Palliative Care Competence Framework for Physiotherapists
Original Editor - Your name will be added here if you created the original content for this page.
Top Contributors - Charlotte Kay, Yasmin Natasha Milne, Emma Clare Sneddon, Sarah Brennan, Lauren Lopez, Kim Jackson, 127.0.0.1, Jane Hislop, Admin, Evan Thomas and Lucinda hampton
</div>
Introduction and Learning Outcomes[edit | edit source]
Welcome to this online learning resource focussing on “The role of the Physiotherapist in Palliative Care for people with Lymphoedema”. This has been designed by a group of fourth year Physiotherapy students from Queen Margaret University as part of the “Contemporary and Emerging Issues in Physiotherapy” module.
Aims
The aim of this wiki is to present a learning resource for final year physiotherapy students and new graduates to develop their knowledge and understanding of:
- The role of a physiotherapist in the management of people with lymphoedema
- The implications for physiotherapy practice when managing people with lymphoedema in a palliative care setting
Learning Outcomes
By the end of this wiki you should be able to:
- Discuss the background of lymphoedema and describe the key presenting symptoms
- Discuss the physiotherapist’s role in the management of people with lymphoedema
- Critically reflect on the physiotherapist’s approach in the management of people with palliative care needs who have lymphoedema
- Critically appraise and synthesise the literature relating to the end of life care for a person with lymphoedema
Overview of Lymphoedema
[edit | edit source]
Introduction[edit | edit source]
This section of the wiki will aim to provide an overview of:
- The pathophysiology of lymphoedema
- The two types of lymphoedema - primary and secondary
- The four stages of the condition
- Clinical features (physical and psychological) those with the condition may present
- Two of the main leading causes related to lymphoedema - cancer and infection
- Epidemiology regarding the condition
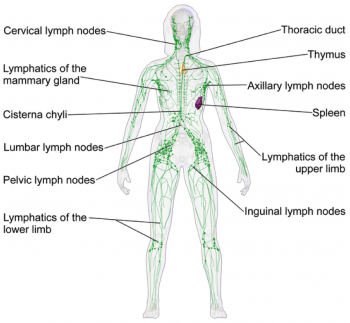
Lymphatic System[edit | edit source]
The lymphatic system is part of the body's immune system that plays a role in fighting harmful cells, for example, bacteria. It consists of lymph fluid, lymph nodes, lymph vessels and lymph tissue.
Lymph tissue insulates and protects the lymphatic system from damaging cells. Lymph fluid contains infection-fighting white blood cells. It circulates throughout the lymphatic system and is formed when interstitial fluid is collected through lymph channels (vessels, ducts and capillaries).
Lymph is primarily made up of a white watery substance:
PICTURE OF LYMPH COMPOSITION
The main lymphatic functions:
1. Helps immune system respond to the body
2. Redistribution of fluid in the body
3. Lymph carries proteins, solids, and liquids away from tissue space
a. Remove waste products from interstitial space (between all body tissue) (Seifter et al 2005)
b. Bacteria, toxins and foreign bodies are removed from tissues
4. Controls the flow of large molecules around the body (National Lymphoedema Network 2013)
5. Controls tissue fluid homeostatsis (Ridner 2013) to maintain the structure and functional aspects of tissue.
The flow of lymph fluid is unidirectional, towards the heart to provide cells with oxygen. It is protein-rich and fights abnormal cells due to its white cell content (Cancer Research UK 2014).
There are approximately 600 to 700 lymph nodes located around the body, specifically under the arm, in the abdomen, groin and neck. (Hampton 2015). Their role involves transporting lymph fluid around the body using specific lymph channels located on left and right sides. The fluid then passes through superficial primary lymph vessels (that drain the skin) and is emptied into deep secondary lymph vessels (which also contains drainage from internal organs). Adequate flow of lymph fluid is dependant on muscle contractions and an efficient respiratory system, for example, exercise (Kerchner et al 2008).
The lymphatic system can become blocked from localised fluid retention and tissue swelling within the body – known as Lymphoedema. It occurs when the function of the lymphatic system is compromised in some way. Lymph pathways are unable to exchange nutrients effectively within the interstitial spaces, causing a build up of excess fluid. Upper and lower extremities are affected depending on which area of the body is damaged. The cause of onset determines whether the affected person has either primary or secondary lymphoedema.
Activity[edit | edit source]
Take 10 mins to complete the activity below. Using the information provdied so far, match the different components of the lymphatic system with their definitions:
Types of Lymphoedema[edit | edit source]
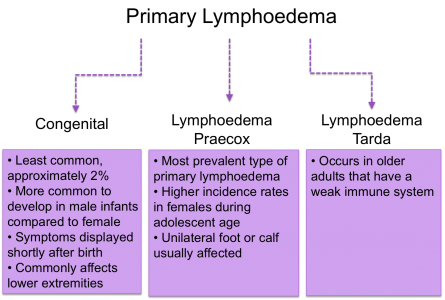
Primary
Approximetaly 1 in 6000 people develop primary lymphoedema. This form of lymphoedema isn’t inherited through family history and wouldn’t be passed onto future generations. However, people can develop primary lymphoedema in relation to other genetic and congenital abnormalities (Lymphoedema Support Group 2003).
There are three classifications depending on the onset of symptoms:
Secondary
Secondary lymphoedema is more common than the primary form. The lymphatic system is damaged due to an external cause compromising the function of the lymph nodes. Consequently, swelling accumulates in the affected part of the body.
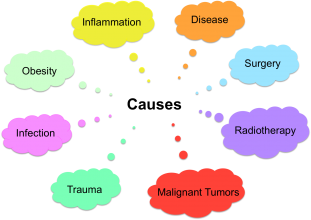
Causes of secondary lymhoedema include (NHS Choices 2014):
- Surgery (cancer and non-cancer related) – increases the risk of disturbing the function of lymphatic pathways
- Radiotherapy - destroys cancerous tissue but can also damage healthly lymph nodes
- Infections – contributes to increased swelling in the affected area
- Inflammation – contributes to excess fluid build up in the affected area
- Obesity – increased the pressure on the lymphatic system that could ultimately damage lymph nodes
- Disease (venous or joint)
The most common causes of secondary lymphoedema are cancer and non-cancer related surgery. Although these treatments have a number benefits, their outcomes can lead to disruption of the lymphatic system.
In developing countries the most common cause of secondary lymphoedema is filiariasis, a parasitic infection with filarial worms (WHO 2016). In more developed countries malignancy is the main root of cause for acquiring secondary lymphoedema (Kerchner 2008).
Causes of upper limb lymphoedema include (The Lymphoedema Support Network year):
- Trauma or injury – removal of lymph nodes during breast cancer surgery, upper body radiotherapy, burns, and scarring
- Cancer that has spread to the upper body compromising the function of the lymph nodes
- Following deep vein thrombosis (DVT) or high doses of intravenous (IV) drugs
- Reduced upper limb mobility as a result of an illness, for example, multiple sclerosis or stroke
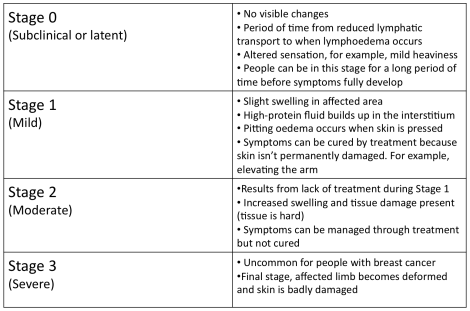
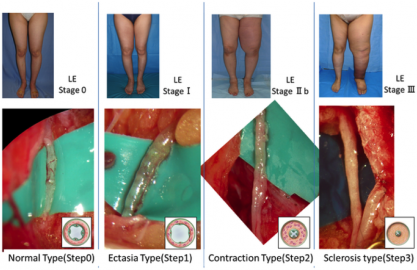
Stages Of Lymphoedema[edit | edit source]
(breastcancer.org 2015)
There are 4 Stages of lymphoedema:
Lymphoedema is a chronic and incurable condition so treatment strategies focus on reducing disease progression, for example, swelling management and infection prevention.
Clinical Features
[edit | edit source]
There are both physical and psychological effective of the chronic condition. Early diagnosis is vital to ensure the correct treatment is chosen.
Physical changes
- In the early stages pitting oedema occurs where the skin is pressed leaving an indent in the swelling. Elevating the arm creates a draining effect to reduce swelling
- Limbs can feel heavy and achy
- There is altered sensation, for example, pins and needles
- Reduced mobility and range of movement of the affected limb/s
- Pain and joint discomfort
- Skin changes, for example redness and increased temperature
- Nail discoloration (Lyons and Modarai 2013)
- Hyperkeratosis (thickening of the skin) and lymphangiectasia (dilated superficial lymph vessels) (The Lymphoedema Support Network 2015)
(Cancer Research UK 2014; McCallin et al 2005)
When the condition affects the lower extremities, over time the affected person’s gait pattern is altered, leading to a higher risk of disability.
Psychological Effects
There are psychological effects associated with the condition as a result of changes to body image.
- Swelling and weight gain impact physical appearance that can affect one’s perception of how they look, consequently decreasing their self-confidence (Harmer 2009; McCallin et al 2005)
- People commonly detach themselves from social events with family and friends leading to social isolation (Ridner 2009)
- Disturbed sleeping pattern
- Some people may feel they have a lack of support
- Financial concerns as a consequence of treatment cost and potential job loss/change (Ridner 2009)
Mason et al (2008) conducted a systematic review of literature that looked at the psychosocial aspects related lymphoedema. It was found that people with the condition experience anger, depression, anxiety and relationship issues. People can feel embarrassed having to wear different clothes due to compression bandaging, swelling and weight gain. Ultimately, there is an overall decrease in quality of life (QoL) from reduced social and leisure activities. The study concluded more research is required that focuses on improving specific psychosocial issues rather targeting QoL to reslove issues such as anger and depression.
Another study looked at the incidence, cost of treatment and complications of lymphoedema following breast cancer treatment. It concluded that 10% of the 1877 participant showed signs of lymphoedema 2 years after breast cancer treatment. A complication of the condition was the high medical costs for treatment. This lead to increased length of stay in hospital and ultimately reduced the patient’s quality of life (Ridner 2009).
It is important for health professionals to recognise and fully understand the psychological and psychosocial implications for each individual patient to ensure person-centred care is provided. Communication and appropriate referrals to other health professionals is important in overall management of the condition, for example social workers and psychologists.
Activity[edit | edit source]
This activity will take approximately 15 minutes to complete.
Relfect on your learning regarding the different stages of lymphoedema and think about how a person's body image will change as they progress through each stage. Other resources such as the internet, books and journals will provide additional information and images to help enhance your understanding when completing this activity.
Leading Causes[edit | edit source]
Cancer
Lymphoedema following breast cancer surgery is the highest overlooked cause of secondary lymphoedema. Harmer (2009) states approximately 20% of people will acquire lymphoedema after receiving this treatment. The procedure involves removing one or more lymph nodes located under the arm. Consequently, the remaining lymph nodes are put under strain and unable to work properly resulting in a build up of excessive fluid in the affected area (breastcancer.org 2015). Cancer Research UK (2014) discusses the vicious cycle between cancer and the body’s immune system. Cancerous cells are destroyed by the immune system and treatments for cancer. However, the condition can weaken the immune system if lymph nodes are blocked by cancerous tissue and unable to function properly.
A combination of surgery and radiotherapy treatment leads to a higher risk of acquiring secondary lymphoedema. Radiation therapy aims to stop cancer from coming back by using high-radiation energy to destroy cancerous cells (National Cancer Institute 2010). It either occurs before surgery to reduce the size of a tumour, or after surgery to abolish the remainder of the tumour. Lymphoedema can occur as a result of this treatment when the function of the lymphatic system has been comprised and fluid isn’t drained away (NHS Choices 2014).
Infection
Infection is a key issue commonly related to lymphoedema. It either results from swelling or causes it to develop (Hampton 2015). Lymph nodes help fight infections but when they are damaged infections can develop quicker. The Lymphoedema Support Network (2010) defines cellulitis as “acute spreading inflammation of the skin and subcutaneous tissue”. It causes the skin to become warm, red, swollen and painful with onset either sudden or progressing over a few hours. If the lymph tissue is damaged there is added strain on the lymphatic system. In an infected limb, the inflammatory process cause attracts fluid causing an increase in swelling. Consequently, lymphoedema is exacerbated during this period of infection (McGilvray year).
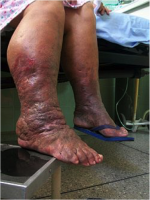
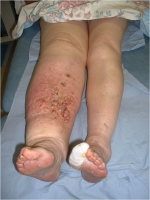
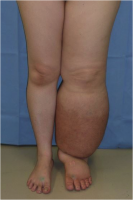
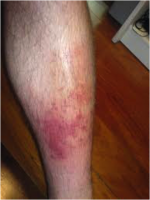
75-90% of cellulitis occurs in the lower body and is caused by bacteria entering inflamed or broken skin. A study found that the condition was responsible for 3% of admissions in a UK hospital (Al-Niaimi and Cox, 2009). This common occurrence puts financial strain on the NHS; therefore, infection prevention is a large part of lymphoedema treatment. There is a strong link between leg cellulitis and lymphoedema, where progression of the condition can lead to ulceration and septicaemia. Each cellulitis episode exacerbates secondary lymphoedema, which in turn increases the risk for a further infection episode. A Cochrane review found that a quarter of lymphoedema patients would acquire cellulitis (Al-Niaimi and Cox, 2009).
Above: Cellulitis in a lower limb
Epidemiology[edit | edit source]
Epidemiology looks at why diseases or conditions develop in different societies and how common the occurnace is. The information gathered is then used to improve current and future healthcare in disease management (BMJ 2016). Below provides an insight into some of the epidemiology regarding lymphoedema:
- Lymphoedema occurs in approximately 240,000 people in the UK with older adults more susceptible than the younger population (Nazarko 2015)
- Within 3 years after cancer surgery 80% of people will develop secondary lymphoedema
- Another study concluded 1 in 5 patients will develop lymphoedema after 6 months post breast cancer surgery (Harmer 2009)
- One study looked at a population of 600,000 people over the age of 65 and concluded 1 in 200 people had chronic lymphoedema. 50% of these people had a reduced quality of life and hospital care cost the NHS £2300 (Hampton 2015)
- Rockson and Rivera (2008) mention that 1.15 in 100,000 people under the age of 20 will acquire primary lymphoedema
- One study surveyed 308 centres (2743 people) in Spain and found that 36.8% suffered from primary lymphoedema. Of the 36.8%, 2% had acquired it at birth, 30% during adolescence and 68% were older adults (Williams et al 2005)
- One study found that out of 287 breast cancer survivors, 48% had upper limb swelling at least once and 34% had clinical symptoms of lymphoedema 6 years post treatment (Ridner 2013)
Activity[edit | edit source]
Now that you have completed this section of the wiki module. Take approximately 15 minutes to complete the following quiz
Conclusion[edit | edit source]
This section aimed to provide an insight into the background of lymphoedema to form a base of knowledge that will be futher developed throughout the rest of this wiki. It is important to understand the pathophysiology and presenting symtoms because this ensures the correct treatment strategy is chosen.
By the end of this section you should be able to:
- Discuss the background of lymphoedema and describe the key presenting symptoms
The next section of the wiki focuses on discussing the physiotherapists role in managing lymphoedema and critically anlayses a range of available. Before progressing onto this section, please ensure you have taken time to complete all the activities above.
Treatment and Management of Lymphoedema[edit | edit source]
Introduction[edit | edit source]
The Lymphoedema Framework (2006) states that the treatment of people with lymphoedema should be specifically tailored based on the site, severity and complexity as well as their psychosocial situation. Furthermore the success of treatment does not solely rest on the therapist, patients and carers must play an active role from an early stage.
Alongside the physical difficulties that people with lymphoedema face, emotional and social implications may also arise. Evidence has suggested that through specific management and targeting of the physical symptoms, the psychosocial issues can be reduced to enhance the individual’s quality of life (Kim and Park 2008).
Decongestive lymphatic therapy (DLT) is viewed as the gold standard of care for lymphoedema (Chang and Cormier 2013). Kim and Park (2008) found this treatment approach effective and significantly reduced the percentage excess limb volume as well as improving quality of life.
Decongestive lymphatic therapy encompasses four main components (Todd 2009);
- Compression
- Skin care
- Exercise
- Massage
The management of lymphoedema is split into intensive and maintenance stages, both of which have very different approaches. The goals during the intensive stage of therapy are to reduce and control the swelling, maintain skin quality and educate the patient in order for them to reach a stage where they are ready to progress into the maintenance phase of treatment (Korpan et al. 2011). This is achieved through a number of approaches aiming to reduce the load and decongest the lymphatic system, stimulate the function and encourage drainage through various routes (Lymphoedema Framework 2006). Once swelling is bought under control patients will progress to the maintenance stage. During this stage people with lymphoedema are educated to self manage their condition and will be reviewed less frequently by a specialist.
Over the next four sections of this wiki you will learn more about each of the components of DLT.
Activity
Take 5 minutes -
Can you...
- Think of any psychological issues that you may encounter if treating a patient with lymphoedema?
- Name the four cornerstones of lymphoedema treatment?
- List the goals during intensive therapy?
By this stage you should be able to identify the four cornerstones of DLT and state the general aims of the intensive and maintenance stages of treatment.
Over the next section this wiki will discuss the four components of DLT in detail with reference to the supporting evidence.
Compression Therapy[edit | edit source]
Compression therapy consists of two main methods – multilayer lymphoedema bandaging (MLLB) and compression garments. Overall, compression therapy increases lymphatic drainage, reduces capillary function, promotes fluid movement to less compressed areas of the body and improves the action of the venous pump (Cooper 2015). Furthermore, bandaging aims to improve the shape of the limb, soften fibrosclerotic tissue, support and improve skin condition and manage symptoms (Foldi et al. 2005; Williams and Keller 2005).
Once no further benefit is being obtained from compression bandaging during the intensive phase, patients should be managed by compression garments for long-term maintenance (Lymphoedema Framework 2012). However MLLB may also be used as part of long-term management if compression garments are not suitable (Moffatt et al. 2005).
The combined treatment of bandaging followed by compression garments has been found to yield better results for reduction of moderate to severe lymphoedema compared with bandaging alone. This benefit was observed as being maintained for at least six months (Badger et al. 2000), hence this is the recommended course of treatment for people with lymphoedema (Lymphoedema Framework 2012).
Indications for compression therapy as stated by the Lymphoedema Framework (2006) are:
- Fragile, damaged or ulcerated skin
- Distorted limb shape
- Limb too large for compression garments
- Areas of tissue thickening
- Lymphorrhoea
- Lymphangiectasia
- Pronounced skin folds
Not all patients will be suitable for compression therapy and this decision needs to be made by patient and clinician. There are a number of contraindications stated below (Lymphoedema Framework 2006):
- Severe arterial insufficiency
- Uncontrolled heart failure
- Severe peripheral neuropathy
If patients present with any of the above conditions, a decision regarding different methods of treatment will need to be discussed.
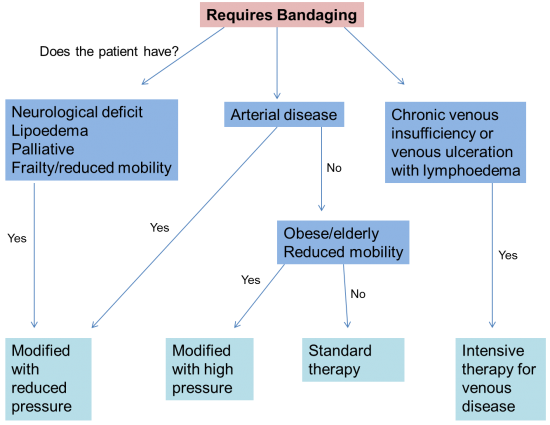
MLLB:
MLLB generally consists of a tubular lining, digit bandages, padding and layers of inelastic bandages. Due to the rapid change in limb shape and oedema reduction during the first 1-2 weeks bandages need to be changed daily to maintain the pressure (Williams and Keller 2005).
The pressure applied through bandages is based on Lapase’s Law (Urgo Medical 2009) –
P=(T x N x 4630)/(C x W)
P = pressure under the bandage (in mmHg),
T = bandage tension (Kgf)
N = number of layers
C = limb circumference (cm)
W = bandage width (cm)
Bandages used are inelastic which result in high and low pressures exerted during movement and rest respectively (Moffatt et al. 2005). Elastic bandages produce less variation of pressure; these may be indicated if patients are immobile, have venous ulceration, lymphatic or venous disease or if the expected time of application is longer than normal (Lymphoedema Framework 2006).
As with most treatments, MLLB can be adapted to suit the patient needs by either adjusting pressure, frequency of reapplication, bulk of bandage and type of bandage (Lymphoedema Framework 2006). If pressure is not applied correctly venous and lymphatic flow can be compromised, therefore the proximal movement of fluid is reduced and swelling may present in the extremities (Williams and Keller 2005). When applied to the lower limb, care must be taken to ensure that the patient is still able to wear shoes during treatment as normal gait pattern is encouraged to maintain an effective calf and foot muscle pump (Williams and Keller 2005).
Bandaging a lymphoedema arm: (approx. 10 mins)
Bandaging a lymphoedema leg: (approx. 10 mins)
Inelastic and elastic bandages have been discussed, however more recently, a new bandaging system known as Coban 2 has been developed which can be used an alternative to MLLB. Coban 2 consists of a comfort layer and a compression layer that cohesively bond together (Lamprou et al. 2011). This eliminates the need for a thick padding layer that MLLB requires, resulting in a much less bulky appearance allowing patient’s more mobility and freedom.
Lamprou et al. (2011) conducted a prospective randomised controlled trial comparing Coban 2 with traditional bandaging methods in the treatment of lower limb lymphoedema. The results of this study found Coban 2 to be equally as effective in reducing limb volume.
Franks et al. (2012) studied the use of Coban 2 in arm and leg lymphoedema. Again this study supported the use of Coban 2 in the effective management of lymphoedema with the lower limb showing a greater reduction in swelling.
Although both of the above studies had relatively small sample sizes (40 and 24 participants respectively) resulting in low statistical power, they both showed encouraging results for the use of the new bandaging system.
A multicentre randomised controlled trial with 82 participants (Moffatt et al. 2011) investigating the frequency of application of Coban 2. Results found constant therapeutic effect was maintained when bandages were reapplied every four days. Compared with MLLB, which requires reapplication daily at certain stages of treatment, the Coban 2 bandages allow patients to have more freedom and independence.
Coban 2 bandaging: (approx. 15 mins)
As discussed, a number of trials have evaluated the effects of compression bandaging for lymphoedema, which have found positive results. The development of Coban 2 bandages is encouraging, however this still requires larger scale trials to fully evaluate the efficacy.
Now that compression bandaging has been considered, this wiki will now move on to discuss the use of compression garments which are used for the long-term management of limb shape and swelling (Lymphoedema Framework 2006).
Compression Garments/Hosiery
These made-to-measure, handmade garments will be considered once regular limb shape has been restored and the patient’s skin is fully intact and robust enough to tolerate the use of garments (Doherty et al. 2009; Linnitt and Davies 2007).
Although garments are important in the management of lymphoedema, patient and clinician must come to an informed decision regarding the appropriateness of this treatment modality. Doherty et al. (2009) explains that patient’s stage and severity of lymphoedema, shape and size of limb, skin resilience, shape distortion, ability to tolerate, lifestyle, mobility, age, psychological status and dexterity should be assessed and considered prior to measurement and fitting.
Once the progression from bandages to garments has been made, swelling and other symptoms must be monitored. If swelling is not controlled within the first three months of wearing compression garments, clinician and patient should consider further intensive therapy using MLLB (Moffatt et al 2005).
Measurement for hosiery will be undertaken by a qualified health professional, which may be a physiotherapist.
Take 10 minutes to refer to the 'Best Practice for the Management of Lymphoedema' pages 40-41 where you will find more information about fitting and measuring for lymphoedema compression garments
Garments are either constructed as a flat knit or a round knit. Flat knit knitted as a flat garment then joined at the seams, these are generally thicker and firmer. Round knitted garments are viewed as more aesthetically pleasing, as they are thinner than flat knit and are continuously knitted cylindrically without any seams (Lymphoedema Framework 2006).
Once measurement and construction of the garment is completed advice regarding the care at home will be provided in person and leaflets may also be given to the patient (Lymphoedema Framework 2006). If garments are poorly fitted, the swelling may not be contained and damage can occur to the tissues. This could result in discomfort and reduced tolerance leading to patients being unwilling to use compression hosiery as a long-term management option (Doherty et al. 2009).
As well as limb compression garments, if patients have trunk or breast lymphoedema garments or specialised bras can be provided (Lymphoedema Framework 2006).
Activity
Before progressing to the next section please take 15 minutes to check your knowledge of the following:
- List 3 indications for compression therapy
- Name 3 contraindications to compression therapy
- List the components of MLLB
- Understand (discuss with a partner) how bandaging can be altered to suit the patients needs
- Discuss the differences between MLLB and Coban 2 bandaging
- What are the benefits of using Coban 2 over MLLB?
- Name and explain the 2 kinds of compression hosiery
- What should be considered when assessing for compression hosiery?
Skin Care[edit | edit source]
Lymphoedema cause changes to the skin including thickening, hyperkeratosis, hyperpigmentation and papillomatous or verrucous nodules (Nowicki and Siviour 2013). As a consequence of swelling, large skin folds can appear where infections may develop (Lymphoedema Framework 2006). Furthermore infections may arise if the skin becomes damaged or broken, therefore adequate skin care to maintain the integrity and manage any problems that occur is fundamental in the care of people with lymphoedema (Lymphoedema Framework 2006; Wigg and Lee 2015). At both intensive and maintenance stages, it is important to emphasise the need for a skin care regime to maintain the skin integrity.
The Lymphoedema Framework (2012) outlines the main principles of skin care:
- Wash daily
- Ensure skin folds are clean and dry
- Monitor the skin for changes
- Apply emollients
- Avoid scented products
- Using vegetable-based products in tropical climates rather than petrolatum or mineral oil based products
Washing can remove the protective lipid layer that prevents water loss and protects the skin from infection. Therefore emollients are applied to re-establish this layer thus preventing any further water loss and maintaining the barrier to protect from bacteria and other irritants (Lymphoedema Framework 2012).
Any soap that is abrasive or scented are to be avoided, natural or pH neutral soaps are recommended (Lymphoedema Framework 2006; Nowicki and Sivour 2013). This is because normal soaps contain detergents, are often scented and include preservatives, which can irritate or dry the skin.
During assessment, health professionals must inspect the skin condition using palpation and observation to check for any changes or damage (Nowiki and Siviour 2013). If changes have occurred these must be managed and monitored correctly.
Following assessment and cleansing of the skin emollients are applied to maintain skin hydration. These can either be moisturisers, soaps substitutes or bath oils. Moisturisers come in different forms including cream, lotion and ointments (Nowicki and Siviour 2013). The Lymphoedema Framework (2006) recommends the use of ointments, which contain little or no water; this hydrates the skin better than creams and lotions.
Despite the treatment offered infections may still occur that must be managed by thorough skin hygiene, ensuring skin is dried following washing and an anti-fungal powder or cream applied until the infection disappears (Nowicki and Sivour 2013).
The body’s natural response to sunburn is to increase blood flow to the affected area. For people with lymphoedema this will increase the load on an already impaired lymphatic system and may increase swelling. Therefore it is advised that people with lymphoedema take extra care to avoid sunburn (Nowicki and Siviour 2013).
Despite being an integral part of lymphoedema management, some patients experience barriers that prevent adequate skin care and result in infections. James (2011) studied the perceived barriers to skin care, which included physical limitations, expense, poor understanding, anxiety and motivational issues. This indicates that health professionals play a large role in educating patients about the importance of skin care to facilitate self-management. Health professionals should be aware of these potential barriers and be able to overcome them through education and support to facilitate self-management.
Activity
Take 10 minutes-
Can you…
List the main principles of skin care?
Explain why are emollients important?
True or false – is ointment recommended over lotions?
Take 5 minutes to think of how you would explain the importance of skin care to a patient you are treating? If possible discuss this with a partner.