Action Observation Therapy
Top Contributors - Redisha Jakibanjar, Kim Jackson, Candace Goh, Admin, Aminat Abolade and Uchechukwu Chukwuemeka
Introduction[edit | edit source]
Action Observation (AO) involves the dynamic process of observing purposeful actions with the intention of imitating and then practicing those actions.
Action Observation Therapy (AOT) is a multi-sensory approach grounded in basic neuroscience which involves somatosensory and cognitive rehabilitation[1]. This approach works by activating the mirror-neural system (MNS) of the brain[2][3].
Recent literature has demonstrated how merely observing a specific action activates the same cortical brain areas that are committed to that motor function[4]. This helps the planning of movement and neuroplasticity.
AOT commonly includes action observation and action execution and allows patients to safely practice movements and motor tasks.[3]
Purpose[edit | edit source]
- To recover damaged cerebral networks and take advantage to rebuild motor function despite impairments, as an alternative or complement to physiotherapy.[5]
- Promote functional reorganization within the brain via activation of mirror neurons in order to promote motor function recovery.[6]
Technique[edit | edit source]
There are no specific rules for performing the therapy but the general process is:
- During each rehabilitation session, the patient is required to observe a specific object-directed daily action presented through a video clip[7] or real-life demonstration[8]. For example, the act of drinking - a healthy adult reaching out his hand to pick up a cup and bringing the cup to his mouth.
- After watching for some time, individuals may or may not be asked to perform the same action[9].
- AO may be applied alone or combined with other practices such as imitation and execution of functional activities to stimulate motor relearning process [10].
- If practiced with execution of action, only one action is practiced during each rehabilitation session. The presented action can be divided into three to four motor tasks. The presented task in video can be shown from different perspectives such as third person perspective or first person perspective for better outcomes[11][9].
Phases[edit | edit source]
- Observation phase: during this phase, the patient is asked to carefully observe the given video.
- Execution phase: during this phase, the patient is asked to perform the observed motor task at the best of his/her ability.[11]
Time Duration[edit | edit source]
There is no specific rule for performing the task but typically, an AOT rehabilitation session takes half an hour. A few minutes are needed by the physiotherapist to explain the task to the patient (carefully looking at the movement, paying attention also to the details of presented actions) and to motivate him to the task, then 12 min of observation (3 min for each of the motor acts into which the action is divided) and finally 8 min of execution (2 min for each motor act). There is currently no evidence available regarding whether a more intensive practice, for example, 1 hour per session, is better than half an hour.[11]
Actions Used[edit | edit source]
- Transitive actions: Actions with object interaction, e.g., using a pencil
- Intransitive actions: Actions without object interaction, e.g., the opposition of the index finger and the thumb as the pantomime of a precision grasping) [12]
Measuring results[edit | edit source]
Evaluation of the result while performing the AOT is a vital thing to be considered. The use of an appropriate outcome measure or index is a basic requisite to analyze the efficacy of any rehabilitative therapy.[12]
Neurophysiological basis[edit | edit source]
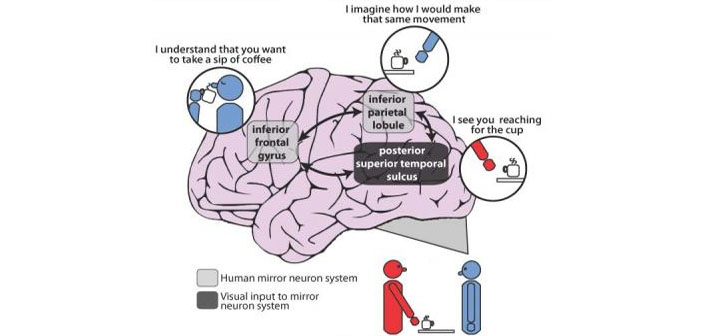
AOT is based on mirror neurons in various regions of the macaque cerebral cortex. Mirror neurons discharge both during the execution of goal-directed actions performed with different biological effectors and during the observation of another individual performing the same or a similar action. Areas containing mirror neurons are often referred to as the MNS. various non-invasive procedure has shown experimental evidence in humans confirming the existence of an action observation–action execution matching mechanism in specific regions of the frontal and parietal lobes.[11]
AOT in Parkinson's and Stroke[edit | edit source]
- A systematic review on efficacy of action observation and motor imagery among Parkinson's concluded that AOT and Motor Imagery Practice (MIP) used as therapeutic programs can improve or slow the deterioration of motor capabilities in Parkinson's patients.[13]
- Study was done among stroke patients (total included number=70 ) who had cerebral infarction diagnostic criteria formulated by Chinese Society of Neurology, Chinese Medical Association; unilateral hemiplegia; first-episode of cerebral infarction determined by CT and MRI; stable vital signs; disease course of 2 to 6 months; age of 40 to 75 years; mini-mental state examination (MME) score ≥27 and treatment instructions can be performed; Fugl-Meyer assessment (FMA) score ≥20 for upper extremity motor function; binocular vision or corrected visual acuity ≥1.0; everyday treatment can be tolerant; and providing informed consent. this study concluded that motion observation and traditional upper limb rehabilitation treatment technology can significantly elevate the movement function of cerebral infarction patients in sub acute seizure phase with upper limb dysfunction, which expanded the application range of motion observation therapy and provided an effective therapy strategy for upper extremities hemiplegia in stroke patients.[14]
- Randomised control trial (RCT) among 67 patients with purely ischemic stroke showed that action observation can stimulate and enhance the beneficial effects of motor training on motor memory formation, especially in left hemiparetic patients following an acute ischemic stroke.[15]
- AOT is an effective intervention for improving post-stroke upper limb function.[16] [17] AOT promotes increased upper limb motor recovery compared to task-oriented training. Improvement in FMA-UE scores was seen in subacute stroke with moderate to severe impairments (p<0.05).[18]
AOT in Total Hip Arthroplasty[edit | edit source]
A prospective study conducted among 24 patients to investigate the effectiveness of AOT compared with written information in patients submitted to a physical therapy program after primary total hip arthroplasty (THA) showed that both treatments were effective at improving pain, functional status, quality of life, and gait features in patients with primary THA. In addition to conventional physical therapy, AOT improved perceived physical function more than written information.[19]
References[edit | edit source]
- ↑ Johansson BB. Current trends in stroke rehabilitation. A review with focus on brain plasticity. Acta Neurologica Scandinavica. 2011 Mar;123(3):147-59.
- ↑ Shih TY, Wu CY, Lin KC, Cheng CH, Hsieh YW, Chen CL, Lai CJ, Chen CC. Effects of action observation therapy and mirror therapy after stroke on rehabilitation outcomes and neural mechanisms by MEG: study protocol for a randomized controlled trial. Trials. 2017 Dec;18(1):459.
- ↑ 3.0 3.1 Ertelt D, Binkofski F. Action observation as a tool for neurorehabilitation to moderate motor deficits and aphasia following stroke. Neural regeneration research. 2012 Sep 15;7(26):2063.
- ↑ Ge S, Liu H, Lin P, Gao J, Xiao C, Li Z. Neural basis of action observation and understanding from first-and third-person perspectives: an fMRI study. Frontiers in behavioral neuroscience. 2018 Nov 22;12:283.
- ↑ Sarasso E, Gemma M, Agosta F, Filippi M, Gatti R. Action observation training to improve motor function recovery: a systematic review. Archives of physiotherapy. 2015 Dec;5(1):1-2.
- ↑ Zhu MH, Wang J, Gu XD, Shi MF, Zeng M, Wang CY, Chen QY, Fu JM. Effect of action observation therapy on daily activities and motor recovery in stroke patients. International journal of nursing sciences. 2015 Sep 1;2(3):279-82.
- ↑ Calvo-Merino B, Glaser DE, Grèzes J, Passingham RE, Haggard P. Action observation and acquired motor skills: an FMRI study with expert dancers. Cerebral cortex. 2005 Aug 1;15(8):1243-9.
- ↑ Cowles T, Clark A, Mares K, Peryer G, Stuck R, Pomeroy V. Observation-to-imitate plus practice could add little to physical therapy benefits within 31 days of stroke: translational randomized controlled trial. Neurorehabilitation and Neural Repair. 2013 Feb;27(2):173-82.
- ↑ 9.0 9.1 Borges LR, Fernandes AB, Dos Passos JO, Rego IA, Campos TF. Action observation for upper limb rehabilitation after stroke. Cochrane Database of Systematic Reviews. 2022(8).
- ↑ Small SL, Buccino G, Solodkin A. The mirror neuron system and treatment of stroke. Developmental psychobiology. 2012 Apr;54(3):293-310.
- ↑ 11.0 11.1 11.2 11.3 Buccino G. Action observation treatment: a novel tool in neurorehabilitation. Philosophical Transactions of the Royal Society B: Biological Sciences. 2014 Jun 5;369(1644):20130185.
- ↑ 12.0 12.1 Plata-Bello J. The Study of Action Observation Therapy in Neurological Diseases: A Few Technical Considerations. Neurological Physical Therapy: IntechOpen. 2017 May 10:1-3.
- ↑ Caligiore D, Mustile M, Spalletta G, Baldassarre G. Action observation and motor imagery for rehabilitation in Parkinson's disease: A systematic review and an integrative hypothesis. Neuroscience & Biobehavioral Reviews. 2017 Jan 1;72:210-22.
- ↑ Fu J, Zeng M, Shen F, Cui Y, Zhu M, Gu X, Sun Y. Effects of action observation therapy on upper extremity function, daily activities and motion evoked potential in cerebral infarction patients. Medicine. 2017 Oct;96(42).
- ↑ Ceravolo MG. Action Observation as a Tool for Upper Limb Recovery. Fizikalna i rehabilitacijska medicina. 2016 Apr 3;28(1-2):144-50.
- ↑ Ryan D, Fullen B, Rio E, Segurado R, Stokes D, O’Sullivan C. Effect of action observation therapy in the rehabilitation of neurologic and musculoskeletal conditions: a systematic review. Archives of Rehabilitation Research and Clinical Translation. 2021 Mar 1;3(1):100106.
- ↑ Zhang B, Kan L, Dong A, Zhang J, Bai Z, Xie Y, Liu Q, Peng Y. The effects of action observation training on improving upper limb motor functions in people with stroke: A systematic review and meta-analysis. PLoS One. 2019 Aug 30;14(8):e0221166.
- ↑ Mancuso M, Tondo SD, Costantini E, Damora A, Sale P, Abbruzzese L. Action observation therapy for upper limb recovery in patients with stroke: a randomized controlled pilot study. Brain Sciences. 2021 Feb 26;11(3):290.
- ↑ Villafañe JH, Pirali C, Isgrò M, Vanti C, Buraschi R, Negrini S. Effects of Action Observation Therapy in Patients Recovering From Total Hip Arthroplasty Arthroplasty: A Prospective Clinical Trial. Journal of chiropractic medicine. 2016 Dec 1;15(4):229-34.