ Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M, Damiano D, Dan B, Jacobsson B. A report: the definition and classification of cerebral palsy April 2006. Dev Med Child Neurol Suppl. 2007;49(Feb s109):8–14.
- ↑ SCPE. Dev Med Child Neurol 42 (2000) 816-824
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 9.8 Rodby-Bousquet E, Hägglund G. Use of Manual and Powered Wheelchair in Children with Cerebral Palsy: A Cross-sectional Study. BMC Pediatrics. 2010 Dec;10(1):59.
- ↑ Rodby-Bousquet E, Hägglund G. Use of Manual and Powered Wheelchair in Children with Cerebral Palsy: A Cross-sectional Study. BMC Pediatrics. 2010 Dec;10(1):59.
- ↑ Rodby-Bousquet E, Hägglund G. Use of Manual and Powered Wheelchair in Children with Cerebral Palsy: A Cross-sectional Study. BMC Pediatrics. 2010 Dec;10(1):59.
- ↑ Rodby-Bousquet E, Hägglund G. Use of Manual and Powered Wheelchair in Children with Cerebral Palsy: A Cross-sectional Study. BMC Pediatrics. 2010 Dec;10(1):59.
- ↑ Lacoste M, Therrien M, Prince F: Stability of Children with Cerebral Palsy in their Wheelchair Seating: Perceptions of Parents and Therapists. Disabil Rehabil Assist Technol. 2009, 4 (3): 143-150. 10.1080/17483100802362036.
- ↑ Tefft D, Guerette P, Furumasu J: Cognitive Predictors of Young Children's Readiness for Powered Mobility. Dev Med Child Neurol. 1999, 41 (10): 665-670. 10.1017/S0012162299001371.
- ↑ Butler C: Effects of Powered Mobility on Self-Initiated Behaviors of Very Young Children with Locomotor Disability. Dev Med Child Neurol. 1986, 28 (3): 325-332. 10.1111/j.1469-8749.1986.tb03881.x.
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 16.13 16.14 16.15 16.16 16.17 16.18 16.19 Sarah Frost, Kylie Mines, Jamie Noon, Elsje Scheffler, and Rebecca Jackson Stoeckle. Wheelchair Service Training Package - Reference Manual for Participants - Intermediate Level. Section B. Wheelchair Service Steps. World Health Organization, Geneva. 2013
- ↑ World Health Organization. (1993). Promoting the Development of Young Children with Cerebral Palsy: A Guide for Mid-level Rehabilitation Workers. Retrieved from http:// whqlibdoc.who.int/hq/1993/WHO_RHB_93.1.pdf
- ↑ Kigger, K. (2006). Cerebral Palsy: An Overview.American Family Physician, 73(1), 91–100.
- ↑ Rosenbaum, P. (2003). Cerebral palsy. What Parents and Doctors Want to Know. British Medical Journal, 326, 970–974
- ↑ Lundy-Ekman L. Neuroscience: Fundamentals for Rehabilitation. 3rd Edition. St. Louis: Saunders, 2007.
- ↑ 21.0 21.1 Medscape. Spina Bifida. https://emedicine.medscape.com/article/311113-overview#a6 (accessed 9 June 2018).
- ↑ 22.0 22.1 Oakeshott P, Hunt GM, Poulton A, Reid F. Open Spina Bifida: Birth Findings Predict Long-term Outcome. Archives of Disease in Childhood. 2011 Nov 1:archdischild-2011.
- ↑ Hoffer MM, Feiwell E, Perry R, Perry J, Bonnett C. Functional Ambulation in Patients with Myelomeningocele. JBJS. 1973 Jan 1;55(1):137-48.
- ↑ Wyszynski DF, editor. Neural Tube Defects: From Origin to Treatment. Oxford University Press; 2005 Oct 13.
- ↑ World Health Organization. (1996). Promoting the Development of Infants and Young Children with Spina Bifida and Hydrocephalus. Retrieved from http://whqlibdoc.who. int/hq/1996/WHO_RHB_96.5.pdf
- ↑ 26.0 26.1 Frederick M Maynard et al., International Standards for Neurological and Functional Classification of Spinal Cord Injury, American Spinal Injury Association, 1996
- ↑ 27.0 27.1 Global Burden of Stroke. The Atlas of Heart Disease and Stroke. MacKay J, Mensah GA. World Health Organization.
- ↑ Feigin VL, Forouzanfar MH, Krishnamurthi R, Mensah GA, Connor M, Bennett DA, Moran AE, Sacco RL, Anderson L, Truelsen T, O'Donnell M. Global and Regional Burden of Stroke during 1990–2010: Findings from the Global Burden of Disease Study 2010. The Lancet. 2014 Jan 18;383(9913):245-55.
- ↑ World Health Organization. (2012). Stroke, Cerebrovascular Accident. Retrieved from http://www.who.int/topics/cerebrovascular_accident/en
- ↑ The Epidemiology of Traumatic Brain InjuryfckLRCorrigan, John D. PhD, ABPP; Selassie, Anbesaw W. DrPH; Orman, Jean A. (Langlois) ScD, MPH The Epidemiology of Traumatic Brain Injury March/April 2010 - Volume 25 - Issue 2
- ↑ 31.0 31.1 World Health Organization, United States Department of Defense Drucker Brain Injury Center, Moss Rehab Hospital. (2004). Rehabilitation for persons with traumatic brain injury. Retrieved from http://whqlibdoc.who.int/hq/2004/WHO_DAR_01.9_eng.pdf
- ↑ 32.0 32.1 World Health Organization. (2012). Poliomyelitis. Retrieved from http://www.who.int/mediacentre/factsheets/fs114/en/
- ↑ 33.0 33.1 World Health Organization. (1993). Rehabilitation surgery for deformities due to poliomyelitis. Retrieved from http://whqlibdoc.who.int/publications/1993/9241544570.pdf
- ↑ Polio Global Eradication Initiative. (n.d.). Polio and prevention. Retrieved from http://www.polioeradication.org/Polioandprevention.aspx
- ↑ 35.0 35.1 TECKLIN, J.S., 2006. Pediatric Physical Therapy [editied by] Jan S. Tecklin. Philadelphia : Lippincott Williams and Wilkins, 2008; 4th ed.
- ↑ 36.0 36.1 36.2 NHS., 2013. Muscular Dystrophy [online]. [viewed 3 October 2014]. Available from: http://www.nhs.uk/conditions/muscular-dystrophy/Pages/Introduction.aspx
- ↑ MEDLINEPLUS., 2014. Duchenne Muscular Dystrophy [online]. [viewed 3 October 2014]. Available from: http://www.nlm.nih.gov/medlineplus/ency/article/000705.htm
- ↑ CENTERS FOR DISEASE CONTROL AND PREVENTION., 2014. Facts About Muscular Dystrophy [online]. [viewed 2 October 2014]. Available from: http://www.cdc.gov/ncbddd/musculardystrophy/facts.html
- ↑ ORPHANET., 2007. Duchenne and Becker Muscular Dystrophy [online]. [viewed 6 October 2014]. Available from: http://www.orpha.net/consor/cgi-bin/OC_Exp.php?Lng=EN&Expert=262
- ↑ FSH SOCIETY: FACIOSCAPULOJUMERAL MUSCULAR DYSTROPHY., 2010. About FSHD [online]. [viewed 5 October 2014]. Available from: https://www.fshsociety.org
- ↑ NHS., 2013. Muscular Dystrophy – Types [online]. [viewed 3 October 2014]. Available from: http://www.nhs.uk/Conditions/Muscular-dystrophy/Pages/Symptoms.aspx
- ↑ SUOMINEN, T., BACHINSKI, L., AUVINEN, S., HACKMAN, P., BAGGERLY, K., ANGELINI, C., PELTONEN, L., KRAHE, R. and UDD, B., July 2011. Population frquency of myotonic dystrophy: higher than expected frequency of myotonic dystrophy type 2 (DM2) mutation in Finland.vol. 19, no. 7 pp. 776-82 Available from: http://www.ncbi.nlm.nih.gov/pubmed/21364698
- ↑ Muscular Dystrophy Campaign. (2002). Duchenne muscular dystrophy. Retrieved from http://www.muscular-dystrophy.org/
- ↑ Brooke, M.H., et al. (1989). Duchenne muscular dystrophy: Patterns of clinical progression and effects of supportive therapy. Neurology, 39, 475–481.
- ↑ 45.0 45.1 Muscular Dystrophy Campaign. (2011).Wheelchair provision for children and adults with muscular dystrophy and other neuromuscular conditions: Best practice guidelines. Retrieved from http://www.muscular-dystrophy.org/
- ↑ 46.0 46.1 46.2 Medscape. Multiple Sclerosis. https://emedicine.medscape.com/article/1146199-overview (accessed 02 June 2018)
- ↑ Brown TR, Sliwa J. Wheelchair Prescription for People With MS: Ask the Right Questions, Get the Right Answers. International Journal of MS Care. 2005;7(3):115-6.
- ↑ 48.0 48.1 Talbot K, Marsden R (2008) Motor neuron disease: the facts. Oxford: Oxford University Press.
- ↑ 49.0 49.1 Talbot K, Turner M, Marsden R, Botell R (2009) Motor neuron disease: a practical manual. Oxford Care Manuals. Oxford: Oxford University Press.
- ↑ 50.0 50.1 50.2 50.3 50.4 50.5 Rolfe J. Planning wheelchair service provision in motor neurone disease: implications for service delivery and commissioning. British Journal of Occupational Therapy. 2012 May;75(5):217-22.
- ↑ Cedarbaum J, Stambler N (1997) Performance of the Amyotrophic Lateral Sclerosis Functional Rating Scale (ALSFRS) in multicentre clinical trials.Journal of the Neurological Sciences, 152(Supplement 1), s1-s9.
- ↑ Limb Loss Definitions. Fact Sheet. Amputee Coalition 2008. http://www.amputee-coalition.org/resources/limb-loss-definitions/ [accessed 24 Sep 2017]
- ↑ 53.0 53.1 53.2 Moxey PW, Gogalniceanu P, Hinchliffe RJ, Loftus IM, Jones KJ, Thompson MM, Holt PJ. Lower extremity amputations—a review of global variability in incidence. Diabetic Medicine. 2011 Oct;28(10):1144-53.
- ↑ 54.0 54.1 54.2 54.3 VA/DoD, 2008, VA/DoD Clinical Guidelines for Rehabilitation of Lower Limb Amputation, Online accessed 1st June 2018 https://www.healthquality.va.gov/guidelines/Rehab/amp/VADoDLLACPG092817.pdf
- ↑ College of Occupational Therapists, 2011, ‘Occupational therapy with people who have had lower limb amputations evidence based guidelines’, College of Occupational Therapists, Brunel, London
- ↑ Fried L, Ferrucci L, Darer J, Williamson J, & Anderson G (2004), 'Untangling the Concepts of Disability, Frailty, and Comorbidity: Implications for Improved Targeting and Care', Journal of Gerontology, Vol.59, No. 3, pp.255-263.
- ↑ Fleury A, Salih A, & Peel N (2013), 'Rehabilitation of the older vascular amputee: A review of the literature', Geriatric and Gerontology International, vol.13, pp. 264-273.
- ↑ 58.0 58.1 58.2 58.3 Sarah Frost, Kylie Mines, Jamie Noon, Elsje Scheffler, and Rebecca Jackson Stoeckle. Wheelchair Service Training Package - Reference Manual for Participants - Intermediate Level. Section A.2 Children with Disabilities. World Health Organization, Geneva. 2013
- ↑ Fried, L., et al. (2001). Frailty in older adults: Evidence for a phenotype. Journal of Gerontology, 56, 146–156
- ↑ Bortz,W. (2002).A conceptual framework of frailty:A review. Journal of Gerontology, 57A(5), M283–M288.
- ↑ Lang, P., Michel, J. P., & Zekry, D. (2009). Frailty syndrome:A transitional state in dynamic process. Gerontology, 55, 539–549.









