Multiple Sclerosis: A Case Study
Top Contributors - Zoe Ellis, Alexa Evelyn Giampuzzi, Kim Jackson and Emilie Noble
Abstract[edit | edit source]
The purpose of this fictional case study is to highlight key clinical findings in a patient diagnosed with Relapsing Remitting Multiple Sclerosis (RRMS). The patient discussed throughout the case study presents with chronic fatigue, lower extremity weakness, impaired balance, lack of coordination and psychosocial characteristics. In turn, these symptoms combined have led to the patient experiencing an overall decreased quality of life. Interventions such as Tai Chi, moderate intensity aerobics, strength training and self management techniques were introduced to the patient upon initial assessment. Baseline scores for patients overall function, balance, coordination, depression and fatigue were obtained during the initial assessment using outcome measures. Outcome measures were then used to reassess patients progress over a 12 week treatment period. Outcome measures used throughout this case study include BERG, Lower Extremity Functional Scale (LEFS), Patient Health Questionnaire (PHQ-9) heel knee shin test, finger to nose test and Fatigue Severity Scale (FSS).
Introduction[edit | edit source]
Multiple Sclerosis (MS) (MS) is an autoimmune disorder characterized by demyelination and subsequent axonal injury and loss in the central nervous system [1]. This injury to the central nervous system causes white matter lesions, also known as plaques, which are responsible for the patients’ symptoms. There are a few different classifications of MS based on occurrence of relapses or progression. The most common form is Relapsing Remitting Multiple Sclerosis (RRMS) whereby the patient will have new symptoms emerge or a worsening of past symptoms, followed by full, or near full recovery [1]. The majority of RRMS cases eventually transition to a progressive form called Secondary Progressive Multiple Sclerosis (SPMS) [1]. About 15% of MS cases are Primary Progressive (PPMS) where function continues to decline from onset [1].
This fictional case study discusses a 27 year-old female diagnosed with Relapsing Remitting Multiple Sclerosis two years ago.
Patient first noticed symptoms that persisted for 24 hours including vision loss in one eye accompanied by facial weakness, numbness and difficulty with speech (dysarthria) in April of 2017. After the symptoms did not subside, the patient reached out to her family doctor who then suggested further testing. The patient underwent magnetic resonance imaging (MRI) and a lesion was revealed on the brainstem. These results lead to the patient being classified as having Clinically Isolated Syndrome [2]. Patients such as this one being discussed are classified as having Clinically Isolated Syndrome when an initial event leads to a clinical presentation of symptoms and the MRI reveals lesions [2]. It wasn’t until three months after the initial MRI that the patient started experiencing extreme fatigue and balance problems possibly due to lower extremity weakness. The patient underwent a second MRI which revealed another lesion in her right cerebral hemisphere. Due to a relapse in symptoms, the patient was formally diagnosed with Relapsing Remitting Multiple Sclerosis (RRMS) [3]. It has been two years since the patients diagnosis and she has opted to come to physiotherapy to help control her fatigue, lower limb weakness, coordination and maintain general fitness.
The purpose of this fictional case study is to present the patients symptoms of MS (fatigue, balance and lower limb weakness) and their response to physical therapy treatment. Similar cases of moderate to severe MS presenting with fatigue and weakness have shown significant improvements through physical therapy treatment [4]. In general, both strength and endurance training result in fatigue reduction; however, evidence is insufficient in specifying which training modality has the strongest effect [4]. Although there is a need for specific balance exercises in MS patients, there is evidence that suggests progressive aerobic and resistance exercises have positive effects on balance in patients who present with mild to moderate symptoms. [5]
Client Characteristics[edit | edit source]
Patient is a 27 year-old caucasian female diagnosed with Relapsing Remitting Multiple Sclerosis that began two years ago. The patient is a current smoker and has a history of depression. The patient self referred herself to physiotherapy to help manage her weakness, coordination and fatigue. Additionally, the patient is looking to learn how to self manage her symptoms.
Examination Findings[edit | edit source]
Subjective Assessments[edit | edit source]
History of Present Illness[edit | edit source]
- Medical diagnosis (Dx): Relapsing Remitting Multiple Sclerosis
- Rehabilitation Hx: no previous physiotherapy intervention used for current symptoms
- Current symptoms: fatigue, weakness (mainly in lower extremities), difficulty with gait, impaired balance and coordination
Medical History[edit | edit source]
- Past medical Hx: diagnosed with Mononucleosis at age 17
- Co-morbid condition: diagnosed with depression at age 15 and currently smokes an average of one pack of cigarettes every two days
Social History[edit | edit source]
- Lives with partner in a bungalow that has 6 steps to reach the entrance of the home. Patients parents live 15 minutes away. Patient works as a 4th grade teacher
- Hobbies include skiing and hiking
Functional Status[edit | edit source]
- Reports difficulty finding motivation to leave the house or do simple housework due to fatigue
- Feels like her legs are too weak to participate in hobbies and hasn’t attempted to ski since diagnosis. She occasionally will go on short, easy hikes if she is having a good day
Medication[edit | edit source]
- Alysse (birth control)
- Ocrelizumab/Ocrevus (infusion treatment for multiple sclerosis)
Self Report Tests[edit | edit source]
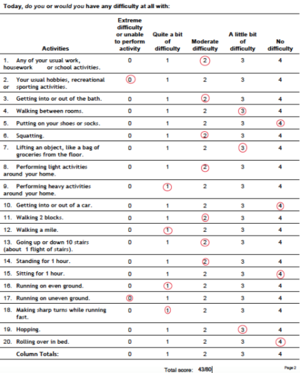
- Lower Extremity Function Questionnaire (LEFS) was used to assess the patient's ability to perform everyday tasks. The lower the score, the greater the disability. The patient scored 43/80 seen in the figure below [6].
Figure 1. Patient completed LEFS with a total score of 43/80[6].
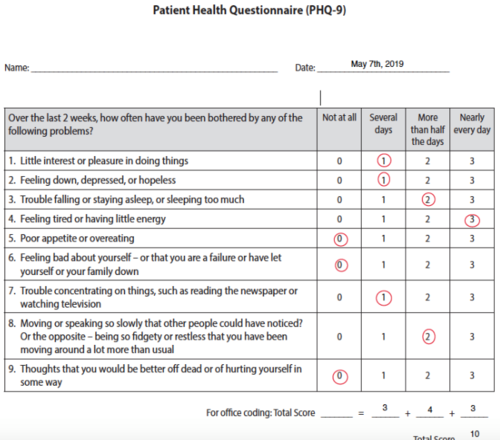
- Patient Health Questionnaire (PHQ-9) was used to assess the patient's depression severity. The patient scored a 10 which suggests moderate depression severity and that judgements on treatment should be based on the patient's functional impairments and duration of symptoms [7].
Figure 2. Patient completed PHQ-9 with a total score of 10[7].
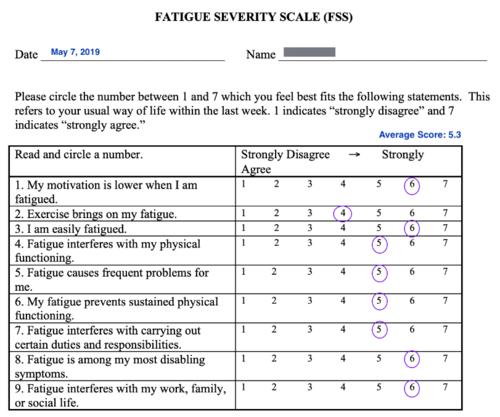
- Fatigue Severity Scale (FSS) was used to assess patients fatigue within the past week. Patient scored a mean score of 5.3.
Figure 3. Fatigue Severity Scale (FSS): Mean score of 5.3 (>/=4 classified as substantial fatigue) [8] [9].
Diagnostic Tests[edit | edit source]
- Magnetic Resonance Imaging (MRI)
- Lumbar puncture (spinal tap)
Objective Assessment[edit | edit source]
- Timed Up and Go (TUG): 10.5 seconds = just above the norm of < or equal to 10 seconds[10]
- Berg: 46/56 = 42-56% at an increased risk of falling[11]
- Cranial nerve function tests: WNL except CNXII had decrease sensation and motor control over V1
- Babinski: positive
- Clonus: positive
- LMN reflexes UE/LE: WNL
- Dermatomes: WNL
- Myotomes: UE: WNL; LE: WNL
- Resisted LE testing: hip flexors, knee extensor, knee flexors 4-/5, DF and PF 4/5
- Squat Test: 2 moderate depth, unsupported squats
- Heel knee shin test: 3 bilaterally showing minimal impairment; patient is able to accomplish activity with slightly less than normal control, speed and steadiness
- Finger to nose test: WNL (4) on right; 3 on left showing minimal impairment; patient is able to accomplish activity with slightly less than normal control, speed, steadiness
- Sensation testing: superficial and deep: WNL
- Spasticity Testing: As seen below:
Table 1. Modified Ashworth Rating of the Upper and Lower Extremities [12]
| Body Segment | Modified Ashworth Rating (Left) | Modified Ashworth Rating (Right) |
|---|---|---|
| Elbow flexors | 1 | 0 |
| Elbow Extensors | 1 | 0 |
| Wrist Flexors | 0 | 0 |
| Wrist Extensors | 0 | 0 |
| Hip Flexors | 2 | 2 |
| Hip Extensors | 1+ | 1 |
| Knee Flexors | 1+ | 1+ |
| Knee Extensors | 1+ | 1+ |
| Ankle Dorsiflexors | 1 | 1 |
Clinical Impression[edit | edit source]
Physiotherapy Diagnosis[edit | edit source]
Patient was a previously active 27 year-old female diagnosed with Relapsing Remitting Multiple Sclerosis two years ago when she first started showing signs of the disease. Three months within that year, the patient experienced her first relapse of the disease which ultimately lead to chronic fatigue, weakness and impaired coordination of the lower extremities affecting functional mobility and impacting her ability to independently engage in activities of daily living.
Problem List[edit | edit source]
- Fatigue impacting overall quality of life
- Lower limb weakness impairing functional mobility
- Impaired coordination affecting activities of daily living
- Current smoke (1 pack every 2 days)
Intervention[edit | edit source]
Patient Centred Goals[edit | edit source]
Short Term Goals[edit | edit source]
- Improve lower extremity strength, by successfully completing 10 consecutive moderate depth unsupported squats by 2 months.
- Successfully coordinate 3 consecutive jumping jacks by 2 months.
- Improve walking endurance to 30 minutes of moderate intensity using a graded exercise walking program by two months.
- Reduce smoking to 1/2 pack biweekly by 2 months.
Long Term Goals[edit | edit source]
- Reduce score on the FSS to average of 4 or below within 6 months.
- Hike a moderate difficulty trail for a duration of 1 hour within 6 months.
- Ski 2 green runs in a day within 2 years.
- Cessation of smoking by 6 months.
Approaches/Techniques[edit | edit source]
Adults with MS should engage in at least 30 minutes of moderate intensity aerobic activity two times per week and strength training of major muscle groups two times per week to achieve important fitness benefits [13].
Resistance Training[edit | edit source]
The patient will start with 10-15 reps for one set and will work up to doing two sets for strength exercises such as squats, leg press, hamstring curls, abductor/adductor machine and calf raises.
Aerobic Training[edit | edit source]
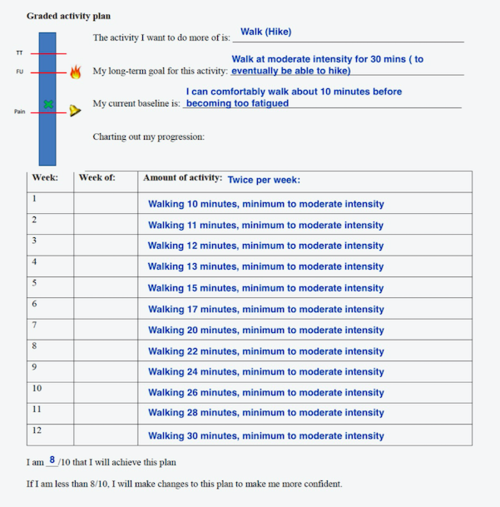
The patient will participate in a graded walking activity plan until she can sustain a moderate intensity walk for a 30 minute duration as seen in the figure below: [14]
Figure 4. A 12 week graded activity walking plan formed in collaboration with the patient. [14]
Balance and Coordination Training[edit | edit source]
Tai Chi will be recommended to the patient to help improve overall balance and coordination. Tai Chi has been proven to have consistent and significant improvements in patients with Multiple Sclerosis’ balance and coordination. In addition, the physical exercise and mindfulness training incorporated in Tai Chi has shown improvements in patients mental health, specifically depression. The patient will begin incorporating Tai Chi into her schedule by participating in 30 minutes per week and eventually progressing to the recommended 45 minutes per week. [15]
Self Management[edit | edit source]
- Keep an activity and symptom diary to track symptoms and discover patterns.
- Education on energy conservation strategies:
- Forming a mental map of resting spots/benches for outings
- Have a set plan for the day to avoid fatigue (ex. doing more fatiguing exercises at the end of the day)
- Education on importance of keeping core temperature low to avoid disease worsening symptoms [16] and how to accomplish this:
- Taking breaks
- Seated exercises
- Working out in a cool environment
- Incorporating social cognitive therapy (SCT) into the exercise program. SCT includes educating patient on goal setting, outcome expectations and self efficacy [17].
Outcomes[edit | edit source]
12 Week Re-Assessment[edit | edit source]
- The patient has been partaking in Tai Chi classes for 30 minutes per week.
- Patients PHQ-9 score decreased from 10 to 8.
- Coordination was re-evaluated using finger to nose test and heel knee shin test which both showed improvements, however, the improvements are not yet clinically significant.
- BERG score has improved to 50/56 indicating 24-32% increase in fall risk.
- After 12 weeks of combined strength and aerobic training twice a week, the patient has noticed an improvement in her fatigue. This was confirmed by retaking the Fatigue Severity Scale where she obtained an average score of 4.5 compared to her original score of 5.3 12 weeks prior.
- Additionally, there was no detectable change in the manual muscle testing results, however, patient was able to perform 8 consecutive moderate depth, unsupported squats.
The patient is encouraged to maintain consistency throughout treatment. It is suggested that patient increases their Tai Chi to 45 minutes per week and continues to increase walking time on graded walking program to continue making improvements.
Discussion[edit | edit source]
This case study examines a young female patient with a typical presentation of Relapsing Remitting Multiple Sclerosis. The patient sought treatment from physiotherapy after her most recent attack left her with symptoms of fatigue, lower extremity weakness, loss of coordination and balance. Through objective measures, the physiotherapists working with this patient were able to create goals based on their findings and ultimately create a treatment plan. Fatigue associated with MS can be one of the most debilitating symptoms and can affect a patient's quality of life tremendously. It is important to address this in treatment through the use of aerobic and resistance training as well as with Thai Chi. In addition, interventions such as these pose secondary positive effects on coordination, balance and depression[15] . Due to MS being a progressive disease, it is important to educate the patient on both self management techniques such as energy conservation strategies and the importance of keeping their core temperature low to avoid worsening of the disease [16]. Furthermore, knowing you have a progressive disease can be mentally taxing. Therefore, it is vital to incorporate SCT with an emphasis on goal setting, outcome expectations and self efficacy [17].
The implications of this case suggest multiple modes of exercise training can have a significant impact on quality of life, fatigue and strength in patients with mild to moderate Relapsing Remitting Multiple Sclerosis [4]. Currently, there is a plethora of research on mild to moderate severity Multiple Sclerosis, however, the literature is lacking for severe cases. Thus, future inquiry should address intervention based research in severe Multiple Sclerosis.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Kamm CP, Uitdehaag BM, Polman CH. Multiple sclerosis: current knowledge and future outlook. European neurology. 2014;72(3-4):132-41.
- ↑ 2.0 2.1 Lublin FD, Reingold SC, Cohen JA, Cutter GR, Sørensen PS, Thompson AJ, Wolinsky JS, Balcer LJ, Banwell B, Barkhof F, Bebo B. Defining the clinical course of multiple sclerosis: the 2013 revisions. Neurology. 2014 Jul 15;83(3):278-86.
- ↑ Lublin FD, Reingold SC. Defining the clinical course of multiple sclerosis: results of an international survey. Neurology. 1996 Apr 1;46(4):907-11.
- ↑ 4.0 4.1 4.2 Khan F, Amatya B. Rehabilitation in multiple sclerosis: a systematic review of systematic reviews. Archives of physical medicine and rehabilitation. 2017 Feb 1;98(2):353-67.
- ↑ Paltamaa J, Sjögren T, Peurala SH, Heinonen A. Effects of physiotherapy interventions on balance in multiple sclerosis: a systematic review and meta-analysis of randomized controlled trials. Journal of rehabilitation medicine. 2012 Oct 5;44(10):811-23.
- ↑ 6.0 6.1 Lower Extremity Functioning Scale. Retrieved From: https://www.honorhealth.com/sites/default/files/documents/medical-services/leg-functional-scale-form.pdf
- ↑ 7.0 7.1 Patient Health Questionnaire (PHQ 9). Retrieved From: https://www2.gov.bc.ca/assets/gov/health/practitioner-pro/bc-guidelines/depression_patient_health_questionnaire.pdf
- ↑ Fatigue Severity Scale. Retrieved From: https://geriatrictoolkit.missouri.edu/fatigue/Fatigue-Severity-Scale.pdf
- ↑ Rosti‐Otajärvi E, Hämäläinen P, Wiksten A, Hakkarainen T, Ruutiainen J. Validity and reliability of the Fatigue Severity Scale in Finnish multiple sclerosis patients. Brain and behavior. 2017 Jul;7(7):e00743.
- ↑ Timed Up & Go Test. Retrieved From: Physiopedia Timed Up and Go Test
- ↑ Berg Balance Scale. Retrieved from: Physiopedia Berg Balance Scale
- ↑ Modified Ashworth Rating. Retrieved From: https://www.med-iq.com/files/noncme/material/pdfs/DOC%201--Modified%20Ashworth%20Scale.pdf
- ↑ Latimer-Cheung AE, Ginis KA, Hicks AL, Motl RW, Pilutti LA, Duggan M, Wheeler G, Persad R, Smith KM. Development of evidence-informed physical activity guidelines for adults with multiple sclerosis. Archives of physical medicine and rehabilitation. 2013 Sep 1;94(9):1829-36.
- ↑ 14.0 14.1 George SZ, Zeppieri Jr G. Physical therapy utilization of graded exposure for patients with low back pain. journal of orthopaedic & sports physical therapy. 2009 Jul;39(7):496-505.[1]
- ↑ 15.0 15.1 Burschka JM, Keune PM, Hofstadt-van Oy U, Oschmann P, Kuhn P. Mindfulness-based interventions in multiple sclerosis: beneficial effects of Tai Chi on balance, coordination, fatigue and depression. BMC neurology. 2i014 Dec;14(1):165.
- ↑ 16.0 16.1 Allen DR, Huang M, Morris NB, Chaseling GK, Frohman EM, Jay O, Davis SL. Impaired thermoregulatory function during dynamic exercise in multiple sclerosis. Medicine & Science in Sports & Exercise. 2019 Mar 1;51(3):395-404.
- ↑ 17.0 17.1 Coote S, Uszynski M, Herring MP, Hayes S, Scarrott C, Newell J, Gallagher S, Larkin A, Motl RW. Effect of exercising at minimum recommendations of the multiple sclerosis exercise guideline combined with structured education or attention control education–secondary results of the step it up randomised controlled trial. BMC neurology. 2017 Dec;17(1):119.