Rotator Cuff
Original Editor - Florence Brachotte
Top Contributors - Els Van Haver, Amanda Ager, Admin, Kim Jackson, Naomi O'Reilly, Uchechukwu Chukwuemeka, Joao Costa, Tony Lowe, Wendy Walker, George Prudden, Vidya Acharya, Rachael Lowe, Florence Brachotte, Oyemi Sillo, WikiSysop and Fasuba Ayobami
Description[edit | edit source]
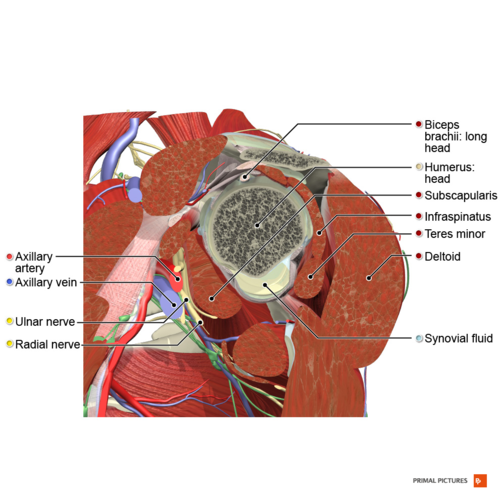
The Rotator Cuff (RC) is a common name for the group of 4 distinct muscles and their tendons, which provide strength and stability during motion to the shoulder complex. They are also referred to as the SITS muscle, with reference to the first letter of their names (Supraspinatus, Infraspinatus,Teres minor, and Subscapularis, respectively). The muscles arise from the scapula and connect to the head of the humerus, forming a cuff around the glenohumeral (GH) joint.
Anatomy[edit | edit source]
The rotator cuff muscles include: [1]
| Origen on scapula | Insertion on humerus | Primary function | |
|---|---|---|---|
| M. supraspinatus | supraspinous fossa | superior facet of greater tuberosity | abduction |
| M. infraspinatus | infraspinous fossa | middle facet of greater tuberosity | exorotation
(lateral / external rotation) |
| M. teres minor | lateral border of scapula | inferior facet of greater tuberosity | exorotation
(lateral / external rotation) |
| M. subscapularis | subscapular fossa | lesser tuberosity or humeral neck | endorotation
(medial / internal rotation) |
Cranial to the rotator cuff, there is a bursa which covers and protects the muscle and tendons, as they are in close contact to the surrounding bones.
Function[edit | edit source]
The RC muscles are each used in a variety of upper extremity movements including flexion, abduction, internal rotation and external rotation. They are essential players in almost every type of shoulder movement. Balanced strength and flexibility in each of the four muscles are vital to maintain functioning of the entire shoulder girdle.
As a group, the rotator cuff muscles are responsible for stabilizing the shoulder joint, by providing the "fine tuning" movements of the head of the humerus within the glenoid fossa. They are deeper muscles and are very active in the neuromuscular control of the shoulder complex during upper extremity movements.
They keep the head of the humerus within the small glenoid fossa of the scapula in order to enlarge the range of motion in the GH joint and avoid mechanical obstruction (i.e. a possible biomechanical impingement during elevation).[1][3]
It is well documented that RC dysfunctions can lead to shoulder pain, impaired functional capacities and a reduced quality of life. [4]
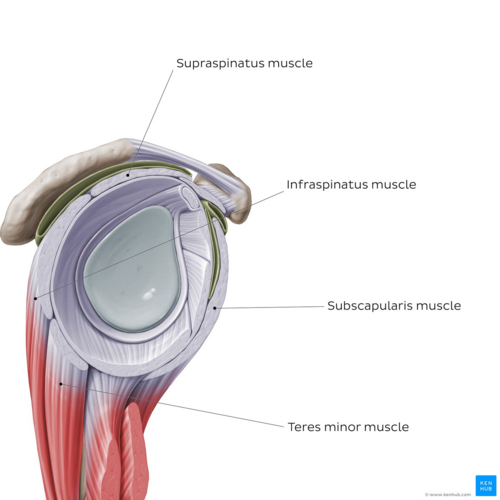
Image: Overview of the rotator cuff muscles - sagittal view[5]
Common Injuries to the Rotator Cuff[edit | edit source]
RC injuries are common injuries that can occur at any age. In younger subjects, most injuries occur secondary to trauma or arise from overuse due to overhead activities (e.g. volleyball, tennis, pitching). Incidence of injuries increases with age, however some individuals with rotator cuff pathology may be asymptomatic.[3][6] The RC muscles can fall victim to muscle degeneration, impingement and tearing with advancements in age. Poor biomechanics, such as postural dysfunctions (anterior posture of the GH in the glenoid cavity, for example) can prematurely affect the quality of the RC muscles and tendons due to repetitive strains and tissue encroachment.
Most common injuries to the Rotator Cuff are often referred to as:
- Rotator Cuff Tears (micro or macro tearing of the muscles or tendons);
- Rotator Cuff Tendinitis (acute inflammation of the RC soft tissue);
- Rotator Cuff Tendinopathy (chronic irritation or degeneration of the RC soft tissue);
- Impingement syndrome (biomechanical dysfunction of the shoulder complex with causes abnormal wear and tear on the RC soft tissue).
Common Symptoms[edit | edit source]
It is important to note that RC tears or injuries are not always associated with pain or patient-reported loss of function.[4] Moreover, it is worth noting that asymptomatic patients may develop symptoms in a relatively short period of time.
The most common signs of rotator cuff injuries are:
- Pain (may or may not be present). Can be localized to anterior / lateral aspect of the shoulder, with referred pain down the upper arm (lateral aspect).
- Painful range of motion
- Painful arch (degrees vary - generally above shoulder height)
- Painful external rotation / internal rotation / ABDuction
- Muscle weakness in the shoulder joint (particularly ABDuction and ER)
- Functional impairments (difficulty lifting, pushing, overhead movements and movements with hand behind the back (IR)).
These signs result mainly from a loss of the superior stability of the glenohumeral joint because of dysfunction of the rotator cuff muscles.[7]
Diagnosis of Rotator Cuff Pathologies[edit | edit source]
Key elements in diagnosing RC pathology are:[8]
- History
- Age / sex / co-morbididies (diabetes / smoking / prior shoulder pain / cervical pain)
- Participation in sports (contact sports / overhead sports)
- Mechanism of injury (acute injury (ie. Fallen on outstretched hand (FOOSH)) / trauma or repetitive strain)
- Physical Examination
- Visual inspection of the shoulder / cervical and thoracic spine
- C-spine scan (rule out referred pain and/or radiculopathy)
- Palpation (pain/deformity/swelling)
- Range of motion / functional movements
- Strength testing (manual muscles testing or with a hand held dynamometer)
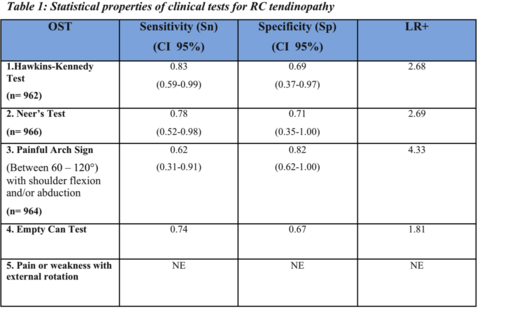
Clinical Tests: The diagnosis of an RC tendinopathy can be done in a clinic with the use of Cluster Tests:
The following Cluster Tests were retrieved from Roy et al. (2015)[9]:
- Hawkins-Kennedy test
- Neer's test
- Painful arch sign
- Empty can test
- Pain or weakness with external rotation.
- Diagnostic imaging of the shoulder:
- X-rays (less accurate for RC diagnosis; unless a suspected avulsion fracture, calcifications, arthritis or bone deformities)
- MRI (best practice for visibility of soft tissue) or
- Ultrasound (US)
It is important to differentiate shoulder pain coming from places other than the shoulder, such as the neck (referred cervical or thoracic pain) or elbow, and also pains from other structures at the shoulder, through anamnesis and physical examination. Pain is mostly provoked by overhead maneuvers and weakness of the shoulder muscles may occur.
RC muscles can not be seen on X-rays but calcifications, arthritis or bone deformations - that are common causes for rotator cuff pathologies - may be visible. The most common imaging method to evaluate rotator cuff pathologies is MRI. It can detect tears and inflammation and may help to determine size and character in order to establish a proper treatment protocol.
Although, MRI is the gold standard imaging method for rotator cuff pathologies, US can be used as it has a good diagnostic accuracy (Evidence level 2a)[10], more cost effective and readily available[11][12].
Possible confounding factors:[edit | edit source]
- Increase in age;
- MRI tear characteristics;
- Worker's compensation status.
Factors, such as age, chronicity, and severity of muscle tendon unit impairments, have been repeatedly associated with higher retear rates and poorer clinical outcomes.[4][13]
Possible co-morbidities:[edit | edit source]
- Diabetes;
- Smoking;
- Prior shoulder infection;
- Cervical disease.
Strength of recommendation: Inconclusive[14]
Common Treatments for Rotator Cuff Pathologies[edit | edit source]
Pain management[edit | edit source]
- NSAIDs, Moderate strength[14] (benefit exceed the potential harm) for use in the absence of a full thickness tear.
- Activity modification, ice, heat, iontophoresis, TENS, PEMF, phonophoresis. Strength of recommendations: inconclusive. [14]
Conservative treatments[edit | edit source]
- Physiotherapy / exercise prescription / modalities. Inconclusive strength.[14]
- Conservative treatment is effective for many rotator cuff injuries and comprises injecting corticosteroid (or sodium hyaluronate) into the subacromial space and physical therapy to increase the strength of residual muscles and ameliorate shoulder stiffness.
- Corticosteroid injections. Strength of recommendations: inconclusive.[14]
Surgical repair for acute RC tears[edit | edit source]
To obtain anatomic healing, the torn rotator cuff tendons must be repaired. Surgical repair has shown moderate to excellent clinical results in most studies. However, surgical treatment for chronic and large rotator cuff tears needs to be improved, especially for those in elderly patients, who continue to demonstrate high failure rates.[7]
For irreparable rotator cuff tears, alternative treatments include:[7]
- Superior capsule reconstruction;
- Reverse total-shoulder arthroplasty;
- Acromioplasty;
- Partial RC repair, debridement or muscle/tendon transfer (when irreparable RC tears);
- Allographs and xenographs.
Strength of recommendation: limited. [14]
Other Helpful Links[edit | edit source]
- Rotator Cuff Tears
- Rotator Cuff Tendinopathy
- Chronic Rotator Cuff Tendinopathy
- Tendinopathy
- Western Ontario Rotator Cuff Index (WORC)
References[edit | edit source]
- ↑ 1.0 1.1 Gray,H. Anatomy of the Human Body. Philadelphia: Lea and Febiger, 1918; Bartleby.com, 2000
- ↑ AnatomyZone. Rotator Cuff | 3D Anatomy Tutorial. Available from: https://www.youtube.com/watch?v=RaIt79pPfgE [last accessed 6/6/2022]
- ↑ 3.0 3.1 Codman EA. The shoulder. Malibar, Florida: R.E. Kreiger; 1934
- ↑ 4.0 4.1 4.2 Bachasson, D., Singh, A., Shah, S.B et al. The role of the peripheral and central nervous systems in rotator cuff disease. J Shoulder Elbow Surg. Vol 24. 1322-1335. 2015.
- ↑ Overview of the rotator cuff muscles - sagittal view image - © Kenhub https://www.kenhub.com/en/library/anatomy/the-rotator-cuff
- ↑ Matsen FA 3rd. Clinical practice. Rotator-cuff failure. N Engl J Med. 2008;358: 2138-47. http://www.nejm.org/doi/full/10.1056/NEJMcp0800814
- ↑ 7.0 7.1 7.2 Teruhisa, M. Chapter: Rotator Cuff Pathology in Textbook of Shoulder Surgery. Jan 2019. doi: 10.1007/978-3-319-70099-1_8.
- ↑ Jia X, Petersen SA, Khosravi AH, Almareddi V, Pannirselvam V, McFarland EG. Examination of the shoulder: the past, the present, and the future. J Bone Joint Surg Am. 2009;91:10-8.
- ↑ Roy et al. (2015). L’évaluationclinique, lestraitementset le retour en emploide travailleurssouffrantd’atteintesde la coiffedes rotators. Bliandes connaissances. Programme REPAR-IRSST. Rapport R-885.
- ↑ Lenza, M, Buchbinder, R, Takwoingi, Y, Johnston, RV, Hanchard, NC, Faloppa, F. Magnetic resonance imaging, magnetic resonance arthrography and ultrasonography for assessing rotator cuff tears in people with shoulder pain for whom surgery is being considered. Cochrane Database Syst Rev. 2013; DOI:10.1002/14651858.CD009020.pub2
- ↑ Day, M, Phil, M, McCormack, RA, Nayyar, S, Jazrawi, L. Physician Training Ultrasound and Accuracy of Diagnosis in Rotator Cuff Tears. Bulletin of the hospital for joint disease(2013). 2016; 74(3):207-11.
- ↑ Thakker, VD, Bhuyan, D, Arora, M, Bora, MI. Rotator Cuff Injuries: Is Ultrasound Enough? A Correlation with MRI. International Journal of Anatomy, Radiology and Surgery. 2017; Vol-6(3): RO01-RO07. DOI: 10.7860/IJARS/2017/28116:2279
- ↑ Le BT, Wu XL, Lam PH, Murrell GA. Factors predicting rotator cuff retears: an analysis of 1000 consecutive rotator cuff repairs. Am J Sports Med 2014;42:1134-42. http://dx.doi.org/10.1177/0363546514525336
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 American Academy of Orthopaedic Surgeons (AAOS). Optimizing the management of rotator cuff problems: Guideline and evidence report. AAOS Clinical Practice Guidelines Unit. v.1.1_033011. 2010.